Risk Factors For Leg Ulcers
- Age peripheral circulation becomes less efficient with old age.
- Varicose veins the one-way valves that stop blood from travelling backwards in the vein stop working. The pooling of blood stretches and distorts the vein.
- Cigarette smoking tobacco is known to constrict the vessels of the circulatory system.
- Arterial disease vein problems are more likely if the person already has other diseases of the arteries.
- Certain disorders these include diabetes and arthritis.
- Pressure sores bed-bound people are at risk of pressure sores, which are areas of damage to the skin caused by constant pressure or friction.
- Medication some cardiovascular medications can contribute to leg oedema and altered circulation.
Can Leg Ulcers Be Prevented
To prevent and promote healing of ulcers:
- Avoid injury, particularly when pushing a supermarket trolley. Consider protective shin splints.
- Walk and exercise for at least an hour a day to keep the calf muscle pump working properly.
- Lose weight if you are overweight.
- Stop smoking.
- Check your feet and legs regularly. Look for cracks, sores or changes in colour. Moisturise after bathing.
- Wear comfortable well-fitting shoes and socks. Avoid socks with a tight garter or cuff. Check the inside of shoes for small stones or rough patches before you put them on.
- If you have to stand for more than a few minutes, try to vary your stance as much as possible.
- When sitting, wriggle your toes, move your feet up and down and take frequent walks.
- Avoid sitting with your legs crossed. Put your feet up on a padded stool to reduce swelling.
- Avoid extremes of temperature such as hot baths or sitting close to a heater. Keep cold feet warm with socks and slippers.
- Consult a chiropodist or podiatrist to remove a callus or hard skin.
- Wear at least Grade 2 support stockings if your doctor has advised these. This is particularly important for the post-thrombotic syndrome, leg swelling or discomfort, and for long-distance flights.
- Have a vascular ultrasound assessment and consult a vascular surgeon to determine whether any vein treatment should be carried out.
- Horse chestnut extract appears to be of benefit for at least some patients with venous disease.
Diagnosis Of Leg Ulcers
- examine the wound
- perform some tests to measure the blood flow in your lower leg, such as the ankle-brachial index. This test compares blood pressure readings taken at the ankle and at the arm using a device called a Doppler machine
- recommend an angiogram for an arterial ulcer, to find out if the artery needs surgery to clear the blockage.
Read Also: What To Eat To Help Stomach Ulcers
What Do The Studies Say
Studies are scarce, with few patients, and most of them do not specify the swabbing technique used. The correlation between the two techniques varies from non-existent to high. It is difficult to compare the results of studies with wounds of different aetiologies ,3 so I will focus on leg wounds. I will highlight the study with the most favourable results for swabbing: No more need for biopsies.4 It included 46 patients with hard-to -heal venous ulcers. All wounds were cleaned with serum but not debrided. When comparing the bacterial species isolated with biopsy and with swab , no significant differences were found. In order of prevalence, the most frequently isolated species in this Danish study were S. Aureus, E. Faecalis and Ps. Aeruginosa. This study also finds that the greater the number of samples collected, regardless of the technique, the greater the probability of finding a greater number of species. This is explained by the polymicrobial environmentof chronic wounds, with a specific distribution of bacteria in the wound. Wound swabs, which may contact a larger area of the wound than the biopsy, might better reflect the microbiological environment of the wound. The authors conclude that the swab is an interesting technique for the microbiological study of infected wounds in our usual clinical practice and, after good cleansing and debridement, the superficial bacterial load corresponds to that in deep tissues.
Can Venous Leg Ulcers Be Prevented
There are several ways to help prevent a venous leg ulcer in people at risk, such as:
- wearing compression stockings
- losing weight if you’re overweight
- exercising regularly
- elevating your leg when possible
This is particularly important if you’ve previously had a leg ulcer once a leg has suffered a venous ulcer, you’re at risk of further ulcers developing within months or years.
Read more about preventing venous leg ulcers.
Read Also: Support Surfaces For Pressure Ulcer Prevention
Iodine And Silver Preparations:
Several new formulations of older topical agents should be considered to treat nonhealing wounds with or without evidence of clinical infection . Iodine, while toxic in high concentrations to tissue in vitro, can be beneficial at low doses. Cadexomer iodine releases low levels slowly into wounds and has been shown to be safe and effective at decreasing bacterial burden in the superficial compartment. Cadexomer iodine is available as an ointment and as an impregnated gauze dressing.
