What Is Ulcerative Colitis
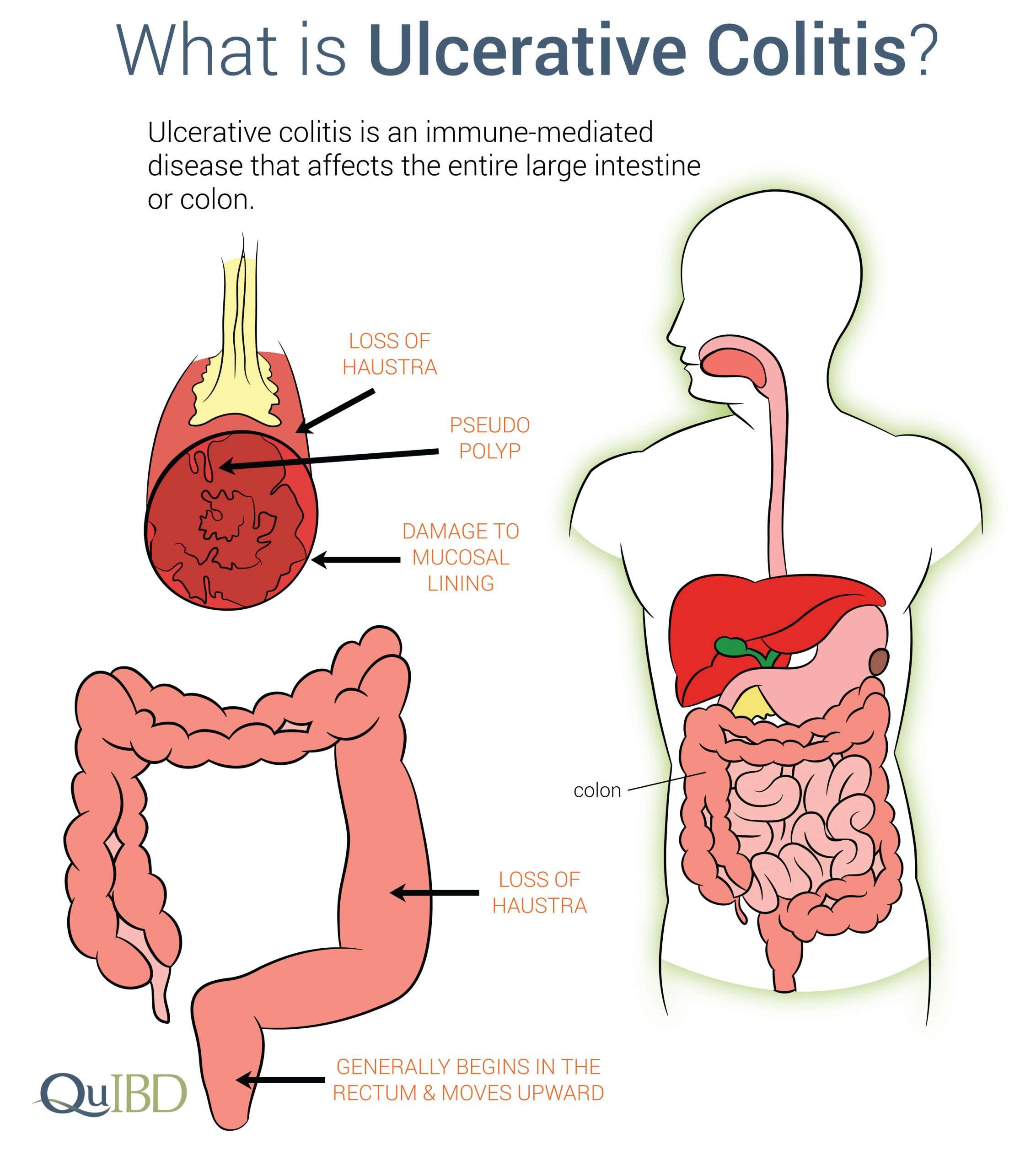
Ulcerative colitis is an inflammatory bowel disease characterized by bloody diarrhea where the colon and the rectum become inflamed.
