When Dining Out With Others
We get ityou may also feel compelled to bring up your UC in social situations when theres eating involved. Here too, let your comfort level be your guide.
Say, for example, someone suggests splitting a dish that you know you cant eat. You have a choice then, Bedell says. You can say something like: Actually, you know what, I haven’t mentioned it yet, but I have some specific dietary needs because of this condition I havemaybe Ill tell you a little bit about it after we order. Or, you can just say you would prefer something else, and deflect until you feel more ready to share.
Moderate To Severe Disease
Patients with moderate to severe colitis should be managed with thiopurines or biological drugs, or both . Thiopurines can be used in patients with steroid-dependent moderate to severe disease to maintain remission. Several small studies129,130 reported the modest efficacy of methotrexate in ulcerative colitis, but results of a clinical trial131 were mixed therefore, its role in ulcerative colitis treatment is still being investigated.
Suggested treatment approach algorithm for moderate to severe ulcerative colitis
Based on Toronto Consensus and European Crohns and Colitis Organisation guidelines.114,118 5-ASA=5-aminosalicylic acid. IV=intravenous. DI=dose intensification.
Anti-TNF- drugs, such as infliximab, adalimumab, and golimumab, are effective at inducing and maintaining remission in moderate to severe disease.132135 Infliximab can also be used in patients admitted to hospital with severe ulcerative colitis and remains the most widely used biological for ulcerative colitis.132,133 Azathioprine alone is less effective than in combination with infliximab to achieve both clinical remission and endoscopic healing, while the difference is statistically significant only for endoscopic healing between azathioprine alone and infliximab monotherapy .136
In My Shoes: 24 Hours With Crohns Or Colitis App
In My Shoes is an immersive experience that allows anyone to find out first-hand what its like to have Colitis.
From low energy levels to managing pain, from rushing to the toilet to juggling work and a social life, the app will allow friends, family and anyone you want, to see first-hand how the condition can affect every part of your body, and every aspect of your life.
We have information for friends and family, employers, and colleagues. Find all our information online.
We have around 50 Local Networks across the UK that bring local people affected by Crohns and Colitis together. They are run by volunteers and host a range of events, from educational talks to socials. Check our website or call our Helpline to find your nearest Local Network.
You May Like: Best Dressing For Stage 2 Pressure Ulcer On Buttocks
Does Ulcerative Colitis Make You Immunocompromised
Ulcerative colitis doesnt make you immunocompromised. Some of the medicines that treat it may change the way your immune system responds. This change is different for each medication. Some of these changes may increase the risk of certain infections or other issues. A discussion with your health care team before starting a medication is the best way to understand these risks and ways to prevent them.
Ulcerative Colitis Questions To Ask Your Doctor
Whether youâre worried your symptoms are UC, or you already have the condition and want more information, here are questions to ask your doctor:
- Are my symptoms a sign of ulcerative colitis or another condition?
- Are there different kinds of UC? Do they have different symptoms?
- What tests will I need?
- If I have ulcerative colitis, what will my treatment plan be?
- Will changing my diet or lifestyle help ease my symptoms?
- How serious is my ulcerative colitis?
- If I take medication for ulcerative colitis, will there be side effects?
- Should I take nutritional supplements like probiotics?
- How often will I need to come in for checkups?
- What should I do if my symptoms suddenly get worse?
- How do I know if my ulcerative colitis is getting worse?
- How do I know if I should change my ulcerative colitis medication?
- Should I consider surgery? What does surgery involve?
- What is my risk of getting colon cancer?
Read Also: What Is The Treatment For Ulcers
Living With Ulcerative Colitis
With careful management, most people with UC are able to enjoy life, including work, travel, recreation, sex and having children.
To keep healthy, consider:
- eating a nutritious diet to help with healing and reduce fatigue
- keeping a food diary to check if there are any foods that make your symptoms worse during a flare-up
- asking your doctor about supplements if you think you may be malnourished
- exercising regularly to lift your mood and help relieve stress
- learning some relaxation techniques to help manage stress
When To Get Medical Advice
You should see a GP as soon as possible if you have symptoms of ulcerative colitis and you have not been diagnosed with the condition.
They can arrange blood or stool sample tests to help determine what may be causing your symptoms.
If necessary, they can refer you to hospital for further tests.