Silver preparations have been used on ulcers for many years. Nanocrystalline silver can deliver topical concentrations to the superficial compartment that are effective against a range of organisms, including yeast., Use of iodine and silver-containing preparations is summarized in .
Cleveland Clinic Heart Vascular & Thoracic Institute Vascular Medicine Specialists And Surgeons
Choosing a doctor to treat your vascular disease depends on where you are in your diagnosis and treatment. The following Heart, Vascular & Thoracic Institute Sections and Departments treat patients with all types of vascular disease, including blood clotting disorders:
Section of Vascular Medicine: for evaluation, medical management or interventional procedures to treat vascular disease. In addition, the Non-Invasive Laboratory includes state-of-the art computerized imaging equipment to assist in diagnosing vascular disease, without added discomfort to the patient. Call Vascular Medicine Appointments, toll-free 800-223-2273, extension 44420 or request an appointment online.
Department of Vascular Surgery: surgery evaluation for surgical treatment of vascular disease, including aorta, peripheral artery, and venous disease. Call Vascular Surgery Appointments, toll-free 800-223-2273, extension 44508 or request an appointment online.
You may also use our MyConsult second opinion consultation using the Internet.
The Heart, Vascular & Thoracic Institute also has specialized centers and clinics to treat certain populations of patients:
Recommended Reading: Ulcers In Small Bowel Crohn’s
The Registry Of Ulcer Treatment
For the past 25years, healthcare professionals in Blekinge have been focused on quality improvement and clinical research within the field of wound management., This tradition of research linked to clinical practice led to the establishment of the Blekinge Wound Healing Centre in 2003. This is a general practitioner -led, primary care-based specialist centre covering the treatment and follow-up of the majority of ulcer patients across the county . It offers a structured team management of ulcer care with an emphasis on diagnosis, documentation and treatment. The GP in charge of the centre is the first author of this study .
The experience of our daily practice combined with research results, soon made it obvious that there was a need for a structured programme for wound management to guarantee optimal treatment. RUT was started in Blekinge County by RFÖ, the registry manager, who then developed the registry further and launched it nationwide.
RUT was the first national registry in primary care. It is web-based and the participating units use the registry as a checklist for ulcer assessment and a base for quality improvement in their units.
To capture the situation of patients with pressure ulcers, during the study period, the pressure ulcer section of the registry was further developed. To improve our coverage of community units , we have established cooperation with another Swedish national quality registry on pressure ulcer prevention.
Infection Status Of Chronic Wounds
The interaction between ulcer and bacteria can be stratified into four levels: contamination, colonization, critical colonization and infection. Whilst, contamination and colonization by microbes are not believed to inhibit healing, the line between colonization and infection can be difficult to define. The term critical colonization has been used to describe the stage at which bacteria begin to adversely affect wound healing. Moreover, the underlying pathogenesis of chronic wounds may result in wounds of different aetiologies being differently affected by bacteria.,,
A range of clinical criteria have been used to define infection in chronic wounds. The Consensus Development Conference on Diabetic Foot Wound Care agreed that a DFU should be considered infected when there are purulent secretions or the presence of two or more signs of inflammation . Guidelines for the management of chronic venous leg ulcers produced by the British Association of Dermatologists and the Royal College of Physicians, recommend that infection should be considered if one of the following is present: pyrexia, increased pain, increasing erythema of surrounding skin, lymphangitis or rapid increase in ulcer size. It is accepted that chronic wounds by their very nature may not always display the classic symptoms of infection and it has been suggested that an expanded list, including signs specific to secondary wounds be employed to identify infection.
