Frequent Urination And Swollen/bloated Abdomen Ulcerstive Colitis
carlacupcake
Hello All
Does anyone experience frequent urination and a swollen/bloated/heavy/tender abdomen with UC flare? I have managed my UC well over the last few years, mainly through diet. I’ve had mild flares in the past, but I don’t usually present with these symptoms. There could be another reason for these symptoms, but now I’m thinking it’s the UC. Thoughts anyone? Any help or advice is greatly appreciated x
0 likes, 10 replies
-
6 years ago
Hi Carlacupcake, I’m yet to be diagnosed but specialist suspects I have UC.
I do get a bloated abdomen and it does get very sorry. Is it possible though that maybe you have a urine infection? X
-
6 years ago
Hi Zoe
Thanks very much for your reply. I was initially treated for a UTI with antibiotics, but no joy. I didn’t think I had a UTI – no culture found in urine either. My UC was diagnosed about 8 years ago and I manage it really well – through diet. I’ve had mild flare ups, but have never had the swollen/heavy abdomen and frequent urination. I’m currently being investigated for possible cyst or fibroid, as a follow on from UTI as these can cause same symptoms. I have a transvaginal scan on Mon and if all fine, I’ll ask for a referral to a gastro to look at my UC and bowel… Lovely! How are you feeling and what symptoms do you have? x
What Causes Ulcerative Colitis
Experts dont know what causes ulcerative colitis.
It may be that a virus or bacteria affect the bodys infection-fighting system . The immune system may create abnormal redness and swelling in the intestinal wall that does not go away.
Many people with ulcerative colitis have abnormal immune systems. But experts dont know if immune problems cause the disease. They also dont know if ulcerative colitis may cause immune problems.
Having stress or being sensitive to some foods does not seem to cause ulcerative colitis.
Right now there is no cure except for surgery to remove the colon.
Blood In Stool And Crohns Disease
Bleeding in Crohns disease can vary depending on the location of inflammation. If it takes place in the colon or rectum, there will be more blood present in stools.
Blood loss in Crohns disease may be due to anal fissures that develops as a complication of Crohns disease. The good news is, anal fissures can be successfully treated without surgery.
Also Check: Wound Vac For Pressure Ulcers
Diagnosis Of Pagets Disease Of The Bone:
The cause of Pagets disease of bone is unknown. Scientists suspect a combination of environmental and genetic factors contribute to the disease. Several genes appear to be linked to getting the disease.
In addition to a physical exam, X-rays, and blood tests can help confirm the diagnosis of Pagets disease of bone. X-rays and bone scan may reveal changes in the bones. While, those with Pagets disease of bone usually have elevated levels of alkaline phosphatase in their blood, which can be discovered by a blood test.
Read Also: Which Side Is Your Kidney On
How Does Blood In The Stools Appear
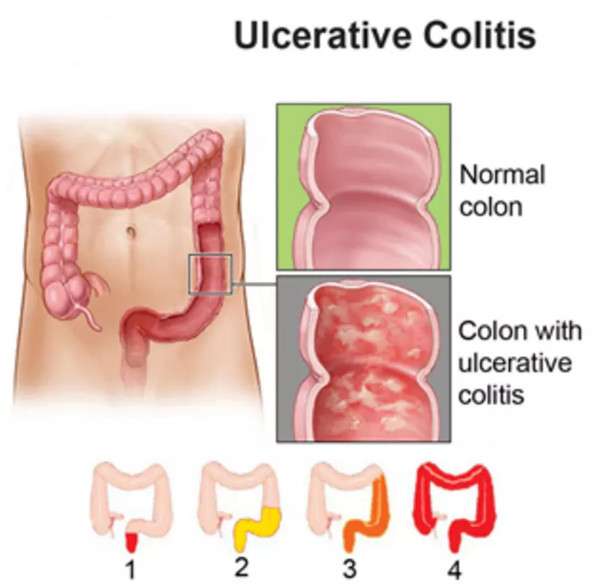
According to the Canadian Institute of Intestinal Research, most people with UC experience varying levels of hematochezia, which refers to blood in the stools. The blood will usually be clearly visible in the stool â which has a semi-solid consistency â or on the surface. The blood color can range from bright red to maroon, with or without blood clots. This symptom often accompanies lower abdominal pain and the urgent need to defecate.
