After The Ulcer Has Healed
Once you have had a venous leg ulcer, another ulcer could develop within months or years.
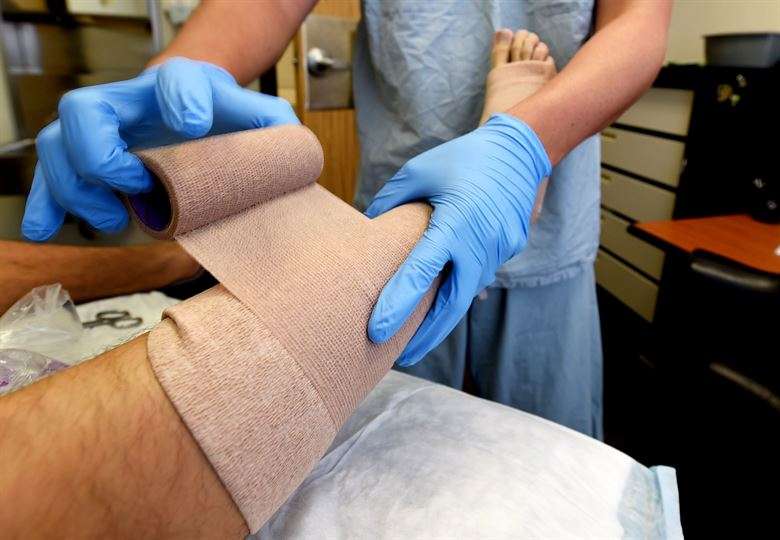
The most effective method of preventing this is to wear compression stockings at all times when you’re out of bed.
Your nurse will help you find a stocking that fits correctly and you can manage yourself.
Various accessories are available to help you put them on and take them off.
Page last reviewed: 11 January 2019 Next review due: 11 January 2022
Healthcare Advice For Leg Ulcers
There are some lifestyle changes you can make that will help boost healing:
- Maintain a healthy weight
- Eat a well-balanced diet that includes 5 portions of fruit and vegetables a day and protein rich foods such as eggs, fish, chicken or pulses
- Take light to moderate exercise such as cycling or walking for about thirty minutes at least three times a week
- Avoid standing or sitting for long periods of time
- Put your feet up elevate your legs above your heart.
- Every so often, move your feet around in circles, then up and down. This helps blood circulate and get back to your heart
Data Collection And Analysis
Selection of studies
Two review authors independently assessed titles and abstracts of studies from the search for relevance and design, in accordance with the selection criteria. We obtained articles if they satisfied the inclusion criteria, or if there was any doubt regarding exclusion. Two review authors independently selected the trials for inclusion we resolved disagreements by discussion.
Data extraction and management
One review author extracted data unblinded and another review author checked this for accuracy .
Assessment of risk of bias in included studies
We assessed the risk of bias of each included study using the Cochrane Collaboration tool for assessing risk of bias . This tool addresses specific domains, namely sequence generation, allocation concealment, blinding, incomplete outcome data, selective outcome reporting and other issues . A risk of bias table was completed for each eligible study.
We will present assessment of risk of bias using a ‘risk of bias summary figure’, which presents all of the judgments in a crosstabulation of study by entry. This display of internal validity indicates the weight the reader may give the results of each study .
Methodological quality summary: review authors’ judgements about each methodological quality item for each included study.
