What Causes Ibs Vs Ibd
Although some patients may show microscopic areas of inflammation in IBS, the causes are speculative and may include hyperreactivity to bacterial gut infections, accelerated or delayed transit of contents through the GI tract , and abnormal bowel contractions caused by triggers such as foods or stress.
The exact cause of IBD is not known. Researchers suggest the IBD types are caused by an immune system malfunction in the bowel tissue, with a genetic predisposition to develop IBD, and the individuals response to gut microorganisms.
What Is The Prognosis For People Who Have Inflammatory Bowel Disease
IBD is a lifelong condition, but it shouldnt shorten your life expectancy. With proper treatment, you can prevent flares and have long periods of remission.
Managing a lifelong condition like IBD can be challenging. Its not unusual for people with IBD to become anxious or depressed. Seeing a mental health counselor can help.
What Causes Ulcerative Colitis And Who Gets It
Docs still cant pinpoint the precise cause of the disease, but its thought the following may contribute to ulcerative colitis:
- genetics
- the gut microbiome
- other environmental factors
Research also suggests that it could be the result of an interaction between infections in the colon and the bods immune response. Basically, experts think the inflammation response is prolonged in patients with ulcerative colitis, which is what causes all those achy, breaky ulcers.
Though anyone can get ulcerative colitis, most people are diagnosed in their mid-30s. These people are also more likely to get it:
- older men
- those with first-degree relatives with the disease
Don’t Miss: How Do You Heal An Ulcer
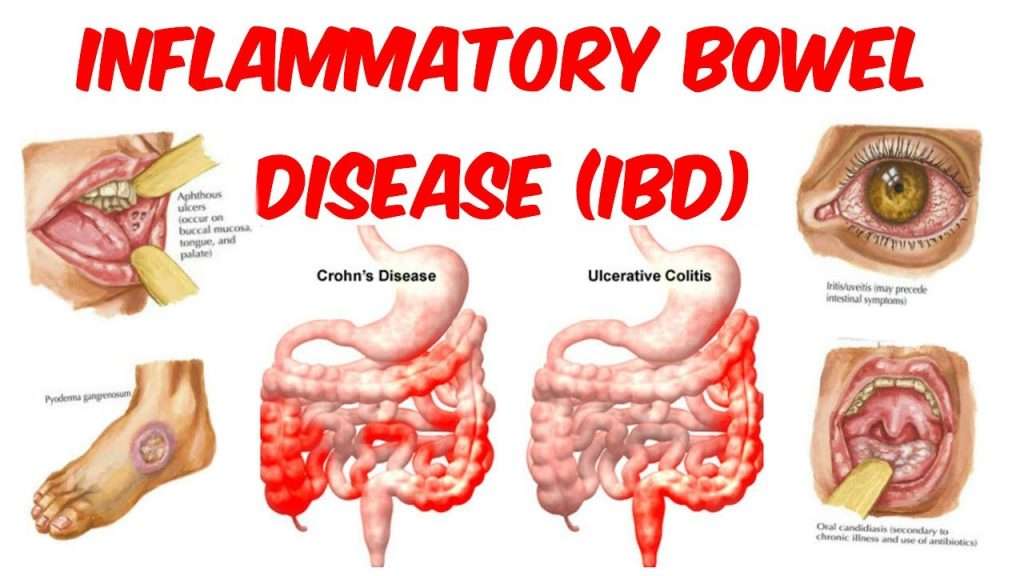
Symptoms Outside Of The Gi Tract
In IBD, inflammation may occur beyond the gut in the skin, joints, and eyes for examples. The resulting dermatitis, arthritis, and iritis can be as debilitating as the IBD itself. None of these physical disabilities result from IBS, and having IBS does not predispose one to IBD, nor any other structural condition such as cancer, celiac disease, nor diverticulosis. While neither condition will shorten life expectancy, most of those with IBD will require surgery at some time during their illness.
