Causes Of Charcots Foot
People who cant feel anything in their feet and ankles because of nerve damage are susceptible to Charcots foot. Diabetes is a typical issue for individuals with this condition. Nerve damage may be caused by a variety of factors, however:
- Alcohol or drug abuse
There is no known cause for Charcots foot. However, some factors can aggravate it:
- A sprain or broken bone that doesnt get treatment quickly
- A sore on your foot that doesnt heal
- An infection
- Foot surgery that heals slowly
Diabetic Foot Ulcer Symptoms
Normally a wound or sore on the skin would cause pain. But the same loss of feeling in the feet that often contributes to the development of a diabetic foot ulcer means that theres often no pain associated with the ulcer. This can make it difficult for people to realize that an ulcer is even there in the early stages, when treatment is most effective.
Aside from pain, another sign to look for is discharge or drainage from the wound in the socks. Ulcers that have been present for some time and that have become infected may also cause an unpleasant odor.
Conditions Such As Peripheral Artery Disease Kidney Failure Diabetes High Cholesterol Or High Blood Pressure
Ulcers are an indication that a severe stage of a condition such as peripheral artery disease, kidney failure, diabetes, high cholesterol, or high blood pressure is present. This is because these conditions impair circulation and damage nerves, increasing the risk for developing ulcers. A primary care physician or PAD specialist can offer strategies on managing these conditions medication, healthy diet, exercise, and proper weight management can often significantly decrease the risk for ulcers.vi
Read Also: How To Stop Ulcerative Colitis Pain
What Are The Risk Factors For Pressure Ulcers:
People with fragile skin are at additional risk, as are people whose nutrition is poor. Diabetes is also a significant risk factor for pressure sores on the feet.
One of the reasons pressure sores are so common among the disabled is that many such people have impaired sensation of pressure and touch due to spinal cord injuries. Because of this, they may not be alerted by pain or discomfort to the need to change position.
People who are bedridden for extended periods may lose a great deal of weight, which reduces the cushioning around their bones, making them more susceptible to pressure sores.
Can My Foot Ulcers Be Treated
Yes. Lets take a look at some of the foot ulcer treatments and methods that your doctor may recommend or perform:
- Avoiding putting weight on the ulcerated foot. Your doctor may fit you with a cast, special boot, or surgical shoe that keeps pressure off the area.
- Maintaining blood sugar levels in order to facilitate healing.
- Medical debridement of your injury, which will involve your doctor removing the infected tissue so the healthy tissue below can heal over the wound.
- Keeping the ulcer dry by covering it with appropriate wound dressings. Clean the wounds each day and re-cover them with fresh wound dressings in order to encourage healing of the ulcer.
With proper treatment and if caught early, a diabetic foot ulcer can show massive improvement within a week. If left untreated, and if the ulcer does not heal, it can worsen over time which may lead to amputation of one or more toes or the foot in order to stop the infection and save your life.
Don’t Miss: What To Eat To Help Stomach Ulcers
Types Of Diabetic Foot Ulcers
There are different types of diabetic foot ulcers. Some of them are:
- Neuropathic ulcers: These occur when there is peripheral diabetic neuropathy, but there is no ischemia, caused by peripheral artery disease.
- Ischemic ulcers: These occur when there is peripheral artery disease present, but without the involvement of diabetic peripheral neuropathy.
- Neuroischemic ulcers: These occur when the person has both peripheral neuropathy, as well as ischemia resulting from peripheral artery disease.
Signs & Symptoms Of A Foot Ulcer
A foot ulcer can be shallow or deep. When it starts, it looks like a red crater or dimple on the skin. If it becomes infected, it can develop drainage, pus, or a bad odor.
If you have nerve damage in your feet, then you won’t notice the pain of a small stone, too tight shoes, or the formation of a foot ulcer. As you get older or have a medical condition like diabetes or Raynaud’s phenomenon, it’s best to check your feet regularly for damage and sore spots and consult your doctor.
Venous ulcers – Patients with vein ulcers may complain of swollen, tired, and achy legs. Venous ulcers are not typically very painful unless touched, or unless they are infected.
Arterial ulcers – Patients with arterial disease may complain of tingling, burning, or coldness in the feet or toes. Patients may also experience leg pain when walking, or foot pain when elevating the legs. Ulcers usually occur at the tips of toes or on the sides of the ankles or lower calves. The ulcer may look punched out with a yellow-brown or black color. They are often very painful unless there is nerve damage.
Don’t Miss: Snack Ideas For Ulcerative Colitis
Symptoms Of Foot Ulcer
The black tissue surrounding a severe foot ulcer is the most visible symptom. This occurs as a result of an absence of adequate blood flow to the surrounding area.
The ulcer can cause gangrene, which refers to tissue death as a result of infections. In this situation, there might be a noxious odor, discomfort, and numbness.
Foot ulcers are difficult to detect. You may not exhibit symptoms of the ulcer until it has become infected, despite the fact that you have a painful ulcer.
If you notice any skin discoloration, especially tissue that has turned black, or feel any discomfort in an area that appears callused or irritated, talk with your doctor.
Your doctor will most likely assess your ulcers severity using the Wagner Ulcer Classification System, which ranges from 0 to 5.
- 0: no open lesions may have healed lesion
- 1: superficial ulcer without penetration to deeper layers
- 2: deeper ulcer, reaching tendon, bone, or joint capsule
- 3: deeper tissues involved, with abscess, osteomyelitis, or tendonitis
- 4: gangrene in a portion of forefoot or heel
- 5: extensive gangrenous involvement of the entire foot
Diabetic Foot Ulcer Surgery
Most non-infected foot ulcers dont require surgery. However, if non-surgical treatment fails, surgical management may be necessary.
Surgical care may include shaving or excision of bone and the correction of deformities .
For ischemic ulcers , a vascular surgeon should be consulted.
For difficult ulcers that refuse to heal, more advanced therapies can be considered. Advanced diabetic foot ulcer wound care may involve grafts with recombinant growth factors, stem cell therapy, or hyperbaric oxygen therapy.
In the worst-case scenario, the ulcer can develop gangrene and your doctor may need to amputate the affected area.
You May Like: What Are The Symptoms Of An Ulcer In Your Stomach
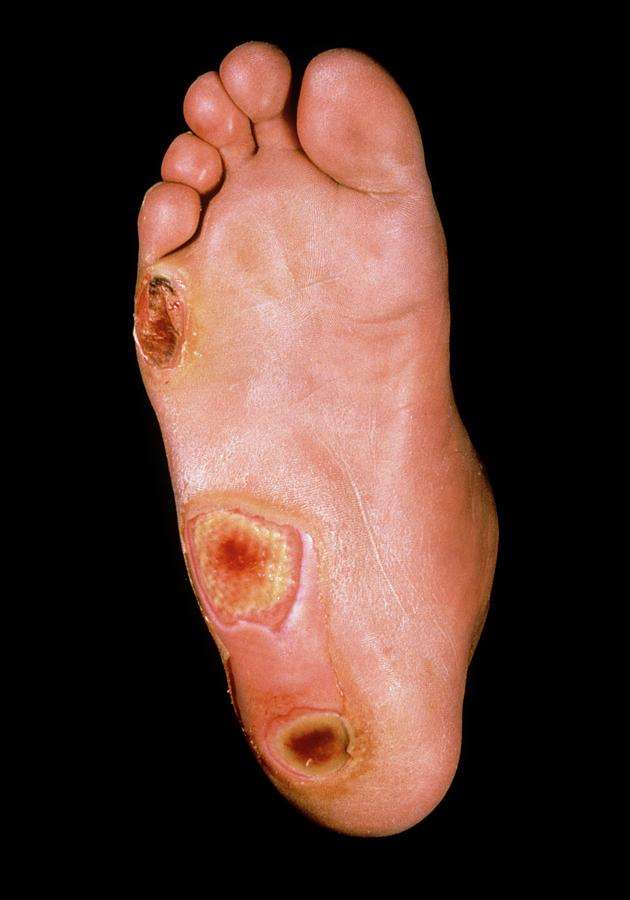
What Are The Symptoms Of Foot Ulcers
Most foot ulcers are located on the side or bottom of the footthe parts of the foot that carry weight when you are walking or standing or on the top or tip of a toe, where the toe can rub against shoes. Foot ulcers may also indicate poor circulation in the extremities, which in turn can be a symptom of diabetes.
