What Exams And Tests Diagnose Colitis
While unpleasant, the rectal examination is very important. Using a finger, the doctor feels inside the rectum, exploring for any masses or tumors. The color and consistency of stool can be evaluated, and if it is not grossly bloody, can be tested for occult blood .
Laboratory Tests
The history will assist the health-care professional decide the tests to order and what cultures would be appropriate. Blood tests help assess the stability of the patient, and also explore any potential issues associated with colitis.
- A complete blood count will assess the red blood cell count, the white blood cell count, and the number of platelets.
- The red blood cell count will help define the amount of bleeding.
- White blood cell counts elevate when the body is undergoing physical , physiological, or emotional stress.
- Platelets help blood to clot, so knowing the platelet number in a patient with bleeding may be useful.
Colonoscopy
Donât Miss: What Are The Symptoms Of An Ulcer In Your Stomach
Radiology Scans Or Diagnostic Imaging
Traditional upper GI endoscopy and colonoscopy are not be able to reach about two-thirds of the small intestine. Therefore, in addition to capsule endoscopy, various radiologic exams or diagnostic imaging may be performed to evaluate these parts of the intestines as well as to evaluate the actual wall of the bowel and surrounding areas outside the bowel.
X-rays
X-rays are the oldest way of imaging the inside of the body. X-rays are cost-effective and useful for detection of blockages in the small or large intestine.
Barium contrast studies
During a barium study, you will ingest a contrast material and have images taken with traditional X-ray technology. Barium is a chalky/milky liquid that you drink prior to the procedure. A series of X-rays are taken to observe the material flowing through the digestive system. These studies include:
Upper GI series examines the esophagus, stomach, and first part of the small bowel for patients with Crohns disease
Small bowel series and small bowel enteroclysis examines the entire small bowel. For a small bowel series, you will drink several cups of barium, and then have an X-ray taken every 1530 minutes as the barium travels down the small intestine and enters the large intestine. The time required varies but may take four to five hours. An enteroclysis is similar, except that the barium is placed directly into the small intestine through a tube introduced into the GI tract via the nose or mouth.
Cross-sectional imaging
Reasons To Be Open And Honest With Your Doctor
Having a good relationship with the right specialist for your UC can help you both have a clear idea of what is going on with your body and how to manage it.
Your doctor relies on what you tell him or her to get the full picture of how your disease is affecting your life. Use resources like the Doctor Discussion Guide to help make appointments go a little more seamlessly.
When you and your doctor have a good sense of whats going on with your UC, youll be able to confidently move toward a treatment plan thats right for you.
Learn about treatment options for ulcerative colitis.
Recommended Reading: Align Probiotic For Ulcerative Colitis
Surgery For Ulcerative Colitis
Even with the availability of medicines to treat ulcerative colitis, surgery may still be needed to manage the disease. There are a few types of surgery that your gastroenterologist with discuss with you.
Proctocolectomy
Removes the colon and rectum. Sometimes ileostomy is also done at this time, which is a procedure that brings the ileum, or end of the small intestine, through an opening in the abdominal wall to allow intestinal waste to drain out of the body. After the procedure, the patient wears an external bag over the opening to collect waste.
Restorative proctocolectomy
Before having surgery for ulcerative colitis, it is important to understand what the aim of the surgery is, what will happen during the procedure and the length of the recovery period. Patients with ulcerative colitis having surgery should speak to other patients who have had the procedure. Previous patients are often very willing to share their experiences and add perspective.
How The Va Assigns A Va Rating For Ulcerative Colitis
The VA assigns a VA rating for Ulcerative colitis from 10% to 100% by considering the severity of your symptoms and how they impact your work and daily life.
The VA uses Diagnostic Code 7323 to rate ulcerative colitis. The VA assigns a diagnostic code to every service-connected condition. There are four separate VA disability ratings you could be granted for ulcerative colitis.
Recommended Reading: Alginate Dressings For Treating Pressure Ulcers
Daisys Story: Symptoms And Medical History
I was 16 years old when I first noticed symptoms that I later found out were due to ulcerative colitis. The first symptom I noticed was severe fatigue, but I put this down to the exams I was taking at the time. I was also noticing abdominal pain more frequent bowel movements, and I was also passing blood. I noticed mucus in my stools and was experiencing frequent bouts of diarrhea.
At first, doctors thought that my symptoms were happening because of hemorrhoids, a stomach bug, parasite, or possibly a small tear. As my exams finished and my stress levels decreased, my symptoms became less noticeable too. However, they still persisted, and I was admitted to the hospital when I began to lose weight after not being able to eat drink.
