How Are Crohns Disease Rashes Treated
Skin complications for people with Crohns disease are often improved by treating Crohns flare-ups as they come. One study found that symptoms of erythema nodosum in particular decreased if the underlying IBD condition improved.
Many of these skin conditions respond well to topical or oral steroids. Sweets syndrome, and mild cases of pyoderma gangrenosum are often initially treated with topical or corticosteroids. Mouth ulcers can also be treated with topical steroids.
If skin symptoms do not respond to those medications, adalimumab is often the second treatment of choice. Unfortunately, one of the side effects of Humira is a rash. It was serious enough for one MyCrohnsAndColitisTeam member to switch medications. I have been on Humira for a little over two years now. I recently developed a rash that itches like no other on my hands and feet, which spread to every other part of my body so I am switching my CD meds.
MyCrohnsAndColitisTeam members report a variety of ways of dealing with rashes:
- Baby powder.
- Oatmeal baths help some. Try soothing lotion.
- My dermatologist has me soaking 20 minutes a day in bleach water. 1/2 cup per tub of water.
- I buy Bepanthen in the pharmacy. I tried loads of creams and this one was the only one that worked for me.
- I use mouthwash and Anbesol liquid and take folic acid tablets for mouth sores.
- I take folic acid every day. It helps with the mouth sores and then I also take Valtrex when I get cold sores.
Living With Uc: Diet Changes
Diet doesn’t cause ulcerative colitis, but some foods may make your symptoms worse. Common ones include dairy, fatty foods, and foods with too much fiber, which can trigger diarrhea. It can help to keep a journal of what you eat and any symptoms you have. Look for links and avoid triggers. If you lose a lot of weight, you may need to work with a dietitian to come up with a healthy diet.
Endocrine And Metabolic Disease
Porphyrias
Porphyrias are inherited or acquired disorders of heme biosynthesis and can be erythropoietic, hepatic, or mixed in nature, each associated with a specific enzyme defect in the heme pathway. Porphyria cutanea tarda, the most common porphyria, is a hepatic porphyria with acquired and sporadic forms . It is caused by a deficiency in uroporphyrinogen decarboxylase, leading to the accumulation of uroporphyrin in the urine and serum.
Precipitating factors include alcohol ingestion, estrogen administration, certain hepatotoxins , HIV infection, hemochromatosis, and hepatitis C infection. Manifestations of porphyria cutanea tarda include photosensitivity, skin fragility, bullae and erosions on sun-exposed skin , and hypertrichosis. Biopsy reveals a subepidermal bulla with festooning of the dermal papilla. Direct immunofluorescence reveals IgG and C3 at the dermal-epidermal junction and in vessel walls.
Differential diagnosis includes bullous SLE, epidermolysis bullosa acquisita, pseudoporphyria, and variegate porphyria.
Treatment includes phlebotomy and antimalarial drugs.
Pseudoporphyria
Pseudoporphyria mimics porphyria cutanea tarda without an enzyme defect plasma and urinary porphyrins are normal. Medications are the most common cause of pseudoporphyria. Less common causes are tanning bed use and hemodialysis.
Differential diagnosis is the same as for porphyria cutanea tarda.
Treatment includes removal of the cause.
Recommended Reading: Diet For Someone With Ulcers
Symptoms Of Ulcerative Colitis
The main symptoms of ulcerative colitis are:
- recurring diarrhoea, which may contain blood, mucus or pus
- needing to empty your bowels frequently
You may also experience extreme tiredness , loss of appetite and weight loss.
The severity of the symptoms varies, depending on how much of the rectum and colon is inflamed and how severe the inflammation is.
For some people, the condition has a significant impact on their everyday lives.
