Complementary And Alternative Medicine
Probiotics may modestly reduce disease activity in active disease, but do not increase remission rates.34 However, Lactobacillus GG and Escherichia coli Nissle 1917 have been shown to be as effective as 5-ASA for maintenance therapy.16,17 Acupuncture has shown a small symptomatic benefit in active disease.35 Wheatgrass has also shown some effectiveness in reducing symptoms of active disease.36
Panel: Major Differential Diagnoses In Diagnostic Examination Of Ulcerative Colitis74
- Infectious colitis: bacterial, viral, fungal , mycobacterial, and Clostridium difficile
- Ischaemic colitis
- Segmental colitis associated with diverticulitis
- Radiation-induced colitis or proctitis
- Medication-induced colitis
- Crohns disease
- Sexually transmitted diseases : Chlamydia trachomatis, Neisseria gonorrhoeae, herpes, and syphilis
- If predominant symptom is diarrhoea and not bleeding: coeliac disease, microscopic colitis, lactose or other food intolerances, and irritable bowel syndrome
Future Directions And Controversies
The number of drugs modulating different disease pathways is expected to expand in the near future. There are at least 27 new drugs for ulcerative colitis with either recently completed or active trials.170 One example is the oral pan-janus kinase inhibitor tofacitinib, which has shown higher rates of clinical remission than placebo in phase 2 studies.171 Etrolizumab, a subcutaneous monoclonal antibody that blocks the 7 subunit of the heterodimeric integrins 47 and E7 achieved higher clinical remission rates than placebo in a phase 2 trial.172 An oral anti-4 integrin therapy significantly increased clinical remission and endoscopic healing in a phase 2 trial.173 An oral drug inhibiting sphingosine-1-phosphate receptors that blocks lymphocyte egress from lymph nodes has also shown efficacy.174 In a small trial of 5-ASA non-responders, curcumin increased endoscopic remission in mild to moderate ulcerative colitis as an add-on therapy.175 Biosimilar biological drugs should decrease the cost of therapy. Results from initial studies with an infliximab biosimilar, CT-P13, have shown efficacy at inducing endoscopic healing in ulcerative colitis.176 However, immunogenicity and efficacy remains a concern particularly in patients switching from the originator to the biosimilar.177
You May Like: How To Heal Peptic Ulcer Naturally
About Irritable Bowel Syndrome
IBS is fairly common, with anywhere from 25-45 million Americans suffering from it. The basic cause isnt understood, but you suffer symptoms because your colon muscle contracts more readily than normal. Triggers for IBS include certain foods, stress, hormones, or other illnesses.
Symptoms of IBS may involve:
- Harder or looser bowel movements than normal
- Pain or cramps in the abdomen, usually in the lower half
- Diarrhea, constipation, or alternating between the two
Rectal bleeding and black stool is not a symptom of IBS. You should seek immediate evaluation at our office if you experience possible blood in your stool.
Rest assured that IBS does not raise your risk of developing other serious issues of the digestive system, including colitis, Crohns disease, or cancer.
