Hydrogel Dressings For Treating Pressure Ulcers
Background
Pressure ulcers, also known as bedsores, decubitus ulcers and pressure injuries, are areas of injury to the skin or the underlying tissue, or both. Pressure ulcers can be painful, may become infected, and affect quality of life. Those at risk of pressure ulcers include those with spinal cord injuries and people who are immobile or who have limited mobility such as some elderly people and people with acute or chronic conditions. In 2004 the total annual cost of treating pressure ulcers in the UK was estimated as being GBP 1.4 to 2.1 billion, which was equivalent to 4% of the total NHS expenditure. Pressure ulcers have been shown to increase length of hospital stay and the associated hospital costs. Figures from the USA suggest that ‘pressure ulcer’ was noted as a diagnosis for half a million hospital stays in 2006 for adults, the total hospital costs of these stays was USD 11 billion.
Dressings are one treatment option for pressure ulcers. There are many types of dressings that can be used these can vary considerably in cost. Hydrogel dressings are one type of available dressing. Hydrogel dressings contain a large amount of water that keeps ulcers moist rather than letting them become dry. Moist wounds are thought to heal more quickly than dry wounds. In this study we investigated whether there is any evidence that pressure ulcers treated with hydrogel dressings heal more quickly than those treated with other types of dressings or skin surface treatments.
+ Best Dressing For Stage 2 Pressure Ulcer On Buttocks Png
Read Also
What is the treatment for a pressure ulcer? This video discusses how to assess and provide localized wound care for a pressure injury, and includes a demonstration of how to clean and . Without treatment, they can get worse. Their international classification recognises four categories or stages of pressure ulcer and two categories of unclassifiable pressure injury. In the early stages of bedsores, the area may heal with relief of pressure and by applying care to the affected skin.
Living With Pressure Sores
Living with pressure sores requires a plan to move and turn frequently. Good hygiene will always be required. Pressure sores should be kept covered with a bandage or dressing. Sometimes gauze is used. The gauze must be changed once a day. Newer materials include a see-through film and a hydrocolloid dressing. A hydrocolloid dressing is a bandage made of a gel. It molds to the pressure sore and promotes healing and skin growth. These dressings can stay on for several days at a time.
Dead tissue in the sore can interfere with healing and lead to infection. Dead tissue looks like a scab. To remove dead tissue, rinse the sore every time you change the bandage. Special dressings can help your body dissolve the dead tissue on its own. The dressing must be left in place for several days. Another way to remove dead tissue is to put wet gauze bandages on the sore. Allow them to dry. The dead tissue sticks to the gauze until it is removed. For severe pressure sores, dead tissue must be removed surgically by your doctor.
Removing dead tissue and cleaning the sore can hurt. Your doctor can suggest a pain medicine. Take it 30 to 60 minutes before changing the dressing.
Healthy eating helps sores heal. Make sure youre eating the proper number of calories and protein every day. Nutrients are important too, including vitamin C and zinc. Ask your doctor for advice on a healthy diet. Be sure to tell them if youve lost or gained weight recently.
Also Check: How To Detect A Bleeding Ulcer
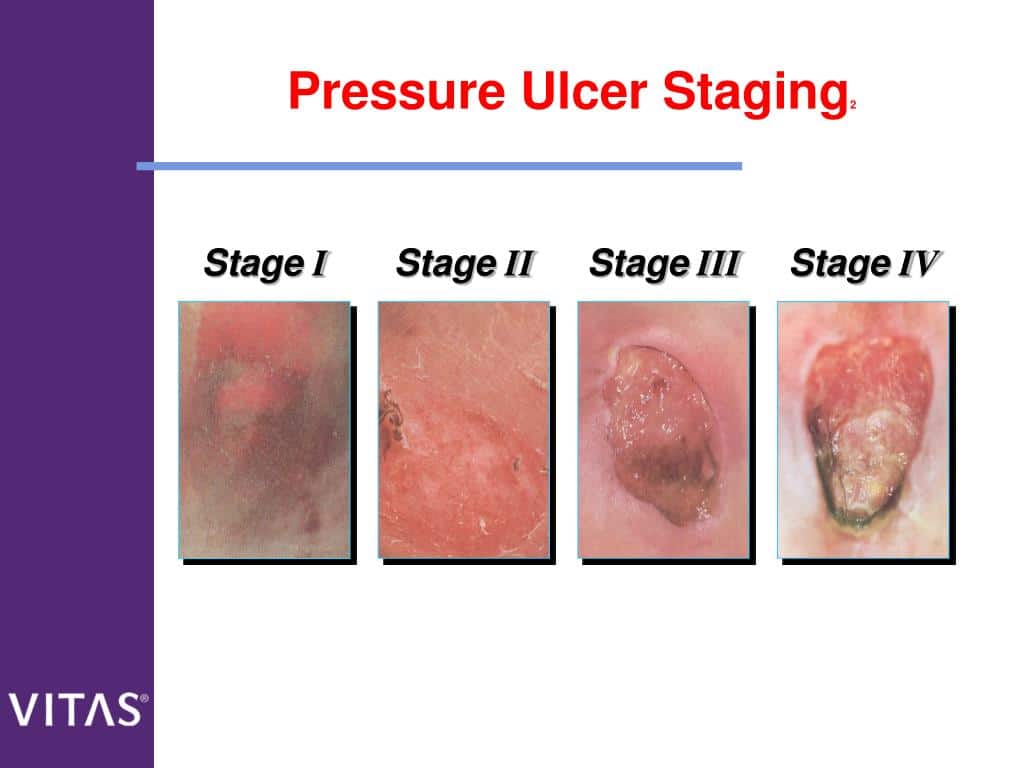
What Are The 4 Stages Of Pressure Ulcers
You might hear medical staff refer to pressure ulcers in stages. Stage 1 is less severe, while an ulcer can progressively increase in severity to stage 4.
