How To Treat Pain
There are various treatment options for UC, and the best approach for a person will depend on the severity of their symptoms. Over-the-counter medications can sometimes help relieve the pain that UC can cause. However, severe cases require stronger pain relievers.
Medications for the treatment of UC include:
How Does Pediatric Ulcerative Colitis Affect My Childs Mental/emotional Health
Like many conditions, ulcerative colitis can have a negative psychological effect, especially on children. They can experience physical, emotional, social and family problems. Because of the medications and/or general stress from the situation, your child may experience:
- Worry about appearance and physical stamina.
- Vulnerability because their body doesnt function normally.
- Poor concentration.
- Misunderstandings with friends and family.
Children need mutual support from all family members. Its helpful for the entire family to learn about the disease and try to be empathetic. Seek out a psychiatrist and therapist to help your child manage such challenges of their ulcerative colitis.
What Is Ulcerative Colitis
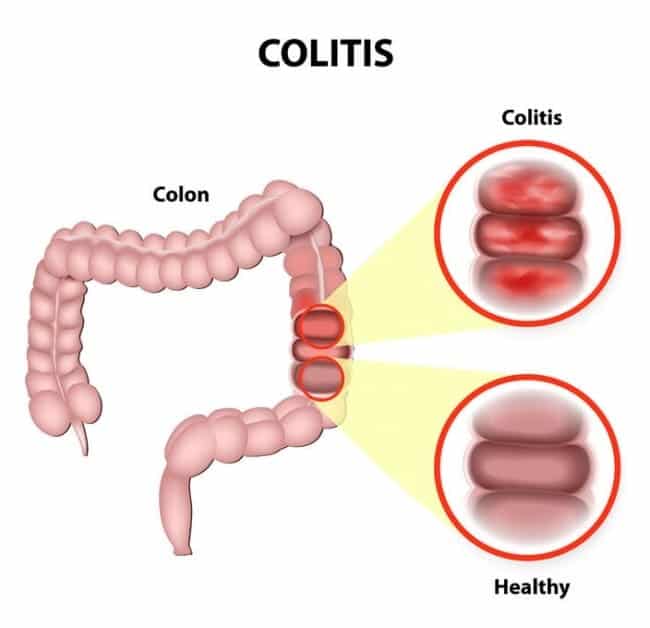
Colitis is a bowel disease , resulting in pain, loose bowel movements or diarrhea, loss of bowel control, and intestinal bleeding . There are over ten types of colitis, with the most common being ulcerative colitis, ischemic colitis, microscopic colitis, and infectious colitis. Causes of colitis include food allergies, infections, poor blood supply, and autoimmune reactions.
After healing myself of serious gastrointestinal disease, consulting with people with all types of colon and bowel conditions for over ten years, and answering thousands of questions on my online forum, I have become internationally recognized as an expert on natural remedies for colitis, Crohns and diverticulitis. Even if you have tried every colitis treatment available without success, dont give up hope my natural remedies for colitis have helped tens of thousands of people worldwide, and my books are sold in over 80 countries.
N.P., London, UK
My daughter had her check up with her Paediatrician yesterday he was amazed at her histology and also her Colonoscopy results. He took notes to see what I have been doing. He was so skeptical in August but was astounded at how minimal her inflammation is and he is taking everything from your book seriously he has ordered a copy of Listen To Your Gut and has asked me to give him a breakdown of everything. I will keep shouting your name from the rooftops thank you so much!
Read Also: Early Stage Venous Leg Ulcer
You May Like: Can An Ulcer Cause Stomach Pain
Ulcerative Colitis Adversely Affects Many Patients And Current Treatments Are Relatively Ineffective
Ulcerative colitis adversely affects the quality of life of many patients with symptoms that include frequent diarrhea, urgent bowel movements, rectal bleeding, and fatigue. Patients quality of life and economic productivity are significantly impaired by chronic ulcerative colitis . This disease often strikes individuals in their teens and twenties, and continues to wax and wane for the remainder of their lives. The severity of the symptoms, as well as the unpredictability of flares of disease, can significantly impair the lives of those affected .