Also Check: Ulcerative Colitis And Lung Disease
Guide To The Causes Of Leg Ulcers
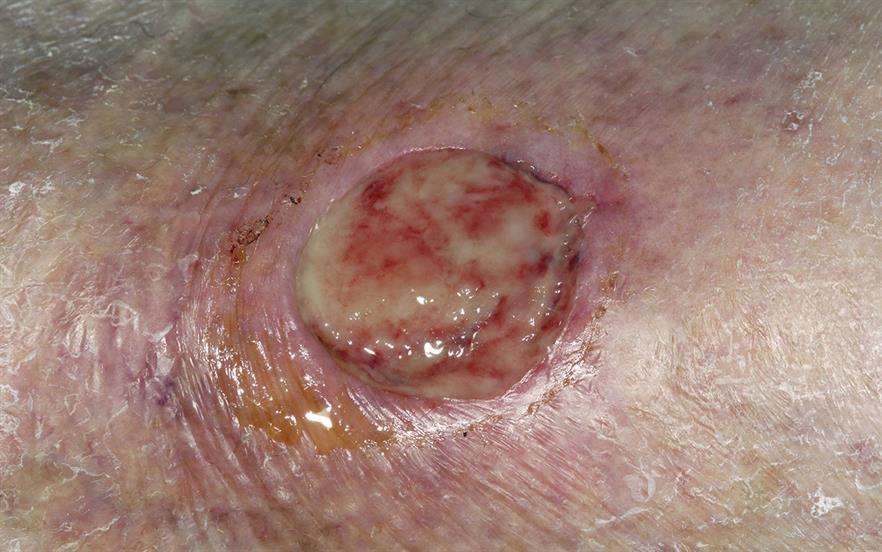
A leg ulcer an open wound or sore that develops on an individual’s leg. Symptoms include pus at the ulcer site, increasing wound size, enlarged veins, pain at the ulcer site, heaviness in the legs, and swelling in the legs. Medical history, physical examination, CT scan, MRI scan, vascular ultrasound, and x-rays may be used to diagnose leg ulcers. The main concern when it comes to leg ulcers is the risk of developing an infection in the wound that progresses to a life-threatening blood infection.
Thankfully, there are many leg ulcer treatment options out there. Patients may need compression bandages to treat their ulcers. Leg ulcer medication includes antibiotics for infections as well as medication for circulation, topical ointments, and pain medication. Leg ulcer wound care should also include natural treatments and home remedies for leg ulcers, such as diet changes and braces or orthotics. Overall, the best leg ulcer treatment can vary based on the underlying cause. Get to know the common causes now.
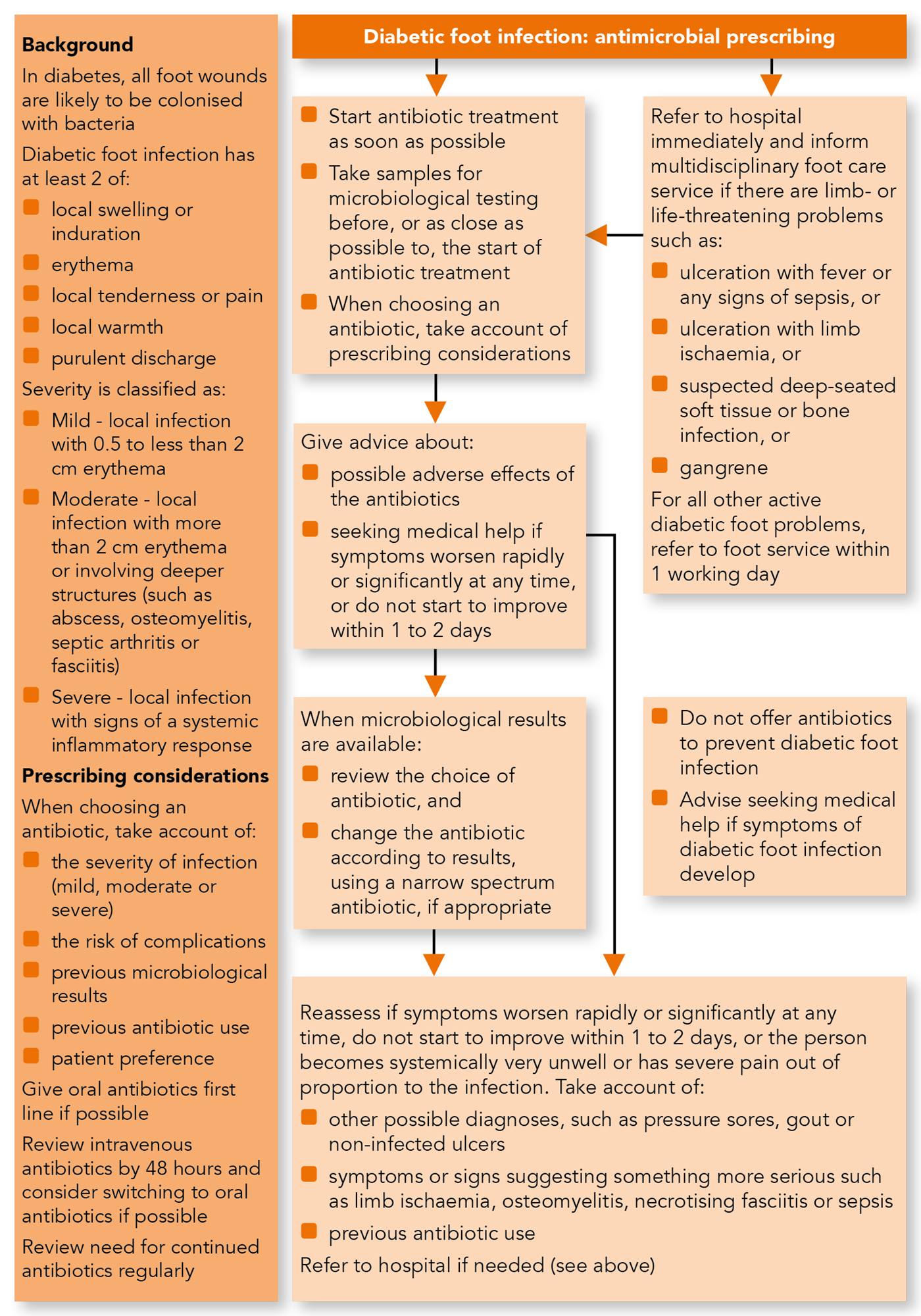
Guideline: Prescribing For Leg Ulcers
13 August 2020
The guideline
NICE has released guidelines with advice on antimicrobial prescribing for leg ulcers. It sets out a strategy for optimising antibiotic use and reducing unnecessary prescriptions, pointing out that while most leg ulcers will be colonised by bacteria, few become clinically infected.
Key points on prescribing for GPs
Dont take a sample from a leg ulcer for microbiological testing at first presentation.
Only offer antibiotics if there are signs of infection, including redness or swelling extending beyond the ulcer, localised warmth, increased pain or fever.
Offer antibiotics based on the severity of symptoms, the risk of the patient developing complications and previous antibiotic use.
When prescribing for an infected ulcer, advise the patient to seek help if their symptoms worsen or do not improve over the next two or three days.
Prescribe oral flucloxacillin 500mg-1g, four times a day for seven days as first line.
