Can Ibs Cause Blood In Urine
Symptoms of IBS may be present in many illnesses, such as infections. However, noticing blood in the urine is often a sign of an infection in the urinary tract.
If any blood is noticed in urine or stool, it often best to inform a GP who may like to investigate further.
Other possible causes of blood appearing in urine include kidney stones and an enlarged prostate.
Ways To Reduce The Risk Of An Ulcerative Colitis Emergency
While many patients with ulcerative colitis may experience only mild or occasional symptoms, emergency situations can develop suddenly in both the newly diagnosed and in people who have had ulcerative colitis for a long time.
Keep in mind that the duration of flare-ups can be unpredictable and that remissions can vary in length, which means you always need to be on alert for any new or different symptoms.
The most important control patients have to prevent flare-ups is to continue their maintenance medications, as directed,” says Hanauer. Antibiotics can also trigger flares, so they should only be used when appropriate not for colds or viral infections. Quitting smoking can also trigger flare-ups, so patients should discuss smoking cessation with their gastroenterologists.
Hanauer also recommends that patients with ulcerative colitis eat a healthy diet when theyre in remission to help ensure theyre meeting their nutritional requirements.
As the caregiver, you’re in a unique position to notice changes in the nature and intensity of your loved one’s ulcerative colitis symptoms. Always contact their medical team if you have any questions or suspect that the person with ulcerative colitis is experiencing an emergency. Your prompt action could save a life.
Additional reporting by Jordan M. Davidson.
When Is Surgery Necessary For Ulcerative Colitis
Most people with ulcerative colitis will never need to have surgery. However, if surgery becomes necessary, the operation permanently cures ulcerative colitis since the disease only affects the colon and not other parts of the intestinal tract.
Sometimes the doctor will recommend removing the colon if medical treatment fails or if the side effects of corticosteroids or other drugs threaten the patients health. For the 23% to 45% of people who eventually may have their colons removed because of massive bleeding, severe illness, rupture of the colon, or risk of cancer, various surgical techniques are used. The choice of surgical procedure is individualized based upon the needs of each patient. What is right for one patient may not be the best type of surgery for someone else.
Read Also: Is Kimchi Good For Ulcerative Colitis
Also Check: How To Heal Stomach Ulcers Naturally
Symptoms By Type Of Ulcerative Colitis
Ulcerative colitis can be broken into subtypes depending on where the inflammation is in your colon.
- Ulcerative proctitis. Ulcerative proctitis affects your rectum, the part of your colon closest to your anus. Its the most common type and affects 30 to 60 percent of people with ulcerative colitis.
- Proctosigmoiditis. Proctosigmoiditis causes inflammation of your rectum and the lower part of your colon, called the sigmoid colon.
- Left-sided colitis. Left-sided colitis affects your rectum, your sigmoid colon, and the descending part of your colon on the left side of your body.
- Pancolitis.Pancolitis affects your entire colon.
Symptoms typically become worse as inflammation spreads farther along your colon.
| Ulcerative proctitis |
show ulcerative colitis is slightly more prevalent in men, but most studies show no difference.
Symptoms of ulcerative colitis are similar regardless of sex, but unique issues may occur for some people.
Rectovaginal fistulas may develop, which are holes that allow stool to leak from the bowel to the vagina.
Ulcerative colitis may also lead to irregular periods or increased menstrual pain. Women may also be at a higher risk of anemia and osteoporosis, and ulcerative colitis can further increase this risk.
How To Stay Healthy

Keep up with treatment even when you’re in remission. That means you need to take your medicine even if you feel good. See your doctor at least once a year so they can see how things are going. And like everyone else, it’s important to stay active and follow a healthy diet.
Get regular screenings for colon cancer. Your doctor will let you know how often you should get checked. You may need a colonoscopy every 1-3 years. That’s a procedure that helps your doctor look for cancer or cells that might become dangerous. Your chances of recovery go way up when you find and treat colon cancer early.
Show Sources
You May Like: What Causes Mouth Ulcers On Gums
Risk Factors For Covid
The main factor that puts ulcerative colitis patients at risk is the kind of medication they take. Immunosuppressants are medicines that weaken the immune system to reduce disease symptoms. There are different kinds of medications that can treat UC by suppressing the immune system. This means their body may have a weakened defense system that wont be able to fight off infections.