Data synthesis
Subgroup analysis and investigation of heterogeneity
Also Check: Best Prebiotic For Ulcerative Colitis
Ten Top Tips On Leg Ulcers
Una Adderley04 Jun 2018
Side Effects Of Leg Ulcers
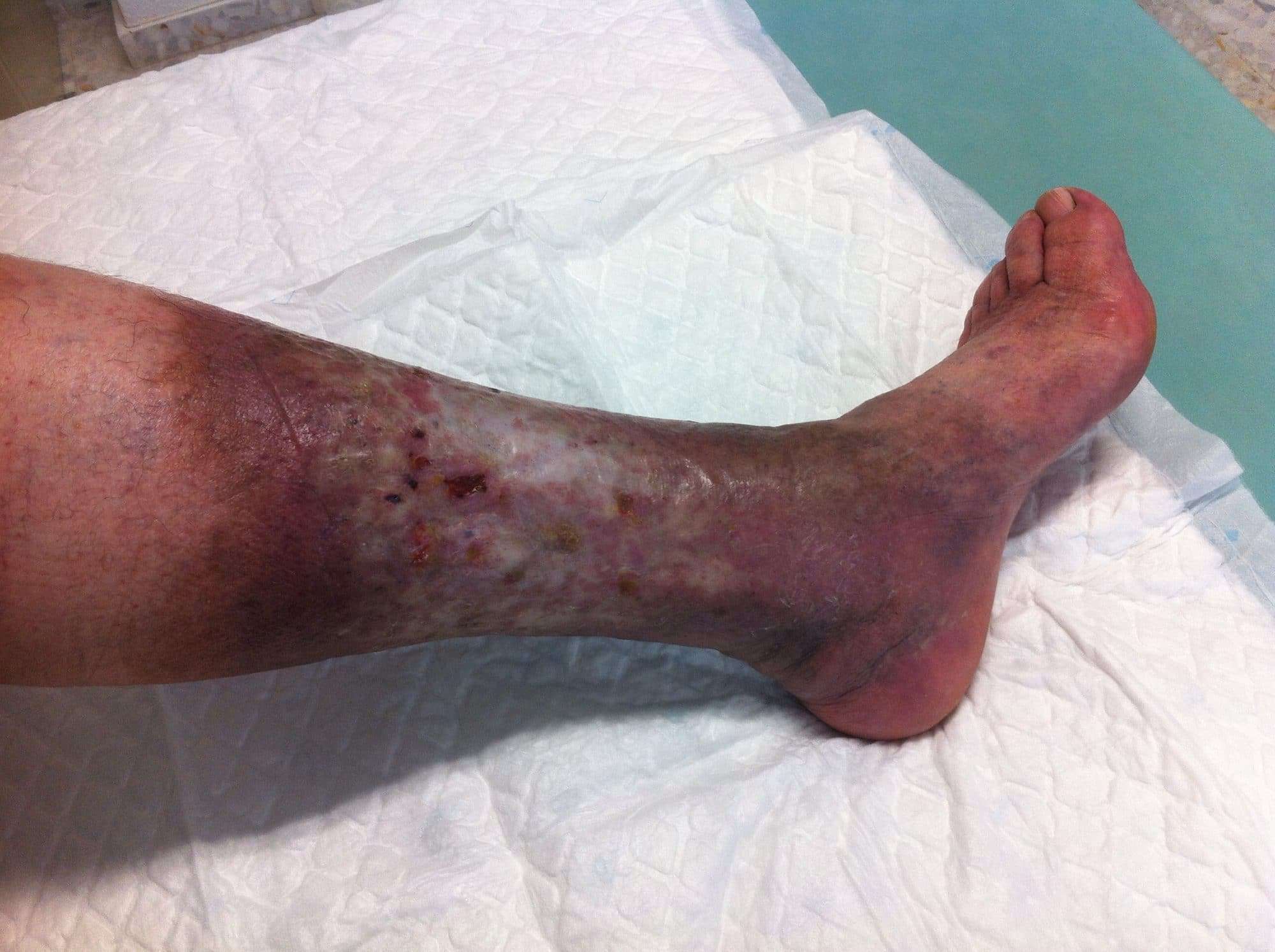
- Fever
- A green and foul-smelling discharge from the ulcers
- The skin around the ulcers begins to swell
- The sores become bigger
- Inflamed skin around the ulcers
Leg ulcers resemble sores that develop when bacteria enter underlying tissues through injured or broken skin. While skin injuries are the most common risk factor for leg ulcers, certain underlying medical conditions like diabetes, arterial disease, and venous disease may also lead to leg ulcers. Some common signs and symptoms that often accompany leg ulcers include irritated or flaky skin, swelling, heaviness, discoloration, and leg pain on prolonged standing. You may use natural ingredients like Gotu kola, turmeric, aloe vera, coconut oil, tea tree oil, and yarrow in home remedies to heal leg ulcers in mild to moderate cases.