When the doctors asked my mother and me about my family history, we explained that bowel cancer had affected some family members in the past. The doctors then ordered some blood and stool tests to investigate further.
Questions To Ask Your Health Care Provider
- How often do I need to see a gastroenterologist?
- How often do I need to undergo testing?
- What are my risks for colon cancer?
- Are there symptoms that should cause worry? If so, what are they?
If you dont know something at any point, ask for more information! For some, hearing that they have ulcerative colitis is a relief, a reason for symptoms and a light at the end of the tunnel. For others, it can be scary and daunting. Many will have a mix of feelings.All of this is completely normal.
Donât Miss: Does Ulcer Pain Come And Go
Recommended Reading: What Treatment For A Stomach Ulcer
Diagnosing Inflammatory Bowel Disease In Adults
In inflammatory bowel disease, or IBD, there is persistent inflammation in the gastrointestinal tract. The condition causes symptoms such as abdominal pain, diarrhea, bloody stool, constipation, and an urgent need to have a bowel movement. The most common types of IBD are Crohns disease and ulcerative colitis.
Gastroenterologists at NYU Langoneâs Inflammatory Bowel Disease Center are experts in the gastrointestinal tract and can recommend the appropriate diagnostic tests to determine the cause of your symptoms. There is no single definitive test to confirm the presence of IBD, so the condition is diagnosed based on a combination of tests, including endoscopy, biopsy, and imaging tests.
You May Like: What Are Some Symptoms Of An Ulcer
Watch A Video On Uc Testing And Disease Management
Understanding ulcerative colitis, or UC, doesnt stop at the diagnosis.
Its important to understand testing and disease management, too. We know this can be a lot, but youve got this.
Your doctor will discuss with you the proper tests that can help you find the proper treatment to manage your UC.
Because UC can progress over time, its important to ask your doctor how routine testing after diagnosis may help ensure your treatment is working.
Often together, doctors may test your blood, test biological molecules, called biomarkers, and take images throughout your body.
The results, along with the severity and area of inflammation in your large intestine, may influence how you manage your disease.
Prescription medication can be a common option to treat inflammation in your large intestine. Your doctor may suggest a range of things from changing your diet to surgery.
Ongoing testing is part of disease management, just like treatment.
Knowing more means you can do more. Youre in control of your condition, and now that youre in the know, you can better manage your UC.
When youre living with UC, tests are a routine part of taking care of yourself and managing your condition. Watch this video to understand the basics and help prepare for future visits to your gastroenterologist.
You May Like: How Do You Get Rid Of Ulcers
How An Intolerance Test Can Help Ulcerative Colitis
A 2018 Chinese study saw that a food intolerance test helped patients improve their ulcerative colitis symptoms markedly. The researchers used an IgG test to inform an elimination diet for patients to follow, and compared to a control group who followed a normal healthy diet, saw a noticeable improvement in symptoms.
After intervention, the Mayo score was significantly lower in the intervention group than in the control group . The number of patients with extra-intestinal manifestations decreased from 7 to 2 in the intervention group and from 6 to 5 in the control group.
Getting Referred To A Gastroenterology Team
If your blood and stool tests show inflammation, you should be referred by your GP to a defined specialist gastroenterology doctor in an IBD service. They have expert knowledge of gut conditions like Crohns and Colitis, and can do specialist tests like endoscopies . In some areas, you may be able to have some choice over which hospital you go to if you have been referred through the NHS e-Referral Service.
It may take some time to get an appointment with your gastroenterology team. The IBD Standards state that you should have a specialist assessment within four weeks of being referred, but it may sometimes take longer. Your GP should let you know how long you can expect to wait contact your GP surgery if you havent heard from the hospital within that timeframe so that they can chase up for you. You can also talk to your GP about how best to manage your symptoms while you wait for an appointment, and what to do if you start to feel worse.