These open sores can range from a shallow, red crater that only breaks the surface of the skin, to a deep crater that extends through the skin into the flesh below. In extreme cases, foot ulcers may even involve tendons, bones and other deep structures. The round crater can have a border of thickened, callused skin that develops over time.
Left untreated, foot ulcers can become infected and develop into:
-
An , a pocket in the flesh filled with
-
A spreading infection of the skin and underlying fat, known as
-
A bone infection, known as
- , an area of dead, darkened body tissue
What Are The Symptoms Of Ankle Ulcers
Venous stasis ulcers arent always painful, but they might slightly burn or itch. Theyre usually red, with yellowish skin over them. An infected ulcer may leak yellow or green fluid. Your skin may feel warm or hot to the touch and the area surrounding the ulcer may be swollen and discolored. Your legs may ache, and, depending on how swollen your ankle is, your skin may feel tight and look shiny.
Don’t Miss: Medication For Ulcerative Colitis Flare Up
When To Call A Healthcare Provider
If the ulcer is large or deep, growing in size, incredibly painful, or if you have any signs of infection , you notice a bad smell coming from your ulcer, or you’re running a fever, call your healthcare provider right away.
You’ll also want to call your healthcare provider if your ulcer, no matter how minor, isn’t showing signs healing after a week to 10 days.
In most cases, the ulcer will be dressed to protect the wound. However, if your ulcer is draining considerably, your healthcare provider may recommend leaving the wound uncovered. Dressing the ulcer if it’s draining considerably can impede healing.
If your ulcer is painful, pain medication can be prescribed. Antibiotics may also be prescribed either prophylactically to prevent infection or to treat an already infected wound.
Debridement is done to remove dead tissue from more serious ulcers. For deep ulcers or those that aren’t healing after a long period of time, skin grafts may be needed. In the most severe cases, part of the foot, leg, or other appendage may have to be amputated.
Restoring good circulation is key in treating and preventing ulcers. This includes elevating the legs, wearing compression stockings, reducing pressure on ulcer-prone areas, superficial vein surgery. Leg ulcers, in particular, are incredibly likely to reoccur, so compression stockings are often needed to be worn for life.
Foot Ulcer Prevention Tips
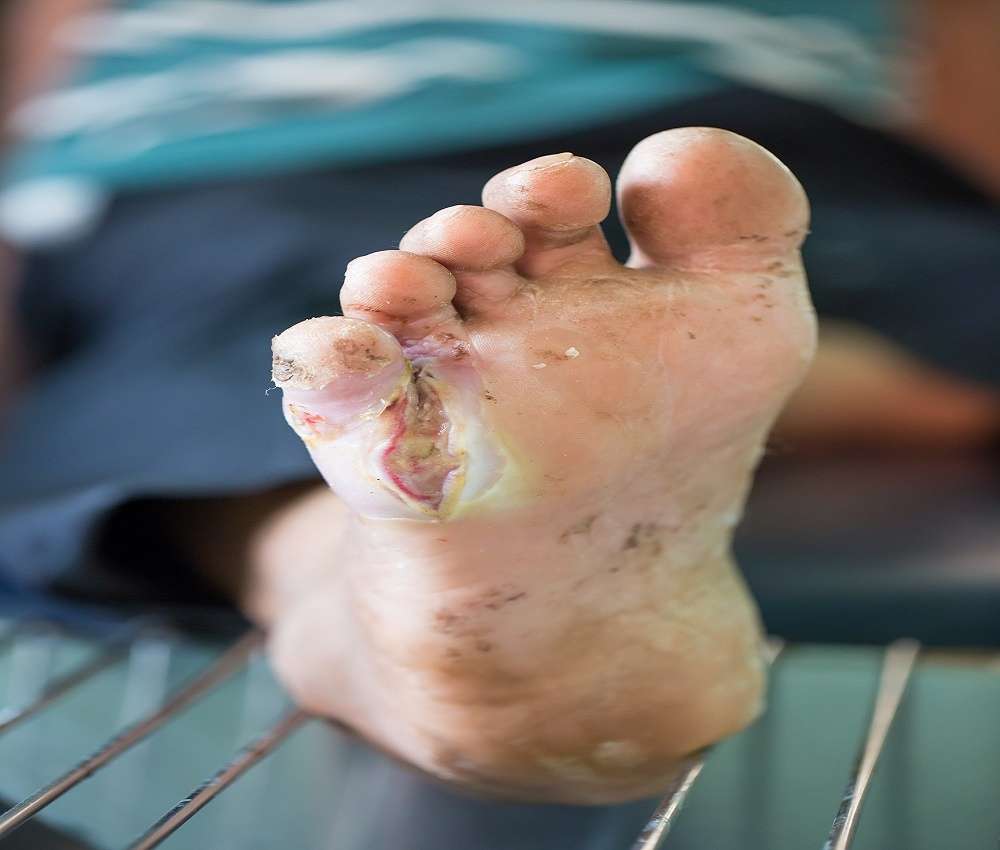