The 4 stages of pressure ulcers are:
|
Stage 1 |
The skin is red, but not broken. When you press the skin, it does not turn white. |
|
|
Stage 2 |
There is some damage to the outer layer of skin. The pressure ulcer looks like a shallow, open wound with a redish-pink centre. It can also look like a blister that may or may not have opened. |
|
|
Stage 3 |
There is full loss or damage of the skin. The wound looks quite deep but is still limited to the skin layers. |
|
|
Stage 4 |
There is full loss or damage of the skin it is deep and goes all the way to the underlying bone, tendon or muscle. |
What Complications Might Come With Pressure Ulcers
Pressure ulcers can be painful and become infected, and infection may spread from the skin , to blood , muscle or bone. Treatment may require antibiotics, usually at home but sometimes in hospital. In very rare cases, chronic pressure ulcers can cause skin cancer. It’s important to recognise pressure ulcers early and to act quickly to prevent complications.
Recommended Reading: Ulcerative Colitis And Life Insurance
Pressure Ulcers: Debridement And Dressings
- Charles F von Gunten MD
- Frank Ferris MD
Background Fast Fact #40 discussed the staging and prevention of pressure ulcers this Fast Fact discusses their management. The first step in deciding how to manage pressure ulcers is an assessment of whether the wound is likely to heal. If the patient has a prognosis of months to years, adequate nutrition, and blood flow to the tissue, then healing is possible. If the patient has a prognosis of days to weeks, anorexia/cachexia, and/or the wound has inadequate perfusion, then symptom control alone is appropriate and uncomfortable/burdensome treatments are not appropriate.
Debridement Always provide adequate analgesia! Necrotic tissue must be removed for ulcer healing surgical debridement is the fastest and most effective method when there is healthy surrounding tissue. Note: If the patient is close to dying, and/or the wound will never heal, then debridement should not be attempted. Debridement gels are applied onto an ulcer under an occlusive dressing , are available for ulcers that do not require surgery or when surgical debridement is incomplete. These products come with or without enzymes to encourage autolytic or enzymatic debridement. For minimally necrotic ulcers, occlusive dressings such as DuoDerm, changed weekly, promote autolysis.
References
Appendix 6 Assessment Of Risk Of Bias
1. Was the allocation sequence randomly generated?
Low risk of bias
The investigators describe a random component in the sequence generation process such as: referring to a random number table using a computer randomnumber generator coin tossing shuffling cards or envelopes throwing dice drawing of lots.
High risk of bias
The investigators describe a nonrandom component in the sequence generation process. Usually, the description would involve some systematic, nonrandom approach, for example: sequence generated by odd or even date of birth sequence generated by some rule based on date of admission sequence generated by some rule based on hospital or clinic record number.
Unclear
Insufficient information about the sequence generation process provided to permit a judgement of low or high risk of bias.
2. Was the treatment allocation adequately concealed?
Low risk of bias
Participants and investigators enrolling participants could not foresee assignment because one of the following, or an equivalent method, was used to conceal allocation: central allocation sequentiallynumbered drug containers of identical appearance sequentiallynumbered, opaque, sealed envelopes.
High risk of bias
Unclear
3. Blinding was knowledge of the allocated interventions adequately prevented during the study?
Low risk of bias
Any one of the following.
High risk of bias
Any one of the following.