Ulcerative colitis is an autoimmune condition that causes inflammation and ulcers on the inner lining of the large intestine.
Along with Crohn’s disease, these two major forms of inflammatory bowel disease represent distinct syndromes with overlapping features.
Extended Data Fig 7 Proportion Of Resident
a, Proportion of resident-like macrophages and inflammatory macrophages among total colonic macrophages represented in individual samples of healthy controls UC and patients. b, Heat-map showing color-coded down-sampled UMI counts of gene programs identifying LPS signature , immune complexes signature and resident macrophage genes signatures .
Sporadic Adenomas Versus Dalms
Patients with ulcerative colitis may also have sporadic adenomas, which must be distinguished from the dysplasia associated with ulcerative colitis , because sporadic adenomas do not appear to carry the same implications for carcinoma risk in these patients. It is helpful for the endoscopist to submit biopsies of the flat “shoulders” of raised lesions specimens should be in separate containers and specifically labeled.
The absence of flat dysplasia near polypoid dysplasia is helpful for distinguishing sporadic adenomas from dysplasia that may involve endoscopically flat mucosa. If dysplasia is seen in an area of active disease and is flat, one may favor a DALM however, if the patient is in remission or if a polypoid lesion is seen in a noninflamed area without adjacent flat dysplasia, one may diagnose a sporadic adenoma, especially in an older patient who has had adenomas before.
Unfortunately, it often is not possible for the pathologist to make a specific distinction, because there may be insufficient sampling of flat mucosa near the polyp or because the pathologist may not have been provided with the endoscopic or clinical information.
Also Check: Stage 2 Pressure Ulcer Treatment Cream
Complementary And Alternative Medicine
Probiotics may modestly reduce disease activity in active disease, but do not increase remission rates.34 However, Lactobacillus GG and Escherichia coli Nissle 1917 have been shown to be as effective as 5-ASA for maintenance therapy.16,17 Acupuncture has shown a small symptomatic benefit in active disease.35 Wheatgrass has also shown some effectiveness in reducing symptoms of active disease.36
Search Strategy And Selection Criteria
We searched for relevant manuscripts in PubMed/MEDLINE, Embase, and Cochrane Central from their inception until March 1, 2016. The search combined the MeSH terms ulcerative colitis and inflammatory bowel disease with the subheadings epidemiology, etiology, physiopathology, innate and adaptive immunity, diagnosis, genetics, diagnosis, endoscopy, therapy, surveillance, and complications. Bibliographies of included articles were searched and experts in inflammatory bowel disease were consulted to identify additional studies. Relevant articles and abstracts published in English were critically reviewed. Priority was given to manuscripts published in the past 5 years, randomised placebo-controlled trials, and meta-analyses.
Also Check: Stage 3 Pressure Ulcer Treatment
Extended Data Fig 8 Characterization Of T Cell Clusters From Single
a, Heat-map showing the relative expression of 5 transcriptional scores in single T cells . Cell clusters are demarcated by gray bars. Detailed cell counts per T cluster per sample are accessible in Supplementary Table . b, Euclidean distance for lineage normalized cell type frequencies was compared within healthy controls , , patients with UC and between HC and patients with UC for T cells, Wilcoxon rank-sum test. c, Relative expression of genes identifying T cell subsets. Heatmap is showing log-2 transformed expression per subset divided by the mean expression across all subsets.
What Are The Main Types Of Ibd
| Crohns Disease | Ulcerative Colitis | |
|---|---|---|
| Affected Location | Can affect any part of the GI tract Most often it affects the portion of the small intestine before the large intestine/colon. | Occurs in the large intestine and the rectum. |
| Damaged Areas | Damaged areas appear in patches that are next to areas of healthy tissue. | Damaged areas are continuous usually starting at the rectum and spreading further into the colon. |
| Inflammation | Inflammation may reach through the multiple layers of the walls of the GI tract. | Inflammation is present only in the innermost layer of the lining of the colon. |
Recommended Reading: Ulcerative Colitis Flare Up Duration
Patients And Tissue Specimens
Before the colonoscopy procedure, consecutive male and female subjects were recruited to the present study. The UC diagnosis was based on the medical history, endoscopic findings, histological examination, laboratory tests, and the clinical disease presentation. The extent of UC and the clinical activity were classified in accordance with the Montreal Classification . In brief, the colonic inflammatory involvement is defined as extension combined with a number between 13 . In addition, the clinical severity grade is defined. The S-score ranges from clinical remission to severe UC . Mucosal biopsies were obtained from the rectum and caecum from all participants.