Are Inflammatory Bowel Diseases Different From Irritable Bowel Syndrome
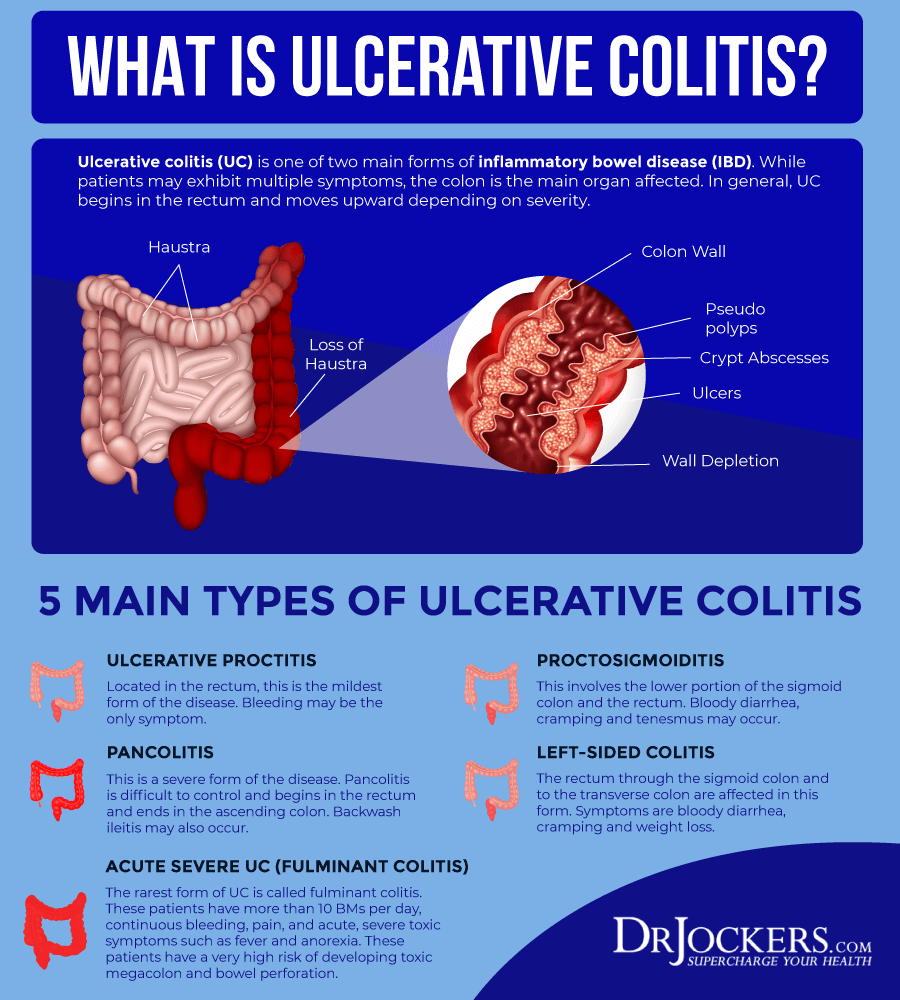
Yes! IBD and IBS are very different, even though the symptoms can be similar. Most importantly, the treatments are not the same. Working with your provider to figure out what condition you have is important so that you can find the best treatment.
IBS is much more common than IBD. About 11% of people have IBS. That makes it about 10 times more common than IBD.
Fortunately, its also less serious. IBD is caused by inflammation and damage to the GI tract. With IBS, this isnt the case. IBS is a collection of gut symptoms caused by unusual functioning of the bowel.
Don’t Miss: Can Stomach Ulcers Be Cured
Symptoms Of Ulcerative Colitis
Most symptoms are related to the inflamed rectum. The inflammation does not allow the rectum to stretch or store properly. This affects a patient’s ability to sense what is in the rectum, making them feel the urgency to use the bathroom more often. Very little stool will pass during these many trips to the bathroom â sometimes just mucus and blood.
When inflammation spreads to the lower part of the intestine, people can feel paradoxically constipated. The reason for this is that the bowel above the inflammation is working fine, but when it gets to the inflamed area, it can’t stretch like it is supposed to. That can cause an internal back up, causing bloating and gas.
Some people may experience extraintestinal manifestations, which refers to inflammation in other parts of their body. The most common manifestation is symmetrical joint pain, which occurs on both sides of the body, often in smaller joints. Other less common types include skin and/or liver inflammation. Extraintestinal manifestations are connected to the bowel inflammation and will get better if the inflammation in the large intestine is treated.
When To Get Treatment
An increase in inflammation causes a flare, and the nature of inflammation means that you should treat it as quickly as you can. Inflammation grows exponentially, because inflammation itself causes an increase in inflammation. The longer you leave it untreated, the worse it will get. In addition, untreated inflammation not only leads to the symptoms associated with ulcerative colitis, it can also increase your risk of developing complications such as colorectal cancer down the line. Pay attention to your symptoms, and visit your physician if you notice that they change or increase even a small amount.
Read Also: Is Imodium Safe For Ulcerative Colitis
What Are The Causes Of Ulcerative Colitis
We do not yet know what causes this disease. Studies indicate that the inflammation in ulcerative colitis involves a complex interaction of factors: the genes the person has inherited, the immune system, and something in the environment. Foreign substances in the environment may be the direct cause of the inflammation, or they may stimulate the bodys defenses to produce an inflammation that continues without control. In patients with ulcerative colitis, once the patients immune system is turned on, it does not know how to properly turn off. As a result, inflammation damages the intestine and causes the symptoms of ulcerative colitis. One of the major goals of medical therapy is to help patients to better regulate their immune system.