Blood from the rectum and large intestine is usually bright red. If blood is a darker color, it may be coming from higher up the gastrointestinal tract.
People with UC may have slow, steady bleeding when they do not have a bowel movement. They may also experience bloody diarrhea and constipation.
Some individuals with severe UC may notice blood in their stools more than 10 times a day.
People with UC will also usually have mucus in the stools but may not be able to see it. The mucus helps protect the inner lining of the intestines, as well as helping with bowel movements.
According to the Crohnâs and Colitis Foundation, people need immediate medical attention if they experience rectal bleeding with blood clots in stools.
Read Also: How Do You Know If You Have Ulcerative Colitis
Cautions With Other Medicines
There are some medicines that affect the way mesalazine works. Tell a pharmacist or doctor if you are taking:
- medicines that make your poo more acidic, like the laxative lactulose
- medicines that affect the way your kidneys work, such as azathioprine, mercaptopurine or thioquanine, and non-steroidal anti-inflammatory drugs , such as aspirin or ibuprofen
- certain medicines that help to prevent blood clots, like warfarin
Cystitis Colitis Bladder Infection
Bladder Trouble, Weak Kidneys and Colitis Cystitis Colitis Bladder Infection
An ailment, distressingly frequent among women, has as its chief symptom a markedly increased desire to urinate. This act is attended with much distress and often with a sharp or burning painful sensation. Not infrequently the condition costs the patient a good nights sleep because of the frequency with which she must visit the bathroom.
As the urgent desire to empty the bladder may recur every few minutes, the patient is continually straining, and becomes weak and depressed. The condition may become chronic after the acute attack has subsided, and the disturbance may persist for years.
This condition is known as cystitis, though it is commonly called a cold in the bladder, since it is believed to arise from having taken cold in that organ. The true nature of the ailment is, however, an infection sometimes of the bladder and sometimes of the tubes leading from the kidneys to the bladder. In this case the doctors will tell you that pyelitis is present also.
Gynecologists often find, however, that infection may extend into the bladder from a loop of the colon which has become adherent to the bladder wall because of some infection.
WEAK KIDNEYS
Read Also: Food To Avoid For Ulcer Patient
Inflammatory Bowel Disease And Colitis
Ulcerative colitis and Crohn’s disease are the two types of inflammatory bowel disease that cause colitis. Crohn’s disease and ulcerative colitis are considered autoimmune diseases .
- Ulcerative colitis always begins in the rectum and may spread to the rest of the rest of the colon, spreading from the rectum to the sigmoid, descending, transverse, and finally the ascending colon and cecum in that order. Ulcerative colitis is considered an autoimmune disease, and symptoms include abdominal pain, and bloody, diarrheal bowel movements.
- Crohn’s disease may occur anywhere in the gastrointestinal tract , including the esophagus, stomach, small intestine, and colon. In Crohn’s disease, there may be “skip lesions,” that is, abnormal segments of the GI tract interspersed with normal segments.
Both Crohn’s disease and ulcerative colitis may have other organ systems involved in addition to the gastrointestinal tract.
Either collagen or lymphocytes infiltrate into the layers of the wall of the colon, presumably as a result of inflammation. This is an uncommon illness and maybe an autoimmune disease. Diarrhea often is watery, and no blood is present in the stool.
Warning Disclaimer Use For Publication
WARNING: Please DO NOT STOP MEDICATIONS without first consulting a physician since doing so could be hazardous to your health.
DISCLAIMER: All material available on eHealthMe.com is for informational purposes only, and is not a substitute for medical advice, diagnosis, or treatment provided by a qualified healthcare provider. All information is observation-only. Our phase IV clinical studies alone cannot establish cause-effect relationship. Different individuals may respond to medication in different ways. Every effort has been made to ensure that all information is accurate, up-to-date, and complete, but no guarantee is made to that effect. The use of the eHealthMe site and its content is at your own risk.
If you use this eHealthMe study on publication, please acknowledge it with a citation: study title, URL, accessed date.
Also Check: Hindgut Ulcers In Horses Treatment
When Should Someone Contact A Doctor About Colitis
Diarrhea is a common sign of colitis. It is usually self-limited and resolves on its own with supportive care, including rest and a short course of a clear-fluid diet. However, seek medical care if diarrhea persists for more than two to three weeks, if there is blood in the stool, fever, or the person has signs of dehydration.