Sometimes psychological disease is thought to be a part of IBS. Certainly, some patients who seek medical attention may also have psychosocial problems that require attention in their own right. However, there is little evidence that this is true of IBS overall, and psychosocial difficulties are found in some people with IBD as well. While many people with IBS complain of social inconvenience, embarrassment, fear of appearing in public, and work loss, these features are more universal and profound in IBD, as the foregoing comparisons imply. While IBD is described as a structural or organic disease, IBS is said to be functional or a disorder of function. None of these terms is entirely satisfactory.
Psychological Therapies In Uc
In addition to antidepressants, psychological therapies have also been shown to be beneficial in IBS. These include cognitive behavioral therapy and gut-directed hypnotherapy, and both are recommended by national guidelines for the management of IBS., However, evidence for their use as an effective treatment for UC, particularly in those with IBS-type symptoms, is lacking. A Cochrane review investigated the efficacy of psychotherapy, patient education, and relaxation techniques for IBD. Outcomes assessed included health-related quality of life, coping, emotional status, and disease activity. In total, 21 studies were included, but there was no clear benefit identified for any of the psychological interventions in adults with UC for any of the outcomes of interest.
Another systematic review of 16 studies of psychological interventions, including stress management, psychodynamically informed therapy, CBT, and hypnosis assessed their effects on anxiety and depression, quality of life, and IBD activity. CBT and psychodynamically informed therapy were beneficial for anxiety and depression, but they appeared to have no effect on disease activity, whereas hypnotherapy, used in two studies, demonstrated a beneficial effect on disease activity, but not anxiety, depression, or quality of life.
You May Like: Aloe Juice For Ulcerative Colitis
Is There A Connection Between Ibs And Colitis
Colitis is defined as inflammation in the large intestine. It can be caused by many things, including:
- Infection
- Autoimmune disease
- Lack of blood supply
- Diverticulosis
- Other serious conditions
Colitis can result in symptoms that are similar to those of irritable bowel syndrome . This raises the question: Is there an overlap or connection between IBS and colitis?
Can Ibd Or Ibs Be Prevented What Is The Prognosis
Inflammatory bowel disease treatment and prognosis
The cause of inflammatory bowel disease is unknown. Researchers believe it is the result of an autoimmune reaction. There is a hereditary connection to IBD, and it can be passed down through your family. You cannot prevent IBD, but it may be possible to reduce the risk of developing it by eating a healthy diet, exercising regularly, and not smoking.
The prognosis for inflammatory bowel disease varies widely with the severity of the disease. The course of IBD includes periods with no symptoms with occasional flare-ups. Many patients are able to manage symptoms effectively with little impact on their daily lives. Some patients may need surgery such as a partial or total colectomy to help them manage the disease. IBD also increases a persons risk for developing colon cancer. Serious complications of IBD include ulcers, fistulas, bowel obstructions, and malnutrition.
Irritable bowel syndrome treatment and prognosis
You cannot prevent irritable bowel syndrome, but you can reduce the symptoms by paying close attention to your diet and the foods that trigger them, along with lifestyle changes, for example, not smoking and getting regular exercise.
The prognosis for IBS depends on the frequency and severity of your symptoms and well they are managed. Changes in diet, probiotics, medications, and other therapies can have an impact on how well do with IBS.
Don’t Miss: How To Heal Leg Ulcers Quickly
Patients And Control Subjects
Between May 2007 to February 2013 all patients with UC who underwent a surveillance colonoscopy at the endoscopy unit at Umeå University hospital were invited to participate in the study . At our clinic all patients with an extensive UC are invited to enter a surveillance colonoscopy program for ten years after diagnosis with the aim to detect dysplasia and early cancer. Control subjects were recruited from patients who underwent a surveillance colonoscopy due to hereditary familiar colon cancer.
Both patients and controls were sent an informed consent, questionnaires and a faecal calprotectin test 46 weeks before the planned colonoscopy.