At the start of the pandemic, it wasnt clear if people with ulcerative colitis had an increased risk of getting or dying from COVID-19. However, its now known that different UC treatments affect COVID-19 risk differently.
What Are The Symptoms Of Urinary Retention
- Difficulty starting a urine stream
- Weak flow of urine
- Feel the need to urinate after voiding
- Small amount of leakage
For acute bladder retention, initial treatment will involve catheterization, a small tube inserted into the bladder through the urethra to drain the urine and relieve immediate pain and distention. Long-term treatment will depend on the cause.
You May Like: How Can You Prevent Pressure Ulcers
You May Like: How To Heal Peptic Ulcer
Free Weekly Newsletter + Report On Secrets Of Strong Immunity
When I wrote my first article on this blog in March 2012, I had been on my gut-healing journey with the GAPS Diet healing protocol for one full year, and I had seen great signs of healing. From March 2012 to this April 2013, even more aspects of my health showed improvement I felt certain that all was well on my journey to full recovery.
Ulcerative Colitis Vs Crohns Disease Vs Irritable Bowel
Other gut diseases can have some of the same symptoms.
- Ulcerative colitis affects only your large intestine and its lining.
- Crohnâs disease causes inflammation, but it affects other places in your digestive tract.
- Irritable bowel syndrome has some of the same symptoms as UC, but it doesnât cause inflammation or ulcers. Instead, itâs a problem with the muscles in your intestines.
You May Like: Good Foods To Eat With An Ulcer
Ulcerative Colitis Causes And Risk Factors
Ulcerative colitis happens when your immune system makes a mistake. Normally, it attacks invaders in your body, like the common cold. But when you have UC, your immune system thinks food, good gut bacteria, and the cells that line your colon are the intruders. White blood cells that usually protect you attack the lining of your colon instead. They cause the inflammation and ulcers.
Doctors arenât sure why people get the condition. Your genes may play a role the disease sometimes runs in families. Other things in the world around you may make a difference, too.
Things that can affect your risk of getting ulcerative colitis include:
- Age. Itâs most likely if youâre between 15 and 30 years old or older than 60.
- Ethnicity. The risk is highest in people of Ashkenazi Jewish descent.
- Family history. Your risk could be up to 30% higher if you have a close relative with the condition.
Food and stress donât cause it, but they can trigger a flare of symptoms.
Can Ulcerative Colitis Be Cured
- Ulcerative colitis is not a fatal illness, but it is a lifelong illness.
- Most people with ulcerative colitis continue to lead normal, useful, and productive lives, even though they may need to take medications every day, and occasionally need to be hospitalized.
- Maintenance medication has been shown to decrease flare-ups of ulcerative colitis.
- Surgery may be required in some patients, but it is not required in every patient with ulcerative colitis.
- Routine cancer screening is a must for those who do not undergo surgical removal of the colon.
Learning about ulcerative colitis is the key to living a long and healthy life. Patient and family education will allow a better understanding of the disease and what steps may be taken to control it. Under a doctors direction, medications, lifestyle and diet modification may be able to lengthen the time between symptom relapse.
Read Also: Can You Drink Coffee With Ulcerative Colitis
Complications Of Untreated Ulcerative Colitis
Although ulcerative colitis may not always be a life-threatening condition, it should not be taken lightly. If left untreated, patients may develop severe medical conditions such as colorectal cancer and colonic dysplasia.
Colorectal cancer is a slow-progressing form of cancer and may be difficult to detect until it reaches a critical stage.
Patients with ulcerative colitis should go for regular cancer screenings to detect possible signs of colorectal cancer early.
Some other medical conditions that may develop due to untreated ulcerative colitis are:
- Osteoporosis: A condition that causes bones to weaken, which may happen due to vitamin D deficiencies caused by ulcerative colitis.
- Arthritis: Pain in the joints.
Aside from other medical conditions, when untreated, ulcerative colitis symptoms could flare up without warning, and the frequent diarrhoea may lead to patients becoming dehydrated and developing vitamin deficiencies.