No uses of corticosteroids, aminosalicylates, or immunosuppressants were registered in the control group, while 9 patients in the UC group were treated systemically with corticosteroids . Twenty-seven UC patients were treated systemically with aminosalicylates . Among these, two patients had additional ongoing therapy with aminosalicylate enemas and three patients were treated with corticosteroid enemas . Seven patients had stable ongoing immunosuppressant treatment .
The remaining demographic and clinical data are presented in Figure .
Figure 1
Classification Of Ulcerative Colitis By Severity
There are several classification systems that can be used to assess disease severity. Criteria include:
- Endoscopic findings
| American College of Gastroenterology ulcerative colitis activity index | |
|---|---|
| Criteria | |
| Frequency of blood in stool | Intermittent |
| Truelove and Witts severity index | |
|---|---|
| Criteria | |
| Amount of blood in stool | Small amount |
| ⤠30 mm/hour | > 30 mm/hour |
Treatment recommendations by the ACG are based on the ACG ulcerative colitis activity index, while recommendations by the American Gastroenterological Association are based on a combination of the Truelove and Witts severity index and the Mayo score for ulcerative colitis activity. There is significant overlap among the criteria used in all ulcerative colitis severity indices.
Read Also: What Are The Best Foods To Eat With An Ulcer
Extended Data Fig 3 Characterization Of The 20 Colonic Clusters Of B Cells From Single
a, UMI counts in B lymphocyte and plasma cell clusters. box plots represent the third quartile , median and first quartile of measurements, and the whiskers represent 1.5 times the interquartile range from the top or bottom of the box. b, Heat-map showing color-coded down-sampled UMI counts of highly-variable genes between clusters of B cells and PC . Clusters are demarcated by gray bars. Cells were down-sampled to 2000 UMIs/cell. Detailed cell counts per B and PB/PC cluster per sample are accessible in Supplementary Table . c, Correlation matrix of gene modules defined by gene-to-gene correlation analysis of single cells within the B lymphocyte clusters. d, Heat-map showing color-coded down-sampled UMI counts of gene programs identifying naïve, memory and germinal center-like B lymphocytes. Clusters are demarcated by gray bars. Cells were down-sampled to 2000 UMIs/cell. e,I FN signature scores on the indicated cell types. Supplementary Table shows cell-counts per cluster, box plots represent the third quartile , median and first quartile of measurements, and the whiskers represent 1.5 times the interquartile range from the top or bottom of the box.
Cxcl13+ Tph Cells Are Expanded In Uc
To assess whether T cell alterations might underpin acute B cell responses in UC, we next analyzed single colonic T cell transcriptomes. We identified 15 T cell clusters , and further curation revealed nine T cell subtypes and/or states , the global composition of which differed in UC versus HC . Activated T cells expanded in UC and had high expression of Th17 and Th1 effector cytokines, including IFN-γ .b). This suggests that activated T cells contribute to establish the type 1 microenvironment associated with the IFN signature that we described in a subset of naive B cells-1 , IgG+ PBs and IgG+ PCs . We also identified TPH expressing high levels of the follicular B-cell-attracting chemokine CXCL13 . Colonic CXCL13+ T cells expressed genes such as PDCD1 , CD200, BCL6, TIGIT, ICOS and BATF but no CXCR5 transcripts . In addition, colonic TPH cells expressed several genes in common with regulatory T cells, such as TIGIT, CTLA4, TNFRSF4 and MAF, whereas key Treg-defining genes, such as FOXP3 and IKZF2, were not detected . Although CXCL13 expression was restricted to TPH cells, Treg cells expressed the immunoregulatory cytokine IL-10 . Concordant with previous reports31, IL-17 was also detected in Tregs, although at lower levels than IL-10 . TPH cells, in turn, uniquely expressed the TFH program as well as previously unreported genes, such as NMB, FABP5 and PGM2L1 . The proportion of TPH cells was significantly increased in inflamed UC colon compared to HCs .
