How Well Is Your Ulcerative Colitis Treatment Working
If you have ulcerative colitis, the right medication can help control your symptoms. But just as your condition can change over time, so can your bodys response to certain medications. How do you know if your treatment is really working or its time to make a significant modification to your regimen?
It can depend on what symptoms youre experiencing, how much inflammation youre experiencing, and what your quality of life is, says Tauseef Ali, MD, FACG, a clinical assistant professor of medicine at the University of Oklahoma, director of the Saint Anthony Hospital Crohns and Colitis Program in Oklahoma City, and author of Crohns and Colitis for Dummies.
Its key for patients to understand and spend some time with their doctor, learning more about the disease, the disease process, and the goal of the treatment, says Dr. Ali.
Even if you dont need to change your treatment altogether, there are some ways to optimize your regimen. Take medications regularly as prescribed, says Ashwin Ananthakrishnan, MBBS, MPH, an associate professor of medicine at Massachusetts General Hospital in Boston. Check in periodically with your doctors for lab work, stool tests, and colonoscopies.
Ananthakrishnan also stresses the importance of regular physical activity, adequate sleep, stress management, and a healthy diet that includes vegetables and fruits and limits sugars, processed foods, and unhealthy fats.
What Makes It Worse
The reasons why aren’t totally clear. Doctors don’t know why it affects only a small section in one person, but spreads through the entire colon in another. But certain triggers sometimes play a role. These include:
Food. It’s different for everyone, but certain foods can irritate your symptoms. For example:
- Caffeine can make severe diarrhea worse
- Dairy may lead to more diarrhea, gas, and pain
- Fizzy drinks can be a problem if you have gas
- Greasy and fried foods often lead to gas and diarrhea
- High-fiber foods, such as fresh fruits and veggies, whole grains, corn, nuts, and seeds, can be hard on you
- Spicy foods can be tough to handle
Stress. It can trigger flare-ups and make your symptoms much harder to deal with. It’s especially challenging because just having ulcerative colitis can bring on more of it.
Skipping meds. Even when you’re in remission, it’s very important to take your meds. In the best case, they prevent flare-ups. And even if not, they can help keep things under control.
Follow these 5 tips to help control your ulcerative colitis flare-ups.
How Is Treatment Effectiveness Assessed
Managing symptoms is an important aspect of treating IBD, but newer research suggests that treating symptoms alone does not always address the underlying disease. Ongoing monitoring can provide evidence of intestinal lesions and inflammation to determine if the gastrointestinal tract is healing or not. Drug monitoring can determine how much of a medication is in your bloodstream and if the dosage is correct.
The effectiveness of Crohns or ulcerative colitis treatment is based on a combination of factors that can be assessed during both disease activity and remission. These include:
- Symptoms
- Biomarkers indicated in blood tests
- Quality of life
You May Like: Black Tarry Stools Ulcerative Colitis
What Causes Ulcerative Colitis
Researchers think the cause of ulcerative colitis is complex and involves many factors. They think its probably the result of an overactive immune response. The immune systems job is to protect the body from germs and other dangerous substances. But, sometimes your immune system mistakenly attacks your body, which causes inflammation and tissue damage.