Risks Of Untreated Ulcerative Colitis
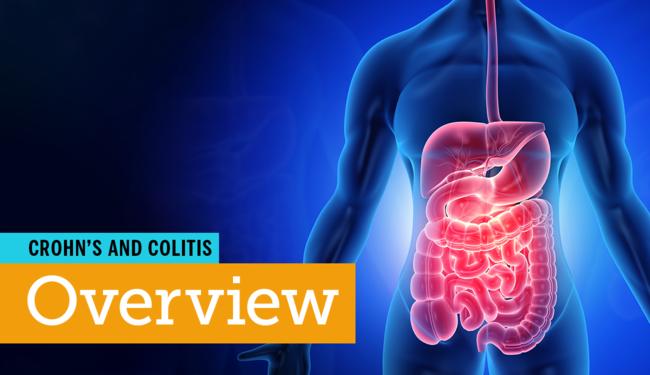
A common issue with UC is ulcers in the colonwhich is where ulcerative colitis gets its name. These are painful sores in the lining of the colon. This is often what causes common UC symptoms like bloody diarrhea and abdominal pain.
If the condition worsens and ulcers become more severe, they may weaken the wall of the colon and develop a connection to other parts of your organs, or create a rupture . Obviously, a hole in any organ is not ideal. A rupture in the colon can allow contents of the intestine to leak into the rest of the abdomen. Even worse, this can lead to a serious infection.
Another risk of untreated ulcerative colitis is fulminant colitis. This is a severe form of UC in which you might experience high fever, stomach pain, and more than 10 bloody bowel movements a day. This is a medical emergency, and you should seek care immediately.
Another emergency complication is called toxic megacolon. As the name suggests, this is when the colon dilates and expands significantly. As a result, the large intestine can no longer function as normal, and you may also have high fever, increased heart rate, abdominal distension, dehydration, and low blood pressure, among other symptoms.
Read Also: Best Treatment For Diabetic Ulcers
Ulcerative Colitis Risk Factors
Most people with UC dont have a family history of the condition. However, about 12 percent of people with UC do have a family member with IBD, according to research from 2014.
UC can develop in a person of any race, but its more common in white people. If youre of Ashkenazi Jewish descent, you have a greater chance of developing the condition than most other groups.
Young people with IBD may also be dealing with acne at the same time. Some older studies have suggested a possible link between the use of the cystic acne medication isotretinoin and UC. However, newer research has yet to find a definitive causal relationship.
Theres no solid evidence indicating that your diet affects whether you develop UC. You may find that certain foods and drinks aggravate your symptoms when you have a flare-up, though.
Practices that may help include:
- drinking small amounts of water throughout the day
- eating smaller meals throughout the day
- limiting your intake of high fiber foods
- avoiding fatty foods
- lowering your intake of milk if youre lactose intolerant
Also, ask a doctor if you should take a multivitamin.
What Are The Risk Factors For Ulcerative Colitis
The exact causes of ulcerative colitis are not understood, but it is thought to be an autoimmune disease. This means the bodys immune system mistakenly attacks harmless bacteria in the colon, thereby inflaming healthy tissue.
Why this happens is unclear, but medical experts suspect a combination of genetics and environmental factors are at play. The disease can occur in all ethnic groups, but whites and people of Eastern European Jewish descent are at highest risk. Oher risk factors include:
- Family history: Having a family member with ulcerative colitis increases the risk of developing the condition.
- Environment: Ulcerative colitis is more common in urban, industrialized areas than it is in undeveloped countries. This suggests that a high-fat and refined-food diet may play a role. It is also more common in northern climates.
- Nonsteroidal anti-inflammatory medications: Medications including ibuprofen , naproxen sodium , diclofenac sodium and others dont cause ulcerative colitis, but they can inflame the bowel and worsen symptoms.
Don’t Miss: Aip Diet For Ulcerative Colitis
How Is Ulcerative Colitis Diagnosed
To diagnose ulcerative colitis in children, teenagers and adults, your healthcare provider has to rule out other illnesses. After a physical exam, your provider may order:
- Blood tests: Your blood can show signs of infection or anemia. Anemia is a low level of iron in your blood. It can mean you have bleeding in the colon or rectum.
- Stool samples: Signs of infection, parasites , and inflammation can show up in your poop.
