Basics Of Inflammatory Bowel Disease
Arthritis means inflammation of joints. Inflammation is a body process that can result in pain, swelling, warmth, redness and stiffness. Sometimes inflammation can also affect the bowel. When it does that process is called inflammatory bowel disease . IBD is actually two separate diseases: Crohn’s disease and ulcerative colitis.
What Are The Symptoms Of Ulcerative Colitis
Ulcerative colitis symptoms often get worse over time. In the beginning, you may notice:
- Diarrhea or urgent bowel movements.
- Abdominal cramping.
- Liver disease.
- Loss of fluids and nutrients.
Symptoms are similar in pediatric ulcerative colitis and may also include delayed or poor growth. Some ulcerative colitis symptoms in children can mimic other conditions, so it is important to report all symptoms to your pediatrician.
Arthritis Affects An Estimated 25% Of Ibd Patients
Inflammatory bowel disease is associated with several other conditions, including the liver disorder primary sclerosing cholangitis, fissures, fistulas, and arthritis. Arthritis is the most common extraintestinal complication, affecting an estimated 25 percent of all IBD patients. The two most common forms of arthritis experienced by IBD patients are peripheral arthritis and axial arthritis.
Because arthritis is so common, it’s important for people with IBD to pay attention to aches and pains. While a certain amount of pain is going to be typical, it should still be brought up at appointments with your physicians. Keeping joints as healthy as possible and avoiding activities that do damage, as well as staying on top of any problems if they crop up, is vital. If pain becomes bothersome, it should be talked over with a gastroenterologist or a rheumatologist before starting any pain medications, because people with IBD may need to avoid certain types of drugs .
Also Check: Is Ulcerative Colitis Considered An Autoimmune Disease
Faqs About Unlock Your Hip Flexors
Q: How is this different from other hip flexibility programs?
A: What makes Rick’s program unique is knowing how to unravel the tricky layers of tension with the very difficult psoas muscle in order to effectively loosen and train it.
Rick’s one-of-a-kind sequential flow is your surest path to looser, stronger and healthier hips.
Q: Why are you selling this so cheap? What’s the catch?
A: There is none. We’re so pleased with the number of our customers who have made the investment in this program and have enjoyed life-changing results.
Our aim is to make this available to as many guys as possible, firstly to welcome more people to our CriticalBench.com audience and secondly because we’re celebrating hitting a quarter million fans on Facebook.
Q: How long will it take me to do the program?
A: The program is designed to take between 10-15 minutes in total to complete.
We recommended adding the program as a daily practice to get the best results over a longer period of time. You may wish to add this program before or after your regular gym session or use it independently.
Q: How long until I see results?
A: Although everyone is different and results may vary, we know from experience how quickly it’s possible to feel and see a difference.
For some it may be as soon as their first session for others it may take a few sessions to really start seeing the benefits. Again, it depends on the body in question.
Q: Who is this program suitable for?
Q: Are the exercises hard to perform?
Treating Back Pain In Ulcerative Colitis
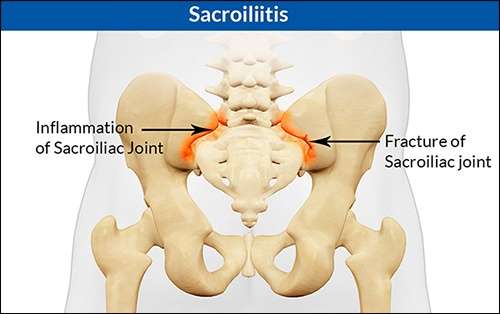
Treating back pain in ulcerative colitis can be complicated. Research shows that treating the underlying UC can help lessen the severity of spondyloarthritis, but it will not resolve spondyloarthritis and back pain. Back pain must be addressed separately and in a way that does not make a persons UC symptoms worse.
People with ulcerative colitis may need to work with both a rheumatologist and a gastroenterologist to manage their gastrointestinal and spinal health properly. These doctors may prescribe or recommend the following treatments and therapies.