Box 1 Common Extraintestinal Manifestations Of Inflammatory Bowel Disease664*
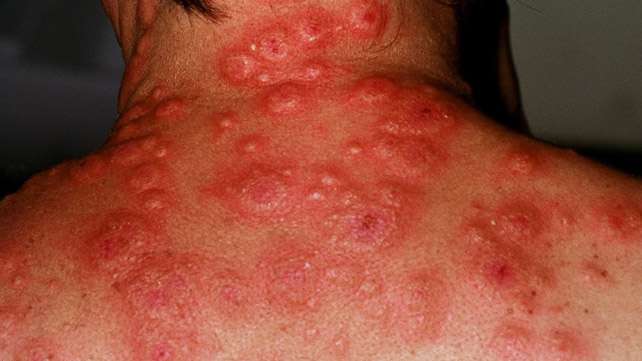
Cutaneous
-
Specific lesions: fissures and fistulas, aphthous stomatitis, mucosal nodularity , pyostomatitis vegetans, metastatic Crohns disease
-
Reactive lesions: erythema nodosum, pyoderma gangrenosum, aphthous stomatitis, vesiculopustular eruptions, necrotising vasculitis, cutaneous polyarteritis nodosa
-
Miscellaneous: epidermolysis bullosa acquisita, vitiligo, psoriasis, secondary amyloidosis, bowel associated dermatosis-arthritis syndrome
-
Cutaneous manifestations secondary to nutritional malabsorption: acrodermatitis enteropathica , scurvy , purpura , pellagra , stomatitis-glossitis-angular cheilitis , non-specific eczema and dry skin , abnormal hair and nails
-
Cutaneous manifestations secondary to treatment: drug eruption, peristomal dermatitis
Musculoskeletal
-
Primary sclerosing cholangitis, autoimmune hepatitis, cirrhosis, fatty liver, hepatic granulomas in Crohns disease
Ocular
Metabolic
-
Growth retardation in children and adolescents, delayed sexual maturation
Patients presenting with IBD should be examined thoroughly for cutaneous manifestations. This article will discuss the epidemiology, pathophysiology, diagnosis, and management of important cutaneous manifestations of IBD.
Read Also: Best Over The Counter Ulcer Medication
What Is Inflammatory Bowel Disease
There are two main forms of inflammatory bowel disease ulcerative colitis and Crohn disease. Both are characterised by abdominal pain and diarrhoea, sometimes with bleeding.
- Ulcerative colitis typically involves only the colon .
- Crohn disease can affect any part of the gastrointestinal tract from the lips to the anus with scattered lesions. Crohn disease is characterised on pathology by non-caseatinggranulomas but these are not always found on bowel biopsy.
Although the two diseases are quite separate, accurate diagnosis can sometimes be difficult especially in the early stages. Therefore the involvement of other organs can help to make the distinction.
What Are Other Common Skin Conditions Linked To Uc
Erythema nodosum is another common skin disorders in patients with inflammatory bowel diseases.1 EN may look like bruises, but they will feel like large raised bumps under the skin.2 They are usually warm to the touch, and very tender or even painful. EN is most commonly found on the legs, but it may occur in other places. Women tend to be more affected by EN than men, but there have been studies that show it happens equally in men and women.1 The treatment for EN is rest, oral corticosteroids, and in severe cases, immunosuppressive agents.3
Don’t Miss: Ulcerative Colitis Prednisone Not Working
Medications For Ulcerative Colitis
Medications can calm the inflammation inside your colon. The first one youâll usually try is from a group called aminosalicylates. If that doesn’t help, your doctor might prescribe a steroid like prednisone. A third option is an immune modifier, which lowers inflammation by changing the activity of your immune system. It can take up to 3 months before you feel the benefits.
Living With Ulcerative Colitis
Dietary Changes from Ulcerative Colitis
There is no scientific correlation between diet and symptoms of ulcerative colitis, therefore, it is also important to ensure that the diet is nutritionally adequate, as ulcers in the intestines may reduce the absorption of essential nutrients, talking to your licensed dietitian and your healthcare team to help you achieve your goals.
Fluid Intake for Ulcerative Colitis
People living with IBD or even IBS will suffer from chronic diarrhea, as diarrhea forces the colon to expel the feces much quicker and decreases the time needed for nutrient absorption, therefore the high water loss in diarrhea can cause dehydration .
It is important to maintain an adequate fluid intake- as humans can only live a couple of days with severe dehydration! Scary! The simplest way to judge whether intake is enough for your body is to look at the volume and color of urine each day. A small amount or if the urine is dark in color can suggest that water intake may not be adequate. A suggested amount of liquid to drink each day is half an ounce per pound of weight. It is important to discuss this with your physician.
However, using the CareClinic Platform, you can track the amount of water you are intaking. Therefore, you can input different kinds of beverages you may be consuming throughout the day. This open discussion with your healthcare team needs to be as transparent as possible.
Supplements and Probiotics for Ulcerative Colitis
Don’t Miss: How To Heal Duodenal Ulcer
Manifestations Secondary To Malnutrition And Malabsorption
Skin manifestations of IBD secondary to malnutrition and/or malabsorption include the acquired form of acrodermatitis enteropathica , pellagra , scurvy , purpura , stomatitis/glossitis/angular cheilitis , xeroderma, or dry skin and unspecified eczema , hair and nail abnormalities . The acquired form of acrodermatitis enteropathica, due to zinc deficiency, is the most common nutritional-deficient cutaneous manifestation of IBD and more common in CD than UC . The skin lesions present as psoriasis involving an erythematous patch and plaque, which may evolve into crusted vesicles, bullae, or pustules. The lesions occur frequently around the mouth, anus, limbs, fingers, and scalp . Adequate supplementation of the deficient nutrients or vitamins is the treatment of choice. For example, acrodermatitis enteropathica is treated with zinc sulfate 220mg/day .
