Who Gets Foot And Toe Ulcers
You’re at higher risk for foot and toe ulcers if you are:
- Native American.
- Male.
- Elderly.
If you have an eye, kidney or heart disease related to diabetes, youre also at a higher risk. About 15% of people with diabetes will get an ulcer, typically on the bottom of their foot. Around 6% of that 15% will have to be hospitalized because of complications.
Youre also at a higher risk of getting foot and toe ulcers if you have any of the following:
- Problems with circulation.
- A foot deformity like a bunion or hammertoe.
- Kidney disease.
- Use alcohol.
Diabetic Foot Pain And Ulcers: Causes And Treatment
Diabetic foot pain is common amongst diabetic patients and can become severe when left untreated. Diabetic foot ulcers are the sores that are usually seen on the foot pad and it occurs in around 15% of the diabetic patients. The risk of lower-extremity amputation is increased once the ulcer develops.
Tips To Prevent Ulcers
Thereâs a lot you can do to lower your chance of having ulcers in the first place:
Keep your blood sugar in check. Good blood sugar control is the single best way to prevent small cuts and sores from becoming ulcers. If you have trouble managing your blood sugar, tell your doctor. They can work with you to make changes to your medication and lifestyle that will keep your blood sugar from getting too high. Even if your blood sugar level is fairly steady, itâs still important to see your doctor regularly. Thatâs especially key if you have neuropathy, because you may not feel damage to your skin and tissue.
Check your skin every day, and pay special attention to your feet. Look for blisters, cuts, cracks, sores, redness, white spots or areas, thick , discoloration, or other changes. Donât rely on pain even feeling more warmth or cold than usual can be a sign that you have an open wound on your skin, and itâs possible that you may feel nothing at all.
Ulcers are most likely to form on the ball of your foot or the bottom of your big toe, so be sure to check your feet every night. If you notice a problem, or you arenât sure if somethingâs normal, call your doctor.
Donât smoke.Smoking damages your blood vessels, decreases blood flow, and slows healing. Those things raise your risk of ulcers and amputation.
Show Sources
Read Also: How Long Does Prednisolone Take To Work For Ulcerative Colitis
Which Ointment Is Best For Diabetic Wound
Hydrogen peroxide is used for very small wounds, but itâs more important to prevent infection when treating diabetic wounds. For a closed incision or wound, you would want to cover the entire surface of the skin with dry non-stick dressing and secure it with adhesive tape.
For an open wound or ulcer, itâs important to cleanse using soap and water as well as to irrigate your wound twice per day in order to maintain a sanitary environment. Wet dressings may be recommended after cleaning which may include sterile gauze/adhesive tapes applied so that the material can absorb any fluids from the surrounding area.
Newer products such as hydrocolloid dressings which are able to create a moist healing environment on surfaces by absorbing wound fluid while protecting the area from infection, dirt, and other external contaminants are available over-the-counter at pharmacies or grocery stores.
If you have a non-healing ulcer after six months of treatment, consult your doctor for further help in promoting wound healing. They may prescribe antibiotics to prevent infections.
Here is a list of supplies required when treating sores on diabetics:
- Hydrogen peroxide
- Cotton balls or cotton swabs
- Gauze pads: regular and compression
- Gauze roll bandages/tubular gauzes
Here are some ways you can avoid getting cuts or sores on your feet.
