Combination Treatment With 6
-
Affiliations Laboratory Medicine, Region Jönköping County, Sweden, Department of Medicine, Solna, Karolinska Institutet, Stockholm, Sweden
-
Affiliation Division of Drug Research, Department of Medical and Health Sciences, Linköping University, Linköping, Sweden
-
Affiliations Department of Medicine, Solna, Karolinska Institutet, Stockholm, Sweden, Center for Digestive Diseases, Karolinska University Hospital, Stockholm, Sweden
A Review Of Azathioprine
*Corresponding author: Hasan Nasir, Second year medical student, California North state University College of Medicine, ElkGrove, California, USA.
Received: November 11, 2021 November 24, 2021
DOI: 10.34297/AJBSR.2021.14.002047
Case Report
One of the most significant inflammatory causes of rectalbleeding is Ulcerative colitis . This disease primarily impactsthe colon, typically causing continuous mucosal ulcerations in therectum extending proximally into the large intestine. Althoughbelieved to not be as severe as Crohns disease, Ulcerative colitis hasa slightly greater prevalence in North America. Aside from bloodydiarrhea, symptoms of UC include left lower quadrant abdominalpain before bowel movements, rectal urgency, fever, and weight loss.Extra-intestinal complications such as ocular disease, arthralgias,and primary sclerosing cholangitis contribute significantly to themorbidity of this disease .
References
- Ungaro R, Mehandru S, Allen PB, Peyrin-Biroulet L, Colombel JF, et al. Ulcerative colitis. The Lancet 389: 1756-1770.
Sample Preparation And Lc
DNA was isolated from whole blood collected in EDTA tubes, using previously published methods, and the ratio of dTG relative to dA in DNA was analyzed using a recently developed HPLC-mass spectrometry method. Briefly, chromatographic separation of dTG and dA was with a XSelect HSS T3 3.5 m 4.6 × 100 mm column with a VanGuard 3.5 m 3.9 × 5-guard column maintained at 30°C. Analytes were eluted with mobile phases of 0.01 M aqueous 0.05% formic acid and 0.05% formic acid in acetonitrile . The flow rate was 0.5 mL/minute, and the mobile phase system consisted of a starting condition of 1% buffer B increasing to 3% at 1.1 minutes, 8% at 2.4 minutes, and increasing to a maximum of 30% at 4.1 minutes then decreasing to 5% at 4.5 minutes, maintained until 5.5 minutes then decreasing to 1% for an equilibration period of 2.5 minutes. Standards ranged from 100 g/mL dA and 2000 ng/mL dTG and were serially diluted in water to 0.39 g/mL dA and 3.9 ng/mL dTG, respectively. High , medium and low matrix controls were prepared in triplicate. Standards, matrix controls, and samples were injected in a volume of 50 L for sample injections this is equivalent to 0.2 g patient DNA per injection.
Don’t Miss: Foods Not To Eat With Ulcerative Colitis
Long Term Clinical Efficacy
Thirteen patients have a minimum of one year follow-up. Nine of these thirteen patients have continued on therapy for at least 2 years. Four of these nine have been on both allopurinol and thiopurine therapy for over 40 months. Of the thirteen patients who have been on allopurinol and thiopurine for at least 1 year, nine were initially on steroids and six of these patients continue to be steroid free during their entire follow-up period with only one patient requiring escalation to biologic therapy. All thirteen of these patients continue to be in clinical remission. The mean partial Mayo score was 1.3 ± 0.8, and the mean HBI score was 1.3 ± 0.6 at the last follow-up visit.
Fda Warning: Cancer Risk
- This drug has a black box warning. This is the most serious warning from the Food and Drug Administration . A black box warning alerts doctors and patients about drug effects that may be dangerous.
- Long-term use of azathioprine may increase your risk of developing certain types of cancer, such as lymphoma, leukemia, and skin cancers.
Read Also: How Can Pressure Ulcers Be Prevented
Warnings For People With Certain Health Conditions
For people with thiopurine S-methyltransferase deficiency: TPMT is an enzyme in your body that breaks down azathioprine. When you dont have enough TPMT, youre at increased risk of side effects and blood disorders from azathioprine. Your doctor may do a test to check the levels of TPMT in your body.
For people with low blood cell counts: Azathioprine raises your risk of lowered blood cell counts. Having certain genetic problems can also increase your risk. Your doctor may do blood tests, lower your dosage of azathioprine, or stop your treatment with the medication.
For people with infections: This medication decreases the activity of your immune system. This may make infections that you have even worse.
