What The Start Of A Foot Ulcer Looks Like
It can be difficult for a person with diabetes to realize that they have a diabetic foot ulcer until it has already progressed. The reason for this is that many people with diabetes do not have feeling in their extremities due to poor circulation and peripheral neuropathy, so they may not feel the pain of a cut or wound.
One of the first signs of a diabetic foot ulcer that a person with diabetes may notice is drainage from the wound that stains their socks. Irritation, swelling, or an unpleasant odor may also be some of the first signs that a diabetic foot ulcer is present.
In more severe cases, a person may notice discoloration around the wound , or the skin around the wound may be callused or painful to the touch.
If these symptoms are present, immediately seek medical care, ideally with a podiatrist, to prevent the wound from getting any worse and begin treatment as needed.
How Can I Prevent Diabetic Foot Ulcers
Diabetic foot ulcers are the most common reason for hospital stays among people with diabetes.
Whats the reason? People with diabetes, not only do they not heal non-diabetics, but in addition to that, they develop a disease called diabetic neuropathy, where they lose feeling in their feet, says Arti Masturzo MD, medical director at the Bethesda North Wound Care Center.
However, with the proper precautions, Dr. Masturzo says diabetic foot ulcers can be avoided.
Custom Orthotics And Braces
To relieve pressure from an ulcer and help it heal, NYU Langone doctors can provide custom-fit orthotic shoe inserts or braces.
Orthotics, or shoe inserts, help redistribute the weight of your body across the bones and joints of your foot while you walk. These inserts are firm but soft and may contain foam or gel to support your foot and make walking more comfortable.
Our doctors can create inserts with soft, donut-shaped padding to surround and support an ulcer. This helps relieve pressure and protect the ulcer from friction when you wear shoes. A custom shoe insert can also shift weight away from the area of the injury to further relieve pressure and help the ulcer heal.
If your doctor recommends taking more weight off of the affected foot, he or she can provide a custom-fit brace that is worn over the foot and leg. There are many types of braces. One version, called a patellar tendon bearing brace, shifts the weight of the body off of the affected part of the foot and onto the strong tendon in the front of the knee, called the patellar tendon.
Our diabetic foot specialists take a mold of your foot to ensure that the custom orthotic insert or brace fits you well and is comfortable. It takes about two weeks for the device to be made, at which time your doctor schedules an appointment to show you how to use it.
Read Also: Hand Foot And Mouth Ulcers
Will An Diabetic Foot Ulcer That’s Been There For A Long Time Ever Heal
So you have a diabetic foot ulcer that just won’t heal. Or maybe it has healed but keeps coming back. I’m sure you are frustrated and feel that it may never heal. In some cases you may have dressed your wound with the same medication for months…even years!
A diabetic foot ulcer should show continuous progress towards healing. If your wound stops healing, there must be a reason why or a change in therapy is needed. First of all, no ulcer will heal if there is not a sufficient blood supply to the foot. Poor circulation is common in people with diabetes. At our Houston podiatry practice, we use a non-invasive, painless system for evaluating your circulation called PADnet. Everyone with diabetes should be evaluated for circulation. Restoring circulation will help your wound to heal.
The underlying cause of your diabetic foot ulcer is pressure. This same pressure that initially caused the wound will prevent it from healing. For this reason, management of your ulcer must include the relief of pressure. The is achieved by casting, wearing a surgical boot, or surgical shoe. If you are not wearing something to manage these pressures, you should ask your doctor or get a second opinion from another podiatrist in Houston.
Taking Pressure Off Your Foot Ulcer
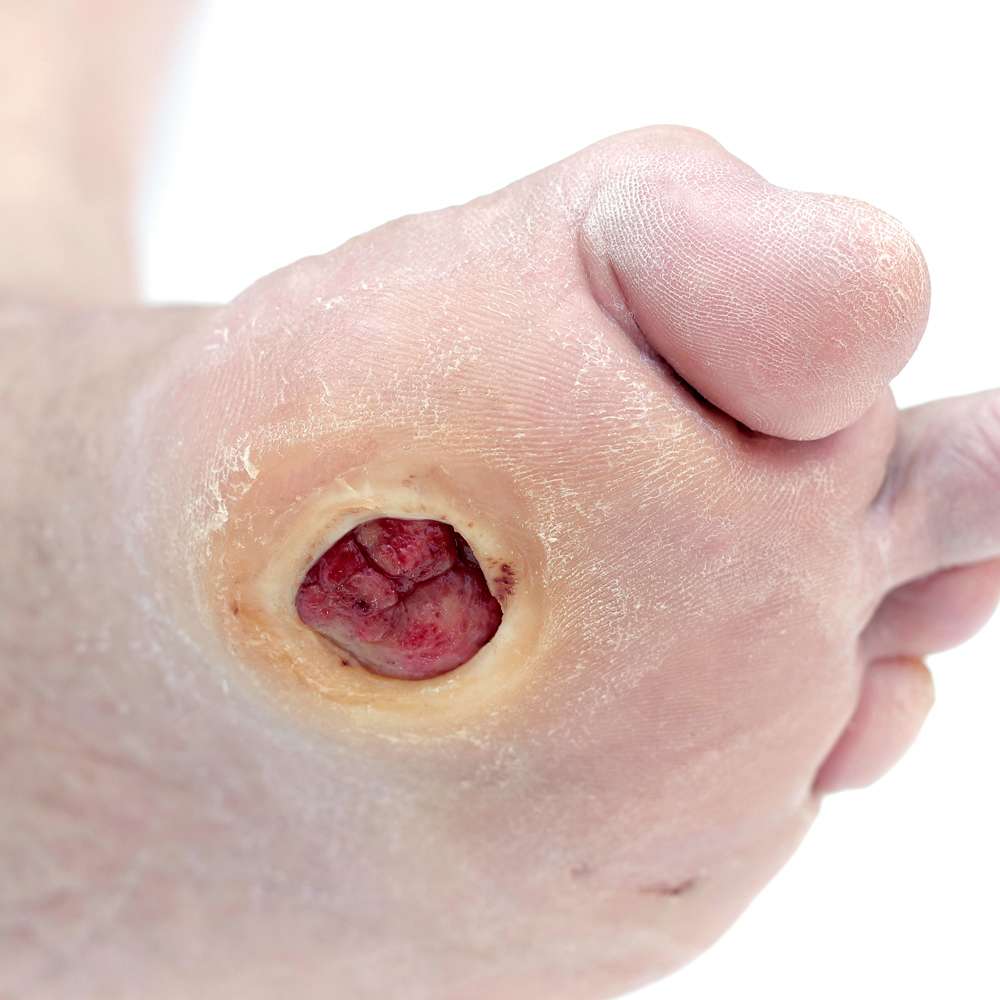
Foot ulcers are partly caused by too much pressure on one part of your foot.
Your provider may ask you to wear special shoes, a brace, or a special cast. You may need to use a wheelchair or crutches until the ulcer has healed. These devices will take the pressure off of the ulcer area. This will help speed healing.
Sometimes putting pressure on the healing ulcer for even a few minutes can reverse the healing that happened the whole rest of the day.
Be sure to wear shoes that do not put a lot of pressure on only one part of your foot.
- Wear shoes made of canvas, leather, or suede. Don’t wear shoes made of plastic or other materials that don’t allow air to pass in and out of the shoe.
- Wear shoes you can adjust easily. They should have laces, Velcro, or buckles.
- Wear shoes that fit properly and are not too tight. You may need a special shoe made to fit your foot.
- Don’t wear shoes with pointed or open toes, such as high heels, flip-flops, or sandals.
Read Also: Air Mattress For Decubitus Ulcers
Proper Dressing Infection Control And Offloading
Its essential to use the proper types of wound dressing, infection control, and offloading to prevent your diabetic wound from regressing during or after treatment.
The best wound dressing maintains a healthy amount of moisture on the foot to create a favorable environment for the wound. It must be changed at least once or twice per day, depending on the stage and severity of the ulcer. Wound dressing helps control infection, as do antibiotics.
Offloading is also a very important but often overlooked component of diabetic foot ulcer treatment. When you offload, you remove pressure from your injured foot and give new, healthy cells the opportunity to thrive. Crushes, knee scooters, and wheelchairs all accomplish offloading.
Where Does An Ulcer Appear
There are many different kinds of ulcers. While peptic ulcers form in the stomach or upper intestine lining, ulcers can also occur almost anywhere on the body.
Ulcers that are found outside the body can include leg and foot ulcers. These ulcers are generally swollen or tender and can cause itchiness or pain. Skin discoloration and changes in texture are also common in ulcers found outside the body.
Whether they are found inside or on the skinâs surface, ulcers are sores that are often slow to heal. Once they have disappeared, ulcers can return if not treated properly. Depending on the cause of the ulcers, they can require different treatment options.
Don’t Miss: What Doctor Treats Ulcerative Colitis
The Wagner Diabetic Foot Ulcer Classification System
Occasionally referred to as the Merritt-Wagner system, the Wagner DFU system was invented in the 1970s. Despite its simplicity with regard to grades, it is also considered highly accurate in predicting the outcome of an ulcer and the likelihood of lower extremity amputation.7
The Wagner DFU system is the system that is required to be used for patients who have Medicare as their primary insurance. Certain treatments, such as hyperbaric oxygen therapy, cannot be considered or covered for a patient unless they are staged as Grade 3 or higher and have not had results with conventional treatment over a period of 30 days.8
Intact skin
Grade 5
Why Are Dfus So Hard To Heal
Poor circulation and high blood glucose levels are some of the leading reasons why wounds dont heal in diabetics. Elevated blood glucose can cause your blood vessels to narrow, and your platelets to grow larger, making it difficult for oxygen and nutrients to reach your wound site.
Another reason why wounds dont heal in diabetics is that high glucose levels inhibit your white blood cells, hindering your immune response. When you get a diabetic wound, its much more difficult for your body to heal and to fight off infection.
Once you notice you have an ulcer, its important to seek podiatric medical care for diabetes foot wound healing as soon as possible. If not managed properly, complications with infection can lead to osteomyelitis, amputation, and, in extreme cases, even death.
That being said, there are plenty of diabetic wound healing products and supplements you can use to properly manage your diabetes foot wound healing.
And of course, the best defense is to prevent your DFUs from happening in the first place!
Don’t Miss: Budesonide Vs Prednisone For Ulcerative Colitis
Why Are Diabetics Prone To Foot Ulcers And Other Chronic Wounds
Diabetic patients are more prone to developing chronic wounds for a few reasons. Two of the most influencing factors are nerve damage and blood circulation issues that are common among diabetic patients.
Nerve damage, or neuropathy, tends to occur in patients who have a longer history with diabetes because elevated blood glucose levels damage nerves over time. Neuropathy causes patients to experience reduced, or lack of, sensation in the areas affected.
Many patients can sustain trauma or develop an infection without realizing it because theyre unable to feel pain in the area. Further, neuropathy commonly affects the feet, so a wound on the bottom of the foot can escalate quickly because the patient cannot feel or see the wound easily.
Blood circulation issues also can increase the risk for developing chronic wounds, as well as making the wounds more prone to infection. High blood glucose levels cause the narrowing of blood vessels, which constricts blood supply, Estocado said. Adequate blood supply is essential to normal wound healing. The secondary effect of impaired blood supply is a decrease in white blood cells, which are responsible for fighting infection and maintaining a strong immune system.
What Are The Risk Factors For Diabetes Foot Ulcers
The following can increase the likelihood of developing a foot ulcer:
- Wearing poor fitting footwear
- Walking barefoot
People who have diabetes for a longer period or manage their diabetes less effectively are more likely to develop foot ulcers. Smoking, not taking exercise, being overweight, having high cholesterol or blood pressure can all increase diabetes foot ulcer risk.
Don’t Miss: Home Remedies For Dog Mouth Ulcers
Preventing Diabetic Foot Ulcers
There are several ways to prevent a foot ulcer. In addition to daily checks of your feet for any signs of an ulcer or other abnormality, the following can be done to help with prevention:
- Never walk barefoot, and always wear socks to protect your feet
- Wear shoes that fit properly and do not rub
- Keep your blood sugar under control and monitored
- Eat a healthy diet
- Avoid alcohol and tobacco products
- Seek immediate medical attention if you have a foot wound that is not healing
What Is A Diabetic Foot Ulcer
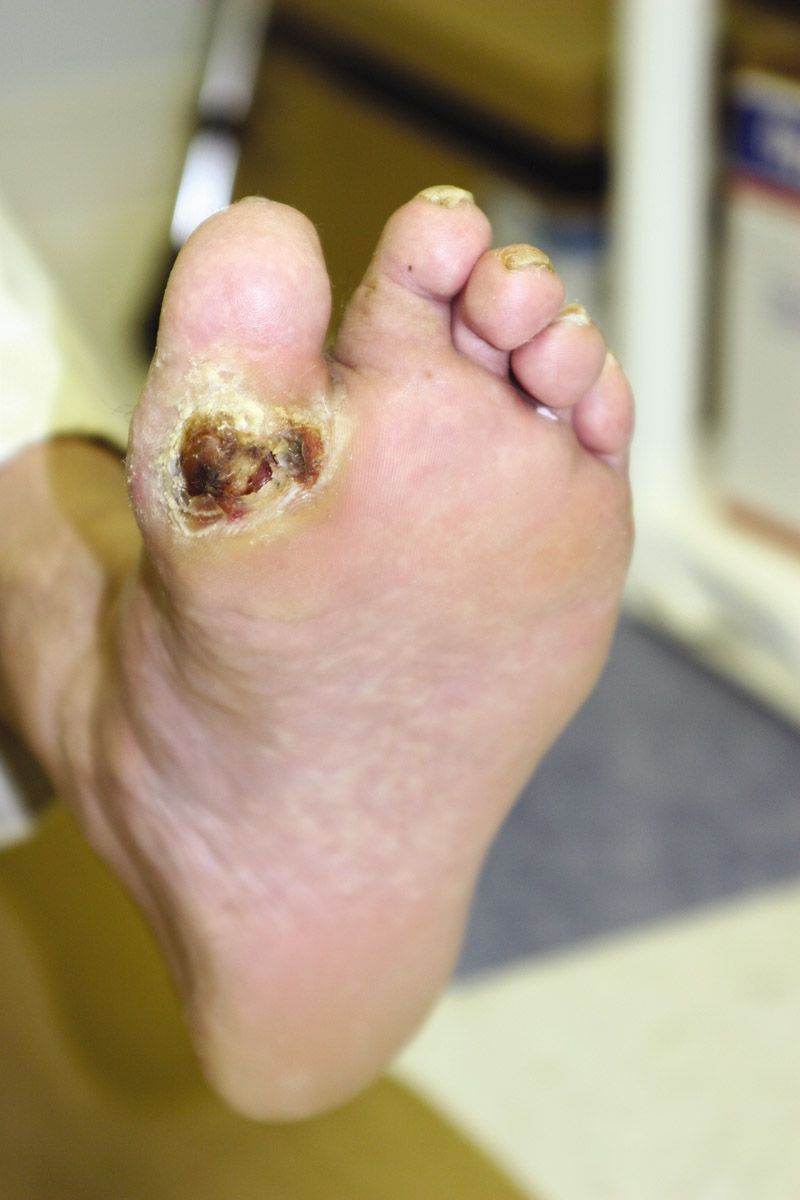
A diabetic foot ulcer is an open sore or wound that occurs in approximately 15 percent of patients with diabetes, and is commonly located on the bottom of the foot. Of those who develop a foot ulcer, six percent will be hospitalized due to infection or other ulcer-related complication.
Diabetes is the leading cause of nontraumatic lower extremity amputations in the United States, and approximately 14 to 24 percent of patients with diabetes who develop a foot ulcer have an amputation. Research, however, has shown that the development of a foot ulcer is preventable.
Read Also: What Can You Take For Ulcer Pain
How Is A Diabetic Foot Ulcer Diagnosed And Treated
Your healthcare provider will ask about your symptoms and examine your foot and the ulcer. He or she may check your shoes. He or she may also send you to a podiatrist for treatment. The goal of treatment is to start healing your foot ulcer as soon as possible. The risk for infection decreases with faster healing. Do the following to help your ulcer heal:
Diagnosing A Diabetic Ulcer
An accurate diagnosis of a diabetic ulcer must be given by a medical health professional. Most doctors will first provide a physical examination of the patients foot. Should further tests be required, a doctor may recommend an X-ray or an MRI scan.
An X-ray can show any changes in foot alignment through a system of imaging. An X-ray image can show loss of bone mass and hormonal imbalances that can potentially relate to the diagnosis of diabetes.
MRI scans use three-dimensional images of the bodys soft tissue. If the extent of damage needs to be assessed, an MRI scan can use magnetic radio waves to reveal possible inflammation. This test can expose any significant infections in the foot.
One of the simplest tests a physician can use to diagnose an infectious diabetic ulcer is the blood test. This test is usually done by drawing blood at a doctors office so that the results can be sent to a lab for further information.
Read Also: Side Effects Of Ulcerative Colitis
The Role Of Pedorthics
Dennis Janisse, CPed, reiterates Hinkess emphasis on patient responsibility.
You can usually tell fairly quickly if youre dealing with someone who is going to take responsibility for themselves, said Janisse, who is assistant professor of physical medicine and rehabilitation at the Medical College of Wisconsin, and president and CEO of National Pedorthic Services Inc., headquartered in Milwaukee. If they dont, it dramatically increases the risk of reulceration.
Not surprisingly for a pedorthist, Janisse considers proper footwear and well-designed orthoses essential to preventing ulcer recurrence. In a 2004 paper he coauthored, for example, researchers found that rocker soles successfully redistributed forefoot pressures in 40 patients, suggesting the soles potential for offloading problem areas.14
Its important to work with a physician who understands the importance of using pedorthics for conservative management of the diabetic foot, he said. The doctors we work with will tell you that our amputation rate is much lower than the national average.
If the wound is on the leg and it closes, then fine, you can forget about it, he said. But if its on the foot, they may get it healed, but they have no idea what to do after that to prevent further ulceration. We have to do appropriate patient education.
How Are Foot And Toe Ulcers Treated
The goal of treating a foot or toe ulcer is to relieve pain and heal your wound. Your treatment plan will be individualized based on what medical condition is causing your ulcers. If you cant correct the cause of your ulcer, its likely to come back after treatment.
There are both surgical and nonsurgical treatments for foot and toe ulcers. For simple, early stage foot and toe ulcers, nonsurgical treatments may work. Ulcers that are more advanced, especially ones that are infected, may require surgery.
You May Like: Ulcers In Small Bowel Crohn’s
Risk Of Bias Within Studies
The quality assessment scores obtained ranged between four and six, indicating moderate methodological quality of included studies. As it is not possible to blind both the participant and treating therapist, studies in this review were not able to achieve a score greater than eight out of ten on the PEDro scale. The PEDro scale scoring of the included studies is shown in Fig. .
Fig. 2
What Do Ulcers Look Like
Ulcers are wounds in your skin shaped like circles or ovals and can vary in size and color. When an ulcer starts you may notice:
- Dry skin.
- Redness.
- A rash.
As the ulcer gets worse, it can get wider, longer and deeper sometimes all the way down to the bone. In advanced stages you may see:
- A callus.
- A halo around the center that gets hard.
- Drainage in your sock, which may mean you have an infection.
- A brown discoloration.
You May Like: Interprofessional Care For Ulcerative Colitis
Healing Factors Of Foot Ulcers
The healing time depends on various factors. It could be the wound size, location, pressure on the ulcer while walking or standing for a long time, blood circulation, swelling, glucose levels, and treatment and dressing given to the ulcer. Healing may occur within weeks, months, or years based on different stages of Foot ulcers.
There are newer products available in the market for treating foot ulcers, and one such innovation is MaxioCel. It is a next-generation wound care dressing made of chitosan, which provides maximum comfort and faster healing to patients suffering diabetic foot ulcers and other chronic wounds.
MaxioCel is a highly absorbent wound dressing, designed to heal patients suffering from diabetic foot ulcers, bedsores, and chronic wounds by effectively managing exudates, pain, and scar improvement. It can be used for moderate to heavily exudating wounds of varied depth, shape and size.
Juwariah Khan
Treating Diabetic Wounds And Helping Them Heal Quicker
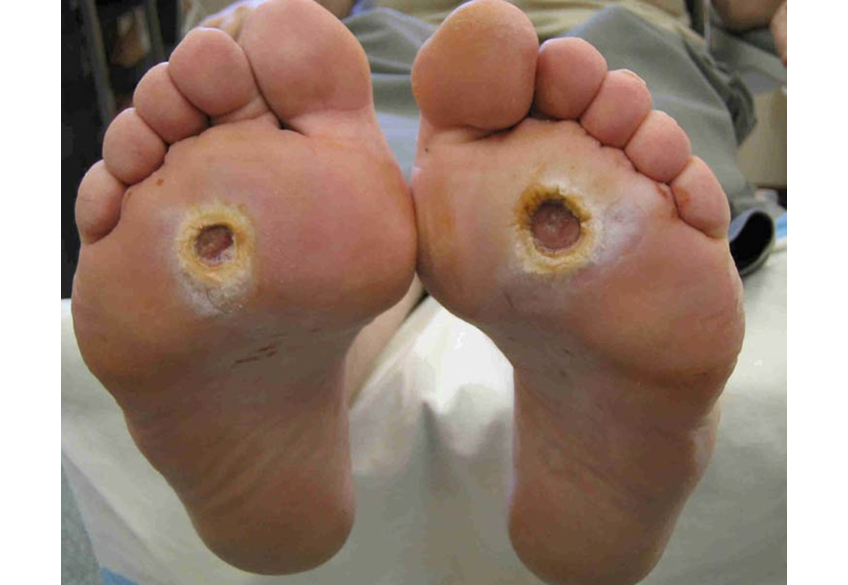
At Encompass Healthcare, Dr. Bruce Ruben and his team of wound doctors treat diabetic wounds on a daily basis.
We see a lot of different types of non-healing wounds from patients with Diabetes and were asked how to help these wounds heal . Here are some treatment processes you can do at home to ensure these wounds do not become bigger health concerns.
First, and very importantly, find any cuts you have, including scrapes, and treat these wounds immediately.
If you treat new wounds right away, you can start caring for them before things get bad.
As soon as you find a cut or sore:
+Wash your hands with soap and water.+Rinse off the wound with warm water.+Apply pressure to stop any bleeding.+Apply antibiotic cream and cover with a bandage.
Also, if you dont know you have a wound, you cant treat it quickly. So if you suffer from neuropathy, keep an eye out for new wounds. Check your hands and feet daily, and dont forget to check between your toes.
Wearing white athletic socks can help, too. If you see a red spot or a place where your sock is sticking to your skin, check your foot to see if you have a wound thats new or not healing.
Take pressure off the area if your wound continues to reopen or experience damage, it wont heal quickly and may get much worse. So avoid putting stress, pressure and weight on wounds.
Keep your wound clean and covered with the right dressings
Common types of dressings for diabetic wound care:
Foot ulcers or wounds
You May Like: Artificial Sweeteners And Ulcerative Colitis