How To Treat Diabetic Ulcers
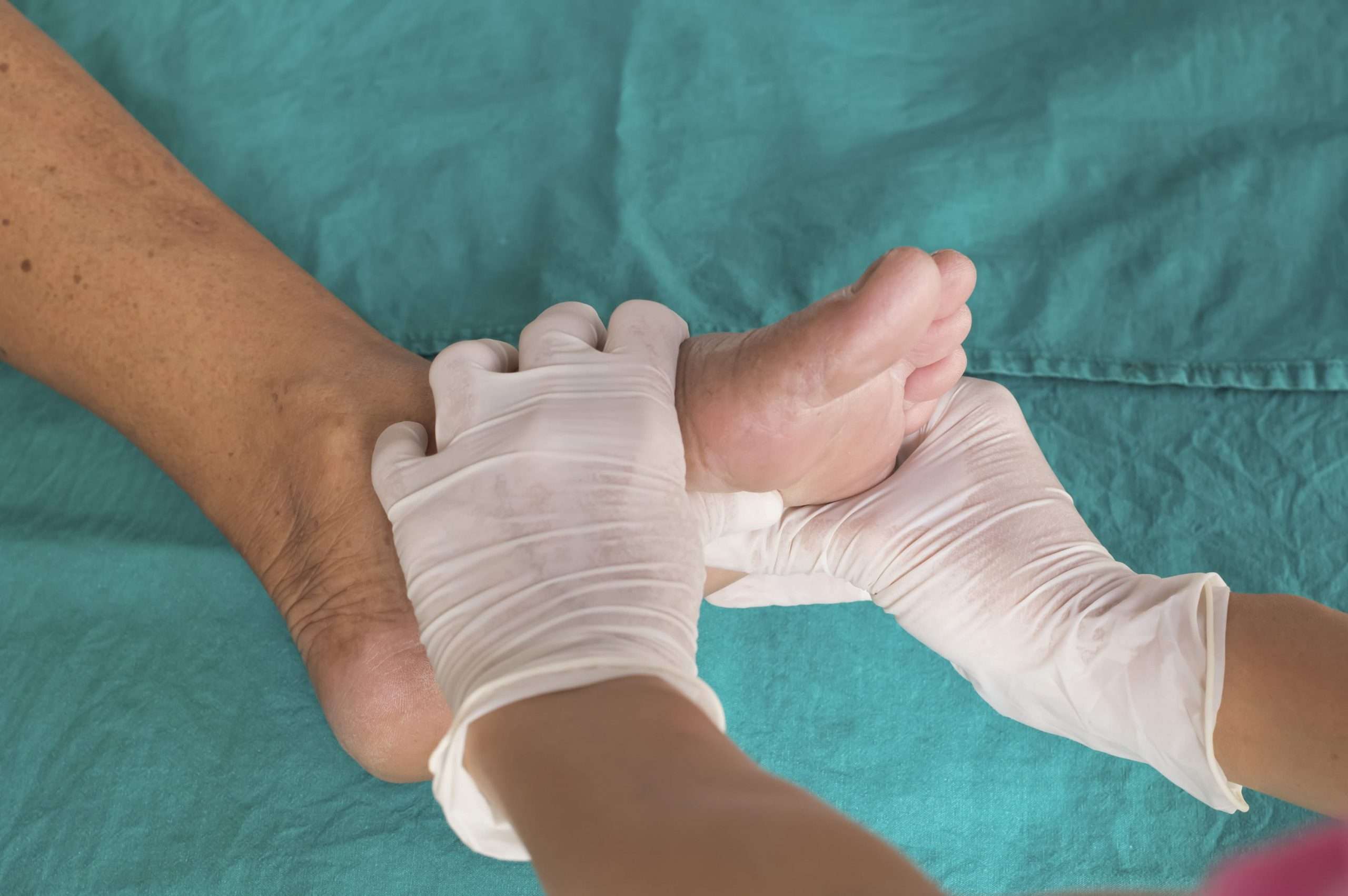
While prevention plays an integral part in managing physical health conditions, diabetic ulcers can occur even if diabetes is properly managed. Treatment options can vary depending on the symptoms and individual but generally consist of medicine or natural ointments.
Diabetic ulcers are generally slow to treat. Taking pressure off the foot is crucial during the healing process. Contact casting or therapeutic boots are often recommended to reduce swelling and irritation from the ulcer. Bandages and other types of wound dressing can usually be found in local pharmacies.
Medications are sometimes used for diabetic ulcers to normalize glucose and heal any potential infection. Hyperbaric oxygen therapy is one method of treatment that can be used as well as surgical debridement. By removing dead tissue, certain diabetic ulcers can be treated by medical professionals.