Ulcerative Colitis In Children
Children with ulcerative colitis that is not controlled often grow more slowly than normal, and may end up shorter than they would have. This occurs because when there is active inflammation, appetite is reduced and an insufficient amount of food is eaten. It may be necessary to recommend high calorie diets or even augment the diet with supplements. Children with psycho-social problems because of their disease may need a therapist to help them develop strategies to cope with the disease.
Also Check: In Order To Prevent Pressure Ulcers
Complementary And Alternative Therapies
Diet
Although diet cannot cure ulcerative colitis, some studies suggest that people who eat foods high in saturated fat and sugar, and who eat less amounts of fruits and vegetables, may be at greater risk of developing the disease. Certain foods may also reduce symptoms.
- Limit intake of dairy products, which may help reduce diarrhea.
- Eat fruits and vegetables and pay attention to fiber. Although fiber is crucial to a healthy diet, some people with inflammatory bowel disease find that fiber makes symptoms worse. If fiber bothers you, steam or bake your vegetables instead of eating them raw, and avoid high-fiber foods such as broccoli, cauliflower, and raw apples. Eat antioxidant foods, including fruits and vegetables .
- A bland, low-fiber diet may be best during acute flares.
- Eat 5 to 6 small meals a day.
- Certain foods may aggravate symptoms of ulcerative colitis .
- Avoid refined foods, such as white breads and pastas.
- Avoid caffeine, alcohol, and tobacco.
People with significant malnourishment, severe symptoms, or those awaiting surgery may require parenteral nutrition.
Nutrition and Supplements
Rocky Mountain Spotted Fever

Rocky Mountain spotted fever is the most common rickettsial disease in the United States.16 It is caused by Rickettsia rickettsii, which is transmitted through a tick bite or contact with tick feces or tissue juices.1
The disease occurs most often in young men between April and September.16 In the United States, the areas with the highest prevalence of Rocky Mountain spotted fever are Oklahoma and the southern Atlantic states.6
The prodrome may include malaise, chills, a feverish feeling, anorexia and irritability. The onset of symptoms may be abrupt, with the predominant features being fever , severe headache , generalized myalgia , shaking rigor, photophobia, prostration and nausea. The diagnosis can be difficult when the onset is gradual and no rash is present, as is the case in up to 20 percent of adults and 5 percent of children with Rocky Mountain spotted fever.16
When rash is present, it develops on approximately the fourth day of illness. Its appearance, combined with the temporal evolution, is characteristic of Rocky Mountain spotted fever. The rash typically begins as pink macules, 2 to 6 mm in diameter, located on the wrists, forearms, ankles, palms and soles. Within six to 18 hours, the rash spreads centrally to involve the arms, thighs, trunk and face. In the ensuing one to three days, the lesions evolve into deep-red papules. Within two to four days after onset of the rash, the lesions become petechiae.1,4,7,13,16,17
Don’t Miss: Pressure Ulcer Care At Home
Psoriasis In Patients With Uc
Approximately 5% of UC patients experience psoriasis.3 Some studies have shown that symptoms of psoriasis can occur up to 15 years prior to the symptoms of UC or other inflammatory bowel diseases.1 Psoriasis and UC both appear to be linked in how they affect the immune system, which seems to explain why they are linked.2 Psoriasis causes red, itchy, scaly patches on the skin, which are known as plaques.3 These patches are common on the joints , the scalp and the chest and stomach area, but can occur anywhere on the body. Psoriasis may also cause changes in nail growth. The most common treatments for Psoriasis include topical corticosteroids, topical salicylic acid, systemic immunosuppressive agents, and injectable biological therapies.3
Living With Uc: Supplements
The bleeding caused by ulcerative colitis may lead to iron deficiency anemia due to the loss of the body’s store of iron in the red blood cells that are lost into the colon. Iron supplementation may be necessary. Medications used to treat ulcerative colitis may reduce the absorption of nutrients such as folic acid and calcium. Supplements of vitamins and minerals may be necessary.
