Does Ibs Get Worse With Age
IBS is long-term disorder of the gut and is an inevitable part of aging. It comes and goes over time. The sensitivity of the gut nerves may elevate with age and the symptoms overlap is possible. Different signs and symptoms related to IBS may show up with age. However, there are some ways like exercise, avoidance of foods that irritate the digestive system etc. that help to help reduce the overall risk of IBS and aid in reducing the symptoms.
Inflammatory Bowel Disease And Colitis
Ulcerative colitis and Crohn’s disease are the two types of inflammatory bowel disease that cause colitis. Crohn’s disease and ulcerative colitis are considered autoimmune diseases .
- Ulcerative colitis always begins in the rectum and may spread to the rest of the rest of the colon, spreading from the rectum to the sigmoid, descending, transverse, and finally the ascending colon and cecum in that order. Ulcerative colitis is considered an autoimmune disease, and symptoms include abdominal pain, and bloody, diarrheal bowel movements.
- Crohn’s disease may occur anywhere in the gastrointestinal tract , including the esophagus, stomach, small intestine, and colon. In Crohn’s disease, there may be “skip lesions,” that is, abnormal segments of the GI tract interspersed with normal segments.
Both Crohn’s disease and ulcerative colitis may have other organ systems involved in addition to the gastrointestinal tract.
Either collagen or lymphocytes infiltrate into the layers of the wall of the colon, presumably as a result of inflammation. This is an uncommon illness and maybe an autoimmune disease. Diarrhea often is watery, and no blood is present in the stool.
What Are The Causes And Symptoms Of Collagenous Colitis
Collagenous colitis is caused by swelling and inflammation due to inflammatory cells traveling to the large, and sometimes small, intestine. If your large intestine is unable to properly reabsorb water, it causes the symptoms of collagenous colitis.
There are many factors that can contribute to collagenous colitis including a potential reaction to bacteria, pollen, or food. Certain medications may be triggers for CC, a list that includes nonsteroidal anti-inflammatory drugs antacids antidepressants diabetes medication and cholesterol medication. Continue reading
Recommended Reading: Foods To Eat To Help Ulcers
What Causes Infectious Colitis
Infectious colitis is not to be confused with other types of colitis, such as ulcerative colitis. Ulcerative colitis is an inflammatory bowel disease, but its causes are normally due to infections from bacteria, viruses, parasites, or fungus. The term colitis refers to the main symptom, which is diarrhea.
Infectious colitis is often linked with food poisoning, which is an infection of the stomach and rectum. The most common cause of a food poisoning type of infectious colitis is contaminated water, and it comes from a parasite called entamoeba histolytica. You can also experience sudden diarrhea after consuming food contaminated with bacteria. E-coli, salmonella, shigella, yersinia, or campylobacter are all bacterial intestinal infections. Continue reading
Symptoms Of Chronic Ulcerative Colitis
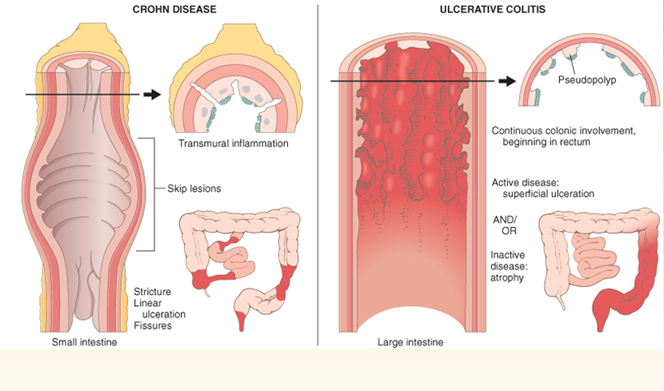
Symptoms vary among patients depending upon where in the colon and rectum inflammation resides as well as its intensity. Inflammation may affect a small portion of the colon and rectum or, in worse cases, engulf the entire large intestine.
Patients with chronic ulcerative colitis are at risk of: anemia, from bleeding within the colon and rectum bone disorders, including osteoporosis, because nutrients are not being absorbed by the intestines and skin and eye disorders, common among patients with immune system diseases, such as rheumatoid arthritis. Patients with chronic ulcerative colitis also are at a higher risk of developing primary sclerosing cholangitis, a disorder of the bile ducts in the liver, and colon cancer.