If you have been diagnosed with ulcerative colitis and think you may be having a severe flare-up, contact a GP or your care team for advice.
You may need to be admitted to hospital.
If you cannot contact your GP or care team, call NHS 111 or contact your local out-of-hours service.
Recommended Reading: What Are The Signs Of A Bleeding Stomach Ulcer
Does Ulcerative Colitis Get Worse With Age
While many conditions do get increasingly worse with age, it appears as though new-onset ulcerative colitis diagnosed in older adults is usually milder than when its diagnosed in younger people.
Generally, older adults have more subtle symptoms of ulcerative colitis than their younger counterparts. But this milder presentation could contribute to delays in diagnosing the condition.
Older adults diagnosed with ulcerative colitis are more likely to experience other forms of inflammatory bowel disease and other non-gastrointestinal chronic health problems.
According to one report, it takes older adults about 6 years to get an accurate diagnosis of ulcerative colitis compared to the 2 years it takes younger adults.
Ulcerative Colitis Symptoms You Should Never Ignore
Ulcerative colitis is an autoimmune disease in which the immune system attacks the colon and causes a range of symptoms, both in the GI tract and around the body.
Symptoms of ulcerative colitis, a type of inflammatory bowel disease , can vary widely depending on how much inflammation a person has and where the inflammation is located.
Abdominal pain and bloody diarrhea are the most common warning signs of UC, and can range from mild and intermittent to severe and chronic. The pain of UC is quite common and can significantly impact quality of life. Ulcerative colitis symptoms tend to come and go, often with extended periods of time in between flares. These are called remission periods.
The disease tends to develop gradually over time, so you might not automatically think of ulcerative colitis or IBD if you have occasional abdominal pain or digestive distress.
Ongoing inflammation along with ulcers and abscesses in the intestines are additional common causes of pain. Scarring in the lining of the intestinal tract can lead to painful obstructions. Pain may occur in different areas such as the abdomen or rectal area, depending where the inflammation is located. For example, people may experience moderate to severe pain on the left side of the abdomen if the UC affects the rectum and the lower segment of colon.
UC symptoms might ebb and flow, but they wont go away unless you see a gastroenterologist and start treatment.
Recommended Reading: Meal Replacement Shakes For Ulcerative Colitis
Rectal Bleeding And Discharge
UC often causes bleeding or mucus discharge from your rectum. You may find spots of blood or mucus in your toilet or on your clothing. Your stool may also become very soft and bloody or contain red streaks or mucus. You may also experience pain in your rectal area, as well as a persistent feeling of needing to have a bowel movement.
Also Check: High Calorie Diet For Ulcerative Colitis
Mild To Moderate Disease
First-line therapy in mild to moderate disease is the 5-ASA drugs, which can be administered as suppositories, enemas, or oral formulations . There does not appear to be any difference in efficacy or safety between different 5-ASA formulations.119 Sulfasalazine, which is metabolised to 5-ASA, appears to have similar efficacy to 5-ASA drugs, but tends to be less well tolerated.114 Patients with proctitis should be treated initially with 5-ASA suppositories since they directly target the site of inflammation and appear to be more effective than oral 5-ASA.114,118,120 In left-sided colitis, 5-ASA should be administered as an enema instead of a suppository in order to reach the splenic flexure. For patients with left-sided or extensive disease, it is recommended that oral 5-ASA be used in combination with topical 5-ASA to induce remission.114,118 Oral 5-ASA doses of 2 g or higher per day are more effective than lower doses at inducing and maintaining remission.121123 5-ASA can be started at a dose of 2.02.4 g per day and increased up to 4.8 g, if needed.114,123 Dosing of 5-ASA once a day has similar efficacy to divided doses and could increase adherence.114,123 Patients typically see a response within 14 days, but this response might take up to 8 weeks for symptomatic remission.114 5-ASA drugs have also been shown to be effective at maintaining remission, and patients who achieve remission with 5-ASA should continue on the same medication.114
Also Check: What Foods Can You Eat When You Have An Ulcer
Prognosis For Ulcerative Colitis
Ulcerative colitis is usually chronic, with repeated flare-ups and remissions . In about 10% of people, an initial attack progresses rapidly and results in serious complications. Another 10% of people recover completely after a single attack. The remaining people have some degree of recurring disease.