Unclear
4. Were incomplete outcome data adequately addressed?
Low risk of bias
Unclear
You May Like: What Causes Mouth Ulcers On Gums
Summary Of Main Results
We have successfully conducted a network metaanalysis of dressings and topical agents for healing pressure ulcers. Alongside the analysis we have applied a new method of GRADE assessment , which allows us to view the results in the light of our certainty in their findings. Using this approach, we found the majority of the evidence to be of low or very low certainty, and was mainly downgraded for risk of bias and imprecision . This level of uncertainty within the totality of the dataset impacts on all subsequent interpretation of its outputs.
This review includes 51 RCTs involving a total of 2964 participants, comparing 39 different dressings or topical agents for the healing of pressure ulcers. Most of the studies were in older participants, but four included participants with spinal cord injuries and one was in younger people said to be chronically ill or physically disabled. Seventeen studies included participants mainly with Stage 2 pressure ulcers and 15 mainly had Stage 3 pressure ulcers 13 studies investigated treatment of ulcers with a mean duration of less than three months.
We treated each topical agent as a separate intervention, but initially grouped dressings by class as described in the BNF 2016 . The network involved 39 studies in 2116 participants, encompassing 21 different interventions in 27 direct contrasts and these informed 210 mixed treatment contrasts.
Nursing Home Abuse & Neglect Resources
Common Cases:
Client Reviews
Nursing Home Law Center, LLC is not a law firm. It is an organization that concentrates solely on helping provide nursing home patients and their families the legal help they need. NHLC LLC has a network of recognized attorneys located across the country who have experience representing clients in all types of nursing home injury cases. References to “NHLC attorneys” or “our attorneys” are references to attorneys within NHLC’s network, and not employees, agents, or partners of NHLC. Please consult the disclaimer page for further information concerning NHLC. All information on this site shall be considered ‘attorney advertising’ and not construed as legal advice. Prior case results should not be relied on when retaining a lawyer.
Read Also: Venous Stasis Ulcer Right Lower Leg Icd 10
Bone And Joint Infection
Infection can also spread from a pressure ulcer into underlying joints and bones .
Both of these infections can damage the cartilage, tissue and bone. They may also affect the joints and limbs.
Antibiotics are required to treat bone and joint infections. In the most serious of cases, infected bones and joints may need to be surgically removed.
Posthoc Sensitivity Analysis Dressings Only
For the individual network, we also investigated, posthoc, our original assumption that topical agents could be used in place of dressings, by examining only the network of studies involving two or more dressings . There were no threearm trials remaining and the 30 studies compared 12 interventions in a total of 1627 participants experiencing 641 events, with 16 direct contrasts and 66 mixed treatment contrasts. The NMA rankings were similarly imprecise .
For the group network, 17 studies compared five interventions in a total of 798 participants experiencing 304 events, with five direct contrasts and 10 mixed treatment contrasts. This network was still sparse in terms of total participants, but, on average, there were more events per contrast. The posthoc sensitivity analysis had less overlap of rankograms than the full group network, and the mean rank was closer to a whole number one SUCRA value was 0 and another was 0.9. The mean ranks were: proteasemodulating 1.4 advanced 1.9 basic 3.1 antimicrobial 3.7: advancedantimicrobial 4.9. For the comparisons with basic dressing, effect estimates were similar to those in Table 4 but CIs were still wide.
Recommended Reading: Ulcerative Colitis And Inflammatory Bowel Disease
Potential Biases In The Review Process
This was a sparse network and there may have been smallstudy effects which impacted on the network . The STATA routines have largely been developed for and tested on larger networks, and our work has contributed to modifications for sparse networks in the netweight routine. Other STATA routines can be modified by the user to take into account smallstudy effects, but we did not explore these approaches because there was too much uncertainty in the network for us to be confident of interpreting the results. Instead, we used the standard routines for NMA and adapted the recent approach to GRADE to bring in sparseness when assessing evidence certainty.
A further effect of the sparseness of the network may have been to hide any inconsistencies. The various statistical tests for inconsistency were generally not significant, but this may have been due to a lack of sensitivity of the tests and the wide CIs around the measures. Despite this, we found inconsistencies in the network for contrasts involving phenytoin. We cannot be sure that there are no other inconsistencies, but this may not matter given the already identified large uncertainties.