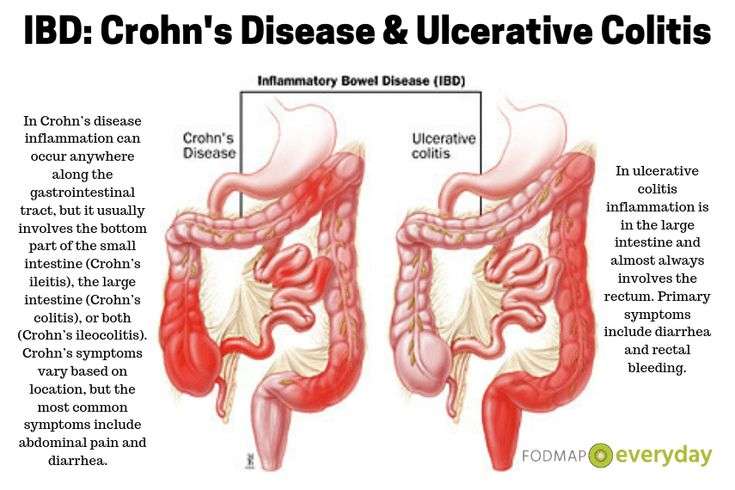
Crohns Disease And Ulcerative Colitis Overview
Crohns disease and ulcerative colitis are the two most common forms of inflammatory bowel disease . Crohns disease and ulcerative colitis can be treated, but there is no cure. UC and Crohns are separate diseases, but they both involve chronic inflammation of the digestive tract. People with IBD may have long periods of good health known as remission and periods of active symptoms known as relapses or flares. Symptoms vary among people with Crohns disease and ulcerative colitis, but most experience abdominal pain and cramping, diarrhea, nausea, vomiting, and fatigue.
Crohns disease and ulcerative colitis are not fatal, and on average, people with IBD have similar lifespans as people without either condition.
Both Crohns disease and ulcerative colitis are immune-mediated diseases, meaning the bodys immune response does not work as it should. In IBD, the immune system has an abnormal response, causing chronic inflammation and damage in the gastrointestinal tract. Read more about the causesof IBD.
Recommended Reading: What’s The Signs Of An Ulcer
It Is Common For Ibd & Ibs To Co
One of the happiest days in the life of someone with inflammatory bowel disease should be when they get the good news that their disease is in remission. But, this isnt how it plays out for everyone.
Lots of folks continue to experience intestinal symptoms despite their inactive disease. Thats because up to 40% of people with IBD also suffer from irritable bowel syndrome . It is not uncommon for IBD and IBS to co-exist. These people have a poorer quality of life compared to those with only IBD.
So, you may ask: What if I have IBS and IBD at the same time?
Fortunately, dietary and lifestyle modifications can significantly improve IBS-related symptoms in people with IBD in remission.
Symptoms Of Crohns Disease
Crohns disease is diagnosed when your intestine is inflamed and ulcerated. Symptoms include:
- Weight loss
- Fever
- Chronic diarrhea
Another key symptom is abdominal pain or a tender mass, particularly on the right side of the lower abdomen.
Crohns disease usually begins in the lower part of your small intestine and can affect any part of your digestive tract including the esophagus, stomach, colon, and small intestine. The inflammation penetrates all layers of your bowel walls.
You may have abscesses in diseased parts of the bowel interspersed among areas that are perfectly healthy. This makes Crohns disease unique from ulcerative colitis, which usually involves inflammation of the colon thats not interrupted.
Also Check: Stage 2 Pressure Ulcer Treatment Dressing
Overlap Between Ibd And Ibs
Although the two disorders have traditionally been seen as distinct in terms of both presentation and cause, some researchers are putting forth theories that perhaps the two diagnoses of IBS and IBD are actually at different ends of the same spectrum.
Some studies have shown that people who have IBS are at higher risk of eventually being diagnosed with IBD . One group of researchers found that this higher risk may be associated with having experienced infectious gastroenteritis .