For people with liver problems: Azathioprine can increase your risk of liver problems, usually in people with kidney transplants. Your doctor will take blood tests to check how well your liver is working. Liver problems usually happen within 6 months of kidney transplant and usually go away when azathioprine is stopped.
Transcriptome Changes As Markers Of Biological Response To Thiopurine Therapy
GO profiling from RNA-seq data for thiopurine-treated patients: biological processes significantly associated with genes underexpressed as a consequence of LDAA therapy sampled data, biological processes significantly associated with underexpressed genes in LDAA-treated patients which were common to all subsampled sets biological processes significantly associated with over-expressed genes in LDAA-treated patients biological processes significantly associated with overexpressed genes which were common to all subsampled sets of LDAA-treated patients in A to D, the BH FDR was set to P< 0.001 for GO categories. E, GO profiling from RNA-seq data for AZA-treated patients, showing biological processes significantly associated with underexpressed genes . No biological processes were significantly associated with increases in gene expression in response to AZA, but only the GO cell compartments cell periphery and plasma membrane, were significantly associated with increases in gene expression in response to AZA and these were common to all subsamples.
The RAC1 GTPase is thought to be a target of thiopurines but was not represented in the lists of genes differentially expressed in response to therapy . Furthermore, GO terms associated with RAC1 function were not included in the lists of GO terms significantly associated with differentially expressed genes.
Also Check: Best Foods To Eat When You Have A Stomach Ulcer
Patient And Therapy Characteristics
In total, 166 LDAA and 118 AZAm patients were included , with a median follow-up of 25 and 27 months, respectively. Collected baseline characteristics were very similar in both cohorts . Primary indication for thiopurines was active disease . All patients were thiopurine-naïve and most patients were immunosuppressant-naïve .
Fig. 1
No malignancies were reported in either cohort and the incidence of pancreatitis was low.
Optimizing Safety And Efficacy
Due to their complex metabolism and genetic polymorphisms in metabolizing enzymes there is a wide inter- and intra-patient variation in the concentrations of active and toxic metabolites. In 9%-25% of patients serious drug toxicity leads to a cessation of therapy and therapeutic efficacy is unachievable in about 15% of patients.
You May Like: What To Eat During Ulcerative Colitis Flare Up
Tioguanine As An Alternative To Aza And Mp
In order to overcome problems of toxicity and delayed action of thiopurines, tioguanine, originally established for treatment of leukemias mainly in children, was investigated for remission induction and maintenance in IBD. It serves as a direct precursor to 6-TGN, the proposed active metabolite of thiopurines. In one group with 37 patients with active CD tioguanine appeared to be effective with acceptable short-term toxicity. 6-TGN levels were far above those documented for classical thiopurines. However, neither toxicity nor efficacy increased. Recent data has shown that hepatotoxicity does not reoccur during tioguanine treatment in most IBD patients who failed conventional thiopurines due to 6-MMP associated hepatotoxicity. Hence, tioguanine appears to be a justifiable alternative in these IBD patients. Another investigation by Dubinsky et al found opposing results and stated that NRH is a common finding in tioguanine treated patients with IBD. As progression or reversibility of NRH remains unknown the authors do not recommend tioguanine therapy for patients with IBD. Tioguanine related hepatotoxicity in the Dubinsky study was surprisingly frequent whereas in other studies this rate is nearly comparable to that of AZA as NRH has been described under therapy with AZA as well . A lower dose of 10-20 mg tioguanine for remission maintenance has been proposed to be safe in the long term. Accordingly, tioguanine should not be abandoned but more surveillance data are needed.
Bone Marrow Suppression Occurs With Azathioprine
The March 1998 meeting of the Medicines Adverse Reactions Committee reviewed a report of an interaction between azathioprine and allopurinol. The patient, who had been taking azathioprine for many years, presented with pancytopenia 2 months after commencing therapy with allopurinol. Recovery followed withdrawal of both medications and transfusion of 2 units of red blood cells. It took the patient about 6 months to feel well again.