People who have disease only in their rectum have the best prognosis. Severe complications are unlikely. However, in about 20 to 30% of people, the disease eventually spreads to the large intestine . In people who have proctitis that has not spread, surgery is rarely required, cancer rates are not increased, and life expectancy is normal.
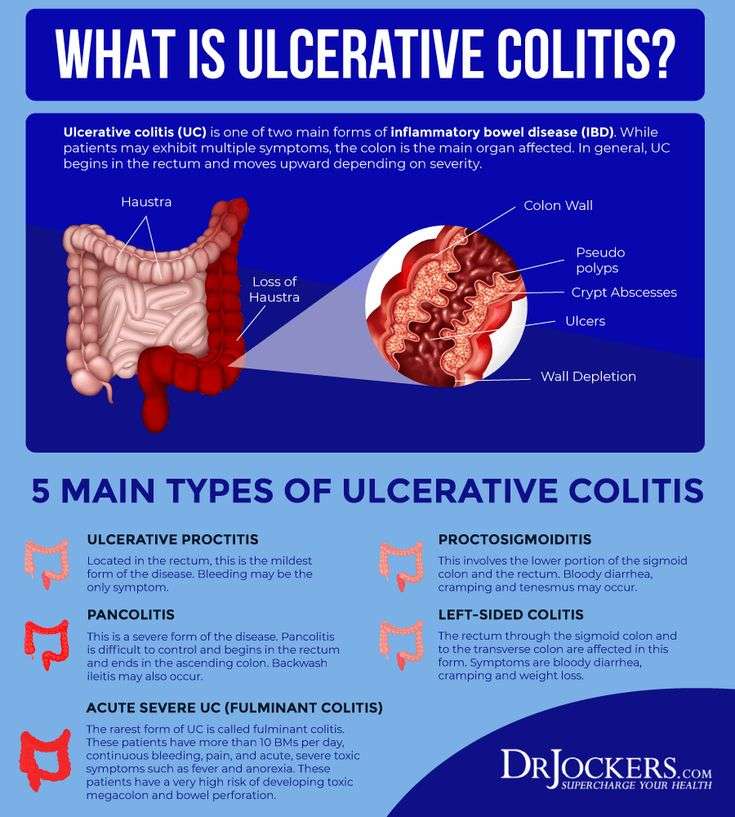
Do Different Types Of Ulcerative Colitis Cause Different Symptoms

Certain symptoms may point to different types of ulcerative colitis. These types, as outlined by the Mayo Clinic, are classified by location within the body:
- Ulcerative proctitis: With this form of the condition, which tends to be the mildest, a person has inflammation in the area closest to the rectum. Rectal bleeding may be the only sign of the disease.
- Proctosigmoiditis: Inflammation with this form of the disease involves a persons rectum and lower end of the colon. Symptoms can include bloody diarrhea, abdominal pain, and an inability to go despite feeling like you need to let loose.
- Left-sided colitis: This involves inflammation from the rectum, through the lower colon, and into the descending colon. In addition to bloody diarrhea and abdominal pain on the left side, you may also experience weight loss. Most patients will have left-sided disease, Dr. Sinha says.
- Pancolitis: This usually impacts a persons entire colon, causing bloody diarrhea that can be severe, abdominal pain, fatigue, and rapid weight loss.
Also Check: How Do You Get Ulcers In Your Colon
Ulcerative Colitis In Children
According to one study of IBD in the United States, 1 in 1,299 children between ages 2 and 17 years old were affected by the condition in 2016. Crohns disease was twice as common as UC, and boys were more likely to have IBD than girls.
For children with IBD, a diagnosis is more likely after 10 years old.
UC symptoms in children are similar to symptoms in older individuals. Children may experience bloody diarrhea, abdominal pain and cramping, and fatigue.
In addition, they may experience issues compounded by the condition, such as:
- anemia due to blood loss
- malnutrition from poor eating
- unexplained weight loss
UC can have a significant effect on a childs life, especially if the condition isnt treated and managed properly. Treatments for children are more limited because of possible complications. For example, medicated enemas are rarely used as a treatment method in children.
However, children with UC may be prescribed medications that reduce inflammation and prevent immune system attacks on the colon. For some children, surgery may be necessary to manage symptoms.
If your child has been diagnosed with UC, its important that you work closely with their doctor to find treatments and lifestyle changes that can help. Check out these tips for parents and children dealing with UC.