Summary Of Findings For The Main Comparison

NMA evidence for individual network: proportion with complete healing interventions versus saline gauze
1Majority of evidence at high risk of bias imprecision: very wide CI .2Imprecision: very wide CI .3Majority of evidence at high risk of bias imprecision: wide CI and direct evidence on collagenase from three studies, 11 events .4Majority of evidence at high risk of bias : imprecision: wide CI and direct evidence on dextranomer from one study, seven participants and four events .5Majority of evidence at high risk of bias imprecision: wide CI .6Majority of evidence at high risk of bias inconsistency: heterogeneity in direct evidence imprecision: wide CI .7Majority of evidence at high risk of bias inconsistency: significant difference between direct and indirect estimates imprecision: very wide CI .8Imprecision: wide CI .9Majority of evidence at high risk of bias : imprecision: wide CI and direct evidence on tripeptide copper gel from one study, six participants and five events .
In this section, we present the results for the individual NMA. Results for the group network are given in Appendix 5.
Interventions and comparisons
The individual network comprised 21 interventions: 13 eligible dressings six topical agents and two supplementary linking interventions .
Risk of bias for the individual network
We report risk of bias in three ways :
Network metaanalysis results
Ranking of treatments
Rankograms for each intervention individual network
Also Check: How Do You Get Ulcers In Your Stomach
Spotlight On Aging: Pressure Sores
|
Aging itself does not cause pressure sores. But it causes changes in tissues that make pressure sores more likely to develop. As people age, the outer layers of the skin thin. Many older people have less fat and muscle, which help absorb pressure. The number of blood vessels decreases, and blood vessels rupture more easily. All wounds, including pressure sores, heal more slowly. Certain risk factors make pressure sores more likely to develop in older people: |
Causes that contribute to the development of pressure sores include
Pressure on skin, especially when over or between bony areas, reduces or cuts off blood flow to the skin. If blood flow is cut off for more than a few hours, the skin dies, beginning with its outer layer . The dead skin breaks down and an open sore develops. Most people do not develop pressure sores because they constantly shift position without thinking, even when they are asleep. However, some people cannot move normally and are therefore at greater risk of developing pressure sores. They include people who are paralyzed, comatose, very weak, sedated, or restrained. Paralyzed and comatose people are at particular risk because they also may be unable to move or feel pain .
Friction can lead to or worsen pressure sores. Repeated friction may wear away the top layers of skin. Such skin friction may occur, for example, if people are pulled repeatedly across a bed.
-
Assessment of nutrition status
-
Sometimes blood tests and magnetic resonance imaging
Treatments Your Physician May Prescribe
In addition to self-care, your doctor might prescribe special pads or mattresses. Special dressings may be used, and whirlpool baths or surgery may be recommended to remove dead tissue. Infection requires antibiotic treatment. Sometimes deep wounds may require surgery to restore the tissue. Experimental work is now being done using honey preparations, high-pressure oxygen, and application of chemicals that stimulate cell growth .
Recommended Reading: Can You Drink Ensure With Ulcerative Colitis
Appendix 10 Ranking Interventions
Data for each intervention were shown as the probability that each intervention is the best, second best, third best treatment, etc. . There was substantial overlap of the individual rankograms, illustrated in Figure 21, which intentionally shows the confusion, together with some indication that dextranomer and tripeptide copper gel may be the best treatments and that the worst treatments may be the sequential hydrocolloidalginate dressings and sugar plus egg white. Across all treatments there was considerable uncertainty in the ranking of interventions and no intervention had more than 50% probability of being the best treatment. This, together with the mean rank being no higher than 3.6 and no lower than 18.6 , and no SUCRA value being 0 or 1, reinforces our view of the considerable uncertainty around treatment estimates in this network.
Rankograms combined individual networkKey to interventions: 1: saline gauze 2: alginate dressing 3: sequential hydrocolloid alginate dressings 4: basic wound contact dressing 5: collagenase ointment 6: dextranomer 7: foam dressing 8: hydrocolloid dressing 9: hydrocolloid +/ alginate 10: hydrogel dressing 11: ineligible radiant heat 12: ineligible skin substitute 13: iodinecontaining dressing 14: phenytoin 15: proteasemodulating dressing 16: PVP + zinc oxide17: silicone + foam dressing 18: soft polymer dressing 19: sugar + egg white 20: tripeptide copper gel 21: vapourpermeable dressing
Diet And Lifestyle Changes To Avoid Pressure Sores
Changes to avoid pressure sores include:
- Make sure you eat a healthy and nutritious diet. This includes a balanced diet and fluids/water. And if necessary,youre your doctor about vitamin and nutritional supplements .
- Low body weight or being overweight can cause pressure sores, so make sure you maintain heathy body weight
- If youre malnourished or at risk of malnutrition, protein, fluid and energy intake should be increased.
- Be aware of using good hygiene practices.
- Maintain activity levels, where appropriate.
- Make sure you quit smoking.
You May Like: Can I Donate Blood If I Have Ulcerative Colitis