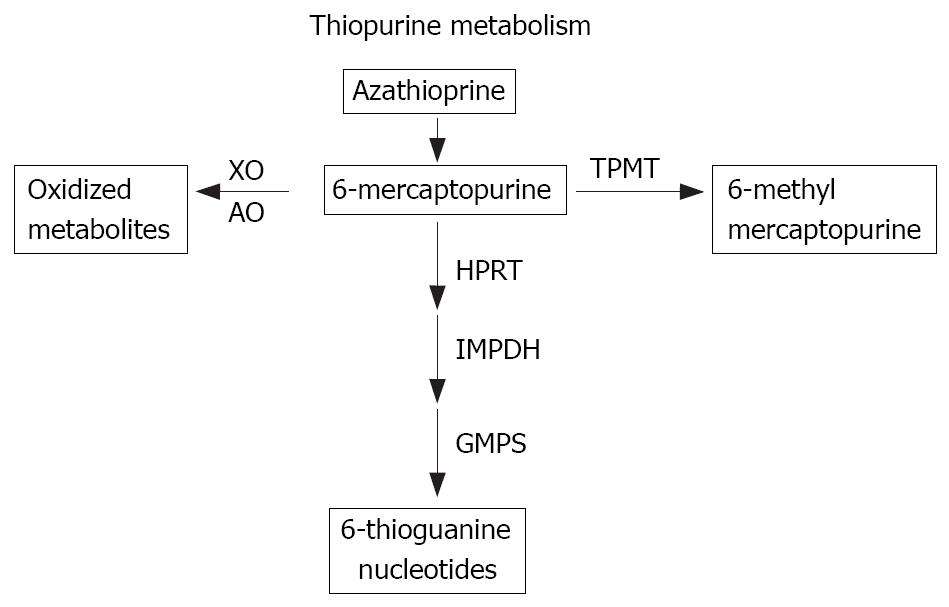
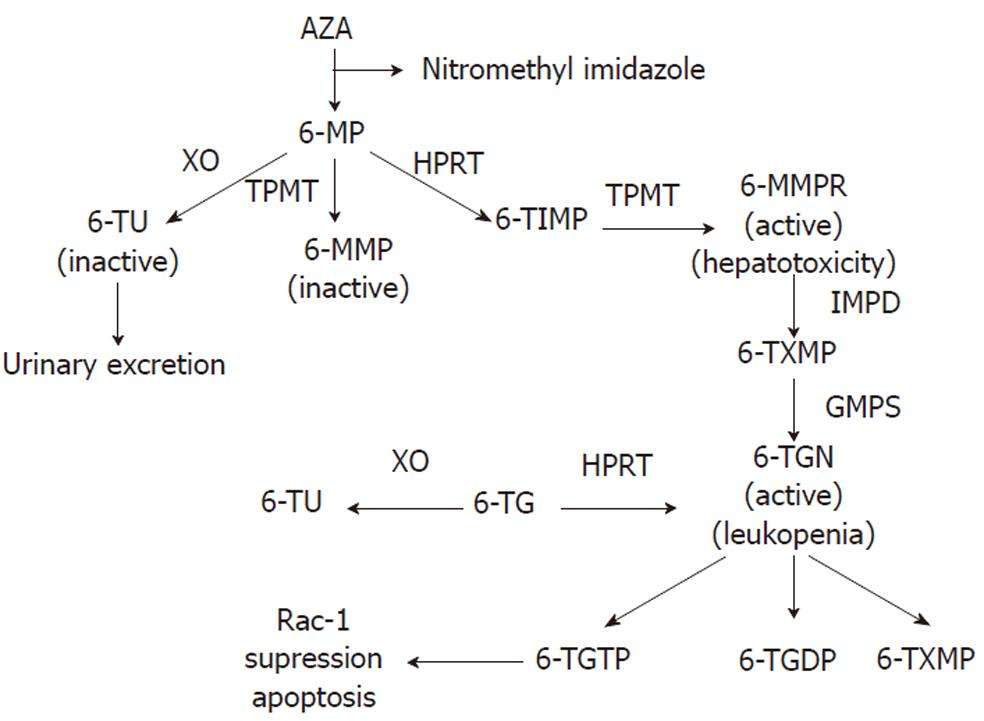
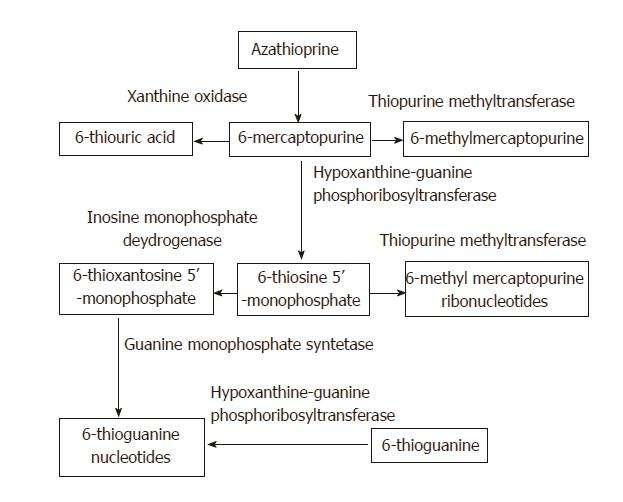
Azathioprine is an immunosuppressive agent. It is first metabolised to 6-mercaptopurine, which in turn is converted to inactive products by xanthine oxidase. Allopurinol inhibits the second step of metabolism, and higher 6-mercaptopurine plasma levels result, with associated toxic effects on the bone marrow and other tissues. The resulting blood dyscrasias, leucopenia, thrombocytopenia or pancytopenia, can be life threatening.