Recommended Reading: What To Eat To Help Stomach Ulcers
Can Venous Leg Ulcers Be Prevented
There are several ways to help prevent developing a venous leg ulcer in people at risk.
These include:
- elevating your leg when possible
- stopping smoking if you smoke
These measures are particularly important if you previously had a leg ulcer.
This is because you’re at increased risk of having another one in the same leg within months or years.
Looking After Yourself During Treatment
The following advice may help your ulcer heal more quickly.
- Try to keep active by walking regularly. Sitting and standing still without elevating your legs can make venous leg ulcers and swelling worse.
- Whenever you’re sitting or lying down, keep your affected leg elevated.
- Regularly exercise your legs by moving your feet up and down, and rotating them at the ankles. This can help encourage better circulation.
- If you’re overweight, try to reduce your weight with a healthy diet and regular exercise.
- Stop smoking and moderate your alcohol consumption. This can help the ulcer heal faster.
- Be careful not to injure your affected leg, and wear comfortable, well-fitting footwear.
You may also find it helpful to attend a local healthy leg club, such as those provided by the Lindsay Leg Club Foundation, for support and advice.
You May Like: Pepto Bismol And Ulcerative Colitis
Getting A Specialist Vascular Referral
If you have venous hypertension, intervention to your veins from a vascular specialist might help with healing and stop your wound or sore from coming back. Sometimes varicose veins can be treated by laser therapy. If you have peripheral arterial disease, you may require further investigations and the vascular team will be able to assess the need to improve the blood supply to your leg or whether your ulcer can be managed in other ways such as reduced/modified compression. Ask your nurse or doctor for a referral to your local vascular team to talk about how their input might help you.
Ways To Treat Venous Leg Ulcer And Its Symptoms
Venous leg ulcer is a sore that develops on the leg and heals very slowly, typically due to poor circulation through the limb. The sore may persist for only a few weeks, or it may last for years.
There are preventative steps you can take to keep from getting them. Venous leg ulcers can cause more serious issues if theyre untreated.
The condition occurs when the veins in your leg fail to send blood adequately back to your heart. The built-up backflow of blood increases the pressure at the end of your leg, which weakens this skin.
In turn, its more difficult for a scrape or cut to heal. These ulcers often occur on bony areas like the ankle.
Read Also: Diet Plan For Ulcerative Colitis Flare Up
Best Cream For Leg Ulcers
Many people suffer from leg ulcers. Leg ulcers are similar to a break in the skin of the leg, which allows air and bacteria to get to the underlying tissues. It can be formed by a minor injury that breaks the skin. It is also caused due to obesity, diabetes, and hypertension.
Contents
What Does This Mean
This means that treating faulty veins under the skin in the superficial vein system by Endovenous Laser Ablation or Sclerotherapy speeds up the rate of healing of the commonest type of leg ulcer and doing so also reduces the risk of the ulcer coming back.
Lets cover what a leg ulcer is, what types of leg ulcer there are, what causes a venous leg ulcer and lets discuss this latest research.
Read Also: Different Types Of Ulcerative Colitis
Dressings And Topical Agents
Dressings are usually applied to open ulcers. As well as offering protection, dressings may be chosen for other reasons, such as antimicrobial properties or absorption of exudate. As well as a wide range of types of dressings available, there are a number of topical products, used to reduce infection risk, aid exudate absorption or promote wound healing by other means, as well as topical painkilling agents. Having reliable evidence to guide choices is important, and not only for healthcare professionals. Patients responding to Cochrane Wounds online open consultation on research priorities, conducted between May and November 2016, asked in particular for evidence relating to specific dressings.