If there is penicillin allergy, prescribe oral doxycycline 200mg on the first day, then 100mg once a day for the next six days.
Prescribe oral co-amoxiclav 500/125mg, three times a day for seven days as second line.
Reassess an infected leg ulcer if there is no improvement after two or three days or if the patient becomes systemically unwell or has severe pain.
Practical issues
Where to find it
Also Check: Can Diverticulitis Cause Ulcerative Colitis
Do Not Take A Swab Or Use Antibiotics For The Management Of A Leg Ulcer Without Clinical Infection
Lower leg ulcers, most commonly venous ulcers are often treated with oral antibiotics, even in the absence of evidence of clinical infection. There is no evidence to support this use, except if screening for carriage of multi-resistant organisms. Also a swab for microscopy and culture, in the absence of signs of infection is not recommended. Unnecessary antibiotics and swabbing will add to healthcare costs, antimicrobial resistance and patient allergy.
Supporting evidence
- OMeara S, Al-Kurdi D, Olugun Y, Antibiotics and antiseptics for Venus ulcers. Cochrane Database Systematic Review 2014 CD003557.
- Hansson C, Hoborn J, Moller A, Swanbeck G. The microbial flora in venous leg ulcers without clinical signs of infection. Repeated culture using a validated standardised microbiological technique. Acta Dermato Venereologica 1995 75:24.
An initial list of 10 low value interventions was compiled by the Lead Fellow of the Australasian Society for Infectious Diseases Inc following an online discussion in ASID’s discussion forum, Ozbug. The Royal Australasian College of Physicians then facilitated a consultation of all ASID members via a survey distributed through the societys e-newsletter. In the survey, members were asked to rank the 10 suggested interventions and suggest additional items for consideration. A subsequent shortlist of items was created by selecting the top 7 interventions as ranked by the members from the initial list.
Looking After Yourself During Treatment
The following advice may help your ulcer heal more quickly.
