Gallbladder Problems And Bad Breath
Gall bladder dysfunction, gallstones or gall bladder removal can lead to unpleasant burping that can cause bad breath.
Your gall bladder produces digestive juices used for fat absorption.
When the gall bladder builds up mineral stones, the bile ducts can become blocked. This can cause infection and also pain, nausea or even vomiting, especially after eating a fatty meal.
Symptoms of gall bladder disease include:
- Agonizing pain in the upper right abdomen especially after a heavy meal. This may last minutes or hours.
- Sudden fever
- Nausea and/or vomiting after meals
- Light clay color stools
- Itchy skin rashes
- Pungent body odor and yellowish skin
- Yellow, discolored eyes, and dark circles beneath the eyes
Gall bladder problems can a serious health issue, so if you are experiencing these symptoms along with bad breath, ensure you see a doctor.
Tips For Managing Fatigue
- Keep a close eye on those blood testsChecking on iron levels, vitamin B12 and other chemical or nutrient deficiencies can help your treatment team to find the right mix of medication for you. Adding iron supplements or reducing the dosage of a medication can make a world of difference to energy levels for some people.
- Focus on keeping fitWhile being careful not to overstress yourself, try gradually increasing the amount of physical activity you do. Make use of a gym membership, walk rather than catching the bus for shorter trips, or commit to a team sport. Improving your overall fitness can ensure your energy stores are higher, potentially reducing the impact of those fatigue-ridden days.
- Assess your dietDo you have any foods that make you feel heavier, or sluggish? Complex carbohydrates such as cereals or porridge can provide you with energy over a longer time frame, while simple carbohydrates will give you a short burst of energy, often followed by a low. Consider if you are getting a good mix of fruits and vegetables, carbohydrates for energy, and rich protein.
- Manage your workloadWherever possible, ensure your workplace, family or education provider is aware of your condition and see what flexibility is available with responsibilities, work hours and prior planning. For example, taking the afternoon off following a doctors appointment may be a welcome break to rest, recover and prepare for the next week.
Stomach Ulcer Treatment Plan: 4 Natural Treatments
1. Boost Immunity Against H.pylori
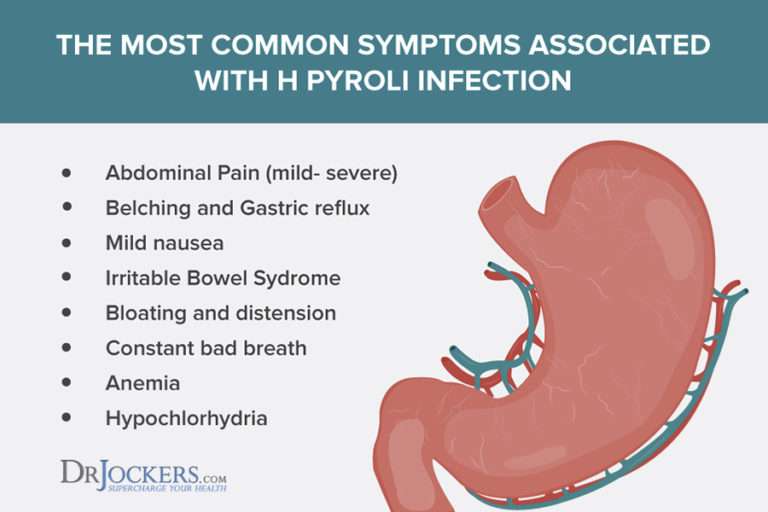
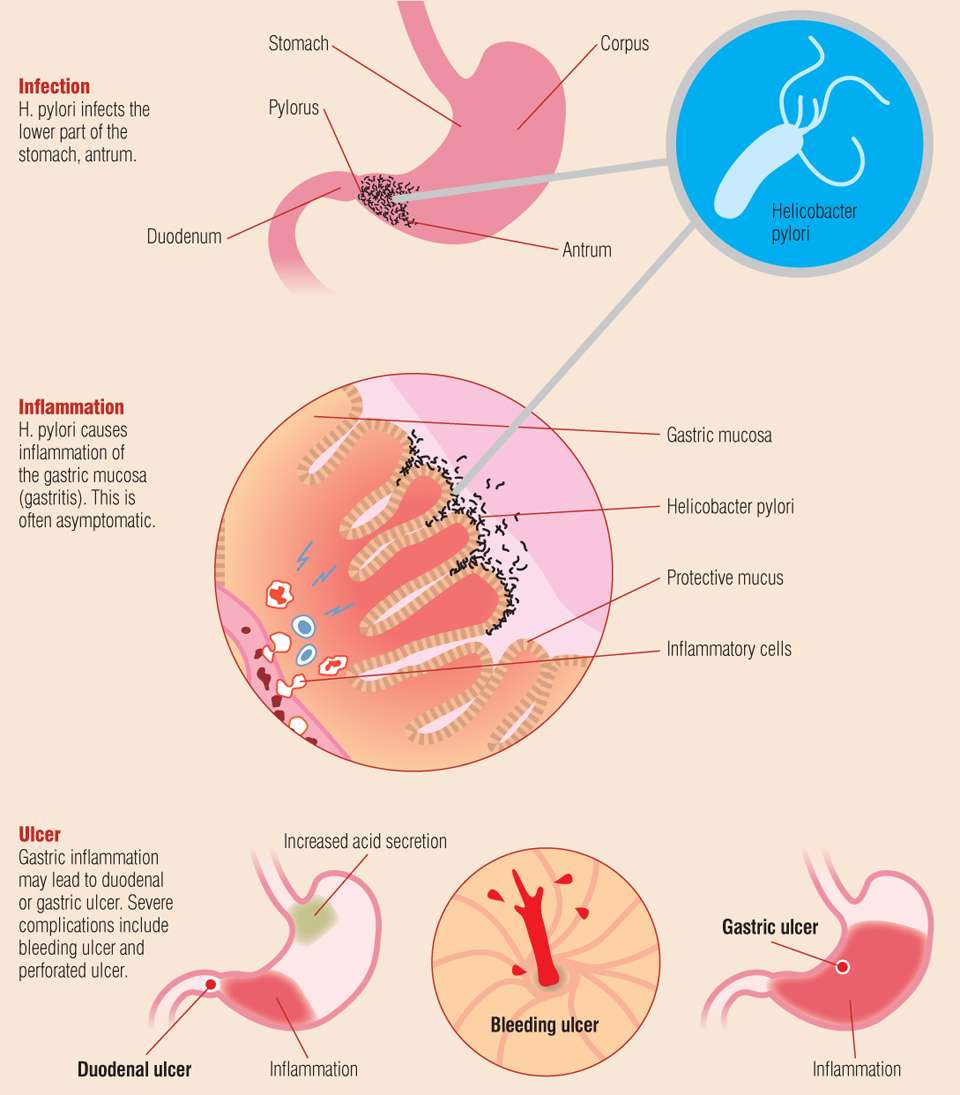
Many people host H. pylori in their bodies, but only a minority of people infected with H. pylori develop ulcers. A highly inflammatory lifestyle weakens the immune system and makes the digestive system more susceptible to an infection caused by H. pylori bacterium. H. pylori itself can then cause even more inflammation within the stomach and small intestine, creating a vicious cycle thats hard to break.