- Blood in the stool is never normal and should always be evaluated. Common causes of blood in the stool include hemorrhoids however, other serious causes of bleeding need to be investigated. Colitis is not the only cause of rectal bleeding. Other causes include diverticular disease of the colon , colon polyps, anal fissures, and cancer.
- Chronic diarrhea may lead to dehydration and changes in the electrolyte balance in the body. If it is severe enough, the dehydration may require treatment with IV fluids or oral rehydration therapy. The symptoms of dehydration may include
- lightheadedness , especially when changing from a sitting or lying position to a standing position
- weakness
Risk Factors In Women
Women are particularly susceptible to urinary tract infections because their urethra is shorter, meaning the infection can spread throughout the urinary tract more easily. Additionally, the anal and urinary openings of a woman are in closer proximity, increasing the risk of bacteria spreading between the two.
In addition to the above, women are also susceptible to the following risk factors for UTIs:
- Sexual intercourse can contribute to the spread of genital or anal bacteria, especially with a new sexual partner when the rate of sexual activity is typically higher. However, UTIs are not a sexually transmitted disease
- Spermicides and birth control methods which use spermicides can affect the natural balance of healthy bacteria within the vagina
- Antibiotics can also alter the natural bacterial balance within the vagina
- Diaphragms can place pressure on a womanââ¬â¢s urethra, resulting in the possibility of the bladder not emptying properly
- Pregnancy. As the uterus grows in pregnancy, it can put added weight on the bladder, leading to the possibility of the bladder not emptying properly
- Menopause can cause hormonal changes which affect the vaginaââ¬â¢s natural bacterial balance
You May Like: Does Magnesium Cause Kidney Stones
You May Like: Symptoms Of Ulcer In Female
Ways To Reduce Complications
Early intervention and frequent surveillance of ailments is key to reducing complications and improving outcomes. It’s important to maintain proper nutrition and avoid emotional stress, though neither stress nor sensitivity to certain foods causes the disease. Avoiding steroids can also be helpful if you and your doctor have an alternative way of treating UC flares.
While the cure for UC has yet to be found, when the disease is treated properly, some complications may disappear altogether. Work with your doctor and other members of your healthcare team to get optimal control of the disease as soon as possible.
Additional reporting by Jordan M. Davidson.
Who Is At Risk For Ulcerative Colitis
Some things may make you at higher risk for ulcerative colitis. These include your:
- Age. The disease most often starts when you are between the ages of 15 and 30 years old.
- Family history. Having a family member or close blood relative with ulcerative colitis raises your risk of the disease.
- Race and ethnicity. It happens more often in white people and people of Jewish descent.
Recommended Reading: Stage 2 Pressure Ulcer Treatment Dressing
Who Can And Cannot Take Mesalazine
Adults and children aged 5 years and older can take mesalazine.
Mesalazine may not be suitable for some people. To make sure it’s safe for you, tell a pharmacist or doctor before taking or using it if you:
- have ever had an allergic reaction to mesalazine, aspirin, or any other salicylates such as methylsalicylate or choline salicylate
- have ever had an allergic reaction to any other medicine
- have any problems with your kidneys or liver
- have a rare blood condition called porphyria
- are trying to get pregnant, already pregnant, or breastfeeding
Living With Uc: Supplements
The bleeding caused by ulcerative colitis may lead to iron deficiency anemia due to the loss of the body’s store of iron in the red blood cells that are lost into the colon. Iron supplementation may be necessary. Medications used to treat ulcerative colitis may reduce the absorption of nutrients such as folic acid and calcium. Supplements of vitamins and minerals may be necessary.
Also Check: Foam Boots For Pressure Ulcers
Ways To Prevent E Coli Hemorrhagic Colitis
Try these strategies for preventing E. coli hemorrhagic colitis:
- Cook all your meat thoroughly until juices run clear, especially any ground beef.
- Avoid eating meat that is pink inside.
- Do not drink unpasteurized milk or apple cider.
- Do not drink untreated water.
- Do not eat cheese or other dairy products that are unpasteurized.
- Wash your hands after touching cattle, sheep, pigs, goats, rabbits, or chickens.
- Wash your hands before preparing or eating food.