Current therapies for ulcerative colitis are only modestly effective, as up to 45% of patients eventually have total surgical removal of their colon . This is a daunting and irreversible choice for young patients to make. It is particularly difficult for young females, in whom the scarring of the pelvic organs after total colectomy can result in a three-fold increase in infertility . Therefore, it is quite important to evaluate all the symptoms that patients perceive as important in assessing disease activity, to determine whether the current medical treatment is truly effective.
Back Pain And Ulcerative Colitis
| | |
Research indicates that nearly 25 percent of people with inflammatory bowel disease including ulcerative colitis and Crohns disease experience chronic lower back pain. Ankylosing spondylitis and axial arthritis both of which can cause back pain are two common causes of back pain for people with UC.
That said, a doctor may not suspect that a person with back pain has UC unless they also experience gastrointestinal symptoms. If you do experience back pain, its important to let your doctor know even if you dont suspect its related to UC. They will be able to determine the cause of your pain and work with you to find the best way of managing it.
A person having backaches may not realize theyre related to digestive problems or think to mention it to their doctor. However, ulcerative colitis can cause extraintestinal symptoms including back pain.
Although back pain can result from other causes, such as injury or overexertion, UC-related back pain stems from inflammation. Generally speaking, people with ulcerative colitis can trace their back pain to spondyloarthritis. Spondyloarthritis, also known as spondylitis, is a type of arthritis that causes inflammation specifically in the axial joints those of the spine, chest, and pelvis. Spondyloarthritis includes axial arthritis and ankylosing spondylitis.
You May Like: Why Do You Get Mouth Ulcers
What Should I Ask My Doctor
If you have ulcerative colitis, you may want to ask your healthcare provider:
- How much of my large intestine is affected?
- What risks or side effects can I expect from the medication?
- Should I change my diet?
- Will ulcerative colitis affect my ability to get pregnant?
- What can I do at home to manage my symptoms?
- What are my surgical options?
Five Tips For Dealing With Ulcerative Colitis Pain
There are ways to combat the pain that comes along with ulcerative colitis flare-ups. However, it is always best to get treatment from a doctor as they are most likely to efficiently and safely resolve your symptoms.
Here are five strategies you can use to help relieve symptoms and avoid a flare-up in the first place.
You May Like: How To Lose Weight With Stomach Ulcers
Don’t Miss: What Can Be Done For An Ulcer
What Are The Symptoms Of Ulcerative Colitis
Ulcerative colitis symptoms often get worse over time. In the beginning, you may notice:
- Diarrhea or urgent bowel movements.
- Abdominal cramping.
- Loss of fluids and nutrients.
Symptoms are similar in pediatric ulcerative colitis and may also include delayed or poor growth. Some ulcerative colitis symptoms in children can mimic other conditions, so it is important to report all symptoms to your pediatrician.
Avoid Foods That May Exacerbate Uc Symptoms
Because a healthy diet is a cornerstone for overall health, its no surprise that it tops Sniders list of natural remedies for ulcerative colitis. Diet is a foundational treatment for patients with ulcerative colitis, he says, adding that thereâs often a dietary component to the disease.
According to a review published in October 2014 in Clinical Gastroenterology and Hepatology, people who reported a diet high in fats were more likely to have a relapse of UC. Other studies highlighted in the paper suggested avoiding greasy foods, dairy products, caffeine, and raw fruits and vegetables if you have ulcerative colitis. But the review notes that theres no one-size-fits-all diet for UC, so youll have to figure out what works best for you through trial and error.
It helps to keep a food diary to discover which foods are best for you. Snider says it canât hurt to limit certain foods, and then if your symptoms improve according to your symptom diary, to continue doing so. He also notes that itâs worthwhile to avoid sugar because its effect on the pancreas hinders the output of anti-inflammatory enzymes.
Recommended Reading: Do Stomach Ulcers Cause Back Pain
Rectal Bleeding And Discharge
UC often causes bleeding or mucus discharge from your rectum. You may find spots of blood or mucus in your toilet or on your clothing. Your stool may also become very soft and bloody or contain red streaks or mucus. You may also experience pain in your rectal area, as well as a persistent feeling of needing to have a bowel movement.
When To Contact A Doctor
People need to discuss any blood in the stools with their doctor, even if they have experienced it before.
A person may also wish to monitor their UC symptoms, so they know what is usual for them to experience. People can then discuss any abnormal symptoms with a healthcare professional.