Getting Diagnosed With A Leg Ulcer
If you have a wound or sore that isnt healing, make an appointment at your GP practice as it could turn into or be the beginnings of a leg ulcer. You might be given an appointment to see the nurse rather than the doctor as nurses are often responsible for caring for patients with leg problems.
Alternatively, there might be a Leg Club or specialist leg clinic in your area. You can attend these without having to be referred by your GP.
Remember to remove any nail polish from your toenails before your appointment.
When you see the nurse or doctor, they should:
- Ask about your symptoms and how long you have had problems
- Examine your lower legs
- Do a simple test called a Doppler ultrasound. This test compares blood flow in your ankle with that in your arm to find out if there are blood flow problems in your lower leg. You may have to come back to have your Doppler test on another day or at another clinic.
You may also be offered some other tests to check for other health problems that can affect your legs such as diabetes and anaemia.
If your GP practice thinks you have problems with your veins or arteries, they may refer you for more tests at your local hospital or specialist clinic.
You may hear different words to describe your wound such as ulcer, leg ulcer, sore, laceration, chronic wound and maybe others. Ask your nurse to explain their choice of word and what this may mean for you.
Read Also: What Is The Best Probiotic To Take For Ulcerative Colitis
What Kind Of Research Was This
This was a phase 2 randomised controlled trial that compared different concentrations and dosing frequencies of a new treatment for venous leg ulcers, called HP802-247.
Venous leg ulcers are a complication of a condition where the valves in the veins of the leg do not work very well . The valves normally prevent blood flowing backwards and help the blood flow towards the heart. When they are damaged the blood begins to pool in the veins of the legs. This increases pressure of blood in the veins causing blood to ooze out and collect in the smaller veins underneath the skin. This damages the skin and potentially causes the skin to break down to form a venous ulcer. The study reports that between 1.65 and 1.74% of adults aged 65 years are affected by venous ulcers. These ulcers are most commonly found above the inner ankle bone. The standard treatment of venous ulcers is usually supportive. This involves care of the skin to prevent infection, application of a compression bandage and keeping the legs elevated as often as possible to try to help the blood flow back up the veins of the legs. However, the authors report that only between 30 and 75% of venous leg ulcers heal completely, with the remainder becoming chronic with the only treatment option being skin graft.
How Can I Prevent Leg Ulcers
Leg ulcers commonly open up again after healing. These steps can lower the risk of getting a leg ulcer or a wound recurrence:
- Elevate your legs above your heart when youre sitting or sleeping.
- Maintain a healthy weight and stay physically active.
- Manage health conditions that affect blood circulation, including diabetes, high blood pressure, high cholesterol and Raynauds syndrome.
- Quit smoking and using tobacco products. Talk with your healthcare provider about ways to stop smoking.
- Use gentle cleansers, and apply moisturizing lotion to prevent dry skin.
- Wear compression stockings or bandages for an hour each day to improve blood flow to the legs.
Don’t Miss: What Are The Symptoms Of An Ulcer In The Esophagus
Pentoxifylline For Treating Venous Leg Ulcers
Venous leg ulcers are a common, recurring and disabling condition. The mainstay of treatment is the use of firm compression bandages or stockings to support the veins of the leg. Some leg ulcers take many months or years to heal and treatment is aimed at preventing infection and speeding up healing. Pentoxifylline is a tablet taken to improve blood circulation. The review of trials suggests that pentoxifylline, 400 mg tablet taken three times a day, increases the chance of healing.
Pentoxifylline is an effective adjunct to compression bandaging for treating venous ulcers and may be effective in the absence of compression. The majority of adverse effects were gastrointestinal disturbances.