Signs and symptoms of chronic ulcerative colitis can include:
- Persistent diarrhea or loose stools
- Bloody stools
Recommended Reading: Can Stomach Ulcer Cause Fever
What Are The Risk Factors Of Ulcerative Colitis
It is estimated that as many as one million Americans have IBD with that number evenly split between Crohns disease and ulcerative colitis. Males and females appear to be affected equally. The usual age of diagnosis with ulcerative colitis is in the mid-30s, although the disease can occur at any age. Men are more likely than women to be diagnosed with ulcerative colitis in their 50s and 60s. The incidence is greater in whites than non-whites, and a higher incidence is found in Jews than in non-Jews.
IBD tends to run in families. Studies have shown that up to 20 percent of patients with ulcerative colitis will have a close relative with either Crohns disease or ulcerative colitis. There is no way to predict which, if any, family members will develop ulcerative colitis.
When Should Someone Contact A Doctor About Colitis
Diarrhea is a common sign of colitis. It is usually self-limited and resolves on its own with supportive care, including rest and a short course of a clear-fluid diet. However, seek medical care if diarrhea persists for more than two to three weeks, if there is blood in the stool, fever, or the person has signs of dehydration.
- Blood in the stool is never normal and should always be evaluated. Common causes of blood in the stool include hemorrhoids however, other serious causes of bleeding need to be investigated. Colitis is not the only cause of rectal bleeding. Other causes include diverticular disease of the colon , colon polyps, anal fissures, and cancer.
- Chronic diarrhea may lead to dehydration and changes in the electrolyte balance in the body. If it is severe enough, the dehydration may require treatment with IV fluids or oral rehydration therapy. The symptoms of dehydration may include
- lightheadedness , especially when changing from a sitting or lying position to a standing position
- weakness
Read Also: Do Ulcers Cause Weight Loss
Actions For This Page
- Crohns disease and ulcerative colitis are collectively known as inflammatory bowel disease .
- Crohns disease can appear in any part of a persons digestive tract from mouth to anus.
- Ulcerative colitis is located only in a persons large bowel .
- Diet and food allergies do not cause IBD.
- Medications help manage the symptoms of IBD.
- People with IBD can lead useful and productive lives.
- Some dietary changes can help you manage symptoms of IBD and allow medications to work better.
- Always talk with your doctor, healthcare specialist or dietitian before changing your diet. Arrange an emergency plan of action with your doctor, including after-hours phone numbers.
What Are The Causes Of Ulcerative Colitis
We do not yet know what causes this disease. Studies indicate that the inflammation in ulcerative colitis involves a complex interaction of factors: the genes the person has inherited, the immune system, and something in the environment. Foreign substances in the environment may be the direct cause of the inflammation, or they may stimulate the bodys defenses to produce an inflammation that continues without control. In patients with ulcerative colitis, once the patients immune system is turned on, it does not know how to properly turn off. As a result, inflammation damages the intestine and causes the symptoms of ulcerative colitis. One of the major goals of medical therapy is to help patients to better regulate their immune system.
Read Also: Icd 10 Stage 4 Sacral Ulcer
What Is Crohns Disease
Crohns disease is a type of IBD where there is inflammation of the entire gastrointestinal tract, or parts of it, from mouth to anus. In addition, the entire thickness of the bowel wall is involved in Crohns disease, which can lead to some serious complications.
What are symptoms of Crohns disease?
The symptoms of Crohns disease depend on what parts of the GI tract are involved. Common symptoms include abdominal pain, weight loss, and diarrhea.
If the lower part of the GI tract such as the colon and the small intestines are involved, you might also experience:
-
Abdominal pain
What are complications of Crohns disease?