Also Check: What To Eat When You Have Gastric Ulcer
Ulcerative Colitis Symptoms You Should Never Ignore
Ulcerative colitis is an autoimmune disease in which the immune system attacks the colon and causes a range of symptoms, both in the GI tract and around the body.
Symptoms of ulcerative colitis, a type of inflammatory bowel disease , can vary widely depending on how much inflammation a person has and where the inflammation is located.
Abdominal pain and bloody diarrhea are the most common warning signs of UC, and can range from mild and intermittent to severe and chronic. The pain of UC is quite common and can significantly impact quality of life. Ulcerative colitis symptoms tend to come and go, often with extended periods of time in between flares. These are called remission periods.
The disease tends to develop gradually over time, so you might not automatically think of ulcerative colitis or IBD if you have occasional abdominal pain or digestive distress.
Ongoing inflammation along with ulcers and abscesses in the intestines are additional common causes of pain. Scarring in the lining of the intestinal tract can lead to painful obstructions. Pain may occur in different areas such as the abdomen or rectal area, depending where the inflammation is located. For example, people may experience moderate to severe pain on the left side of the abdomen if the UC affects the rectum and the lower segment of colon.
UC symptoms might ebb and flow, but they wont go away unless you see a gastroenterologist and start treatment.
What Your Physician Isn’t Telling You And What They Dont Know
Diagnosing tight hip flexors is tricky.
If you’ve seen a therapist or physician, chances are they weren’t able to pinpoint the issue.
Buried so deep within your abdomen, it’s no wonder identifying it as the root cause of any of your symptoms is difficult to do.
It’s why tight hip flexors are left undiagnosed and untreated for far too long, as physicians look for a simpler explanation.
So understand that this it’s not your fault.
However, knowing this hands you the power to finally do something about it before it’s too late.
Recommended Reading: Symptoms Of Bleeding Ulcer In Esophagus
How Uc Affects The Entire Body
Medically reviewed by Matthew J. Hamilton, MD
Ulcerative colitis is a type of inflammatory bowel disease, or IBD, that causes chronic inflammation in the large intestine. This can lead to gastrointestinal symptoms ranging from abdominal pain and cramping to frequent bowel movements.
However, inflammation and associated symptoms can go beyond your gutits estimated that up to 40 percent of people with IBD experience one or more non-GI symptoms.
Ulcerative colitis can be more systemic in the way it affects the body, explains David T. Rubin, MD, professor of medicine and chief of gastroenterology at the University of Chicago, and chair-elect of the national scientific advisory committee for the Crohns and Colitis Foundation. Meaning, ulcerative colitis can affect the entire body. Find out what you should watch for, plus ways to take control of your health.
Enjoy Looser Hips Greater Strength And More Poweror Your Money Back Guaranteed
EVERYONE suffers from tight hip flexors. Which means everyone can benefit. It’s not a case of whether this will benefit you, but how much
That’s why I want to make this a no-brainer for you with a 100% risk-free money back guarantee.
For the next 60 days, try using the simple techniques demonstrated by Rick either on their own or incorporated into your daily workout.
I’m confident youll be delighted with the results but, if youre not, simply email us and ask for a prompt and hassle-free, no questions asked 100% refund.
In fact, if you’re not happy for ANY reason, I insist you ask for a refund and well be more than happy to give you all your money back.
After seeing the effect of the program for myself and those close to me, Im sure you’ll be amazed at how quickly you feel the benefits of looser hips and greater strength and vitality.
Also Check: Over The Counter For Ulcers
Back Pain And Ulcerative Colitis
Research indicates that nearly 25 percent of people with inflammatory bowel disease including ulcerative colitis and Crohns disease experience chronic lower back pain. Ankylosing spondylitis and axial arthritis both of which can cause back pain are two common causes of back pain in people with UC.