- Try to keep active by walking regularly. Sitting and standing still without elevating your legs can make venous leg ulcers and swelling worse.
- Whenever you’re sitting or lying down, keep your affected leg elevated.
- Regularly exercise your legs by moving your feet up and down, and rotating them at the ankles. This can help encourage better circulation.
- If you’re overweight, try to reduce your weight with a healthy diet and regular exercise.
- Stop smoking and moderate your alcohol consumption. This can help the ulcer heal faster.
- Be careful not to injure your affected leg, and wear comfortable, well-fitting footwear.
You may also find it helpful to attend a local healthy leg club, such as those provided by the Lindsay Leg Club Foundation, for support and advice.
Don’t Miss: Carbohydrate Diet For Ulcerative Colitis
What Are The Symptoms Of Leg Ulcers
The main symptom of a leg ulcer is a deep sore on the leg. You might also have:
- bad-smelling fluid weeping from the wound
- bleeding
- injury to the leg
- an infection
Older people are more at risk of developing a leg ulcer. You are also more at risk if you have diabetes or high blood pressure, if you are obese, or if you are a smoker.
What Is The Treatment For Leg Ulcers
Where possible, treatment aims to reverse the factors that have caused the ulcer. As an ulcer is often the result of both arterial and venous disease, careful assessment is needed first.
Venous leg ulcer, in the absence of arterial disease, is usually treated with exercise, elevation at rest, and compression. Compression must not be used if there is significant arterial disease, as it will aggravate an inadequate blood supply. Surgery, ultrasound-guided sclerotherapy or endovascular laser treatment of superficial and perforator leg veins may also help, particularly if the deep venous system is intact. Venous-return assisted calf compression devices may be of additional benefit.
A vascular surgeon should also assess patients with arterial leg ulcers as they may require surgery to relieve the narrowing of the arteries. Revascularisation is particularly important if the ABPI is less than 0.5.
It is also very important to treat underlying diseases such as diabetes and to stop smoking.
You May Like: How Can Ulcers Be Treated
Prevention Of Ulcer Recurrence
Factors that are associated with ulcer nonhealing and recurrence: Overweight body mass index, history of deep venous thrombosis, large ulcer area, noncompliance with compression therapy, and triple-system venous disease involving superficial, perforating, and deep veins . The strategies to prevent the ulcer recurrence should target these factors. These could be implemented as regular clinical evaluations, patient education and life-long compression therapies. Patient’s education should be regarding skin care, elevation of the affected limb when immobile, compliance to compression therapy, encourage mobility, and exercise. To encourage, early self-referral at signs of possible skin breach.
Compression therapy
Use of compression stockings reduces ulcer recurrence and is thus highly recommended in patients of venous leg ulcers. Patients are encouraged to wear the strongest compression they can tolerate for life-long, if not contraindicated otherwise .
How The Intervention Might Work
For millennia healers have applied various compounds to infected wounds, some of which are still in use today. Use of a topical application has many potential advantages compared with giving systemic antibiotic therapy, including: a high and sustained concentration of the antimicrobial agent at the site of infection the need to use only a limited amount of the antimicrobial at the selected site avoidance of potential toxicity associated with systemic treatment ability to use novel agents not available for systemic use easy application in the outpatient setting and potentially better patient adherence to treatment. Topical treatments may also prove helpful in addressing the globally increasing problem of multidrugresistant organisms that are now untreatable with most systemic agents. For example, a study of 47 organisms from burn wounds that were multidrugresistant to systemic antibiotics were susceptible to 11 commonly used topical antibiotics and antiseptics, although the rates of resistance were higher than in nonmultidrugresistant organisms .
Recommended Reading: What Are The Symptoms Of An Ulcer In Your Stomach
What Are Leg Ulcers
Leg ulcers, sometimes called venous leg ulcers, are deep sores in the skin or membranes of the leg that often take a long time to heal. Unlike a graze, which only affects the first few layers of skin, an ulcer means the whole thickness of skin is lost. They are very common, especially among older people. It is important to see a doctor if you think you have a leg ulcer.
Ulcers can take a long time to heal sometimes weeks or months usually because there is poor circulation to the leg. When they do heal, they always leave a scar. Unfortunately, leg ulcers often come back.
Leg ulcers are the most common wounds in Australia. About 1 or 2 people in every 100 will develop a leg ulcer at some time in their lives.