If individuals have ongoing diarrhea that lasts for a couple of weeks, they can contact their doctor to discuss concerns and treatment.
The Crohnâs and Colitis Foundation advises people to seek emergency medical attention if they experience any of the following:
- inability to keep down liquids due to nausea, vomiting, or pain
- rectal bleeding with blood clots in stools
- continuous pain
Managing UC with treatment may help reduce bleeding. There are medications that may reduce inflammation in the rectum and large intestines, which may, in turn, reduce bleeding.
Anti-inflammatory medications for UC can include:
- 5-Aminosalicylic acid: Medication that may help reduce acute inflammation and causes inflammation to become inactive over time.
- Corticosteroids: A short-term treatment to help reduce inflammation.
- Immunosuppressants: These medications can help suppress the immune response that can cause inflammation. However, they may take up to 6 months to be effective.
- Biologics: For treatment of moderate to severe UC, biologics help block molecules that trigger inflammation.
Don’t Miss: Foods That Help Ulcerative Colitis
Where The Pain Occurs
Pain is a common symptom of UC. According to the Crohns & Colitis Foundation, 33% of people with UC experience chronic abdominal pain. Pain management is, therefore, an important part of the treatment plan.
Pain due to UC occurs most commonly in two regions: the rectum and the lower left side of the abdomen. Doctors associate the areas of inflammation with a certain type of UC.
The severity of the symptoms can vary over time, with people often experiencing periods of mild or no symptoms, known as remission, alternating with periods of more severe symptoms, known as flare-ups.
Be Diligent And Careful With Medication
A physician will usually prescribe an anti-inflammatory and medication to help with an overactive immune system with a diagnosis of ulcerative colitis. This medication is vital to fight off flare-ups and missing a dose can be a trigger all by itself.
When taking medication for this condition, it is always wise to consult a doctor. Certain over-the-counter medications, like NSAIDs, can exacerbate ulcerative colitis as well as cause other issues.
Read Also: How Do You Treat A Peptic Ulcer
Also Check: Vsl 3 And Ulcerative Colitis
Common Ulcerative Colitis Symptoms
Stool, defecation, feces, poop whatever you call it, its no fun to talk about. But the truth is, your stool can tell a lot about your health status, so if you notice its out of the ordinary, its important to seek professional medical help.
Dr. Darrien Gaston at Metropolitan Gastroenterology Consultants sees patients throughout Chicago, Illinois, and specializes in identifying and treating potentially dangerous conditions like ulcerative colitis. Here, he takes a deep dive into this incurable inflammatory bowel disease.
Get Regular Exercise To Reduce Uc Inflammation
Snider says exercise is useful in managing many of the complications associated with ulcerative colitis, including decreased bone density, a weakened immune system, emotional health problems, stress, and weight gain.
âTry to engage in a moderate-intensity exercise like swimming or biking, three or four days per week,â he says. A review published in August 2016 in Pharmacological Reports noted that moderate exercise releases protective myokines such as irisin from working skeletal muscles, which promotes healing and helps with inflammatory bowel disease inflammation.
Snider also strongly recommends yoga as a natural treatment for ulcerative colitis, as it promotes relaxation and targets the digestive system, flooding the area with oxygen and nutrition for healing. Find what type and frequency of exercise works for you and take it slow: Too much exercise can cause mild systemic inflammation.
Research indicates that stress plays a role in inflammatory bowel diseases such as ulcerative colitis. Researchers analyzed data on 2,007 adults in a Swiss IBD study and found a relationship between depression and anxiety and disease symptoms. The results were published in June 2016 in Clinical Gastroenterology and Hepatology.
Counteract stress with relaxation techniques such as meditation, deep breathing, and progressive muscle relaxation to help your body relax.
Donât Miss: Do Ulcers Cause Acid Reflux
Read Also: Best Alcohol To Drink With Ulcerative Colitis
Bleeding In Ulcerative Colitis
Ulcerative colitis causes inflammation and sores called ulcers in the large intestine. Blood in the stool is more common in ulcerative colitis than it is in Crohn’s disease.
The inflammation in ulcerative colitis often involves the rectum. Because the rectum is at the end of the large intestine, blood from this source is quite visible in or on the stool.
Bleeding also occurs with ulcerative colitis because this form of IBD attacks the lining of the large intestine. The ulcers that form in the mucosa of the large intestine tend to bleed.