That said, a doctor may not suspect that a person with back pain has UC unless they also experience gastrointestinal symptoms. If you do experience back pain, its important to let your doctor know even if you dont suspect that its related to UC. They will be able to determine the cause of your pain and work with you to find the best way of managing it.
What Causes Ulcerative Colitis Flareups
When youre in remission from ulcerative colitis, youll want to do everything you can to prevent a flareup. Things that may cause a flareup include:
- Emotional stress: Get at least seven hours of sleep a night, exercise regularly and find healthy ways to relieve stress, such as meditation.
- NSAID use: For pain relief or a fever, use acetaminophen instead of NSAIDs like Motrin® and Advil®.
- Antibiotics: Let your healthcare provider know if antibiotics trigger your symptoms.
Read Also: Crohn’s Versus Ulcerative Colitis Pathology
Joint Pain: The Most Common Non
About 30 percent of people with ulcerative colitis experience joint pain, according to the Crohns and Colitis Foundation, making it the most common non-GI symptom of the disease. Joint pain often occurs in the knees, ankles, elbows, and wrists. Its usually joint pain thats symmetrical, meaning both knees or both ankles, says Dr. Rubin. This type of joint pain tends to parallel bowel activityso if you fix the intestine, the joint pain goes away.
However, ulcerative colitis is also related to inflammatory joint conditions that affect your spine, like ankylosing spondylitis. This type of joint pain can be independent of your bowelso your bowel can be completely in remission, and your back or your pelvis is inflamed, and you can have joint damage, says Rubin.
The good news: Some medications used to treat ulcerative colitis are also used to treat inflammatory joint conditions like ankylosing spondylitis. Its not that fixing the bowel makes these joints betterits that the medication that works on the bowel also works on these joint conditions, says Rubin. So if youre experiencing joint pain, its important to work with your doctor to understand what type of joint pain you have and get proper treatment. In some cases it may be necessary to see a doctor who specializes in the joints, a rheumatologist, to work with your IBD doctor.
What Role Does Diet And Nutrition Play In Ulcerative Colitis
Diet does not cause the development of ulcerative colitis nor can any special diet cure the disease. However, the foods you or your child eat may play a role in managing symptoms and lengthening the time between flareups.
Some foods may make symptoms worse and should be avoided, especially during flareups. Foods that trigger symptoms are different from person to person. To narrow down what foods affect you, keep track of what you eat each day and how you feel afterward .
Problem foods often include:
- High sugar foods and drinks.
- Carbonated beverages.
- High-fiber foods.
- Alcohol.
In addition to the problem foods listed above, infants, children and teenagers can also experience issues with:
- Salt.
- Dairy products.
Keep a careful eye on your childs diet and nutrition. Their appetite may decrease during a flareup and they might not eat enough to stay healthy, and grow. Also, the inflammation caused by ulcerative colitis may keep their digestive tract from absorbing enough nutrients. This can also affect your childs health. For these reasons, you may have to increase the amount of calories your child consumes.
Its best to work with your provider and nutritionist to come up with a personalized diet plan if you or your child has ulcerative colitis.
You May Like: Ulcerative Colitis Flare Up Treatment Guidelines
Research And New Developments
Previous research has shown that ankylosing spondylitis has a strong genetic component and were currently funding several research projects to further understand this. Previously, we part funded research that identified a specific gene, called IL23R, thats linked to the condition. Were now funding a follow-on project to investigate how changes in this gene lead to the development of ankylosing spondylitis.
Were also supporting a study thats investigating a gene called RUNX3. Researchers are investigating whether this molecule can be targeted with drugs. Results from this research may lead to the development of new and more effective drug treatments.
Were funding a project investigating the protein HLA-B27. This protein is found in over 90% of people with ankylosing spondylitis. Its thought that HLA-B27 proteins tend to fold incorrectly inside cells, which may lead to the immune system releasing chemicals that cause inflammation. This research aims to generate HLA-B27 specific treatments that overcome the problems associated with current treatment options.