Active Uc Of Any Extent Not Responding To Aminosalicylates
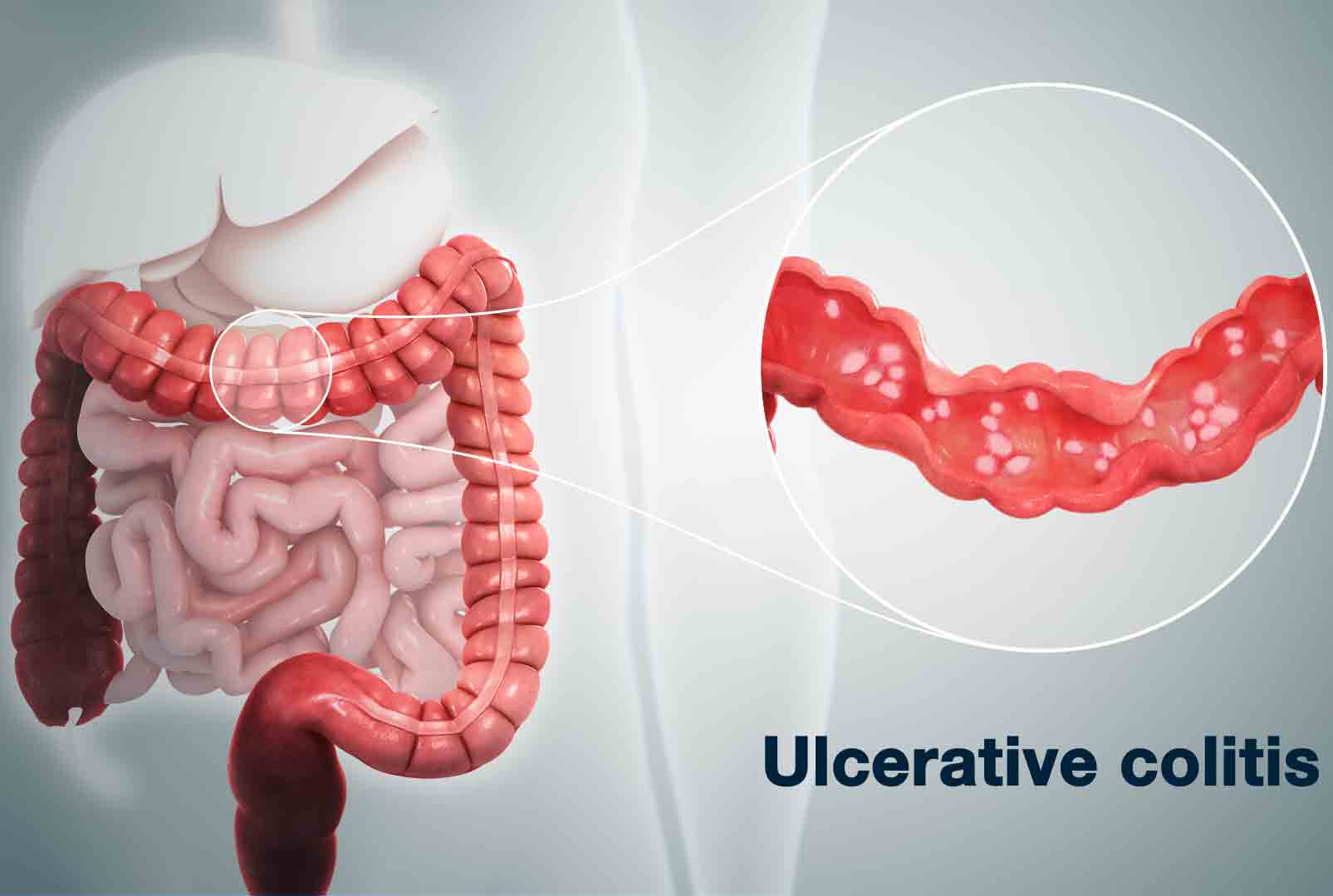
In mild-to-moderate UC of any extent, aminosalicylates such as mesalamine are the preferred initial treatment . In patients with disease activity limited to the rectum, topical therapy alone might suffice, but combination therapy is more effective and is also recommended for left-sided and extensive UC . Table 2 gives an overview on current treatment options.
Table 2.
Medical therapy for UC
Fig. 1.
Active ulcerative colitis of any extent not responding to 5-aminosalicylates . MMX, multimatrix AZA, azathioprine 6-MP, 6-mercaptopurine.
Except in case of isolated proctitis, where topical corticosteroids alone may be considered, treatment with oral corticosteroids should be initiated in patients who do not respond adequately to 5-ASA . In case of isolated proctitis, topical corticosteroids alone might be considered. The introduction of corticosteroids should be a shared decision-making process that includes patients preference of therapy and tolerance to 5-ASA. It is, however, recommended to start corticosteroids in patients with sustained rectal bleeding for 2 weeks, persistent abdominal symptoms after 6 weeks of adequate therapy with 5-ASA or if symptoms deteriorate . In selected cases, a prolonged therapy with up to 16 weeks might still be able to achieve remission.
Read Also: Ulcerative Colitis Social Security Disability
Secondary Loss Of Response
Secondary loss of response refers to patients who had previously responded to a biologic agent but then demonstrated evidence of ongoing disease activity despite continued therapy. Once ongoing inflammation has been confirmed, the drug level and antibodies to the drug should be assessed if the assay is available . After drug levels and antibodies are assessed, the drug dosing should be increased if drug levels are low and antibodies are not present, switched to another drug in the class if drug levels are low and antibody levels are high, or switched to another drug mechanism if drug levels are high and antibodies are not present .
Primary Nonresponse Vs Secondary Loss Of Response
Once a patient has been evaluated for infection and objective evidence of active IBD has been found, the clinician needs to determine whether the symptoms represent primary nonresponse to the biologic drugs mechanism of action or secondary loss of response. Primary nonresponders may react to a different class of drugs, whereas secondary loss of response may be addressed through dose escalation or the addition of an immunosuppressant.
You May Like: Stage 2 Pressure Ulcer Treatment Dressing
What Is A Flare
When you have ulcerative colitis, your physician will try to find the right medications to control your symptoms. However, since there is no cure, the systemic disease is always there. When the symptoms arent present, you are in remission. If the symptoms return, especially if they are worse than before, it is a flare. This is why it is important to continue taking any medications your doctor prescribes, even if you feel better. If you stop taking your medication, then you can increase your chance of experiencing a flare and progression of the disease. Infections, stress, and taking antibiotics or NSAIDs can also make you more susceptible to a flare.
Follow A Recommended Corticosteroid Dose
Corticosteroids are common treatments for UC flare-ups. It is important that a person follows their exact dosage over time.
Doctors may prescribe a higher dose that reduces gradually over time.
This is because if a person takes too much of a corticosteroid over a long period, it can put them at a greater risk of a number of problems, including heart problems and mood disorders.
It is important that a person gradually tapers off their use of corticosteroids. This is because instantly or rapidly stopping the course may harm their body.
Read Also: Surgical Management Of Ulcerative Colitis Ppt
Make Some Dietary Changes
Keep in mind that medication is not the only way of controlling your symptoms. Many times, modifying your diet may also help because there are many foods and drinks that are known to aggravate your Ulcerative Colitis symptoms. You should avoid or restrict the intake of these foods if you know that they aggravate your symptoms. Some of these foods and beverages that worsen Ulcerative Colitis symptoms include:
- Coffee, sodas, tea, and other caffeinated drinks
- Milk and other dairy products
- Fried foods
- High-fiber foods such as whole-grain bread
- Cruciferous vegetables such as broccoli and cabbage
- Steak
- Artificial sweeteners and colors
- Peanuts
- Oils like coconut oil and olive oil
Remember that your diet has a vital role to play in your overall health and can also help you recover from acute Ulcerative Colitis symptoms such as diarrhea, abdominal pain, etc. Maintaining a food diary will help you pinpoint exactly which foods and drinks worsen your symptoms.
What Is The Best Diet For Ulcerative Colitis
Theres no single diet that works best for ulcerative colitis. If the disease damages the lining of the colon, your body might not absorb enough nutrients from food. Your healthcare provider may recommend supplemental nutrition or vitamins. Its best to work with your provider and nutritionist to come up with a personalized diet plan.
Read Also: Ulcerative Colitis Left Side Pain
What Should I Ask My Doctor
If you have ulcerative colitis, you may want to ask your healthcare provider:
- How much of my large intestine is affected?
- What risks or side effects can I expect from the medication?
- Should I change my diet?
- Will ulcerative colitis affect my ability to get pregnant?
- What can I do at home to manage my symptoms?
- What are my surgical options?
Ulcerative Colitis Constipation: Tips For Relief

Constipation may be a problem for you if you have ulcerative colitis , an inflammatory bowel disease . According to one study on individuals with ulcerative colitis, nearly half experienced proximal constipation. Proximal constipation refers to constipation that occurs alongside other abdominal symptoms, including abdominal pain, cramping, and the feeling that the bowels have not been completely emptied .
In some cases, UC only affects one side of the colon . Research has shown that people with this form of UC are more likely to experience constipation as a symptom. If you experience constipation with ulcerative colitis, there are several ways you can manage it, at home and with your doctors help.
Recommended Reading: How Can You Tell You Have An Ulcer
What Is Considered Long
Long-term prednisone use is the use of the medication for more than a month.
Using prednisone long term can have adverse effects. The longer the treatment time, the more negative side effects can be expected.
Long-term use of corticosteroids can cause other conditions, such as diabetes, cataracts, high blood pressure, and osteoporosis.
To manage UC long term, talk to your healthcare provider about other options for controlling your disease.
Severe Or Fulminant Colitis
Severe or fulminant colitis. Patients need to be hospitalized immediately with subsequent bowel rest, nutrition, and IV steroids. Typical starting choices are hydrocortisone 100 mg IV q8h, prednisolone 30 mg IV q12h, or methylprednisolone 16â20 mg IV q8h. The last two are preferred due to less sodium retention and potassium wasting. 24-hour continuous infusion is preferred than the stated dosing. If the patient has not had any corticosteroids within the last 30 days, IV ACTH 120 units/day as continuous infusion is superior than the IV steroids mentioned above. In either case, if symptoms persist after 2â3 days, Mesalazine or hydrocortisone enemas daily or bid can be given. The use of antibiotics in those with severe colitis is not clear. However, there are those patients who have sub-optimal response to corticosteroids and continue to run a low grade fever with bandemia. Typically they can be treated with IV ciprofloxacin and metronidazole. However, in those with fulminant colitis or megacolon, with high fever, leukocytosis with high bandemia, and peritoneal signs, broad spectrum antibiotics should be given . Abdominal x-ray should also be ordered. If intestinal dilation is seen, patients should be decompressed with NG tube and or rectal tube.
Read Also: Different Types Of Ulcerative Colitis
Tell Other Health Professionals Youre Taking Steroids
You must tell any doctor, dentist or other health professional treating you that youre taking steroids. If you have a steroid alert card, always carry this with you.
You can drink alcohol in moderation while taking steroids, but you may be more likely to have stomach problems.The Department of Health recommends drinking no more than 14 units of alcohol per week thats around six pints of beer or six glasses of wine.
Always speak to your IBD nurse if you have any concerns or side effects. They see lots of people with IBD and have lots of valuable experience.
Barry, age 41Living with Crohn’s Colitis
We offer more than 50 publications on many aspects of Crohns Disease, Ulcerative Colitis and other forms of Inflammatory Bowel Disease. You may be interested in our comprehensive booklets on each disease, as well as the following publications:
Some Ingredients In Supplements
Some supplements are very beneficial for people with UC. These include calcium, folic acid, and iron. However, some ingredients in supplements may worsen the symptoms of UC.
According to the Crohns and Colitis Foundation, people should avoid supplements that contain:
- lactose
- preservatives
All of these may aggravate a persons UC symptoms, particularly during a flare-up.
The Crohns and Colitis Foundation also adds that people should avoid taking any supplements on an empty stomach.
A person should check with a medical professional before taking any supplements, including herbal supplements, over-the-counter medications, and complementary therapies.
Don’t Miss: What Causes Acute Ulcerative Colitis
Can You Ever Stop Taking Uc Meds
UC is a chronic disease with no cure, says Tauseef Ali, MD, chief of gastroenterology at SSM Health St. Anthony Hospital in Oklahoma City. Unlike a cut, UC doesnât heal and get better. Without treatment, the inflammation comes back. That means youâll likely have to take medications for the rest of your life. These may include anti-inflammatory drugs, immune system suppressors, and biologic therapies.
In rare cases, people whoâve been in remission for years with no signs of inflammation can try going off their medicine. But this is always done under a doctorâs care, Ali says. Youâll need to get regular blood tests and endoscopies to check for inflammation.
Ulcerative Colitis Causes And Risk Factors
The exact cause of ulcerative colitis remains unknown. Most medical practitioners claim it to be a result of a problem with the immune system.
Causes
These include:
- GeneticsStudies report that more than one in four people suffering from ulcerative colitis have a family history of the condition. Research studies have also pointed out the presence of certain abnormal genes, which are present in people with ulcerative colitis.
- Overactive immune systemResearchers believe that an abnormal immune reaction in the intestine may be one cause of ulcerative colitis. Presence of certain bacteria or viruses may trigger an immune response, which attacks the inner lining of the large intestine. The immune response then leads to inflammation which gives rise to the symptoms.
- Environmental factorsEnvironmental factors such as stress and an intake of certain medications can also cause ulcerative colitis.
Risk Factors
As previously stated, the exact cause of ulcerative colitis remains unknown. Hence, the suspected causes also tend to be the risk factors of the condition.
- Ulcerative colitis can occur in people of any age group. However, certain people may be at a higher risk of developing it. It is more likely to develop in people who:
- Belong to the age group of 15-30 years.
- Are older than 60 years,
- Have a family history of an inflammatory bowel disease.
Recommended Reading: Support Surfaces For Pressure Ulcer Prevention
Ulcerative Colitis Prognosis And Complications
Prognosis
Ulcerative colitis is an unpleasant disease to deal with and can have a significant impact on the individuals lifestyle. The longer the person suffers from the disease, the higher is the risk of complications. Long-term presence of ulcerative colitis also increases the risk of developing colon cancer. Hence, the course of treatment for ulcerative colitis has to be carefully chosen. During the treatment or even after surgery, regular check-ups are essential.
Complications
Surgery For Ulcerative Colitis
Surgery can eliminate ulcerative colitis but it typically means removal of the entire colon or rectum. Removing all or part of the rectum and colon is usually reserved for severe cases or ones presenting serious complications, says Dr. Englander. In some cases, the surgeon will remove the colon and rectum, then create a J-pouch from the small intestine that acts like a new rectum. Other times, the digestive systems might be connected to an external pouch that collects stool for the patients to dispose of.
Also Check: Nursing Care Plan For Pressure Ulcer Prevention
Dose Optimization Of Certolizumab Pegol And Golimumab
Although assays are not commercially available to assess drug levels or antibodies to certolizumab pegol or golimumab, clinical trial data for both agents suggest that antibodies can form to both drugs, and the incidence of antibody formation to the drugs decreases with the use of immunomodulators. Dose intensification was also allowed in the MUSIC trial, discussed below, and may be an option in patients who are not responding to standard dosing of certolizumab pegol.
In a trial assessing golimumab maintenance therapy for patients with UC, the incidence of antibodies through week 54 was 2.9% . The rate was lower for patients who received concomitant immunomodulators vs patients who were on golimumab monotherapy .
Is It Important To Treat A Flare Early Or Is It Ok To Wait A Bit
Inflammation typically does not resolve without treatment and early intervention has a better outcome than waiting to treat. At an early stage of a flare, a more optimal baseline treatment is often enough to get the inflammation under control. If you wait, there is a greater risk that you might need drugs with greater side effects, such as oral steroids. By waiting, you will have to manage longer with your symptoms before getting relief. Living with constant or longer periods of inflammation might increase your risk for future complications, as inflammation might cause damage to the gut wall that accumulates in severity with each flare.
If you are experiencing worsening symptoms, you have probably already had the flare for some time without symptoms. Evidence shows that a stool test for inflammation in the colon, called fecal calprotectin, is often elevated for two to three months before any symptoms appear. Your colon might also start to show visual evidence of inflammation before you have symptoms, or at least indicate an increased risk for a flare.
Read Also: How Do You Heal An Ulcer