Read Also: Foods Not To Eat With Stomach Ulcer
How Do Doctors Diagnose Ulcerative Colitis
To diagnose ulcerative colitis, doctors review medical and family history, perform a physical exam, and order medical tests. Doctors order tests to
- confirm the diagnosis of ulcerative colitis
- find out how severe ulcerative colitis is and how much of the large intestine is affected
- rule out other health problemssuch as infections, irritable bowel syndrome, or Crohn’s diseasethat may cause symptoms similar to those of ulcerative colitis
Blood And Stool Laboratory Tests
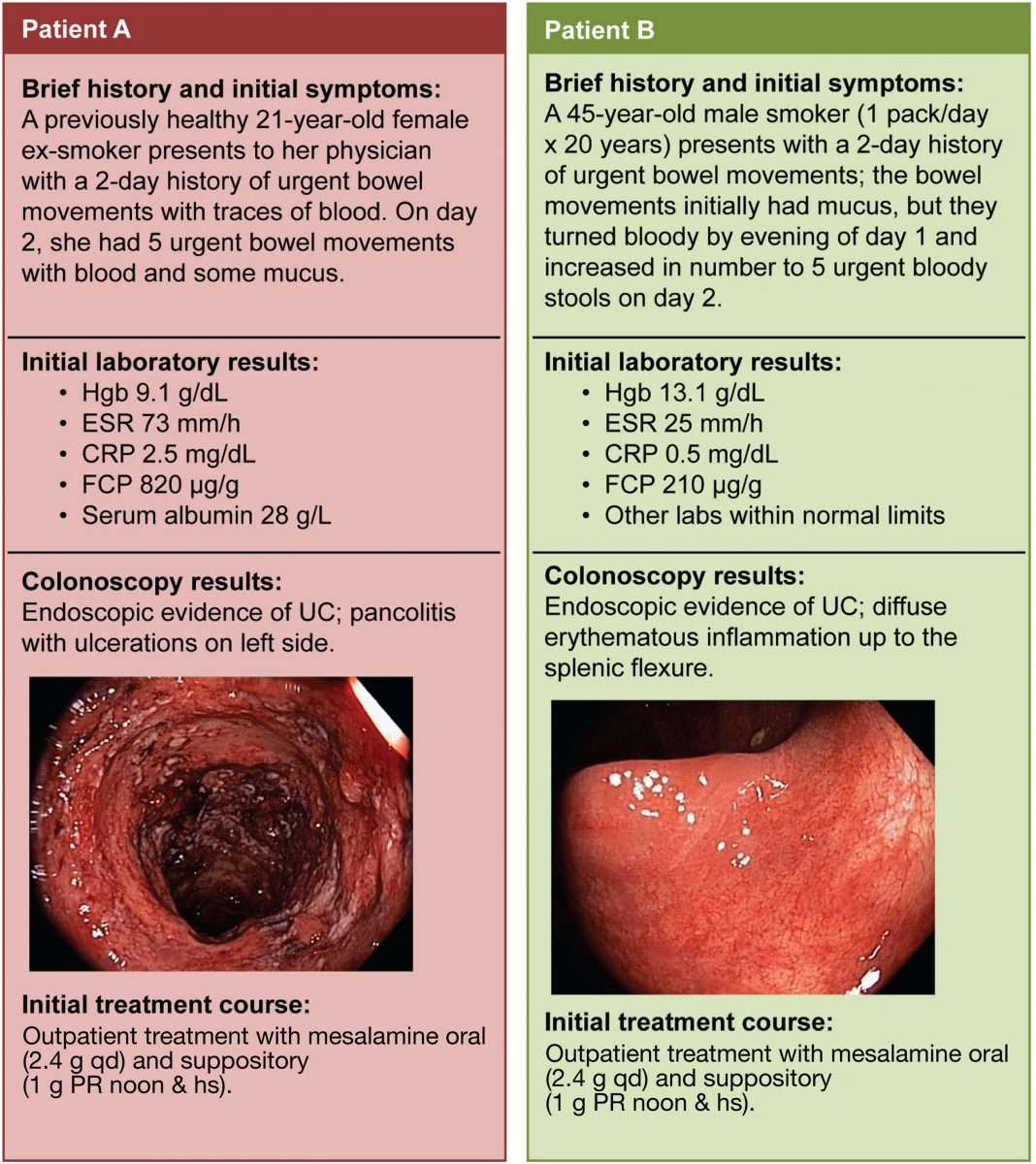
Doctors commonly use blood and stool tests as part of your initial diagnostic work-up. Proteins found in blood and stool, also called biomarkers, during blood and stool tests may be useful for detecting inflammation. Although these tests will not reveal whats causing the inflammation, they may indicate that further testing is needed to identify where the inflammation is coming from. Specific biomarker levels may also be followed over time to help assure that the therapy being used is optimized and that your inflammation is truly controlled.
Blood biomarkers include c-reactive protein and erythrocyte sedimentation rate , both of which help detect the presence of inflammation in the body.
Fecal biomarkers include calprotectin and lactoferrin, both of which are proteins found in stool that can indicate gastrointestinal inflammation.
Blood tests involve a blood draw from a vein in your arm. Stool tests involve utilizing a stool collection kit provided by your doctor or the lab along with specific instructions on how to collect a sample.