- Imaging tests: Your healthcare provider may need a picture of your colon and rectum. You may have tests including a magnetic resonance imaging scan or computed tomography scan.
- Endoscopic tests: An endoscope is a thin, flexible tube with a tiny camera. Specialized doctors can slide the endoscope in through the anus to check the health of the rectum and colon. Common endoscopic tests include colonoscopy and sigmoidoscopy.
What Can I Expect If I Have A Diagnosis Of Ulcerative Colitis
Ulcerative colitis is a lifelong condition that can have mild to severe symptoms. For most people, the symptoms come and go. Some people have just one episode and recover. A few others develop a nonstop form that rapidly advances. In up to 30% of people, the disease spreads from the rectum to the colon. When both the rectum and colon are affected, ulcerative symptoms can be worse and happen more often.
You may be able to manage the disease with medications. But surgery to remove your colon and rectum is the only cure. About 30% of people with ulcerative colitis need surgery.
Recommended Reading: Can Ulcerative Colitis Make You Vomit
Determining The Severity Of The Disease
The severity of the disease can be measured objectively by determining symptoms such as:
- The number of stools in a day
- Appetite
- Fever
- The number of days in a month when an individual must modify his or her work, home, or social schedule because of diarrhea, fatigue, fever, and other symptoms
It can also be measured subjectively, through questioning by a doctor of an individuals general state of being, such as whether that person is angry, depressed, in pain, embarrassed by needing to use the toilet frequently in social or business situations.
The severity of the objective signs seen on x-rays does not necessarily correspond to how severe the subjective symptoms are. One individual with disease that looks severe on radiological exam might have the ability to lead a relatively normal life, while another person with few objective signs of disease may find the conditions totally debilitating, both physically and mentally.
You May Like: How To Treat A Diabetic Foot Ulcer On The Sole
Poor Growth And Development
Ulcerative colitis, and some of the treatments for it, can affect growth and delay puberty.
Children and young people with ulcerative colitis should have their height and body weight measured regularly by healthcare professionals.
This should be checked against average measurements for their age.
These checks should be carried out every 3 to 12 months, depending on the persons age, the treatment theyre having and the severity of their symptoms.
If there are problems with your childs growth or development, they may be referred to a paediatrician .