Read Also: Treating Hindgut Ulcers In Horses
Analysis Of Cells In Blister Fluid
Exudates were centrifuged at 1,000g for 5min at 10°C, after which supernatants were aliquoted and immediately frozen at 80°C. Cell pellets were resuspended in 100l ACK erythrocyte lysis buffer for 1min, then centrifuged at 1,000g for 5min at 10°C. Supernatants were discarded and cells resuspended in 100l PBS with 5% foetal bovine serum and 0·1% sodium azide . Cell were counted with a manual haemocytometer. Leukocyte subpopulations in blisters and peripheral blood samples were characterized by polychromatic flow cytometry, using a previously described gating strategy . For isolation of circulating leukocytes, 4ml blood was collected, erythrocytes lysed with ACK buffer, and cells washed with PBS prior to resuspension in PBS/5% FBS. Cells were incubated with an antibody cocktail for 30min at room temperature in the dark. Stained samples were washed in PBS containing 1% FBS and 2mM EDTA , then centrifuged at 800rpm for 5min at 4°C. Cells were resuspended in PBS/5%FBS then fixed in an equal volume of 1% paraformaldehyde and stored in the dark at 4°C prior to analysis on a BD LSR FortessaTM or LSR2 flow cytometer . Data were analysed using FlowJo software . Clearance of cells between two time points was defined as /t, where n is the number of cells present at a specified time point, and t the interval between time points.
Immunofluorescence Staining From Colonic Biopsies
Immunofluorescence staining was performed on five patients with untreated active colitis and five HCs. Formalin-fixed, paraffin-embedded human tissue sections 3 μm in thickness were treated in xylene, a decreasing alcohol gradient and distilled water to achieve de-waxing and rehydration of the tissue. Heat-induced epitope retrieval was performed for 15 min in Tris-EDTA buffer . After epitope retrieval, tissue sections were permeabilized with 0.2% Triton X-100 in PBS, blocked with 5% BSA and 5% Fc receptor blocking reagant and stained with polyclonal rabbit anti-human IgA , monoclonal mouse anti-human CD79a and monoclonal rat anti-human Ki67 . Staining with primary antibodies was followed by detection with polyclonal donkey Alexa Fluor 546-conjugated anti-mouse IgG antibody , Alexa Fluor 647-conjugated anti-rabbit IgG antibody and Alexa Fluor 488-conjugated anti-rat IgG antibody . Nuclear DNA was visualized with DAPI, and coverslips were applied with FluorSave reagent . Images were acquired with either a Leica TCS SP5 upright confocal microscope or a Nikon Eclipse Ni-E microscope and were further analyzed with ImageJ software.
Read Also: Stage 1 Pressure Ulcer Pictures
The Names: Ulcerative Colitis Crohns Disease
Burrill B. Crohn
You or a member of your family has been confronted with the diagnosis inflammatory bowel disease or IBD. In most cases, this means either ulcerative colitis or Crohns disease. At first, these names seem strange and you probably wonder what they can mean. Both refer to chronic inflammation of the mucosal lining of the intestine or bowel, though each has quite specific characteristics.
What do the names mean?
The use of different names is based on the fact that the disease is often named according to the portion of the bowel it affects and which becomes inflamed. The chart shows the digestive tract and gives the names of the various segments. The small bowel is normally 35 m in length, while the large bowel or colon is about 1.5 m long. We distinguish between two main forms of IBD.