Crohns disease can lead to some serious complications, such as:
-
Fistulas, where a hole is formed between the intestines and other parts of the body such as the skin, bladder, or vagina
-
Abscesses, which are pockets of infection that may need surgery or a procedure to drain them
-
Strictures, which are a narrowing of the bowel that can lead to blockages
-
Cancers of the GI tract
Crohns Disease Vs Ulcerative Colitis: Differences In Symptoms Causes And Treatment
Crohns disease and ulcerative colitis are part of the group of conditions known as inflammatory bowel diseases . Prior to the 20th century, before the rise of hygiene and urbanization, inflammatory bowel disease was quite rare. Currently, IBD is found in developed countries and is believed to be caused by a lack of germ resistance development although the exact cause is still unknown.
For those living with IBD, their immune system mistakes food and bacteria in the gastrointestinal tract for an allergen or foreign substance, so it sends out cells to destroy it. The result of these attacks is chronic inflammation.
Although the exact causes of Crohns disease and ulcerative colitis are unknown, genetics and environmental factors are believed to play a role. Crohns disease and ulcerative colitis are often interchanged for one another, but we will outline the differences between the two, including symptoms, causes, and treatments in order to provide you with a better understanding of either condition. Continue reading
Recommended Reading: Best Treatment For Diabetic Foot Ulcer
What Kind Of Doctor Diagnoses And Treats Colitis
Most often colitis is treated by a primary health care provider or internal-medicine specialist, especially when the colitis is first diagnosed and the cause is uncertain. Once the cause is found, that health care provider may be the only person needed to continue care. Should there be a need for further investigation and diagnostic testing, specialists may be consulted, such as a gastroenterologist. If an infection is the cause of colitis, an infectious-disease specialist may be consulted. In some cases, other specialists may be involved in treatment, such as surgeons and interventional radiologists.
Patient history
Infectious Colitis: Causes Symptoms And Treatment Tips
The term infectious colitis sounds awful, and it can be. Infectious colitis is inflammation of the main part of the large intestine and can lead to sudden lower abdominal pain. In some cases, the pain can be severe.While inflammation is a common medical term and may not seem all that serious, the reality is that when left untreated, it can lead to complications and has the potential to be deadly.
Read Also: What To Eat With An Ulcerative Colitis Flare Up
Similar Symptoms With Important Differences: Colitis Vs Ibs
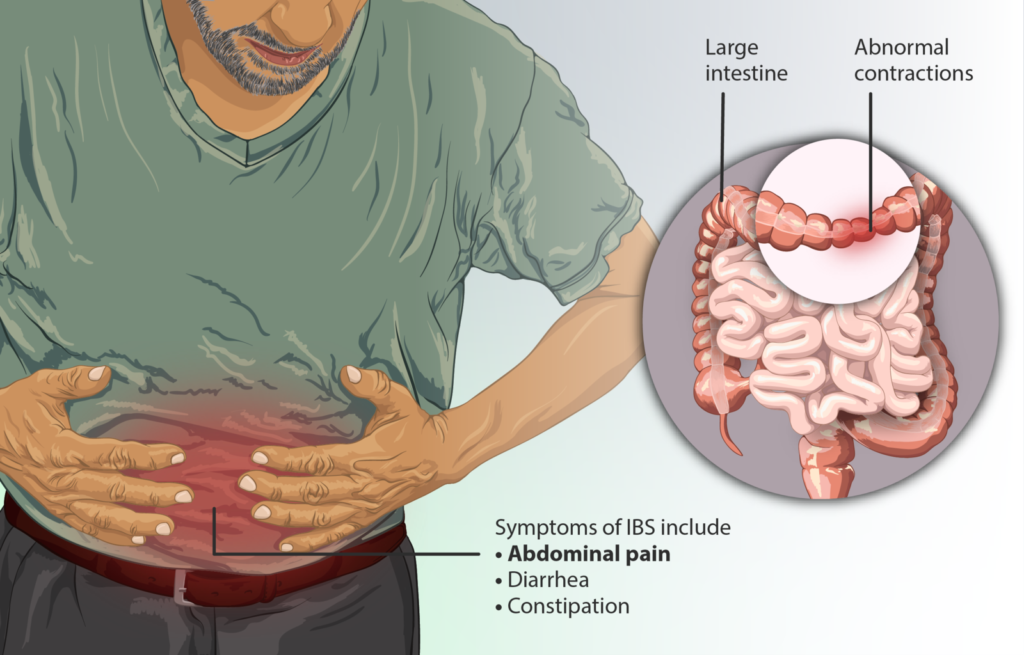
The main symptoms of colitis are ongoing diarrhea and pain in the stomach. Some people will feel very tired or even exhausted, and they may also lose weight and find that their appetite goes down. Sufferers of the ulcerative type may find that when they pass a bowel movement, they also pass blood or mucus however, blood is not present in microscopic colitis.