You May Like: Dog Skin Ulcer Home Treatment
Is Ulcerative Colitis A Disability How To Get Disability Benefits
The Center for Disease Control estimates that 3 million US adults suffer from inflammatory bowel disease because ulcerative colitis and Crohn’s disease have increased by one-third since 15 years ago. Because most people are diagnosed with IBD in their 20s and 30s, this statistic excludes children under 18 who can also be affected by IBD. While ulcerative colitis and Crohn’s disease share some symptoms and are both considered inflammatory bowel diseases and impact the person’s Quality of life, there are also some differences.
Disability Attorneys Can Help
Disability benefits may be available to you if you have ulcerative colitis or Crohn’s disease. Since disability attorneys have helped thousands of others like you navigate the Social Security Administration’s application process, they know how to prove your disability case.
Having a fear of rejection shouldn’t prevent you from submitting your application. It is not uncommon for people suffering from diseases like cancer to suffer from anxiety, discomfort, and stress associated with working 40 hours or more per week to make ends meet. Ensure that you receive the benefits you are entitled to by hiring expert disability lawyers.
Applying for Social Security’s benefits can be an overwhelming process. If you are interested in seeking SSDI benefits, check out our article on how to find the right disability lawyer. To learn more, please visit DisabilityHelp.org today!
Also Check: What Not To Eat With An Ulcer
Taking Care Of Yourself
Its natural that living with ulcerative colitis can make you feel stressed at times. Stress can sometimes trigger flare-ups so you may find it helpful to try some relaxation techniques. These may include deep breathing, meditation, yoga and mindfulness.
Regular exercise can also help to give you a boost and make you feel better. It can also improve your general health and help to keep your bones and muscles strong. This is important because some medicines for ulcerative colitis may affect your bone health.
Immunomodulators In The Treatment Of Cmv Colitis
The continued use of immunomodulators, including corticosteroids, thiopurines, and biologics, during antiviral therapy for CMV remains controversial. The European guideline recommends that cessation of all immunomodulatory therapies, including steroids, should be considered until the CMV colitis symptoms are controlled, and that no immunomodulator should be prescribed for patients with systemic CMV disease . However, the evidence level for these recommendations is 5 . Ciccocioppo suggested that steroids should be quickly tapered and discontinued, but immunosuppressants and biological agents with long-lasting effects should be maintained in patients with viral colitis and those exhibiting reactivation of latent infection . On the other hand, it has been suggested that any already initiated IBD treatment should be continued during antiviral therapy for CMV colitis . Sager et al. proposed that conventional corticosteroid therapy should be combined with antiviral therapy, and medical rescue therapy using immunosuppressants should be prescribed when necessary. Therefore, additional studies are required to explore the effects of immunomodulators employed to treat UC complicated by CMV colitis.
Several studies have shown that ganciclovir is essential for patients with steroid-refractory or -dependent UC and histologically high-grade CMV infections. Concomitant anti-TNF therapy to treat the UC may also be appropriate .
Don’t Miss: What Is Peptic Ulcer Disease
Causes Of Ulcerative Colitis Flares
Ulcerative colitis flares can be caused by a variety of things, including:
- Skipping medications or not taking the correct dose. If you regularly take medicine for your ulcerative colitis, you need to be consistent even when your disease is in remission. If you dont follow prescription instructions, flares can occur.
- Taking non-steroidal anti-inflammatory drugs. Common drugs like aspirin, naproxen, and ibuprofen can inflame the bowel and bring on serious symptoms. If you need mild pain relief or fever treatment, you should take acetaminophen.
- Taking antibiotics. Although theyre useful when you have bacterial infections, they affect the bacteria that live in your intestine. These changes can result in diarrhea or the growth of too much of a certain bacteria that then causes inflammation. If you have a bacterial infection, make sure your healthcare provider knows you have ulcerative colitis.
- Not managing stress. Physical and emotional stress can bring on flare-ups. Once you understand that stress causes such a reaction, you can find out what stress management strategies work to keep flare-ups at bay.
- Eating and drinking triggering items. The foods and drinks that bring on symptoms vary by person. Youll need to track your diet so you can pinpoint triggering items when you experience ulcerative colitis flares.
You May Like: How To Get Rid Of Ulcers In Horses
Don’t Delay Seeking Help
We know its not always easy talking about your bowel habits, but the sooner you get diagnosed, the easier your condition will be to treat.
Some important things to remember:
I always knew something wasnt right. Its not normal to bleed or feel like that. Initially, I felt scared and didnt want to tell anyone but being diagnosed helped me come to terms with it and get on with life.
ArizonaLiving with Indeterminate Colitis
Read Also: How To Find Out If You Have Ulcerative Colitis