Dont Miss: How Do Biologics Work For Ulcerative Colitis
What Are The Symptoms Of Ulcerative Colitis
Ulcerative colitis symptoms often get worse over time. In the beginning, you may notice:
- Diarrhea or urgent bowel movements.
- Abdominal cramping.
- Loss of fluids and nutrients.
Symptoms are similar in pediatric ulcerative colitis and may also include delayed or poor growth. Some ulcerative colitis symptoms in children can mimic other conditions, so it is important to report all symptoms to your pediatrician.
Also Check: Signs Of Stomach Ulcer In Adults
Eat This: The Best Ulcerative Colitis Diet Foods
People with ulcerative colitis are more likely to experience vitamin shortages due to the possibility that they won’t be able to eat a variety of meals. Other elements, like issues with nutrition absorption, may also play a role in this.
Anyone with UC must consume meals abundant in vitamins and minerals, such as iron, calcium, and vitamin A, to make sure they obtain enough nutrients.
For those with ulcerative colitis, the following foods might be better options:
Fruits low in fiber: Bananas, watermelons, peaches, papayas, etc.
Cooked vegetables: Those who suffer from UC may be able to tolerate cooked, skinless, non-cruciferous vegetables. These consist of asparagus tips, cucumbers, and squash.
Probiotic foods: Include yogurts, which have probiotics that are active. Digestion may be aided by the “good” bacteria in them. According to several studies, taking probiotics frequently can help lessen the symptoms and flare-ups of colitis.
Omega-3-rich foods: Consuming foods high in omega-3 fatty acids, such as salmon, walnuts, flaxseed, and chia seeds, may be beneficial.
How Is Ibd Diagnosed
- A combination of endoscopy or colonoscopy and imaging studies, such as:
- Contrast radiography.
- Types of common medications to treat IBD:
- 5-aminosalicyclic acids.
Links with this icon indicate that you are leaving the CDC website.
- The Centers for Disease Control and Prevention cannot attest to the accuracy of a non-federal website.
- Linking to a non-federal website does not constitute an endorsement by CDC or any of its employees of the sponsors or the information and products presented on the website.
- You will be subject to the destination website’s privacy policy when you follow the link.
- CDC is not responsible for Section 508 compliance on other federal or private website.
Also Check: Side Effects Of Bleeding Ulcer
What Causes Ulcerative Colitis Vs Crohns Disease
Its not entirely known what causes ulcerative colitis or Crohns disease. However, experts believe it has something to do with genetic factors and environmental factors . Your gut microbiomethe bazillion bacteria that live in your digestive tractis thought to have influence as well. In fact, a 2020 study published in the journal Frontiers of Medicine, found that not only was the gut bacteria in people with IBD different from people without IBD, but it was also different between people with ulcerative colitis vs. people with Crohns disease.4
What is known is that something sets off your immune system to mistakenly attack healthy areas of your digestive tract, causing chronic inflammation.
This overreaction of the immune system can also affect areas outside of your digestive system and can include your skin, eyes, and other organs. This can occur with both ulcerative colitis and Crohns disease, but ulcerative colitis is more likely to affect the skin, eyes, and bones, while Crohns disease is more apt to affect the kidneys and gallstones.1
Read Also: What Is Good For Ulcers
Can Celiac Disease Be Confused With Ulcerative Colitis
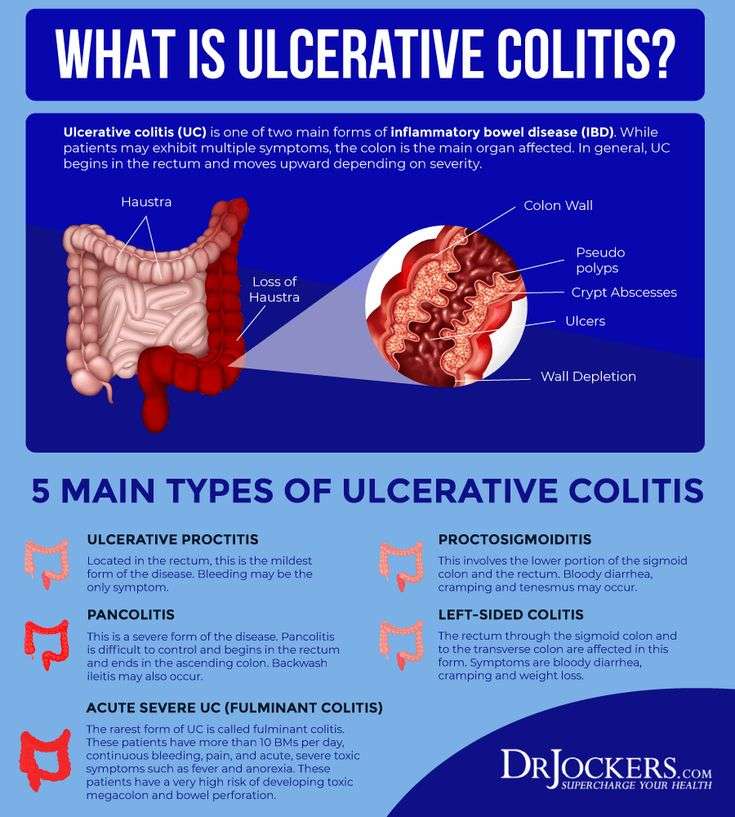