Also Check: Is Ibs And Ulcerative Colitis The Same
Incorporation Of Dtg Into Dna Of Nucleated Blood Cells
Eighteen samples with data on white blood-cell counts were received from newly diagnosed patients with IBD at initiation of treatment with AZA or LDAA these patients were not prescribed additional medication. Twelve weeks after initiation of therapy, there was a significant reduction in neutrophil and white-blood cell counts 3 patients in the AZA group were leukopenic . There was no significant difference in reduction of neutrophil or white-blood cell count between the 2 drug regimens , although dTGDNA for patients in the LDAA group was significantly lower .
Changes in white blood-cell counts , neutrophil counts , and levels of dTGDNA in newly diagnosed patients at 12 weeks after therapy with AZA or LDAA. The data show a significant reduction in mean white-cell and neutrophil counts from 9.3 to 6.6 as a result of therapy with AZA or LDAA , but no significant difference between the AZA or LDAA treatments . However, there were significantly lower dTGDNA levels in the LDAA group . Units: neutrophil and white blood-cell counts × 109/L dTGDNA, moles dTG/106 moles dA.
Probabilities for Kendall Rank Correlations Between Azathioprine Dosea, RBC TGN, RBC MMP and dTGDNA for the AZA and LDAA Drug Treatment Groups
Warnings For Other Groups
For pregnant women: Azathioprine is a category D pregnancy drug. That means two things:
Tell your doctor if youre pregnant or plan to become pregnant. Azathioprine should be used during pregnancy only if the potential benefit justifies the potential risk.
If you become pregnant while taking this drug, call your doctor right away.
For women who are breastfeeding: Azathioprine passes into breast milk and may cause side effects in a child who is breastfed. Breastfeeding isnt recommended while taking this medication.
For seniors: The safety and effectiveness of azathioprine havent been established in people aged 65 years and older.
For children: The safety and effectiveness of azathioprine havent been established in people under the age of 18 years.
All possible dosages and forms may not be included here. Your dose, form, and how often you take it will depend on:
- your age
- how severe your condition is
- other medical conditions you have
- how you react to the first dose
Recommended Reading: Ulcerative Colitis And Back Pain
Regular Blood Tests During Treatment
Taking azathioprine can sometimes affect your liver, kidneys or bone marrow.
You will have blood tests to check your liver function, kidney function and blood count before you start taking this medicine.
From week 1 to week 8 of your treatment you’ll have blood tests every week. This is particularly important if you’re taking a high dose, or you have kidney or liver problems.
From week 9 onwards you will have blood tests less often. Your doctor will decide how often you need them. You may only need them every few months.
It’s important to have ongoing monitoring for as long as you’re taking this medicine.
Use Of Thiopurines In Ulcerative Colitis
Although thiopurines are widely used in the treatment of patients suffering from ulcerative colitis controlled data are limited. If thiopurines have any place in the treatment of UC it is for remission maintenance or steroid-dependence. A recent meta-analysis including 6 studies reported an OR of 2.56 in favour of thiopurines . Moreover, a steroid sparing potential of thiopurines in UC is obvious.
In patients presenting with steroid refractory disease thiopurines play a role as they enhance the beneficial effect of the rescue therapy with cyclosporine. Despite fundamental evidence, thiopurines remain a therapeutic option for UC patients failing 5-ASA monotherapy or requiring multiple steroid courses. One half of the UC patients responding to a first course of corticosteroids will require immunosuppressives mainly because of steroid-dependence. In accordance with the SONIC trial for CD, a similar study was conducted in UC. The results and drawbacks are comparable though the difference between AZA and infliximab monotherapy vanished. Thus, combination treatment was stated to be the most effective with regard to steroid-free remission and mucosal healing at 16 wk.
You May Like: Budesonide Vs Prednisone For Ulcerative Colitis
Metabolite Levels And Liver Enzymes
Within the first month of therapy 6-TGN metabolite levels increased from a mean of 186.5 ± 17.4 to 352.8 ± 37.8 pmol/8 × 10 8 RBC . Over the same period 6-MMP levels decreased from a mean of 11,966 ± 1697 to 2004 ± 536 pmol/8 × 10 8 RBC . Mean AST decreased from 39.6 ± 7.3 to 24.2 ± 1.6 , and mean ALT decreased from 82.0 ± 31.9 to 27.5 ± 4.8 .