The best way to prevent an ulcer on the foot from forming in the first place is to treat the underlying health problem. In diabetes, keeping blood sugar at normal levels will help prevent some of the complications that can lead to foot ulcers.
Heres what else you can do to keep a step ahead of foot ulcers:
Vlahovic says if you have diabetes, its important to develop a good relationship with a podiatrist. This foot specialist can assess whether you are at higher risk for developing a foot ulcer and give you the regular care you need so that a small problem doesnt turn into a major one.
Recommended Reading: How To Cure Gastritis And Ulcers Naturally
What Are The Different Types Of Foot Ulcer
Neuropathic ulcers : These are commonest cause for lower extremity amputation. Nerve damage results in impaired sensation in the feet. When a person has an injury, blisters, or cracks on the foot, they cannot feel it. The injury may go unnoticed and untreated, leading to an ulcer.
Diabetic foot ulcer is a major complication of Type I & 2 diabetes. In fact it is estimated that one in every six people with diabetes will have a foot ulcer during their lifetime. Foot problems such as ulcerations, infections, and gangrene, are the most common causeofhospitalization among diabetic patients.
Arterial leg ulcers : These approximate 10 percent of all leg ulcers. They are due to insufficient arterial blood supply. They usually do not bleed.
Venous leg ulcers : These are found in people who have varicose veins or blood clots. Damaged valves or blocked veins cause the blood to pool in the vein. Sometimes, the blood leaks out of the vein into the surrounding tissue, causing the tissue to breakdown and form an ulcer.
Diabetic foot ulcers usually occur on the pressure areas of the feet. The bottom of the foot, esp head of the second and fifth metatarsal bones. Diabetic foot ulcers can affect ones quality of life.
Venous ulcers mostly occur above the medial malleoli.
Arterial leg ulcers are usually found on the heels, tips of toes, between the toes or where the bones protrude.
- Check out edge of the ulcer
- Check out presence of granulation tissue
- Check out discharge from the ulcer
What Are The Symptoms Of Pressure Ulcers
Pressure sores on the feet and ankles begin as areas of red, inflamed skin. Over time, the inflammation gets worse, and a blister develops.
This blister eventually becomes an open sore, and if treatment has not been administered before this, it is now a very serious condition. Skin that is this badly compromised is susceptible to infection, which can affect the entire body.