While celiac disease and ulcerative colitis are both diseases of the digestive system that are associated with abdominal discomfort, they present with symptoms that would differentiate them. The presence of bloody diarrhea points to celiac disease. The presence of symptoms beyond the digestive tract, for example, muscle cramps, joint pains, and tingling in the lower extremities, suggests ulcerative colitis as opposed to celiac disease.
Recommended Reading: Bed To Prevent Pressure Ulcers
Ulcerative Colitis And Diverticulitis: Whats The Outlook
UC is a lifelong condition, and your symptoms may come and go. About 30% of people with UC have severe symptoms, and flare-ups might happen more frequently. While medications often help, surgery may also be needed.
In contrast, most cases of diverticulitis, even though itâs also considered a lifelong condition, clear up with a 7- to 10-day course of antibiotics and plenty of rest. If you have severe symptoms, talk to your doctor about other treatment options.
Managing your diet and stress and making time for regular physical exercise are key to lowering your risks for both conditions. However, because some of the symptoms are specific, there are steps you can take to avoid your condition flaring up or getting worse.
To prevent diverticulitis, you should:
- Eat more fiber. This helps your poop move better in your digestive tract and reduces any pressure on the colon walls
- Drink lots of water, this prevents constipation.
If youâre not sure what to eat, talk to your doctor.
To lower your odds for UC or manage flare-ups, you should:
- Get plenty of sleep. This can ease emotional stress and keep your immune system in check.
- Avoid using too many nonsteroidal anti-inflammatory drugs . For pain relief and fever, switch to alternatives like acetaminophen .
- Be careful when you take antibiotics. These drugs can trigger UC flare-ups. Let your doctor know if it does.
Show Sources
What Procedures And Tests Diagnose Crohns Disease And Ulcerative Colitis
Doctors diagnose ulcerative colitis by endoscopy . During this procedure the doctor can see and take pictures of the patients abnormal gut mucosa , and the presence of continuous disease . Other blood tests and imaging tests like CT scan or MRI are used, but these tests are not definitive.
Doctors use the same procedures and tests to diagnose Crohns disease. However, they also use small bowel studies, colonoscopy, and upper GI endoscopy to identify the abnormal gut mucosa that usually occur in multiple areas anywhere in the intestinal tract. These areas are not continuous, but are separated by normal areas of intestinal mucosa that distinguish them from ulcerative colitis lesions.
As with Crohns disease, nutrition is important if you have ulcerative colitis because symptoms of diarrhea and bleeding can lead to dehydration, electrolyte imbalance, and loss of nutrients. It may be necessary to take nutritional supplements if your symptoms do not allow you to eat a nutritionally balanced diet. Talk to your health-care professional about what supplements to take.
Recommended Reading: Icd 10 Stage 4 Sacral Ulcer
Effects Of Crohns Disease And Ulcerative Colitis
Every person responds differently to IBD. The severity of symptoms will vary from time to time and from person to person. IBD is not a progressive disease . Rather, flare-ups can range from mild to severe and back to mild again. Some people will experience periods of relief from symptoms in between flare-ups.We cannot predict how long a person will stay free from symptoms, or when their next flare-up will occur. Some flare-ups settle down quite quickly with treatment. Other times, it may take months for a persons symptoms to respond to treatment.IBD interferes with a persons normal body functions. Signs and symptoms can include:
- pain in the abdomen
- delayed or impaired growth in children.