Natural ointments are also used for certain types of diabetic ulcers. Since homeopathic treatments that reduce inflammation can help with pain reduction, this can be a beneficial treatment for healing while allowing the individual a level of comfort.
You May Like: Why Do We Get Ulcers In Stomach
Advanced Therapies For Diabetic Foot Ulcers
Physicians of individuals with diabetic foot ulcers may have difficult decisions to make if wounds do not heal. Many of these patients have a significant cardiac risk and health care practitioners need to make complicated decisions about whether to perform invasive procedures like angiography. Other options can be:
- Covering the wound with cultured human cells.
- Heterogenetic dressings or grafts with recombinant growth factors.
- Hyperbaric oxygen therapy.
Wet To Dry Dressing Or Simple Saline
This dressing has a good debriding action and helps in wound bed preparation. Wet-to-dry dressings are described in the literature as a means of mechanical debridement. It is very absorptive as well as adherent and one of the cheapest dressings used throughout the world, but requires frequent dressing change based on wound severity. Dressings should be moistened before removal to minimize any chance of bleeding. A gentle cleanser will minimize wound irritation and discomfort. When treating a granulating or epithelizing wound one should soak the dressing thoroughly with normal saline for five minutes to prevent trauma and heavy bleeding.
Also Check: How To Heal Mouth Ulcers Quick
What Causes Foot And Toe Ulcers How Do You Get An Ulcer
There are many possible causes. The most common include:
- Neuropathy from diabetes.
- Peripheral arterial disease.
- Deformed toes.
- Walking in an odd way where you put too much pressure on one part of your foot or toe.
- Friction. Your foot or toe may rub against the toebox of your shoe.
Although they dont cause ulcers, foot and toe ulcers are often found alongside toe deformities such as hammertoe, mallet toe and clawtoe.
Diabetic Foot Ulcer: Treatment And Prevention
Estimates are that by 2030 there will be 550 million individuals with diabetes in the world. Because almost a quarter of all people with diabetes will develop a foot ulcer at some point, health care workers need to know the best practices for diabetic foot ulcer prevention and treatment.
Determining which diabetic foot ulcer type is important to determine an effective treatment. Here are the different types of these wounds:
- Neuropathic ulcers arise when the nerve damage from diabetic neuropathy causes the individual with diabetes to not feel pain from an injury, which often leads to the ulcer progressing substantially before the person is even aware of it. Foot and toe deformities, corns, calluses and areas repetitive stress are likely places of injury. Footwear can not only hide these issues, but can exacerbate the injury if the shoe is ill-fitting.
- Ischemic ulcers or arterial ulcers as they are sometimes called may occur due to lack of blood flow to the extremity. When an ulcer occurs as the result of an injury to the extremity, the lack of blood flow makes these ulcers difficult to heal.
- Neuroischemic ulcers occur in individuals with both neuropathy and poor arterial blood flow and are the most difficult to heal.
- Infected wounds occur in about half of patients with a diabetic foot ulcer and require particularly close care.
Read Also: Signs And Symptoms Of Ulcerative Colitis Flare Up
Diabetic Foot Ulcer Causes
The main cause of diabetic foot ulcer is neuropathy and vascular complications caused due to diabetes. Nerve damage can cause complete loss of feeling in your foot or leg and this condition is generally referred to as peripheral neuropathy. During peripheral neuropathy the pressure caused by cuts, bruises or injury may go unnoticed.
The loss of protective sensation in your body may make you unaware of the fact that you are being injured and may result in skin loss, blisters and ulcers,
Apart from peripheral neuropathy, vascular diseases also increase the risk of ulcer development. Vascular diseases mainly affect the small blood vessels feeding the skin. During this condition your arteries in the feet are unaffected. In few cases the arteries become narrow and no pulse can be found by your doctor in your feet that is a clear indication of ischemia.
Lack of healthy blood flow in your feet may generally lead to ulceration. Due to the presence of vascular diseases, the wound healing ability is also impaired. Vascular diseases are usually aggravated due to excess smoking.