What Is Ankylosing Spondylitis
Ankylosing spondylitis is a type of arthritis that mainly affects the back, by causing inflammation in the spine. This can make your back, rib cage and neck stiff and painful.
It often starts in people who are in their late teens or 20s.
In response to the inflammation, the body produces extra calcium around the bones of the spine. This can make extra bits of bone grow and cause your back and neck to be more stiff.
In rare cases some of the bones of the spine may link up, or fuse together because of the extra calcium. In serious cases this can make the spine curve forward more. You can reduce the risk of this happening, if you:
- keep active
You May Like: How To Heal Ulcerative Colitis With Food
He Had Recurring Pain For Nearly A Decade
- Read in app
The pain woke the 52-year-old physician from a dead sleep. It was as if all the muscles in his right leg, from those in the buttock down his thigh to the very bottom of his calf, were on fire. He shifted slightly to see if he could find a more comfortable position. There was a jag of pain, and he almost cried out. He glanced at the clock: 4 a.m. In just three hours he would have to get up. He had a full day of patients to see. Massage didnt help. He couldnt get comfortable lying flat, so finally he moved to the living room, to a recliner. Only then, and only by lying completely still, did he manage to get the pain to abate. He drifted off, but never for long. The searing pain in his leg and buttock slowly eased, and by the time his alarm went off, he could stand and walk though his muscles still ached and he had to baby his right leg, causing a limp.
Between patients, he arranged to see his own doctor. Hed had pain off and on in his buttocks, one side or the other, for more than a year. The pain was in the middle of each cheek and was worse when he was sitting and at the end of the day. Walking to and from his car on the way home was brutal. And then, as mysteriously as it came, it would disappear only to come back a week or two later.
Order Today And You’ll Receive These Two Powerful Bonuses
The 7-Day Anti-Inflammatory Diet“Automatically Heal Your Body with The Right Foods”
The Unlock Your Hip Flexors program is designed to bring you all the benefits of looser hip flexors with greater strength, power and flexibility.
But its benefits are multiplied when combined with a holistic diet to naturally alleviate pains, aches, soreness and stiffness by tackling inflammation caused by injury or environmental toxins in our food and water.
Your diet is one of the major causes of inflammatory responses leading to health deteriorating.
You can instantly improve your body’s response to inflammation by choosing the right foods that work with your body to stimulate your natural healing response.
The 7-Day Anti-Inflammatory Diet is a Done-For-You nutrition program featuring diet recommendations, meal plans, shopping lists and supplement tips to help your body automatically heal itself.
In as little as 24 hours, your body will switch on its natural healing process rather than causing pain and inflammation which can lead to many chronic diseases and health problems.
Don’t Miss: What Is The Best Treatment For Ulcerative Proctitis
When Back Pain May Mean Arthritis
Many forms of arthritis and related conditions can cause back pain, stiffness and swelling.
About 80% of back pain is acute and usually lasts one to seven days. Otherwise, its considered chronic and may be caused by arthritis. The lower back is the most common site of arthritis back pain. Several types of arthritis are part of a group of conditions called spondylarthropathies . Spondylarthropathies can affect adults and children.
If you are experiencing pain, swelling and stiffness in the back, you may have one of the following types of arthritis or related conditions.
Axial Spondyloarthritis
Axial spondyloarthritis is a chronic inflammatory disease that primarily affects hip joints and the joint that connects the bone at the bottom of the spine to the pelvis .
There are two types of axSpA: Radiographic axSpA includes damage to the sacroiliac joints and spine that can be seen on X-rays, and nonradiographic axSpA does not include damage you can see on X-rays but it may show up on magnetic resonance images .
Osteoarthritis
Psoriatic Arthritis
Psoriatic arthritis is a form of arthritis that affects joints and usually the skin . For about 20 percent of people with PsA, the disease involves the spine . In some cases, bony overgrowth can cause two or more vertebrae to grow together , causing stiffness.
Reactive Arthritis
Enteropathic Arthritis
Spinal Stenosis
Getting a Proper Diagnosis
Quick Links