When Should You Call Your Doctor
If youre experiencing certain symptoms, chances are, your current treatment is not working and its time to consider a change in therapy, says Ha. Call your doctor if:
- Cramping is severe
- Youre experiencing a significant amount of abdominal pain that requires medication
- You have a fever that lasts longer than a couple of days
- You experience nausea or vomiting
- You have ongoing diarrhea or blood in your stool
Recommended Reading: Ulcers On Legs From Diabetes
Analysis Of Focus Group Data
Each focus group meeting was audiotaped and fully transcribed. Each transcript was entered into NVivo version 2.0. Two members of the study team independently reviewed each transcript with a holistic view of symptoms and themes from each of the five focus group meetings and generated a list of symptom domains and common themes discussed by participants of each focus group . These lists were compared for agreement and consensus was reached . This list served as a template for a coding scheme used to analyze each transcript. The transcripts were independently coded by symptom domain and theme by J.C.J. and A.K.W. and codes were compared for agreement.
When To Seek Medical Advice
You should see your GP as soon as possible if you have symptoms of ulcerative colitis and you haven’t been diagnosed with the condition.
They can arrange blood or stool sample tests to help determine what may be causing your symptoms. If necessary, they can refer you to hospital for further tests.
Read more about diagnosing ulcerative colitis.
If you’ve been diagnosed with ulcerative colitis and think you may be having a severe flare-up, contact your GP or care team for advice. You may need to be admitted to hospital.
If you can’t contact your GP or care team, call NHS 24 111 service or contact your local out-of-hours service.
You May Like: Biological Medicine For Ulcerative Colitis
Ankylosing Spondylitis And Ulcerative Colitis
When bone fusion occurs, axial spondyloarthritis progresses into ankylosing spondylitis. AS is a specific type of axial arthritis that causes inflammatory back pain and limits range of motion. If a person has AS that causes significant fusing in their vertebral column and affects their rib movement, they may also struggle to take deep breaths.
According to the University of Washington, ankylosing spondylitis symptoms generally dont present alongside gastrointestinal symptoms in people with UC. Although doctors arent entirely sure what causes AS, some research suggests a genetic component contributes to the diseases development. Bowel or urinary tract infections are also believed to trigger the onset of AS in genetically susceptible people.
How To Deal With Ulcerative Colitis
Ulcerative colitis, a type of inflammatory bowel disease, causes painful open sores in your large intestine and rectum. The disease can affect both children and adults. Although there is currently no cure for ulcerative colitis, symptoms can be managed with medications and dietary changes in many cases.
What are the symptoms of ulcerative colitis?
Although symptoms of ulcerative colitis vary depending on the severity of the disease, diarrhea that contains blood or pus is a frequent problem. It may be difficult to get the bathroom in time, particularly if a bout of diarrhea strikes in the middle of the night. Other symptoms can include:
- Difficulty defecating
If you have severe ulcerative colitis, you may be more likely to develop one or more serious complications, such as severe dehydration or bleeding, a perforated colon, osteoporosis, megacolon, blood clots or colon cancer.
What are the risk factors for ulcerative colitis?
Ulcerative colitis symptoms usually appear between the ages of 15 and 35. Youre more likely to develop ulcerative colitis if other people in your family have it. Your ancestry may also affect your risk. Caucasians and people of Ashkenazi Jewish descent get the disease more often than other ethnic groups.
How is ulcerative colitis treated?
You May Like: Natural Remedies For Mouth Ulcers
What Should I Ask My Doctor On Behalf Of My Child Or Teenager
Ask your healthcare provider the following questions in addition to the ones listed above:
- What vitamins should my child take?
- Will my other children have pediatric ulcerative colitis?
- Is my child at risk for other conditions?
- Can you recommend a psychiatrist or therapist to help my child with emotional issues related to pediatric ulcerative colitis?
- Is my child growing at a normal rate?
- What can I do to help my child cope at school?
A note from Cleveland Clinic
When you have ulcerative colitis, its essential to work closely with your healthcare team.
Take your medications as prescribed, even when you dont have symptoms. Skipping medications youre supposed to take can lead to flareups and make the disease harder to control. Your best shot at managing ulcerative colitis is to follow your treatment plan and talk to your healthcare provider regularly.