New Wound Therapytopical Pure Oxygenappears Effective In Healing Food Ulcers
Investigators from Midwestern University invited 73 people who had diabetes, both type 1 and 2, to participate in a study to test this new treatment for diabetic foot ulcers.
They found that nearly 42% of those who were randomly assigned to receive the oxygen therapy experienced significant symptom relief, compared to just 13.5% of those who were treated with regular room air for 12 weeks.2
This new food ulcer therapy is called TWO2 for Topical Wound Oxygen home care therapy. The treatment involves placing an inflatable chamber, similar to a large stocking, over the wound, and then an oxygen generator fills the chamber with pure oxygen administered under pressure.2
As a result of the oxygen therapy, Dr. Frykberg says, “it stimulates production of collagen, growth factor, new blood vessels and increased ability to fight infection.”
Oxygen has long been viewed as crucial in the wound-healing process,3-7 the researchers say. For years, hyperbaric oxygen therapy has been studied intensely to heal foot ulcers and prevent amputation. But results remain inconsistent, the researchers say.
However, Dr. Frykberg and his colleagues say that the use of topically administered oxygen therapy has been hampered by studies that weren’t well designed and complicated by results that were inconsistent.8-10
You May Like: How Can I Get Rid Of Mouth Ulcers
Make Sure You Dont Have An Infection:
- This is an area where your podiatrist can work with an infectious disease doctor. If you have any redness around your wound or drainage from the center of your wound, you likely have an infection of the current. In the short term, it is essential to start taking antibiotics and to get antibiotic medication onto this site. This can be life-threatening if allowed to continue for lengthy periods of time without improving.
- If you have redness or drainage developing around your ulcer, dont waste any time, this is the single most urgent thing you can do, dont be someone who loses their leg because they waited one or two days too long.
Insurance Coverage For Pure Oxygen Treatment Is Limited But Expanding

The Food and Drug Administration considers the oxygen delivery product, a class II medical device, to which it granted premarketing clearance in 2009.
The therapy is available now in limited areas of the country but the company is working to gain broader availability, says Mike Griffiths, DProf, CEO and medical director of AOTI Inc. based in Oceanside, California, and Galway, Ireland.
This therapy is now prescribed in Veterans Administration facilities, he says, and ”we have approval for New York State Medicaid reimbursement.” He declined to provide the cost to a patient who doesnt have insurance coverage, but he says the new study results is expected to help the company get broader healthcare coverage from Medicare and other insurers soon.
Don’t Miss: Ulcerative Pancolitis With Rectal Bleeding
How Can I Prevent Or Reduce My Risk Of Foot And Toe Ulcers
It may be possible to reduce your risk of getting ulcers, and even stop them from coming back. Try to:
- Manage your diabetes. If you have diabetes you should wear appropriate footwear and never walk barefoot.
- Every day, examine your legs as well as the tops and bottoms of your feet and the areas between your toes. Look for any blisters, cuts, cracks, scratches or other sores. Also check for redness, increased warmth, ingrown toenails, corns and calluses. Use a mirror to view your leg or foot if necessary, or have a family member look at the area for you. See a healthcare provider immediately if you notice any problems.
- Wear appropriate shoes and socks. Talk to your podiatrist about what you need.
Proper Dressing Infection Control And Offloading
Its essential to use the proper types of wound dressing, infection control, and offloading to prevent your diabetic wound from regressing during or after treatment.
The best wound dressing maintains a healthy amount of moisture on the foot to create a favorable environment for the wound. It must be changed at least once or twice per day, depending on the stage and severity of the ulcer. Wound dressing helps control infection, as do antibiotics.
Offloading is also a very important but often overlooked component of diabetic foot ulcer treatment. When you offload, you remove pressure from your injured foot and give new, healthy cells the opportunity to thrive. Crushes, knee scooters, and wheelchairs all accomplish offloading.
Also Check: Foods You Can Eat With An Ulcer
Know More About Treat Pa
Treat Pa is a healthcare startup that has partnered with reputed clinics and hospitals in 8 major cities ChennaiBangaloreMumbaiCoimbatoreTrichyMaduraiCochin and Trivandrum. We connect patients with the best and the affordable treatment plan based on their requirements.