-
Symptoms: pain plus constipation and/or diarrhea
-
Rarely leads to serious complications, surgery, or death
-
Symptoms: pain, diarrhea, bloody stool, fever, weight loss
-
Can lead to bowel perforation, infection, surgery, cancer, and death
Why Crohns Disease Happens
Researchers arent 100% sure why certain people develop Crohns disease. Diet and stress aggravate the condition, but dont cause it.
Sometimes people with Crohns disease are just part of an unlucky gene pool. Although in most cases of Crohns disease theres no family history of the disease.
Crohns is considered a problem of your immune system. Its surmised that when a specific type of virus or bacterium attacks, your body tries to fight it off and mistakenly attacks cells in the digestive tract, too.
Recommended Reading: What Is The Best Treatment For Ulcerative Proctitis
The Low Fodmap Diet For Ibd
Over the last decade Ive counseled countless patients with IBD on what to eat. Many people see me because they continue to have symptoms despite being in remission. They need help to identify the food triggers for their overlapping IBS.
Emerging research supports using the low FODMAP diet for managing IBS-related symptoms in patients with inactive IBD, particularly for abdominal pain, bloating and gas. My clinical experience aligns with these findings.
WARNING: Patients and healthcare professionals must be cautious when using any kind of restrictive diet with this population. Nutrient deficiencies, food intolerances, and disordered eating behaviors are common among IBD patients. We must not impose unnecessary dietary restrictions.
If someone cant do the entire low FODMAP diet, then start with just one or two groups of FODMAPs to eliminate. A registered dietitian can review ones current diet to help decide where to begin.
Lactose intolerance is more common in people with Crohns and ulcerative colitis, and Crohns patients are less likely to absorb fructose compared to the general population. Perhaps start by eliminating lactose and/or fructose?
Are There Ibd Or Ibs Diets
There is no special recommended diet to treat IBD, but some people may respond to dietary changes such as eating smaller and more frequent meals, taking nutritional supplements, and avoiding certain foods, for example, fatty and fried foods, meats, spicy foods, and fiber-rich foods. People with Crohns disease may have difficulty tolerating dairy products because of lactose intolerance.
Patients with IBS may respond to dietary changes. Low fat, high carbohydrate, and low FODMAP foods may help ease symptoms. Fiber can be helpful in some people.
You May Like: How Do You Get Ulcers In Your Stomach
How Can I Tell If I Have Ulcerative Colitis Or Crohns Disease
Its important that you, your healthcare provider, and a GI specialist work together closely to figure out whats causing your symptoms. This is especially important since the symptoms of Crohns disease and ulcerative colitis can be similar. Your providers may check blood work and a stool sample. To get an accurate diagnosis, your GI specialist may do a colonoscopy, where a camera is pushed into the colon. Your provider will look at the inside of the colon and take tissue samples, which are important for making the right diagnosis. Your providers might get a CT scan or an MRI of your abdomen to check for complications related to your condition.
How Is Ibd Diagnosed
Crohns disease and ulcerative colitis cause similar symptoms. No single test can diagnose either condition.
To make a diagnosis, your healthcare provider will ask about your symptoms. Your workup may start with a complete blood count and stool test to look for signs of intestinal inflammation.
You may also get one or more of these diagnostic tests:
- Colonoscopy to examine the large and small intestines.
- EUS to check the digestive tract for swelling and ulcers.
- Flexible sigmoidoscopy to examine the inside of the rectum and anus.
- Imaging scan, such as a CT scan or MRI, to check for signs of inflammation or an abscess.
- Upper endoscopy to examine the digestive tract from the mouth to the start of the small intestine.
- Capsule endoscopy using a small camera device that you swallow. The camera captures images as it travels through the digestive tract.
Don’t Miss: Herbal Medicine For Ulcerative Colitis
How Is Treatment Of Crohns Disease Different From Ulcerative Colitis
Although the medications may seem similar, there are differences in how Crohns disease and ulcerative colitis are treated. Many medication classes treat both conditions, so there is a lot of overlap. However, there are enough differences that getting the right diagnosis is important. For example, people with ulcerative colitis usually take aminosalicylates, while only a limited number of people with Crohns disease will benefit from these medications. When it comes to more advanced therapies like biologic agents, some can only be used for ulcerative colitis and some can only be used for Crohns disease.