Additional reporting by Christine Gordon
What Is Ulcerative Colitis
Ulcerative colitis is a disease in which there is chronic inflammation of the inner lining of the colon. The inflammation can cause the lining tissue to break down, forming ulcerations that can bleed. Inflammation can involve the entire colon or only parts of it. Almost always, ulcerative colitis requires treatment.
You May Like: Can You Drink Coffee With Ulcerative Colitis
Unique Mechanisms In Ibd Patients Prompt Revised Guidelines
Although both gallstones and kidney stones may be associated with IBD, the studys authors described different mechanisms that may influence their development. Without sufficient ileal activity, for example, they noted that a patients bile may contain excess bilirubin, which may form gallstones. Furthermore, a patient with IBD may experience multiple effects in the digestive tract that potentiate a risk of gallstones.
Kidney stones typically form due to a high abundance of oxalate or similar compounds in the urine, according to the study publication. IBD may result in more concentrated urine due to factors such as dehydration from diarrhea and dysregulation of absorptionof salts in the ileum. An ileostomy may also result in urine that is more acidic.
Dr.Fagagnini and her co-authors suggested that clinical trials further explore treatment and relationships between IBD and the development of gallstones and kidney stones. Specifically, they recommended studying the use of ursodeoxycholic acid in IBD patients at risk of gallstones and a diet low in oxalate and high in fluid, with decreased ingestion of some fatty acids, for IBD patients at higher risk of kidney stones.
The authors disclosed no competing financial interests.
T Cell Isolation And Stimulation
Peripheral venous blood was obtained from healthy volunteers in compliance with the AIIMS Institutional ethics committee protocols. Peripheral blood mononuclear cells were separated by Ficoll-Paque plus gradient centrifugation. The PBMCs were stained with CD4- Allophycocyanin , CD25-phycoerythrin-Cy7 and CD45 RA- Phycoerithrin . Naive T cells were sorted by high speed flow cytometry with FACS AriaIII to > 95% post sort purity. Cells were cultured at 105 cells/well in a 96 well U bottom plate for 6 days in serum free X vivo medium and stimulated with plate bound anti CD3 and soluble anti CD28 . In Th polarization assay, at the start of the culture, cells were differentiated with recombinant IL-2 for Th0, TGF1 , IL-1 , IL-6, IL-21 and IL-23 for Th17 in the presence and absence of potassium chloride.
You May Like: How To Cure Ulcerative Proctitis
Living With Uc: Probiotics
Probiotics consist of bacteria that confer a health benefit on the person who ingests them. In general, they are bacteria that are normally found in the human intestine. Probiotics have beneficial effects in several medical conditions. Studies have shown that probiotics help people with ulcerative colitis maintain their remissions. Probiotics are found in yogurts and some other foods, but the probiotics that have been studied and found to be effective are sold separately as supplements and are not food products. The effects of probiotics vary greatly and depend on the exact bacteria that are present. Therefore, it is likely that many probiotics that are sold have no beneficial effect, and, therefore, the one that is used for treatment needs to be chosen carefully on the basis of scientific studies.
Colitis And Crohns Disease And Incontinence
Incontinence can be a problem for some suffering from Colitis and Crohns. Both conditions can cause diarrhoea and also an urgent need to go to the toilet. This can lead to accidents which can leave you feeling embarrassed and uncomfortable. To avoid accidents, or if they cannot be avoided, to help you deal with them, it is a good idea to always be prepared.
When you are at home, accidents should be relatively easy for you to manage. Make sure you have the necessary equipment in the bathroom to hand should you have an accident, such as disposable tissues which are a lot more hygienic to clean yourself with and less likely to irritate the skin. Air fresheners are also useful to disguise any smells.
If you are concerned about having an accident when you are out and about, keep some spare, clean underwear in your bag and a packet of baby wipes to help you stay fresh and comfortable. Keep a plastic bag handy so you can dispose of any soiled items too. It is also a good idea to know where the nearest toilets are located.
B& BC can provide a Just Cant Wait toilet card which could help you gain access to a toilet when out shopping or socialising. The card states that the card holder has a medical condition and may require the urgent use of a toilet. If you would like to apply for a toilet card online or order one by phone, please visit our toilet card page for more information.
Don’t Miss: How To Treat A Diabetic Ulcer