Healing of venous leg ulcers is improved by the use of compression bandaging but some venous ulcers remain unhealed, and some people are unsuitable for compression therapy. Pentoxifylline, a drug which helps blood flow, has been used to treat venous leg ulcers.
To assess the effects of pentoxifylline for treating venous leg ulcers, compared with a placebo or other therapies, in the presence or absence of compression therapy.
For this fifth update we searched the Cochrane Wounds Group Specialised Register The Cochrane Central Register of Controlled Trials Ovid MEDLINE Ovid MEDLINE Ovid EMBASE and EBSCO CINAHL .
Randomised trials comparing pentoxifylline with placebo or other therapy in the presence or absence of compression, in people with venous leg ulcers.
Split Thickness Skin Graft
This method is used for large ulcers under general, spinal, or extensive local anaesthesia. These grafts are usually successful, but the grafts may contract after harvesting and need a large donor site, which may be slow to heal and cause a lot of pain. In grafting large leg ulcers, graft failure may occur because of build-up of exudate underneath the graft this is best avoided by the use of a meshed graft.
Don’t Miss: How Can You Get Ulcerative Colitis
Trust South Valley Vasculars Expertise
The medical experts at South Valley Vascular in Visalia, Porterville, and Hanford, California, specialize in the diagnosis, treatment, and management of diseases and conditions of the blood vessels. Our vascular surgeons will determine a treatment plan that provides the best benefits for your specific needs.
Prevention Of Arterial Ulcers:
The lifestyle changes that the patient can adopt will contribute to improve peripheral circulation and help prevent arterial leg ulcers.
- Stop smoking: Smoking severely reduces the tissue perfusion and is one of aggravating factors for arterial leg ulcers.
- Healthy diet and weight loss: It Is important to reduce the intake of fat and to keep your cholesterol levels low. The patient should exercise as much as possible: this will help improve the blood circulation in your legs. If during exercising the patient feel some pain in his/her legs, it is normal. If the pain is more pronounced, or severe, it may be a sign that his/her arteries are seriously narrowed due to atherosclerosis. This needs to be addressed by a doctor.
- Take good care of patient’s feet: Advice shoes which fit correctly and are not too small Advice to keep feet warm avoiding feet and legs injuries Examinate feet and legs daily for any changes in color or developing sores Moisturizing the skin well to prevent skin damage which can develop ulcers.
You May Like: What Can You Do For A Stomach Ulcer
Treating Leg Ulcers At Home
Ulcers on the leg can be very painful. Treating them at home can help reduce healing time and discomfort. Itâs very important to keep the wound clean, bandaged, and dry. This helps to curb the risk of infection given the extended healing time. Following your physicianâs directives for changing the bandages can help aid in healing.
Patients should be careful to properly maintain bandaged leg ulcers. If the skin around the wound gets too wet, this can cause the ulcer to expand into these healthy tissues. Expansion of these painful wounds may require more involved treatment protocols.
Wearing compression socks daily can help support lower extremity blood circulation, speeding up the healing process. The compression can also help reduce pain and swelling. Keeping active and elevating the ulcer above the heart can also aid in healing because it promotes good circulation.
One out of twenty diabetes patients experience neuropathic ulcers each year. Neuropathic ulcers call for even more treatment interventions to encourage healing. Since they are most often caused by uncontrolled blood sugar, adhering to a diabetes maintenance plan is key. These ulcers are frequently located on the foot instead of the lower leg. As a result, avoiding pressure on the wound requires that the patient avoid walking and other activity unless absolutely necessary.