Getting the correct diagnosis can be tricky. Sometimes it might look like you have ulcerative colitis at first, but later your providers will find out that its actually Crohns disease. Work closely with them to be sure you get the right treatment.
Causes Of Ibd And Ibs
Physical signs have helped doctors learn what causes IBD.
The long-lasting inflammation in the digestive tracts of people who have IBD can cause bleeding and ulcers . In turn, this irritation causes pain. That triggers the immune system, which leads to symptoms like fever and fatigue.
The causes of IBS arenât as clear. Scientists have found links to the immune system and how muscles move food through your gut. Many people have triggers that make their symptoms worse, including certain foods, stress, infections, and hormonal changes.
Read Also: How To Treat A Diabetic Foot Ulcer On The Sole
Ibd Vs Ibs: What’s The Difference
Here’s a rundown of IBD and IBS. Understand the similarities, differences and what to do if you think you have one.
IBS and IBD both cause some heavily unpleasant symptoms, but they are not the same condition.
Irritable bowel syndrome, leaky gut, functional gut disorder. It seems like everyone has some sort of stomach issue these days — and it’s not unreasonable to think so, considering the quality of the average American diet.
Two common digestive disorders, irritable bowel syndrome and inflammatory bowel disease, have some symptoms in common and people often use the terms interchangeably. IBD and IBS are not one and the same, though: The underlying causes differ, as do the diagnostic processes and treatments.
Get the CNET How To newsletter
This guide breaks down the differences between IBD and IBS, from definition to diagnosis to treatment options.
Irritable Bowel Syndrome Vs Colitis
Chronic illnesses of the gastrointestinal tract can be among the most debilitating of chronic diseases. It is frustrating and frightening to face abdominal pain or bowel issues and not know what is causing them.
Two of the more common of these diseases are irritable bowel syndrome and colitis. Although they share symptoms, they are very different diseases with very different complications. Heres a look at some of the differences between IBS and colitis.
What is Irritable Bowel Syndrome?
Irritable bowel syndrome is a chronic gastrointestinal disorder that requires long term treatment to provide any semblance of normalcy. IBS may be constipation or diarrhea or both, depending on the person. Though the cause of IBS is still under investigation, it may have something to do with abnormal contractions of the gut or abnormalities of the nerve endings there. Common symptoms of IBS include abdominal discomfort, bloating, gas, mucus in the stool, constipation, diarrhea, or alternating bouts of constipation and diarrhea. Treatment entails a careful diet, avoiding triggers, and pharmaceuticals.
What is Colitis?
Additionally, colitis may cause fatigue, fever, unintended weight loss. Children may experience failure to thrive. Treatment may involve anti inflammatories, immunosuppressants, and symptomatic treatment. Surgery to remove the rectum and colon may lead to complete remission of the disease.
Whats the Difference?
You May Like: What Are The Symptoms Of An Ulcer In Your Stomach
What Is Crohns Disease
Crohns disease is a type of IBD where there is inflammation of the entire gastrointestinal tract, or parts of it, from mouth to anus. In addition, the entire thickness of the bowel wall is involved in Crohns disease, which can lead to some serious complications.
What are symptoms of Crohns disease?
The symptoms of Crohns disease depend on what parts of the GI tract are involved. Common symptoms include abdominal pain, weight loss, and diarrhea.
If the lower part of the GI tract such as the colon and the small intestines are involved, you might also experience:
-
Abdominal pain
What are complications of Crohns disease?
Crohns disease can lead to some serious complications, such as:
-
Fistulas, where a hole is formed between the intestines and other parts of the body such as the skin, bladder, or vagina
-
Abscesses, which are pockets of infection that may need surgery or a procedure to drain them
-
Strictures, which are a narrowing of the bowel that can lead to blockages
-
Cancers of the GI tract