How To Cope With Side Effects
What to do about:
- feeling sick â stick to simple meals and do not eat rich or spicy food while you’re taking this medicine. It might help to take azathioprine after you have had a meal or snack.
- headaches â make sure you rest and drink plenty of fluids. Do not drink too much alcohol. Ask a pharmacist to recommend a painkiller.
These side effects are more likely when you first start taking azathioprine or when your dose is increased. You will usually feel better after a week or so.
Talk to your doctor if these side effects do not go away or they get worse.
Don’t Miss: What To Do When You Have A Stomach Ulcer
The Mechanism And Drug Interaction
Summary:
- While not commonly used together for the treatment of various chronic conditions, the concomitant use of allopurinol and azathioprine hasbeen used to improve outcomes in pediatric and adult patients withinflammatory bowel disease, prevention of rejection in organtransplantation, and reducing thiopurine-induced hepatotoxicity. Coadministration of these medications did require dose reductions andextra monitoring for life threatening reductions in WBC.
- Allopurinol inhibits the enzyme xanthine oxidase , which is one of 3 enzymesresponsible for inactivating 6-mercaptopurine . It may also have effects on TPMT activity as one study showed a reduction in methylated metabolites with the combination.
- Due to this inhibition, 6-mercaptopurine isshunted down to form metabolites that are incorporated into theDNA resulting in a reduction in WBC replication/activation, as well asinhibition of the activity of Rac1 GTP which stimulates apoptosis ofWBCs.
- The coadministration of allopurinol and azathioprine can therefore result inlife-threatening reductions in WBCs and should only be done by clinicians with specific expertise.
Editor-in-Chief:
Reviewers: Jon D. Herrington, PharmD, BCPS, BCOP
Expert Contributor: Paul A. Blaker, PhD, MRCP
Last Reviewed: January 2017
What If I Forget To Take A Dose
Check with your doctor or a pharmacist if you miss 2 doses or more.
If you forget to take 1 dose, take it as soon as you remember, unless it’s almost time for the next dose. In this case, skip the missed dose and take the next one at the usual time.
Do not take a double dose to make up for a missed dose.
If you forget doses often, it may help to set an alarm to remind you. You could also ask a pharmacist for advice on other ways to help you remember to take your medicine.
Also Check: Mouth Ulcer On Tongue Remedies
Rbc Metabolites And Relationships With Dtgdna
With respect to the relationships between RBC-TGNs and -MMPs, there was no correlation between RBC-TGN and RBC-MMP for LDAA patients, but the converse was true for AZA. However, there was a significant positive correlation between prescribed azathioprine dose and RBC-MMP levels for LDAA but not for AZA. Conversely, RBC-TGN showed no correlation with thiopurine dose for either AZA or LDAA. Finally, no significant relationship was apparent between dTGDNA and RBC-TGNs or RBC-MMPs for patients on AZA or LDAA .
RBC-TGN levels differed between patients in the 2 drug groups with patients on LDAA having higher median RBC-TGN levels , although the effect was not significant for the ESH data alone . Although median and mean RBC-MMP levels were lower in the LDAA group, this difference was not statistically significant . In contrast to dTGDNA measurements, there was no difference between the early and late time periods of treatment for either RBC metabolite .
Study Population And Sample Collection
Clinical samples were provided from adult IBD patients treated with either AZA or LDAA at 8 centers in the UK . Patients treated with LDAA were from East Surrey Hospital where patients were normally treated with LDAA as a first-line therapy, and without preselection based on RBC metabolites. The numbers of adult patients being treated for IBD comprized 81 with Crohn’s Disease, 57 with ulcerative colitis, 4 with indeterminate colitis, and 3 with microscopic colitis. At all centers, patients treated with AZA were treated according to standard clinical guidelines. Of the 145 patients, 84 were not prescribed other medication the remaining 61 patients were receiving a variety of additional drugs, including mesalamine , infliximab and/or steroids other drugs included statins, antidepressants, and proton pump inhibitors. Data were analyzed only with respect to thiopurine treatment status, using patients treated with LDAA at ESH, and patients treated with AZA across all centers to avoid bias, LDAA/AZA data from ESH were also analyzed separately. As part of routine clinical practice some participating centers requested RBC thiopurine metabolite measurements at the same time as samples were taken for dTGDNA analysis most of the samples with these data were from ESH.
You May Like: Hand Foot And Mouth Ulcers