What To Expect At Home
Diabetes can damage the nerves and blood vessels in your feet. This damage can cause numbness and reduce feeling in your feet. As a result, your feet are more likely to get injured and may not heal well if they are injured. If you get a blister, you may not notice and it may get worse.
If you have developed an ulcer, follow your health care provider’s instructions on how to treat the ulcer. Also follow instructions on how to take care of your feet to prevent ulcers in the future. Use the information below as a reminder.
The Top 4 Causes Of Dangerous Foot Ulcers
There are several medical conditions in podiatry that can result in frequent or non-healing wounds to the feet . Diabetes is one of the most common, but there are others, such as peripheral neuropathy, atherosclerosis, and Raynaud’s phenomenon. Without going into the scientific differences of these medical issues, there are four main reasons that ulcers form and get worse.
From Injury Or Blister To Ulcer
If a person with decreased sensation gets a blister or other injury, they may not notice it and it can develop into an ulcer.
Neuropathy:Neuropathy is a general term for nerve dysfunction. Peripheral neuropathy is the most common type of neuropathy in people with diabetes and typically affects the nerves of the feet, legs, and sometimes the arms and hands.
People with diabetes are at increased risk for peripheral neuropathy if they have a history of hyperglycemia and have had diabetes for a long time. Other risk factors for neuropathy include smoking and genetic predisposition.
Over time elevated blood sugar levels can affect nerve functioning and nerve signaling. Small nerve dysfunction results in the inability to feel pain, and large fiber dysfunction causes disturbances in balance, which can increase the risk of falls.
If a person has neuropathy and injures their foot without feeling it, they may not notice it until it gets much worse. Recurrent, unnoticed injuries to the foot can increase the risk of Charcot foot, in which progressive destruction of the bones and joints leads to foot deformity.
Autonomic neuropathy can cause a decrease in sweating, resulting in dry feet. Having dry feet can increase the risk of developing calluses. While calluses are healthy, if you have lost sensation, they can grow deeper cause damage to the skin surface known as breakdown, putting the foot at risk of blisters or ulcers.
You May Like: What To Take For An Ulcer Over The Counter
Who Gets Diabetic Foot Ulcer
Diabetic foot ulcer has an annual incidence of 26% and affects up to 34% of diabetic patients during their lifetime. Risk factors for developing a diabetic foot ulcer include:
- Type 2 diabetes being more common than type 1
- A duration of diabetes of at least 10 years
- Poor diabetic control and high haemoglobin A1c
- Being male
- A past history of diabetic foot ulcer.
How Do I Take Care Of My Ulcers
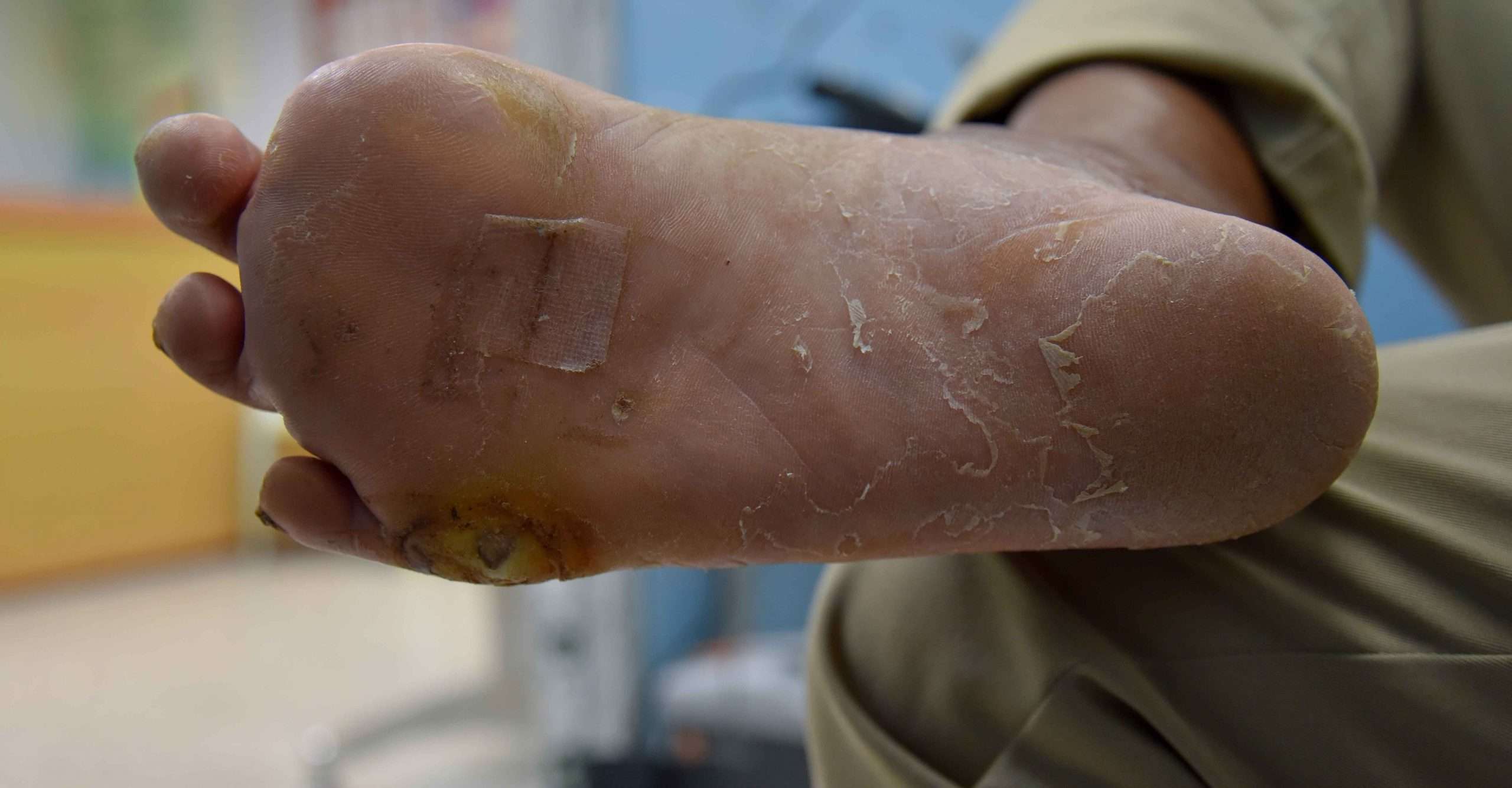
Your healthcare provider may teach you how to care for your ulcers at home. Some instructions may include:
- Wash the affected area with mild soap.
- Keep the wound clean and dry.
- Change the bandages as directed.
- Take prescribed medications as directed.
- Drink plenty of fluids. Ask your healthcare provider how much water you should drink every day.
- Follow a healthy diet, as recommended by your healthcare provider.
- Exercise regularly, under your healthcare providers care.
- Wear appropriate shoes.
- Wear compression wraps as directed.
Recommended Reading: Best Treatment For Diabetic Foot Ulcer
How Can Diabetic Foot Ulcers Be Prevented
Looking after your feet can help prevent foot ulcers and avoid serious complications. Good foot care includes checking your feet every day, keeping them clean and dry, wearing proper footwear and trying to avoid doing things that could damage them.
Get a foot check at every healthcare visit and seek urgent medical advice if you notice a cut, ulcer or other injury on your foot.
Learn more about diabetes and foot care.
Sores On Bottom Of Feet Causes Symptoms And Treatments
Sores or blisters on the bottom of feet can emerge from several causes. Common causes are dyshidrotic Eczema or Athlete`s foot infections. Injuries or underlying diseases can also contribute to this unsympathetic condition. Symptoms can be mild, moderate or severe i.e. bleeding. Here, you`ll learn more about causes, symptoms, and remedies for this nerve-racking foot problem.
Also Check: What Are The Symptoms Of Stomach Ulcers In Humans
How Can A Foot Ulcer Be Prevented
The best way to treat a diabetic foot ulcer is to prevent its development in the first place. Recommended guidelines include seeing a podiatrist on a regular basis. He or she can determine if you are at high risk for developing a foot ulcer and implement strategies for prevention.
You are at high risk if you:
- Have neuropathy
- Have a foot deformity
- Wear inappropriate shoes
- Have uncontrolled blood sugar
Reducing additional risk factors, such as smoking, drinking alcohol, high cholesterol, and elevated blood glucose are important in the prevention and treatment of a diabetic foot ulcer. Wearing the appropriate shoes and socks will go a long way in reducing risks. Your podiatric physician can provide guidance in selecting the proper shoes.
Learning how to check your feet is crucial in noticing a potential problem as early as possible. Inspect your feet every dayespecially between the toes and the solefor cuts, bruises, cracks, blisters, redness, ulcers, and any sign of abnormality. Each time you visit a health care provider, remove your shoes and socks so your feet can be examined. Any problems that are discovered should be reported to your podiatrist or a medical professional as soon as possible, no matter how simple it may seem to you.
The key to successful wound healing is regular podiatric medical care to ensure the following gold standard of care:
- Lowering blood sugar
Diabetes And Foot Sores
img source: spineorthocenter.com
Food problems are common in diabetic people but it is possible to limit the chances of suffering from this giant. Diabetes may result in nerve damage and this can lead to tingling or pain on the bottom of the foot but again, you can lose feeling on the feet. If you lose feeling in the feet, you may not notice the pebbles or sharp objects in your socks or shoes. This may contribute to the bottom of foot cut or sores. This may thereafter be accompanied by lowered blood flow in the feet or secondary infections.
In the case of diabetes, you should see a specialist called podiatrist to attend to you. Other foot care tips should also be considered.
You May Like: What To Do When You Have A Stomach Ulcer
Signs And Symptoms Of A Diabetic Foot Ulcer
It is important to note that when the nerves in the foot are functioning well, then the ulcer will be painful. But if the nerves are damaged, pain may not be felt. Therefore, the ulcer may not be noticed, more particularly if it is located on a less visible portionof the foot.
Blisters are seen on the foot or lower leg. The diabetic foot ulcer may look like a red crater or depression in the skin. In more advanced ulcers, it can be deep enough to expose the tendons or even the bones. Sometimes, the crater can be bordered by a margin of callused or thick skin.
Another sign that may point to foot ulcer is difficulty in walking. Doctors also check the gait to see any lower leg abnormalities that can cause ulcers. Any difference in walking consult your doctor right away!
It makes the persons skin more apt to changes like cracking, scaling, and excessive skin dryness may mean that circulation to the skin is compromised.
Also, signs and symptoms like swollen feet may also come with diabetic ulcers. This is usually accompanied by tired, aching legs. With chronic venous stasis, the lower legs are usually edematous and there may be hyperpigmentation of the skin.
Do to diabetic complications, decreased circulationmay lead to temperature changes, either increased warmth or coolness. If there is an ongoing infection, then the patient may have fever, chills, redness, and the wound may have drainage.
How Is Diabetic Foot Ulcer Treated
Debridement to remove all necrotic tissue. This is done using surgical instruments, ointments containing enzymes or pulse lavage therapy. After debridement, the wound is irrigated with saline or cleanser and a dressing is applied.
Offloading or removing pressure from foot ulcers by avoiding walking, using crutches, wheelchair, wearing casts, braces, inserts, diabetic shoes.
Infection control: Polymicrobialinfectionsinclude hemolytic streptococci, pseudomonas aeruginosa, enterococci, MRSA etc. Antibiotics such as Amoxicillin and Clavulanate Potassium, Ampicillin and Sulbactam, Cephalexin, Ciprofloxacin are started after initial cultures are taken.
Honey dressings are showing promising results in ulcer treatment. Also homeopathy medicines like Hepar Sulph, Merc Sol, Silicea, Kali bichromicum are very useful.
This is advised if there is no significant improvement even after a month of treatment.
- Skin grafting
- If you have corns or calluses, ask your doctor about how to care for them.
- If you are overweight, follow a plan to lose weight.
- Temperature control of feet can prevent ulcers in diabetics.
Tips for Patients who Have Recovered from Foot Ulcer:
Read Also: Best Probiotic For Ulcerative Colitis
What Are The Clinical Features Of Diabetic Foot Ulcer
A diabetic foot ulcer is a skin sore with full thickness skin loss often preceded by a haemorrhagicsubepidermal blister. The ulcer typically develops within a callosity on a pressure site, with a circular punched out appearance. It is often painless, leading to a delay in presentation to a health professional. Tissue around the ulcer may become black, and gangrene may develop. Pedal pulses may be absent and reduced sensation can be demonstrated.
Diabetic foot ulcer
Treatments For Sores On The Bottom Of Feet
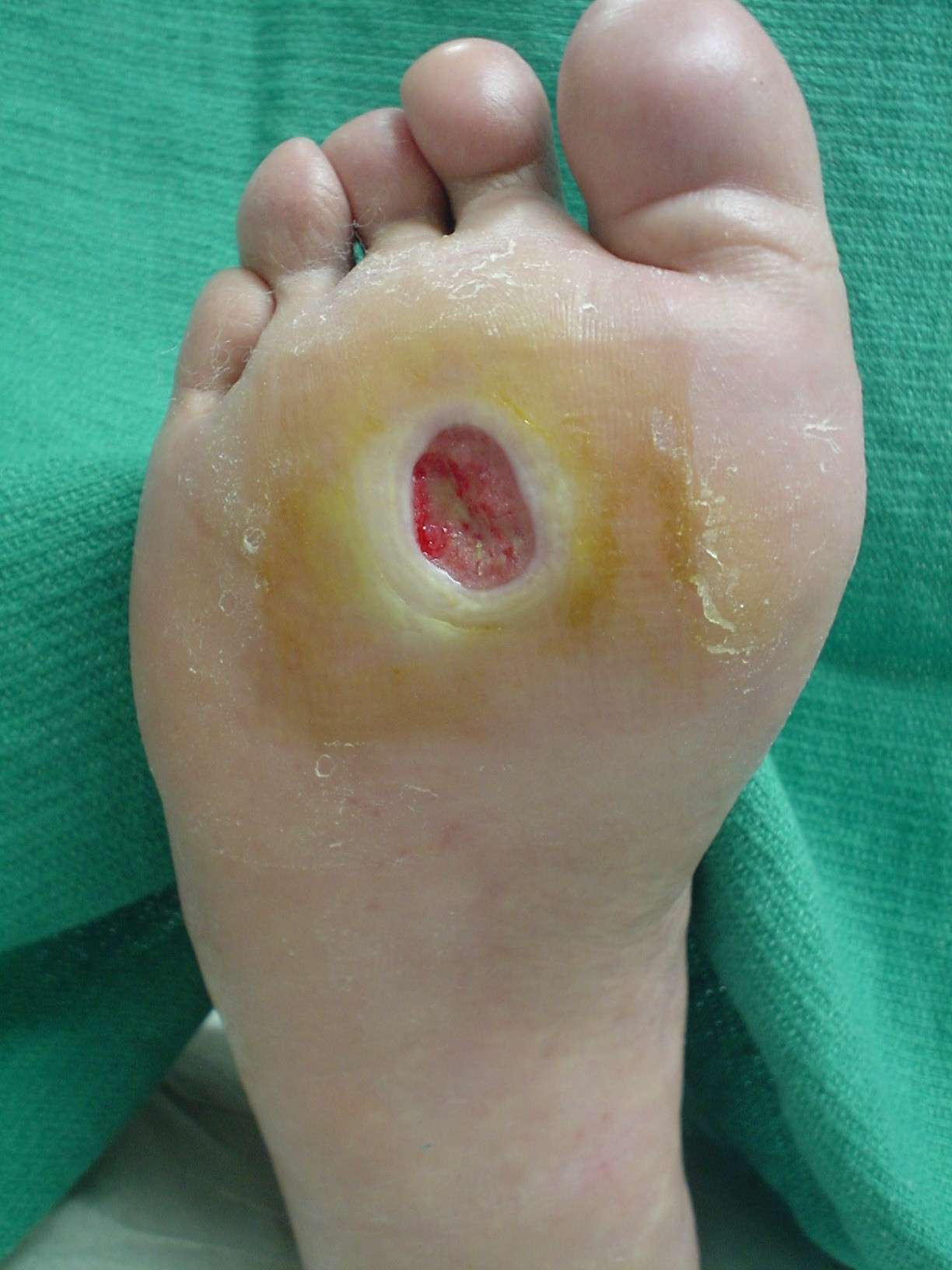
To treat such kind of sores, there are two factors we have to consider. Treatment for underlying causes or treating the resultant symptoms. These may involve over the counter therapies, prescribed medicines or home remedies. Efforts to prevent infections must too be included. Here are the common treatments you can employ for your cases.
Read Also: Prednisone For Ulcerative Colitis Reviews
Types Of Diabetic Ulcers
There are several types of diabetic foot ulcers
- Neuropathic ulcers occur where there is peripheral diabetic neuropathy, but no ischemia caused by peripheral artery disease.
- Ischemic ulcers occur where there is peripheral artery disease present without the involvement of diabetic peripheral neuropathy.
- Neuroischemic ulcers occur where the person has both peripheral neuropathy and ischemia resulting from peripheral artery disease.
Arriving at the correct diagnosis and identifying the cause of a diabetic ulcer is critical since it affects the treatment plan.
How To Prevent Diabetic Foot Ulcers
The first line of defense in preventing diabetic wounds is to follow the guidelines recommended to keep the disease itself under control:
- Maintain healthy blood sugar levels through a healthy diet and by taking medications as instructed by your doctor.
- Keep your blood pressure within a healthy range.
- Avoid alcohol and tobacco.
You should also take measures to avoid causing sores or wounds on the feet:
- Never walk barefoot.
- Wear shoes that fit properly and dont rub the skin.
- Wash your feet daily with mild soap and lukewarm water to prevent the buildup of bacteria on the skin, which can cause infection even in the tiniest skin breaks.
Because a loss of sensation in the feet may mean theres no pain felt even when an ulcer is present, its also extremely important for those with diabetes to regularly check for any foot sores or skin irritation. This way, the ulcer can be properly treated as early as possible.
Also Check: What Medicine Is Good For Ulcers
When Is It Crucial To Seek Medical Attention
If patients observe flesh that has turned black around a region that is numb, it is important to seek medical attention. This can be a sign of infection in the foot ulcer. In the absence of treatment, foot ulcers can cause abscesses. The infection can also spread to other regions in the legs and feet.
Doctors assess the infection and decide if they need to perform surgery or amputation or need to use synthetic skin substitutes to replace the lost skin.
The risk for diabetics to experience an amputation is 10 to 20 times more than non-diabetics. Close to 85% of all lower-limb amputations are complications from a foot ulcer.
Symptoms Of Foot Ulcers
A foot ulcer may be painful if the wound is open and doesnt heal however, if you have neuropathy, you may not feel pain and you wont realize you have an ulcer unless you inspect your feet daily. Blood or discharge stains on socks or in footwear may signify a sore, a cut or an ulcer, so if you have neuropathy also inspect your sockwear and shoes daily.
Read Also: How Do You Treat A Duodenal Ulcer
Who Can Get A Diabetic Foot Ulcer
Anyone who has diabetes can develop a foot ulcer. Native Americans, African Americans, Hispanics and older men are more likely to develop ulcers. People who use insulin are at a higher risk of developing a foot ulcer, as are patients with diabetes-related kidney, eye, and heart disease. Being overweight and using alcohol and tobacco also play a role in the development of foot ulcers.
What To Do If You Notice A Problem
The signs of diabetic ulcers on the foot should never be left untreated. If you have any of the symptoms mentioned above or think you might have a foot sore or ulcer, you should be seen by a doctor as soon as possible to avoid further damage and possible infection. The earlier you seek medical help, the less chance of complications further down the line.
Here at the Midwest Institute for Non-Surgical Treatment , we have qualified podiatrists who can provide you with the right treatment for your diabetic foot ulcer. We’ll also advise you on how best to look after your feet to prevent reoccurrences.
Book an appointment with Dr. Akinwande and the team who can treat you at one of our convenient locations in the St Louis area. Call us today, and we’ll get you back on your feet and the path to recovery.
Don’t Miss: Why Is Ulcerative Colitis Worse At Night
How Can I Prevent Or Reduce My Risk Of Foot And Toe Ulcers
It may be possible to reduce your risk of getting ulcers, and even stop them from coming back. Try to:
- Manage your diabetes. If you have diabetes you should wear appropriate footwear and never walk barefoot.
- Every day, examine your legs as well as the tops and bottoms of your feet and the areas between your toes. Look for any blisters, cuts, cracks, scratches or other sores. Also check for redness, increased warmth, ingrown toenails, corns and calluses. Use a mirror to view your leg or foot if necessary, or have a family member look at the area for you. See a healthcare provider immediately if you notice any problems.
- Wear appropriate shoes and socks. Talk to your podiatrist about what you need.
Age Distribution For Diabetic Ulcers
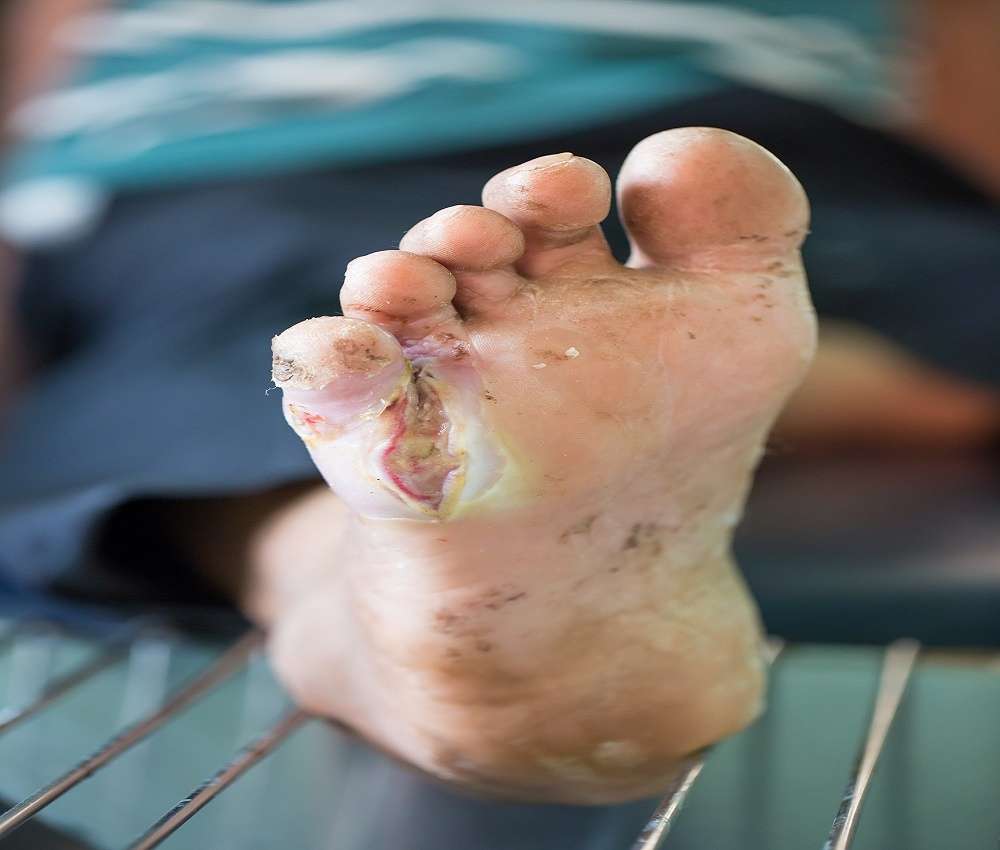
Diabetes occurs in 3-6% of Americans. Of these, 10% have type 1 diabetes and are usually diagnosed when they are younger than 40 years. Among Medicare-aged adults, the prevalence of diabetes is about 10% . Diabetic neuropathy tends to occur about 10 years after the onset of diabetes, and, therefore, diabetic foot deformity and ulceration occur sometime thereafter.
Also Check: What Can I Do For Ulcers In My Stomach
Treatment Of The Foot Ulcer Depends On The Severity Of The Wound
|
Severity |
|
|
|
|
Not infected |
|
|
Mild infection |
|
|
Moderate infection |
|
|
Severe infection |
|
How Are Foot And Toe Ulcers Treated
The goal of treating a foot or toe ulcer is to relieve pain and heal your wound. Your treatment plan will be individualized based on what medical condition is causing your ulcers. If you cant correct the cause of your ulcer, its likely to come back after treatment.
There are both surgical and nonsurgical treatments for foot and toe ulcers. For simple, early stage foot and toe ulcers, nonsurgical treatments may work. Ulcers that are more advanced, especially ones that are infected, may require surgery.
Don’t Miss: How Do I Get Rid Of A Stomach Ulcer
What Causes A Diabetic Ulcer On Your Foot
Foot ulcers are common among those with poorly managed diabetes. Anyone with diabetes can develop these ulcers, but managing your diabetes can prevent the issue. Foot ulcers require immediate attention, so once you notice any issue, its important to talk with a medical professional for help. They can provide you with treatment options in addition to finding the root cause of your foot ulcers. Below you will find more information on what specifically causes a diabetic ulcer on your feet.
What Is Diabetic Foot Ulcer
When most people hear the word ulcer they often think of the illness associated with the lining of the stomach, but in reality, this is just one type of ulcer found in or on the body. In simple terms, an ulcer involves layers of the skin breaking open and then not healing properly. Exterior skin ulcerations are usually accompanied by redness, swelling, and pain.
Read Also: Diabetic Ulcer On Big Toe