Irritable bowel sufferers can have ongoing diarrhea as a key symptom, but they may also swing from diarrhea to constipation or only ever have constipation. Unlike colitis, IBS does not cause bleeding as the bowel itself is intact, so even a severe bout of IBS does not damage the gut. Weight loss and fatigue are also not symptoms of IBS, but stomach pain definitely is, along with bloating and an urgent need to get to a bathroom.
Usually IBS sufferers only experience bowel and stomach symptoms, but colitis can cause problems with other parts of the body such as painful swelling of the joints, eye or skin irritation and mouth ulcers. If the condition is very severe, patients can also have a high temperature or fast heartbeat.
Colitis is similar to IBS in that it can come and go over time. Patients with both disorders might refer to a flare-up when their symptoms are particularly bad, but they will usually have times when they feel much better and the symptoms are in remission.
Main Difference Colitis Vs Ulcerative Colitis
Colitis and ulcerative colitis are two medical conditions which affect the colon. These two terms often used interchangeably since they share similar signs and symptoms. But, it is important to distinguish the difference between them in order to make an accurate diagnosis and treatment. The main difference between colitis and ulcerative colitis is that ulcerative colitis is one form of colitis which results in the chronic inflammation of colonic mucosa and rectum giving rise to ulceration and bleeding.
1. What is Colitis ? Causes, Signs and Symptoms, Diagnosis, and Treatment
2. What is Ulcerative Colitis? Causes, Signs and Symptoms, Diagnosis, and Treatment
3. What is the difference between Colitis and Ulcerative Colitis?
Read Also: Can You Donate Blood If You Have Ulcerative Colitis
What Should I Ask My Doctor On Behalf Of My Child Or Teenager
Ask your healthcare provider the following questions in addition to the ones listed above:
- What vitamins should my child take?
- Will my other children have pediatric ulcerative colitis?
- Is my child at risk for other conditions?
- Can you recommend a psychiatrist or therapist to help my child with emotional issues related to pediatric ulcerative colitis?
- Is my child growing at a normal rate?
- What can I do to help my child cope at school?
A note from Cleveland Clinic
When you have ulcerative colitis, its essential to work closely with your healthcare team.
Take your medications as prescribed, even when you dont have symptoms. Skipping medications youre supposed to take can lead to flareups and make the disease harder to control. Your best shot at managing ulcerative colitis is to follow your treatment plan and talk to your healthcare provider regularly.
Does Ulcerative Colitis Make You Immunocompromised
Ulcerative colitis doesnt make you immunocompromised. Some of the medicines that treat it may change the way your immune system responds. This change is different for each medication. Some of these changes may increase the risk of certain infections or other issues. A discussion with your health care team before starting a medication is the best way to understand these risks and ways to prevent them.
Also Check: Can Tylenol Cause Stomach Ulcers
What Is The Difference Between Ulcerative Colitis And Pancolitis
Ask U.S. doctors your own question and get educational, text answers â it’s anonymous and free!
Ask U.S. doctors your own question and get educational, text answers â it’s anonymous and free!
HealthTap doctors are based in the U.S., board certified, and available by text or video.