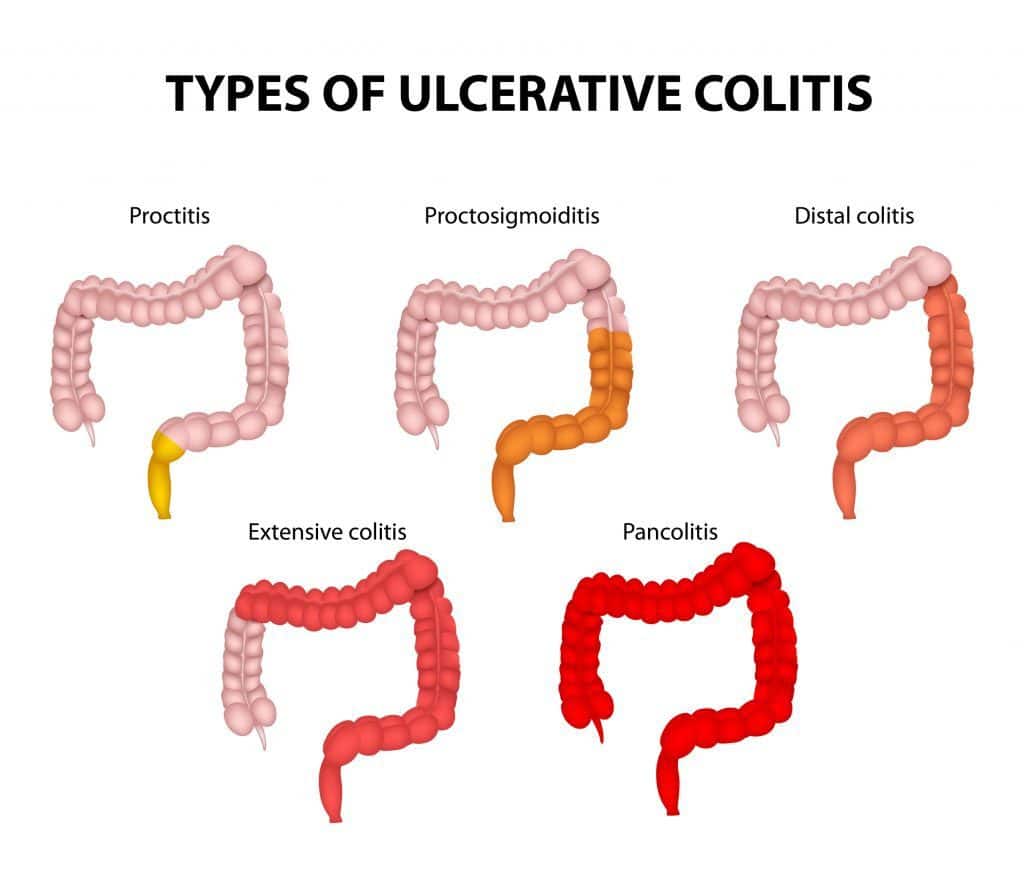
The first is ulcerative colitis, an inflammation affecting only the colon and associated with the formation of ulcers. In some cases, only the rectum is involved, and we speak of ulcerative proctitis .
Major Disruptions Of B Cell Populations In Uc
Next, we examined colonic B cell populations in a subset of patients within the primary cohort using multi-parametric flow cytometry . Consistent with scRNA-seq analyses, there was a significant increase in IgG+IgAâIgMâCD38++CD27+ colonic PC and IgG:IgA PC ratios in patients with active UC compared to HCs ,b), with a significant proportion of actively cycling colonic PCs .d). Using published criteria28, we defined short-lived , long-lived and ultra-long-lived CD38++CD27+ PCs. Concordant with the PB expansion, we observed a significant increase in the frequency of short-lived PCs and the ratio of short-lived PCs:long-lived PCs in patients with UC with active disease .f). Naive B cells were significantly increased in UC inflamed colon as compared to HCs, possibly reflecting the increased proportion of IFN-imprinted naive B cells observed by scRNA-seq analysis . In addition, although HCs and patients with UC had similar frequencies of total CD19+ B cells and CD19+CD38âCD10âCD27+IgMâIgDâ switched memory B cells , significantly higher frequencies of IgG+ SM B cells and IgG:IgA SM B cell ratios were detected in UC .
Major disruptions of B cell populations in inflamed colon of patients with UC.
Overall, these data confirm major changes in the intestinal B cell compartment identified by scRNA-seq and demonstrate an acute âsystemic-likeâ B cell response skewed toward the production of pro-inflammatory IgG most pronounced in the inflamed colon.