Treat Pa neither provides any treatment nor has any hospitals or clinics of its own. We are a hospital aggregator that partners with the best hospitals and clinics and provides the list to each patient to carefully compare and select the best out of it based on their needs .
This list is cautiously prepared by Treat Pa. We recommend the hospitals and clinics that only pass our checklist. Based on the patient’s needs, Treat Pa is driven to make sure you have a hassle-free surgical experience that will work within your budget.
We at Treat Pa also provide free concierge services and a post-surgery consultation.
Connect with us to know more about our services and best offers.
What Is The Outlook For People With Diabetic Foot
Diabetic foot ulcers are fairly common in people who have had diabetes for a long time. Even with foot checks and careful blood glucose monitoring, some people with diabetes develop infections.
The outlook depends on factors such as:
- How early the wound was found.
- Presence of infection and how much it spreads.
- Treatment effectiveness.
If the infection cant be controlled and spreads too far, amputation may be necessary.
Recommended Reading: Ulcer In My Stomach Symptoms
What Are Foot And Toe Ulcers
An ulcer is a wound or open sore that is either difficult to heal or keeps returning after it heals. Although there are several possible causes, youre more likely to get an ulcer on your foot or toe if you have diabetes specifically a complication called neuropathy that causes you to lose sensation. A scrape, cut or puncture can develop into an ulcer, but if you cant feel it you might not know its there.
Ulcers can lead to infections, and sometimes infections can lead to the amputation of a toe or foot. About 15% of diabetics will get a foot or toe ulcer. Around 14% to 24% of diabetes patients in the United States need an amputation after they get an ulcer.
Ulcers are sometimes painful, sometimes not. You may also experience:
- Burning.
What Happens If A Diabetic Gets A Cut On Their Foot
A wound is an injury to the skin or other external part of the body that breaks its surface. A wound may be caused by blunt force trauma, a cut from a sharp object, or pressure. Diabetes can increase your risk for wounds because it affects blood circulation and nerve function in your feet. It also makes you more prone to infection than someone without diabetes. If you get a cut on your foot, elevated protein levels will make your cells vulnerable to forming scar tissue which blocks red and white corpuscles called platelets from joining together to form clots during the healing time.
If a diabetic gets a cut on their foot, it can lead to ulceration that may eventually result in amputation of the limb, when not treated correctly. There wound treatment is very important for people with diabetes.
Diabetic wounds are often very difficult to heal. There are a lot of reasons why they may not heal well, but one common cause is that the person has poor diabetes management including high blood glucose levels and poor blood flow in their feet. This means that even if someone cuts themselves or gets an open wound on their foot, itâs harder for them to get better at healing because there is less blood flowing through the area around the cut or wound site.
Also Check: Foam Dressings For Leg Ulcers
How To Treat Ulcers
If you do get an ulcer or notice a change in your skin that youâre not sure about, tell your doctor right away. Youâll likely get a procedure called debridement, which removes unhealthy tissue from the wound to spur healing.
Your doctor will also work with you to try to keep your sore or ulcer from getting infected and becoming bigger. Some of the steps they may recommend include:
Clean your ulcer daily. Use soap and water, unless your doctor recommends another cleanser. Donât use hydrogen peroxide or soak your wound in a bath or whirlpool, because this could reduce healing and may boost your odds of infection.
Keep your ulcer bandaged or covered with a wound dressing. While you may have heard that itâs important to âair outâ wounds, experts now know that not covering a wound actually increases the odds of infection and slows healing.
Keep pressure off your ulcer, especially if itâs on your foot. This may mean you need to use crutches, special footwear, a brace, or other devices. Reducing pressure and irritation helps ulcers heal faster.
Use the topical medications your doctor recommends. These may be saline, growth factors, and/or skin substitutes.
Keep your blood sugar under control. In addition to reducing your risk of ulcers, tight blood sugar control helps your body heal existing ulcers.