Differences Between Ulcerative Colitis And Crohn’s Disease
The differences between ulcerative colitis and Crohn’s disease are:
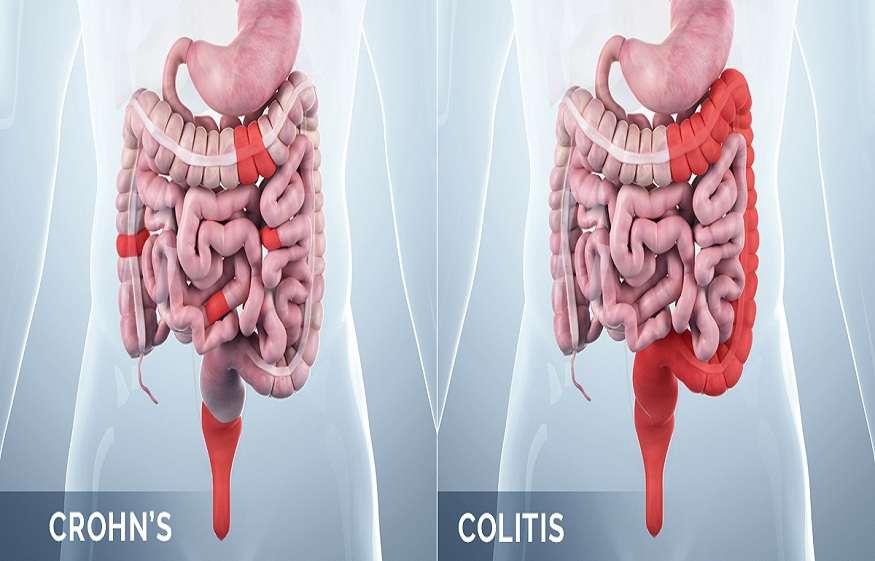
- Ulcerative colitis is limited to the colon while Crohn’s disease can occur anywhere between the mouth and the anus
- In Crohn’s disease, there are healthy parts of the intestine mixed in between inflamed areas. Ulcerative colitis, on the other hand, is continuous inflammation of the colon
- Ulcerative colitis only affects the inner most lining of the colon while Crohn’s disease can occur in all the layers of the bowel walls
Don’t Miss: Ulcerative Colitis Flare Up Treatment Guidelines
Allergic Colitis In Infants
Allergic colitis is a condition that can occur in infants, usually within the first months after birth. The condition can cause symptoms in infants including:
- reflux
- fussiness
- possible flecks of blood in a babys stool
Doctors dont know exactly what causes allergic colitis. One of the most popular theories is that infants with allergic colitis have an allergic or hypersensitive reaction to certain components in breast milk. A 2020 review of studies indicated that a protein allergy, either through breast milk, cows milk, or formula, could contribute.
Eosinophilic colitis is a type of allergic colitis that can also show up in infants with these symptoms. Its causes are similarly unknown , but its likely also related to a protein allergy.
Doctors will often recommend an elimination diet for the birthing parent, which involves slowly cutting out certain foods known to contribute to allergic colitis. Examples include cows milk, eggs, and wheat. If the baby stops having symptoms of allergic colitis, these foods were likely causing the problem.
In severe cases, monoclonal antibodies, such as those used to inflammatory bowel disease , may also be another treatment option.
Treating Colitis And Chronic Ulcerative Colitis
Medications, and in severe cases surgery to remove the colon, are the mainstay of treatment for patients with chronic ulcerative colitis and Crohn’s disease. Because these diseases are disorders of the immune system, in which the body attacks cells within the colon, the goals of treatment are to suppress inflammatory episodes and to improve quality of life. Unfortunately, as patients know all too well, the disease can flare up repeatedly, the reason why treatment is usually life long.
The Digestive Disease Institute at Virginia Mason is at the forefront in immune system research, specifically at Benaroya Research Institute at Virginia Mason, where scientists are unlocking the genetic causes of immune system disorders that includes rheumatoid arthritis, multiple sclerosis and inflammatory bowel disease.
Recommended Reading: What To Eat When You Have Gastric Ulcer
Treatments For Ibs And Ibd
Treatment is very different for IBS and IBD. If you have IBD, you will take medications that lower the inflammation in the GI tract such as anti-inflammatory medications, biologic agents, and immunomodulators which can reduce the damage IBD is causing.
Treatment of IBS is different. You and your providers will focus on treating the specific symptoms you are having. Changes to your diet and exercise habits are a good first step.
Heres a few examples of some foods to avoid when you have IBS:
-
Apples
If diarrhea is one of your main IBS symptoms, you might take medications that reduce the diarrhea, such as rifamixin and eluxadoline . If you are more often constipated, you might take medications that help keep the GI tract moving, such as lubiprostone , linaclotide , or plecanatide .
You might also need treatment of stress, anxiety, or depression with medications or therapy if you and your provider think this is playing a role in your IBS.