Also Check: How Long Does Ulcerative Colitis Flare Up Last
Ulcerative Colitis And Colorectal Cancer
Ulcerative colitis increases the risk of colorectal cancer. Colorectal cancer often begins as small growths on the inside of the large intestine. The risk of colorectal cancer increases based on:
- the length of time a person has had ulcerative colitis
- how much of the colon is affected by ulcerative colitis
People with ulcerative colitis should have more frequent tests for polyps and colorectal cancer than people at average risk. The gold standard screening test is a colonoscopy. Polyps can be removed during a colonoscopy. This reduces the risk of colorectal cancer. Ask your doctor how often you should be checked for colorectal cancer.
Surgery to remove the entire colon eliminates the risk of colon cancer.
Ulcerative Colitis: Warning Signs To Look For
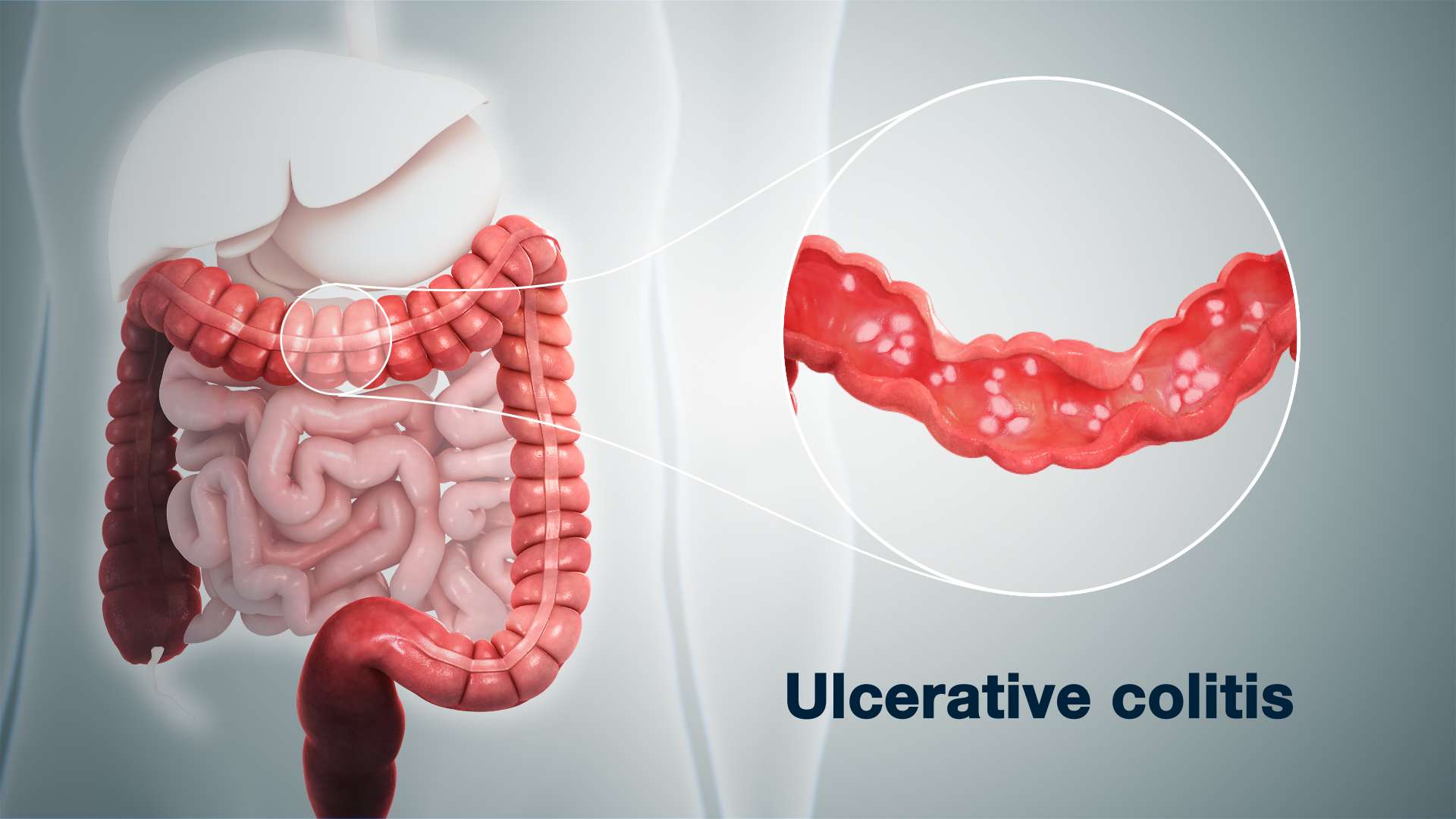
Ulcerative colitis is a type of inflammatory bowel disease that causes chronic inflammation in the digestive tract. This condition typically affects the innermost lining of the colon or the large intestine and rectum. Ulcerative colitis can be mild to severe, but it does put a person at an increased risk of getting colon cancer.1,2
Also Check: Best Ointment For Leg Ulcers
Stanford Scientists Link Ulcerative Colitis To Missing Gut Microbes
Bacteria normally inhabiting healthy peoples intestines and the anti-inflammatory metabolites these bacteria produce are depleted in ulcerative colitis patients, a Stanford study shows.
Aida Habtezion is the senior author of a study that describes how people with ulcerative colitis have insufficient amounts of a metabolite produced by a family of gut-dwelling bacteria.Steve Castillo
About 1 million people in the United States have ulcerative colitis, a serious disease of the colon that has no cure and whose cause is obscure. Now, a study by Stanford University School of Medicine investigators has tied the condition to a missing microbe.
The microbe makes metabolites that help keep the gut healthy.
This study helps us to better understand the disease, said Aida Habtezion, MD, associate professor of gastroenterology and hepatology. We hope it also leads to our being able to treat it with a naturally produced metabolite thats already present in high amounts in a healthy gut.
When the researchers compared two groups of patients one group with ulcerative colitis, the other group with a rare noninflammatory condition who had undergone an identical corrective surgical procedure, they discovered that a particular family of bacteria was depleted in patients with ulcerative colitis. These patients also were deficient in a set of anti-inflammatory substances that the bacteria make, the scientists report.