Pressure ulcers are categorized according to their severity:
- Stage I: An area of skin that does not blanch that is, it does not turn white when pressure is applied to it with a finger or other object. Stage I pressure ulcers on the ankles and feet can be harder to detect in this manner in people with darker skin, although the affected skin may appear blue or purple, and there may be sufficient discomfort to motivate the affected person to see a doctor. Regardless of skin color, the skin will be tender to the touch, and may be slightly warmer than the surrounding skin.
- Stage II: The epidermis is severely damaged, and may even be gone. The affected area becomes a blister and then an open sore. Redness and inflammation are apparent on the skin surrounding this blister or sore.
- Stage III: Tissue loss becomes more apparent at this stage. Tendons and muscles are not exposed , but subcutaneous fat may be. The sore has now become a sunken hole this is known as a crater.
- Stage IV: At this stage the sore is much deeper, and there may be damage to muscles, tendons, and even bone.
Also Check: Ways To Prevent Pressure Ulcers In Hospitals
Causes Of The Bottom Of Feet Sores
Contents
There are quite a number of causes resulting in sores under the feet. They can be external or internal foot conditions. The resultant symptoms definitely will be unpleasant to everyone. So accurate diagnosis should be done since if you know the exact cause, then a definition of effective treatment may be quite easy. Explore the following possible causes of sores on the bottom of feet:
What Is A Diabetic Foot Ulcer
A diabetic foot ulcer is an open sore or wound that occurs in approximately 15 percent of patients with diabetes, and is commonly located on the bottom of the foot. Of those who develop a foot ulcer, six percent will be hospitalized due to infection or other ulcer-related complication.
Diabetes is the leading cause of nontraumatic lower extremity amputations in the United States, and approximately 14 to 24 percent of patients with diabetes who develop a foot ulcer have an amputation. Research, however, has shown that the development of a foot ulcer is preventable.
You May Like: Prednisone For Ulcerative Colitis Reviews
Symptoms Of Foot Ulcers
Foot ulcers may look almost like a wound on the flesh of the foot. Key points about ulcer and their appearance:
Summary:
The symptoms of the foot ulcer are different from person to person. If you notice any change of skin color or a wound around the foot, consult the doctor.
How To Spot The Signs Of A Diabetic Ulcer On The Foot
A foot ulcer is one of the most common and serious complications for people with diabetes, occurring in approximately 15% of patients, according to the American Podiatric Medical Association. Diabetic ulcers on the foot can occur in anyone with type 1 and type 2 diabetes and refer to an open sore on the foot, usually forming under big toes and at the bottom of feet. The main reasons people with diabetes develop foot ulcers are:
- Trauma or injury to the foot
- Poorly fitting shoes
- Poor blood flow to the foot
- Increased pressure to the foot
- Nerve damage which means you are unable to feel your feet properly
If you’ve had a diabetic ulcer on the foot for a long time, you are at greater risk of infection, which can spread from the wound to the bone. While there are antibiotics that can treat these infections, if too much bone has been damaged, the foot will have to be removed or amputated.
Therefore patients and caregivers need to be able to identify these types of wounds to prevent them from getting worse. So how do you know if you have a diabetic foot ulcer?
If the ulcer is at an advanced stage, it should be obvious. A foot ulcer looks like a round red crater in the skin bordered by thickened callused skin. Severe ulcers can be deep enough to expose tendons or bones. However, other symptoms may not be easy to identify or could be an indication of another problem. That being said, here are some of the common signs of diabetic foot ulcers to look out for.
Read Also: How Do I Get Rid Of A Stomach Ulcer
Other Tips To Get Rid These Sores
img source: ties.com
Here is more to tips to prevent or treat the bottom of foot sores:
- Protect your foot from harsh weather i.e. cold or hot weather
- Wash your feet daily
- Wear shoes and shocks almost every time if possible
- You are able to examine every part of your feet daily
- You should also not forget good foot hygiene
- In case you suffer corns and calluses, you should consult the doctor for good care
- You should drink plenty amount of water daily to stay hydrated
- Avoid extreme sweating by removing your tight shoes or socks at some points
- You should avoid hot showers, this robs the skin its moisture