Articles On Ulcerative Colitis Overview
Ulcerative colitis affects your colon, which is part of your digestive system. A lot of things can cause trouble in that general area, so how do you know what it feels like to have ulcerative colitis?
It depends on how severe it is, and on what part of your colon is affected.
Also, symptoms can come and go. You might not have any for weeks, months, or even years, and then they come back. Chances are about 50-50 that the effects will be mild.
Still, most people with the disease have a few common issues:
Don’t Miss: Can Ulcerative Colitis Cause Weight Gain
What Are The Types Of Ulcerative Colitis
Sharing With A New Relationship
Tomasino says this is a top question she gets from newly diagnosed patients who are single. Her advice? Share the amount you feel comfortable sharing just as you would with any other personal info when youre dating someone. The degree to which it impacts your life will vary from time to time, she adds, so you may feel its unnecessary to share at one point in time but becomes worth disclosing later on. Heres some guidance on how to navigate it.
Recognize how you are if you take UC out of the equation, Bedell says. If you tend to be open, you might want to tell someone when you first start seeing themor even before when youre chatting on a dating app to just get it over with and weed out anyone who isnt understanding or accepting.
Try this icebreaker: Bedell recommends something straightforward such as, Hey, I have this digestive condition, and this is what the experience is like for me. Again, you dont have to get deep into the details, she says, if a simple explanation will do: This means I have inflammation in my GI tract, which can cause some uncomfortable bathroom-related symptoms and fatigue.
Recommended Reading: Best Mattress For Pressure Ulcers
Is It Important To Treat A Flare Early Or Is It Ok To Wait A Bit
Inflammation typically does not resolve without treatment and early intervention has a better outcome than waiting to treat. At an early stage of a flare, a more optimal baseline treatment is often enough to get the inflammation under control. If you wait, there is a greater risk that you might need drugs with greater side effects, such as oral steroids. By waiting, you will have to manage longer with your symptoms before getting relief. Living with constant or longer periods of inflammation might increase your risk for future complications, as inflammation might cause damage to the gut wall that accumulates in severity with each flare.
If you are experiencing worsening symptoms, you have probably already had the flare for some time without symptoms. Evidence shows that a stool test for inflammation in the colon, called fecal calprotectin, is often elevated for two to three months before any symptoms appear. Your colon might also start to show visual evidence of inflammation before you have symptoms, or at least indicate an increased risk for a flare.
Favorite Orgs For Essential Uc Info
CCF is the leading nonprofit organization dedicated to finding the cure for UC and Crohns. The organization is at the forefront of IBD research and works to educate, empower, and support individuals afflicted with these diseases. Find your local chapter by visiting the CCF website.
This research institute at Virginia Mason in Seattle is one of the few establishments devoted to finding the causes of autoimmune diseases like UC and their cures. Benaroya has already helped advance research in more than 80 diseases of the immune system. The autoimmune life blog provides information on community events and personal stories from patients living with an autoimmune disease.
Recommended Reading: Does Ulcerative Colitis Cause Hair Loss
Learn The Causes Types Symptoms And Treatment Of Ulcerative Colitis
Introduction:
The large intestine becomes irritated and develops ulcers as a result of ulcerative colitis . It is a member of the inflammatory bowel disease subclass of illnesses . It frequently results in diarrhoea that is bloody, urgent, and cramping. These symptoms can occasionally cause someone to wake up in the middle of the night to use the restroom.
The consequences of ulcerative colitis can occasionally be fatal and draining. Although there is no known cure, there are several innovative therapies that can significantly lessen the disease’s signs and symptoms and result in long-lasting remission.
Causes:
It is still unclear what exactly causes ulcerative colitis. Previously, stress and nutrition were suspected. Researchers now understand that while these variables may worsen ulcerative colitis, they do not cause it.
Immune system dysfunction is one potential factor. An abnormal immune response results in the immune system targeting the cells in the digestive tract when it attempts to combat an invading virus or bacteria.
Additionally, it appears that hereditary factors contribute to the higher prevalence of ulcerative colitis in families with affected individuals. However, this family history is uncommon among those who develop ulcerative colitis.
The location of ulcerative colitis is frequently used by medical professionals to categorise it. The symptoms of each kind frequently overlap. The following are types of ulcerative colitis: