Medical History And Examination
Your GP or practice nurse will ask whether you have any other symptoms associated with venous leg ulcers, such as:
- swelling in your ankles
- discoloured or hard skin
They’ll try to determine the cause of the ulcer by asking about underlying conditions or previous injuries, such as:
Read more about how venous leg ulcers are treated.
What Is Venous Stasis Ulcer
Contents
Venous stasis ulcer is a common type of leg and foot ulcer. Venous ulcers are open sores that do not heal or keeps on recurring. These ulcers are situated below the knee and mainly develop on the inner part of the leg above the ankle. It could possibly affect both legs.
They are red in color that can be coated with yellow fibrous tissue, but yellow or green discharge can also be found if there is infection. The shape of the wound is usually irregular and the skin around the sore is swollen and discolored. It might even feel hot or warm.
The skins appearance may look tight and shiny due to the swelling. Venous stasis is commonly seen in individuals who have had a history of varicose veins, leg swelling, or blood clots. This ulcer is accountable for about 80 to 90 percent of leg ulcer cases and affects more females than males. It often occurs to older individuals.
Referral To A Specialist
In some cases, your GP or nurse may decide to refer you to a specialist in conditions affecting the blood vessels .
For example, you may be referred to a vascular specialist if your GP or nurse is unsure about your diagnosis, or if they suspect your ulcer may be caused by artery diseases, diabetes or rheumatoid arthritis.
After taking your medical history and examining you, the vascular specialist may need to arrange further investigations to plan your treatment.
Recommended Reading: How Can You Tell You Have An Ulcer
The Role Of The Pharmacist In Educating Patients About Vsus
Since pharmacists are often perceived as one of the most accessible healthcare professionals, they have a critical role in the treatment and care of patients at risk of, or with, VSUs. This includes effective patient counseling and education, especially with regard to therapy for VSUs, proper use of medications used to treat VSUs, and reminders about preventive measures to decrease reoccurrence of VSUs. Since the incidence of VSUs is common in elderly and diabetic patient populations, pharmacists play a key role in identifying those patients at greater risk of developing VSUs. Pharmacists should also seize every possible opportunity to remind patients about the critical importance of adhering to therapy to enhance therapeutic outcomes and prevent further complications.
Pharmacists can also reinforce patient education with regard to the preventive measures for VSUs such as staying vigilant about oneâs overall health and adhering to the goals of therapy. Patients should be reminded of the importance of routine wound care and follow-up with their primary healthcare provider, monitoring the ulcer for signs of infection, and immediately seeking medical attention if the wound shows signs of worsening or not healing. Patients at risk for VSUs should be aware that with early diagnosis and implementation of and adherence to therapy, the condition can be effectively treated and healed to avoid complications.
Can Venous Leg Ulcers Be Prevented
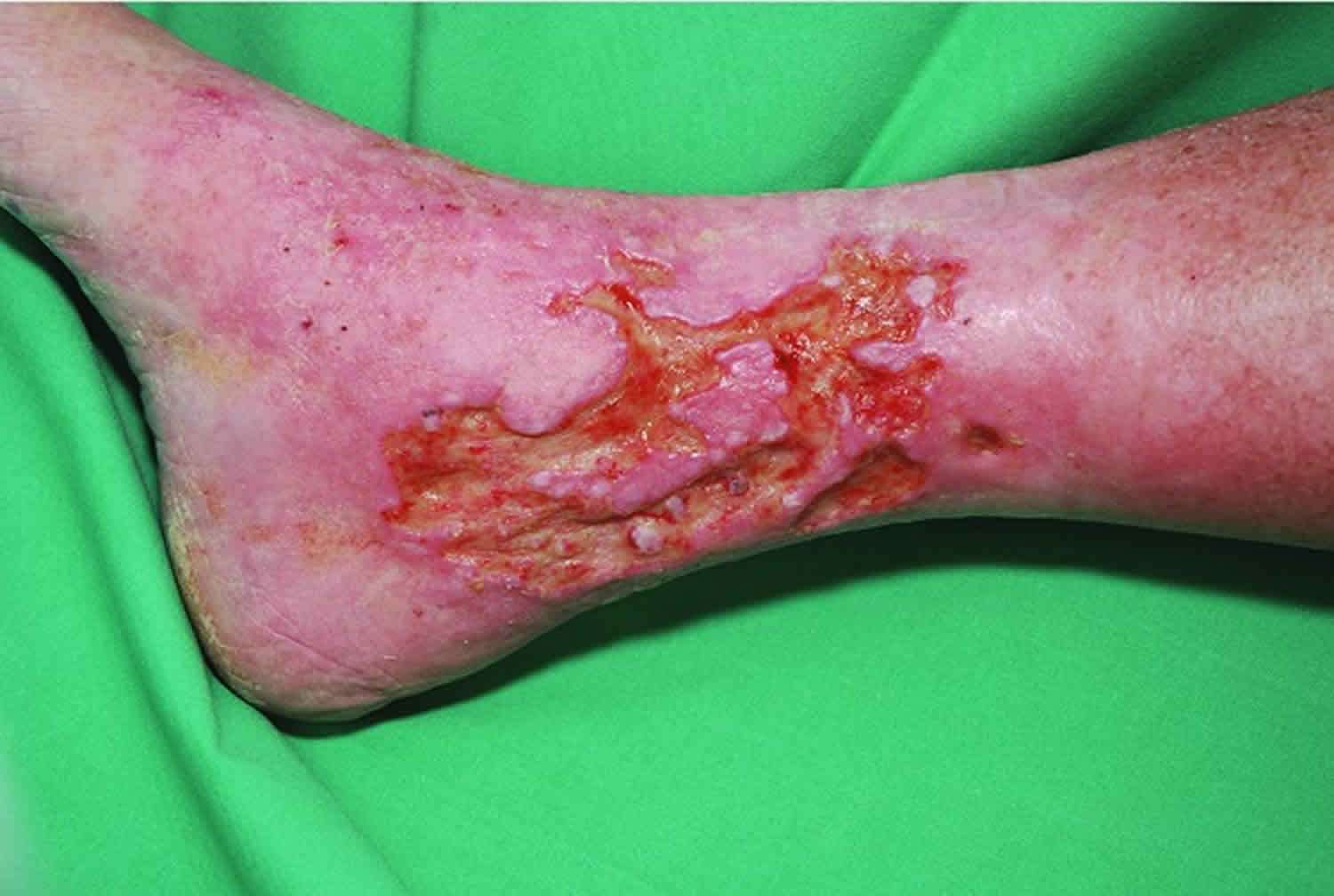
There are several ways to help prevent a venous leg ulcer in people at risk, such as:
- wearing compression stockings
- losing weight if you’re overweight
- exercising regularly
- elevating your leg when possible
This is particularly important if you’ve previously had a leg ulcer once a leg has suffered a venous ulcer, you’re at risk of further ulcers developing within months or years.
Read more about preventing venous leg ulcers.
Also Check: What Is The Best Treatment For Ulcerative Proctitis
How Venous Leg Ulcers Are Treated
Most venous leg ulcers heal within 3 to 4 months if they’re treated by a healthcare professional trained in compression therapy for leg ulcers. However, some ulcers may take longer to heal, and a very small number never heal.
Treatment usually involves:
- cleaning and dressing the wound
- using compression, such as bandages or stockings, to improve the flow of blood in the legs
Antibiotics may also be used if the ulcer becomes infected, but they don’t help ulcers to heal.
However, unless the underlying cause of the ulcer is addressed, there’s a high risk of a venous leg ulcer recurring after treatment. Underlying causes could include immobility, obesity, previous DVT, or varicose veins.
What Causes Venous Stasis Ulcers
3.9/5causevenous ulcersveinsveinsveinsvenous insufficiencyof the answer
Venous skin ulcers are caused by poor blood circulation from the legs, such as from venous insufficiency. Your veins have one-way valves that keep blood flowing toward the heart. In venous insufficiency, the valves are damaged, and blood backs up and pools in the vein.
Secondly, how can venous stasis ulcers be prevented? Preventing venous ulcers
Similarly, you may ask, what is the best treatment for venous stasis ulcers?
Compression therapy has been proven beneficial for venous ulcer treatment and is the standard of care. Leg elevation minimizes edema in patients with venous insufficiency and is recommended as adjunctive therapy for venous ulcers. The recommended regimen is 30 minutes, three or four times per day.
What causes ulcers on the lower legs?
arterial leg ulcerscaused by poor blood circulation in the arteries. diabetic leg ulcerscaused by the high blood sugar associated with diabetes. vasculitic leg ulcers associated with chronic inflammatory disorders such as rheumatoid arthritis and lupus. traumatic leg ulcerscaused by injury to the leg.
To help treat a venous ulcer, the high pressure in the leg veins needs to be relieved.
Also Check: Support Surfaces For Pressure Ulcer Prevention
What Causes These Ulcers
Poor blood circulation often causes ulcers. When theres reduced blood flow, skin and tissues in the affected areas are deprived of oxygen and nutrients. These areas will become inflamed and form an open wound.
Though ulcers can form anywhere on the body, arterial and venous ulcers are more commonly found on the legs and feet.
Identifying The Cause Of Venous Ulcers
The root of the problem is increased pressure of blood in the veins of the lower leg. This causes fluid to ooze out of the veins beneath the skin, followed by swelling, thickening, and damage to the skin. The damaged skin may eventually break down to form an ulcer.The increased pressure of blood in the leg veins is due to blood pooling in the smaller veins next to the skin. This pooling occurs because the valves in the larger veins are damaged by a previous thrombosis causing blockage of the vein, or by weakening of the walls of the veins causing the valves to malfunction,as in varicose veins. When the valves no longer function properly gravity causes blood to backflow down the leg in the erect individual and pool in the lower leg veins. This produces high pressure in the veins which results in damage to the surrounding tissue and ultimately to skin breakdown and ulceration.
Read Also: Can Diet Help Ulcerative Colitis
Spider Vein Treatment Coststarting At $250
What is the cost of sclerotherapy? Very simple, Sclerotherapy costs start at $250 per leg. Touch-up or follow-up is $100.
Sclerotherapy is a very popular procedure used to treat deficient blood vessels. Medicine is injected, using a very small gauge needle, into the veins that act as an irritant of the inner vein walls, causing closure of the treated spider vein. Most patients require multiple sessions, however, the number of treatments is based on your specific condition.
Over time, the appearance of spider veins fade from sight, leaving you with clearer, healthy looking legs. Your spider vein specialist is able to treat more than one vein at the same time.
Together well get you to love your legs!
Our state-of-the-art Pulsed Dye Laser and Intense Pulsed Light delivers an intense but gentle burst of light into selectively targeted areas of the skin. The light is absorbed by specific blood vessels or melanin pigmented areas in the dermis depending on the condition being treated. Factors such as the age, color and type of lesions, as well as the location on the body, all determine whether lesions can be removed. The Harmony DYE VL we utilize will help fade vascular lesions to look like normal skin.
Signs Of An Infection
A venous leg ulcer can be susceptible to bacterial infection. Symptoms of an infected leg ulcer can include:
- worsening pain
A number of factors can increase your risk of developing a venous leg ulcer, including:
- obesity or being overweight this increases the pressure in the leg veins
- if you have difficulty walking this can weaken the calf muscles, which can affect circulation in the leg veins
- previous deep vein thrombosis blood clots that develop in the leg can damage valves in the veins
- varicose veins swollen and enlarged veins caused by malfunctioning valves
- previous injury to the leg, such as a broken or fractured bone, which may cause DVT or impair walking
- previous surgery to the leg, such as a hip replacement or knee replacement, which can prevent you from moving about
- increasing age people find it harder to move around as they get older, particularly if they suffer from arthritis
Don’t Miss: Whey Protein And Ulcerative Colitis
Cleveland Clinic Heart Vascular & Thoracic Institute Vascular Medicine Specialists And Surgeons
Choosing a doctor to treat your vascular disease depends on where you are in your diagnosis and treatment. The following Heart, Vascular & Thoracic Institute Sections and Departments treat patients with all types of vascular disease, including blood clotting disorders:
Section of Vascular Medicine: for evaluation, medical management or interventional procedures to treat vascular disease. In addition, the Non-Invasive Laboratory includes state-of-the art computerized imaging equipment to assist in diagnosing vascular disease, without added discomfort to the patient. Call Vascular Medicine Appointments, toll-free 800-223-2273, extension 44420 or request an appointment online.
Department of Vascular Surgery: surgery evaluation for surgical treatment of vascular disease, including aorta, peripheral artery, and venous disease. Call Vascular Surgery Appointments, toll-free 800-223-2273, extension 44508 or request an appointment online.
You may also use our MyConsult second opinion consultation using the Internet.
The Heart, Vascular & Thoracic Institute also has specialized centers and clinics to treat certain populations of patients:
What Is The Treatment For A Venous Leg Ulcer
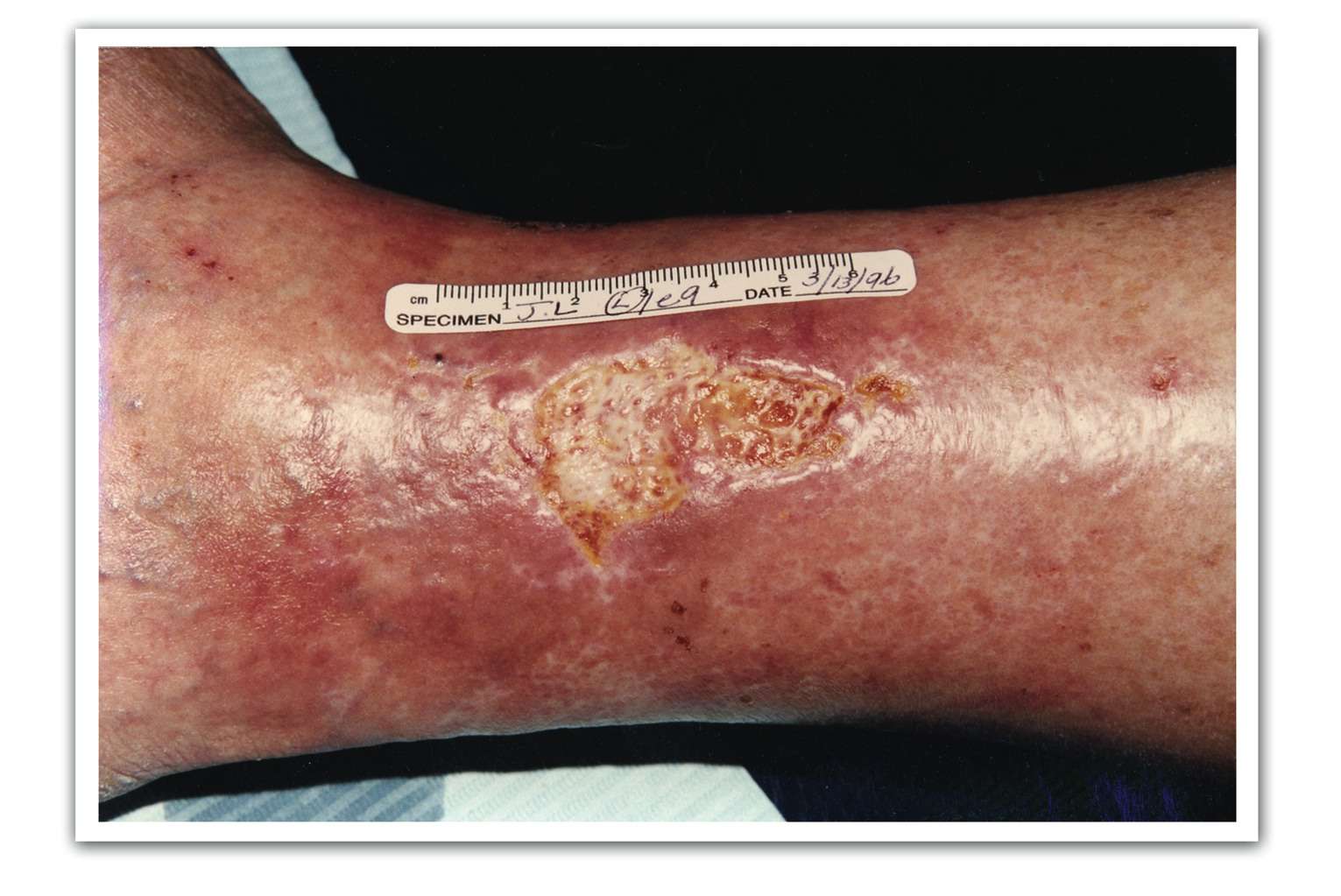
A venous leg ulcer usually wont get better without treatment from a healthcare professional. The aim of treatment is to make sure the wound heals while providing relief from symptoms such as pain in and swelling of your affected leg.
Your GP may recommend specialist wound care and compression therapy to help with healing. Treatment will usually be done by a district nurse who is specifically trained to manage leg ulcers.
Compression therapy applies pressure to your affected leg, which reduces the amount of blood pooling in the veins and helps to redirect the blood flow to your heart. It can help to reduce swelling and encourages delivery of oxygen and nutrients, critical for healing, to the wound.
Your GP may consider referral to a vascular surgeon to discuss a minimally invasive procedure for varicose veins. This will reduce the risk of recurrent ulcers.
You May Like: Can I Eat Oatmeal With Ulcerative Colitis
Venous Ulcer Diagnosis And Treatment
Doctors at Vascular surgeons at UPMC’s Heart and Vascular Institute use duplex ultrasound, a noninvasive test, to diagnose abnormal veins that cause venous ulcers. Part of the UPMC difference is that we actively look for the causes of the ulceration to treat venous pathology and keep the ulcer healed.
After an evaluation of your veins, we recommend a treatment plan based on your needs:
- Compression
- Compression of the leg is vital to healing venous wounds.
- Compression stockings are most commonly used for this treatment.
- The pressure from the compression dressing counteracts the pressure from the veins of the leg and allows skin to heal.
What Are Some Symptoms Of Venous Stasis Ulcers
- Skin Color ChangesPrior to the skin opening up into an ulcer you may notice changes to the appearance of your skin. Thinning, scaling, and peeling of the skin can occur. Skin color may change to red, brown, or yellow. Dark red or purple coloration can appear as well.
- UlcersAn ulcer is an opening of the skin. Venous stasis ulcers develop on the legs and are normally close to the surface of the skin and not very deep. These ulcers can get large. Their shape is normally that of an oval or circle, but irregularly shaped ulcers can also develop with curvy margins.
- DrainageSometimes there is drainage from the opening in the skin. This can take on different appearances. Sometimes it looks like clear fluid, just like water dripping down the leg. Other times this drainage can have red or yellow color and be thicker than water. This drainage can also look like oozing blood.
- PainWhile venous stasis ulcers can be painless for some, other people do experience pain associated with the ulcer. For some, the pain is worse if the swelling increases. Others may experience pain when something touches the area where the ulcer is. When this pain occurs, it may be worse when walking.
Read Also: Does Stomach Ulcer Cause Pain
How Are Stasis Ulcers Diagnosed
Stasis ulceration is usually a clinical diagnosis, made on the basis of the patient’s history and examination findings, and includes the presence of risk factors for venous stasis, that is, congestion and slowing of venous circulation, and the characteristic features of the wound and surrounding tissues.
- Duplex ultrasonography is used to confirm venous obstruction or valvular incompetence prior to saphenous vein ablation surgery
- Concomitant arterial disease is identified using the ankle-brachial index
Other investigations to evaluate venous insufficiency and provide haemodynamic information may include:
- Intravenous ultrasonography
- Ascending or descending venography/phlebography
- Venous air plethysmography
- Haematological studies of the coagulation system.
Preventing Venous Insufficiency And Venous Ulcers
Fortunately, venous insufficiency and venous ulcers, along with their complications, can be prevented through a number of lifestyle changes.
Cigarette smoke is a vascular constrictor, which means it tightens the veins and arteries in the body. As a result, smokers are more likely to experience circulatory problems, so its important to quit smoking to prevent venous insufficiency from progressing.
Obesity is also a big risk factor in venous insufficiency. Reaching a healthy weight through diet and lifestyle changes is an effective way to reduce the pressure on the veins in the lower leg, which subsequently alleviates many of the symptoms of venous insufficiency.
Many underlying conditions have venous insufficiency as a potential complication. Individuals with high blood pressure or diabetes are more likely to develop venous insufficiency and venous ulcers, so efforts should be made to correct these conditions with the help of a physician.
Regular exercise promotes healthy circulation and reduces swelling in the lower legs. Individuals with a sedentary lifestyle are more likely to experience circulatory problems and venous insufficiency, so its important to have an active lifestyle. This could be as simple as short walks, light jogs or riding a stationary bike a few times a week. Mild stretching also helps to improve blood flow in the legs.
You May Like: What Is Refractory Ulcerative Colitis
Swelling In The Legs And Ankles
Venous leg ulcers are often accompanied by swelling of your feet and ankles , which is caused by fluid. This can be controlled by compression bandages.
Keeping your leg elevated whenever possible, ideally with your toes at the same level as your eyes, will also help ease swelling. You should put a suitcase, sofa cushion or foam wedge under the bottom of your mattress, to help keep your legs raised while you sleep.
You should also keep as active as possible and aim to continue with your normal activities. Regular exercise, such as a daily walk, will help reduce leg swelling. However, you should avoid standing or sitting still with your feet down. You should elevate your feet at least every hour.
What Are The Causes Of A Venous Leg Ulcer
Venous leg ulcers develop because of problems with the blood circulation in your leg veins. Valves in your legs help to push blood from your legs and feet back up towards your heart. If these valves become damaged, the blood pools in the leg veins, causing pressure symptoms and skin changes.
Often an ulcer will develop after a minor injury to your leg, and because of blood circulation problems, the wound fails to heal.
Youre more at risk of developing a venous leg ulcer if you:
- are overweight
- have a history of deep vein thrombosis
- have had a previous venous leg ulcer
- are aged over 60.
Also Check: Ulcerative Colitis Is It Deadly
Diagnosis And Treatment Of Venous Ulcers
LAUREN COLLINS, MD, and SAMINA SERAJ, MD, Thomas Jefferson University Hospital, Philadelphia, Pennslyvania
Am Fam Physician. 2010 Apr 15 81:989-996.
Patient information: See related handout on venous ulcers, written by the authors of this article.
Venous ulcers, or stasis ulcers, account for 80 percent of lower extremity ulcerations.1 Less common etiologies for lower extremity ulcerations include arterial insufficiency prolonged pressure diabetic neuropathy and systemic illness such as rheumatoid arthritis, vasculitis, osteomyelitis, and skin malignancy.2 The overall prevalence of venous ulcers in the United States is approximately 1 percent.1 Venous ulcers are more common in women and older persons.36 The primary risk factors are older age, obesity, previous leg injuries, deep venous thrombosis, and phlebitis.7
Venous ulcers are often recurrent, and open ulcers can persist from weeks to many years.810 Severe complications include cellulitis, osteomyelitis, and malignant change.3 Although the overall prevalence is relatively low, the refractory nature of these ulcers increase the risk of morbidity and mortality, and have a significant impact on patient quality of life.11,12 The financial burden of venous ulcers is estimated to be $2 billion per year in the United States.13,14