You May Like: How To Tell If I Have Stomach Ulcer
Urgent Care For Ulcerative Colitis
During a flare of ulcerative colitis, treatment is important to avoid complications. The most common complication is bleeding that can lead to anemia. With a severe flare, the colon may stop working and dilate . If not successfully treated, the colon may rupture and become a medical emergency. If treatment is not successful, surgery may be necessary. Usually, the entire colon is removed.
Skin Rashes Caused By Ulcerative Colitis
One of the most common symptoms of ulcerative colitis is a skin rash. More than 3,200 members of MyCrohnsandColitisTeam report skin disorders as a symptom.
Several skin conditions are more common in those with inflammatory bowel diseases like ulcerative colitis than in the general population. These include psoriasis and erythema nodosum, as well as less common conditions like pyoderma gangrenosum, Sweets syndrome, aphthous ulcers , angular cheilitis, pyostomatitis vegetans, and leukocytoclastic vasculitis. Vitiligo, which is not a rash but a loss of skin pigmentation, is also associated with ulcerative colitis.
Don’t Miss: How To Treat Ulcerative Colitis Pain
Living With Uc: Probiotics
These “friendly” bacteria are similar to those that live in your intestine and prevent the growth of too many harmful bacteria. We need more research to know if probiotics can help with ulcerative colitis. You can find probiotics in some yogurts, milk, tempeh, and soy beverages. Or you can buy them as supplements.
What Causes A Skin Rash In Ulcerative Colitis
While there are several rashes associated with ulcerative colitis, nearly all have one thing in common. They result from inflammation and problems with the immune system. Psoriasis is a known autoimmune condition. Vitiligo is an inflammatory condition that has been recently genetically linked to an assortment of autoimmune syndromes. Pyoderma gangrenosum is associated with several autoimmune conditions, as well as with skin trauma. Immunodeficiency, a common concern for people living with inflammatory bowel diseases, is associated with an increased risk of canker sores and angular cheilitis.
The cause of Sweets syndrome is currently unknown, but it is thought to be a form of allergic reaction or immune system dysfunction. Besides autoimmune conditions, Sweets syndrome is also associated with certain cancers of the blood that cause immunodeficiency. One review of the literature on inflammatory bowel disease and skin complications found that overactive immune pathways lead to IBD and some other autoimmune conditions.
You May Like: What’s The Signs Of An Ulcer
Ulcerative Colitis Or Crohn’s
Ulcerative colitis symptoms are similar to those of another inflammatory bowel condition called Crohn’s disease. UC only affects your large intestine. But Crohn’s can happen anywhere in your digestive tract. It can cause symptoms from your mouth to your anus. Another disease called irritable bowel syndrome can cause long-term belly pain and diarrhea, but it doesn’t lead to inflammation or sores in your intestines.
Less Common Skin Conditions Linked To Ulcerative Colitis

While these are the most common skin conditions associated with UC, there are some other, less common skin conditions that may occur.
- Vitiligo– While this disease is rare in patients with inflammatory bowel diseases it is more common in UC patients than patients with Crohns disease.2 Patients with vitiligo have white patches on their skin where the pigment is missing. These patches may occur on the face, hands, feet or joint areas. Vitiligo is an autoimmune disease, and like psoriasis, it appears to be linked to UC because it works on the same immune pathways in the body.
- Sweets syndrome– While rare, Sweets Syndrome is more likely to happen in patients with UC than Crohns disease.2,3 Patients with SS experience raised, tender, red or purple patches on their skin, and usually, experience a sudden fever.3 They may also have a headache, and may feel tired, or just generally not well, or not themselves.2 SS is usually treated with oral corticosteroids or immunosuppressive agents.
- Bowel-associated dermatosis-arthritis syndrome – BADAS occurs in patients who have undergone bowel bypass surgery. Patients usually have a fever and experience flu-like symptoms, followed by aches and pains in the smaller joints of the hands and feet, which may become arthritic.3 They may experience eruptions on the skin that start as flat, reddish spots these spots may become raised bumps and may fill with fliud.2 Treatment for BADAS is usually systemic corticosteroids and antibiotics.2,3
Also Check: How To Fix A Stomach Ulcer
When To Get Medical Advice
You should see a GP as soon as possible if you have symptoms of ulcerative colitis and you have not been diagnosed with the condition.
They can arrange blood or stool sample tests to help determine what may be causing your symptoms.
If necessary, they can refer you to hospital for further tests.
If you have been diagnosed with ulcerative colitis and think you may be having a severe flare-up, contact a GP or your care team for advice.
You may need to be admitted to hospital.
If you cannot contact your GP or care team, call NHS 111 or contact your local out-of-hours service.