Read Also: Fda Approved Drugs For Ulcerative Colitis
Ulcerative Colitis Versus Crohn Disease
To distinguish ulcerative colitis from Crohn disease, a number of factors are considered. Ulcerative colitis is typically a disease that is limited to the colon . This condition generally involves the entire colon diffusely , including the rectum, and inflammation may become worse as it progresses from the right side of the colon to the left. Perianal disease is uncommon, and mesenteric adenopathy is only occasionally seen.
Despite its name, ulcerative colitis often does not present with macroscopic ulcers , and fissuring disease is typically absent. In contrast, Crohn disease is overtly ulcerative, with characteristic fissures.
Unlike Crohn disease, ulcerative colitis does not exhibit transmural inflammation, and serositis is absent, except in the setting of fulminant colitis or toxic megacolon. Instead, the inflammation in ulcerative colitis is typically limited to the mucosa and submucosa. Granulomas are not a characteristic feature of this disease, although granulomas may be seen with mucous extravasation in sites of crypt abscess or crypt destruction. The muscularis mucosa is usually thickened, and mucosal atrophy may be seen.
Medications To Treat Ulcerative Colitis
When treating ulcerative colitis with medications, our goals are to suppress inflammation, heal tissue, and relieve symptoms. Commonly used medications include:
- 5-Aminosalicylic acid : Given orally or rectally, to decrease inflammation in mild or moderate cases
- Corticosteroids: Given topically, orally, or intravenously to quickly decrease inflammation in moderate to severe cases
- Antibiotics: Given orally or IV to reduce intestinal bacteria, suppress the immune system, and treat infection
- Immunomodulators: Given orally or by injection to weaken the activity of the immune system to decrease inflammation
- Biologic agents: Given by injection or through a vein to stop the inflammatory reaction in moderate to severe cases
Also Check: Medications To Treat Ulcerative Colitis
How Can It Be Diagnosed
Ulcerative colitis may have similar symptoms compared to irritable bowel syndrome . The key to the differential diagnosis is the presence of blood in the stools that is not a feature of IBS. The biopsy will show a definitive conclusion.
The presence of bloody diarrhea along with extra-intestinal symptoms are decisive for the diagnosis of ulcerative colitis.
Colonoscopy is the critical diagnostic test. Tissue samples can be taken during a colonoscopy. Plain abdominal radiology of the abdomen may also provide useful information.
Mass Cytometry Data Analysis
The CyTOF panel included 37 antibodies with samples run in three batches of pre-mixed lyophilized antibody. Representative samples were analyzed and visualized using a combination of manual gating and viSNE dimensionality reduction as implemented in Cytobank. For semi-automated analysis of the whole subject cohort, CyTOF-defined populations were detected using a semi-supervised approach through the Astrolabe Cytometry Platform . In summary, single-cell data were clustered using the R package FlowSOM and then labeled using the EkâBalam algorithm based on canonical markers as previously reported54. Cell subset definitions follow the schema defined by Maecker et al.55 and Finak et al.56. Secondary statistics, such as population frequency and median marker expression, were then exported for secondary analyses. We interrogated subtype differences in the percentage of PBs for patients of VCo1, adjusting for age and gender and processing batch in a linear model.
You May Like: Stage 4 Pressure Ulcer Dressing
+ Pbs/pcs In Blood Correlate With Uc Activity
We tested the relevance of circulating gut-homing PBs as a potential cellular biomarker of disease activity in two validation cohorts using complementary methodologies. In VCo1, using mass cytometry, we confirmed that PB frequencies were significantly increased in patients with active versus quiescent UC or HCs .b). We validated increased expression of β7 integrin and CXCR3 and decreased β1 integrin expression in PBs from patients with active UC . Next, we assessed whether levels of circulating PBs could help predict later disease complications. Patients with levels above the median had a significantly higher probability of disease complications over a median follow-up of 1.6 years . PBs were associated with disease complications after adjusting for age, sex, disease extent and disease duration using Cox regression analysis .
An increase in gut-homing PBs/PCs is associated with disease complications and activity in two validation cohorts of patients with active UC.