How Can I Tell If I Have Ulcerative Colitis Or Crohns Disease
Its important that you, your healthcare provider, and a GI specialist work together closely to figure out whats causing your symptoms. This is especially important since the symptoms of Crohns disease and ulcerative colitis can be similar. Your providers may check blood work and a stool sample. To get an accurate diagnosis, your GI specialist may do a colonoscopy, where a camera is pushed into the colon. Your provider will look at the inside of the colon and take tissue samples, which are important for making the right diagnosis. Your providers might get a CT scan or an MRI of your abdomen to check for complications related to your condition.
Recommended Reading: Ulcerative Pancolitis With Rectal Bleeding
What Symptoms Do Colitis And Ulcerative Colitis Share
Colitis can cause similar belly and bowel issues no matter the cause. Some symptoms are mild while others are more serious.
General signs of colitis and UC include:
- Stomach cramps that come and go
- Constant belly pain
- Mucus or blood in your poop
- Weight loss without trying
- An urgent need to poop
- A feeling like you didnât get all your poop out
If you have periods, you may have:
- Worsening diarrhea during your period
Is It Important To Treat A Flare Early Or Is It Ok To Wait A Bit
Inflammation typically does not resolve without treatment and early intervention has a better outcome than waiting to treat. At an early stage of a flare, a more optimal baseline treatment is often enough to get the inflammation under control. If you wait, there is a greater risk that you might need drugs with greater side effects, such as oral steroids. By waiting, you will have to manage longer with your symptoms before getting relief. Living with constant or longer periods of inflammation might increase your risk for future complications, as inflammation might cause damage to the gut wall that accumulates in severity with each flare.
If you are experiencing worsening symptoms, you have probably already had the flare for some time without symptoms. Evidence shows that a stool test for inflammation in the colon, called fecal calprotectin, is often elevated for two to three months before any symptoms appear. Your colon might also start to show visual evidence of inflammation before you have symptoms, or at least indicate an increased risk for a flare.
Also Check: Ulcerative Colitis Shortness Of Breath
Differences Between Ulcerative Colitis And Crohn’s Disease
The differences between ulcerative colitis and Crohn’s disease are:
- In Crohn’s disease, there are healthy parts of the intestine mixed in between inflamed areas. Ulcerative colitis, on the other hand, is continuous inflammation of the colon
- Ulcerative colitis only affects the inner most lining of the colon while Crohn’s disease can occur in all the layers of the bowel walls
J& j Sues Amgen Over Plan To Sell Ulcerative Colitis Drug Similar To Stelara
-Johnson & Johnsons Janssen unit has sued Amgen Inc over its plan to market a drug for ulcerative colitis and other conditions similar to J& Js Stelara, saying it would infringe two patents in a lawsuit made public on Wednesday.
Stelara is J& Js top-selling drug, accounting for $9.1 billion of the companys $52 billion in global drug sales last year. Sales for the first nine months of this year were $7.3 billion, up 7.9% over the same period last year.
The drug is also approved to treat Crohns disease, the skin condition psoriasis and a related form of arthritis. It is a biologic drug, meaning it is made inside living cells.
A 2009 law allows companies to make so-called biosimilar versions of biologic drugs that can be substituted for them, much like generic versions of conventional drugs. However, J& J alleges that Amgen failed to follow the legal process required by that law for the companies to litigate any patent disputes.
If Amgen launches its drug, J& J said it would infringe J& Js patent on the drugs active ingredient and on its use for treating ulcerative colitis.
Amgen did not immediately respond to a request for comment.
Also Check: Can Ibuprofen Cause Ulcerative Colitis
How Ulcerative Colitis Is Treated
Treatment for ulcerative colitis aims to relieve symptoms during a flare-up and prevent symptoms from returning .
In most people, this is achieved by taking medicine, such as:
- aminosalicylates
- corticosteroids
- immunosuppressants
Mild to moderate flare-ups can usually be treated at home. But more severe flare-ups need to be treated in hospital.
If medicines are not effective at controlling your symptoms or your quality of life is significantly affected by your condition, surgery to remove your colon may be an option.