Natural Ways To Cure Ulcer In Leg Fast And Effective
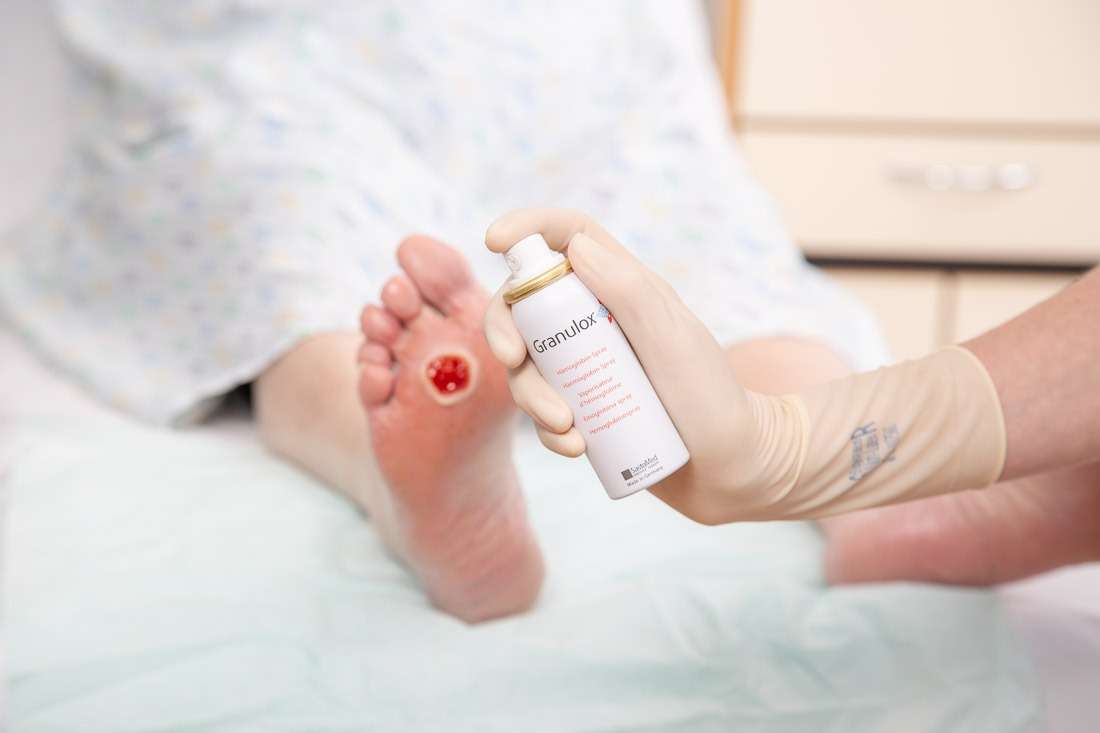
Leg ulcers are really annoying, right? They are sores that caused by the infection on the surface of the skin. This infection then makes the skin becomes itchy that triggers reddish lumps as we call ulcers. Severe ulcers can be more painful that cause fever, intolerable itching, and also severe aching.
Types of Ulcer
There are types of ulcer that you have to know, these are the three of them:
- Acne Cyst, is an ulcer that occurs on the surface of the skin due to excess oil. It generally appears on your face, especially someone who has oily face.The main cause of this type is the presence of bacteria in the oil glands where the bacteria flourish.
- Pilonidal Cyst, a type of ulcer that usually occurs on buttocks. This ulcer frequently secretes pus and blood when it breaks. The common cause of this ulcer is the infection that occurs in the hair follicles. When the ulcer in the area is exposed to pressure and friction, this will be bigger and worse that induces unbearable pain.
- Hidradenitis Suppurativa, is a type of ulcer that commonly appears on the under arms and groins. This type of ulcer will cause the most ache due to the friction with sweat glands.
Causes and Symptoms of Ulcers
Ulcers is mainly caused by the bacteria that live on the skin surface. Further,ulcers can also be caused by the following things:
- Unhealthy eating patterns, too often consume fatty and oily food
- Lack of personal and environmental hygiene
- Immune system is weak
How to Cure Leg Ulcers
Also Check: What Is Stomach Ulcer Pain Like