Research shows that today about 30 percent to 40 percent of people in the U.S. get an H. pylori infection, but usually the infection remains dormant, without any noticeable symptoms emerging for years or even ever. Other research suggests that H. pylori is present in more than 90 percent of duodenal ulcers and about 80 percent of stomach ulcers.
H. pylori contributes to ulcers by damaging the mucous coating that protects the lining of the stomach and duodenum from acids. Once damaged, stomach acid is able to get through to the sensitive lining, causing burning and irritation. H. pylori can be spread through unclean water, food or utensils, plus through bodily fluids but its only likely to cause an ulcer when someones immunity is low for other reasons.
You can also protect yourself from H. pylori infection by frequently washing your hands with soap and water and by eating foods that have been cooked completely.
2. Limit Use of NSAID Pain Relievers
3. Manage Stress
4. Eat A Stomach Ulcer Diet
Read Also: Stomach Ulcer And Chest Pain
What Is The Treatment Of Ulcerative Colitis
Ulcerative colitis is a lifelong disease with constant periods of flare-ups and remission . Presently, there is no permanent medical cure for it, but there are various medications that can provide symptomatic relief, reduce inflammation, and manage flare-ups.
Treatment involves medical and surgical management depending on the disease severity. Patients would also require dietary and lifestyle changes.
- Medical treatment includes the following:
- Medication to suppress and/or modulate the immune system
- Painkillers
Treating Back Pain In Ulcerative Colitis
Treating back pain in ulcerative colitis can be complicated. Research shows that treating the underlying UC can help lessen the severity of spondyloarthritis, but it will not resolve spondyloarthritis and back pain. Back pain must be addressed separately and in a way that does not make a persons UC symptoms worse.
People with ulcerative colitis may need to work with both a rheumatologist and a gastroenterologist to manage their gastrointestinal and spinal health properly. These doctors may prescribe or recommend the following treatments and therapies.
You May Like: Does Stelara Work For Ulcerative Colitis
Could Bad Breath From The Back Of The Mouth Signal An Illness
Bad breath may be caused by many things from the build-up of bacteria in the mouth to poor oral hygiene, which is called halitosis.
Bad breath may not always originate from the mouth, howeverthe source of bad breath may be coming from deeper inside the body.
While bad breath from the stomach may be mistaken for halitosis, it may be a sign of an underlying gastrointestinal condition that needs to be diagnosed and treated as soon as possible.
What Can I Expect If I Have A Diagnosis Of Ulcerative Colitis
Ulcerative colitis is a lifelong condition that can have mild to severe symptoms. For most people, the symptoms come and go. Some people have just one episode and recover. A few others develop a nonstop form that rapidly advances. In up to 30% of people, the disease spreads from the rectum to the colon. When both the rectum and colon are affected, ulcerative symptoms can be worse and happen more often.
You may be able to manage the disease with medications. But surgery to remove your colon and rectum is the only cure. About 30% of people with ulcerative colitis need surgery.
Don’t Miss: Histiocytic Ulcerative Colitis Boxer Treatment
Warning Disclaimer Use For Publication
WARNING: Please DO NOT STOP MEDICATIONS without first consulting a physician since doing so could be hazardous to your health.
DISCLAIMER: All material available on eHealthMe.com is for informational purposes only, and is not a substitute for medical advice, diagnosis, or treatment provided by a qualified healthcare provider. All information is observation-only. Our phase IV clinical studies alone cannot establish cause-effect relationship. Different individuals may respond to medication in different ways. Every effort has been made to ensure that all information is accurate, up-to-date, and complete, but no guarantee is made to that effect. The use of the eHealthMe site and its content is at your own risk.
If you use this eHealthMe study on publication, please acknowledge it with a citation: study title, URL, accessed date.
Nutrition Tips For Inflammatory Bowel Disease
Inflammatory Bowel Disease is a term used for two specific and separate diseases: Crohn’s disease and ulcerative colitis. Nutritional recommendations are different for each disease and for each individual patient. It is important to discuss the treatments that are right for you with a registered dietitian and with your doctor.
Recommended Reading: Can Stress Cause Ulcerative Colitis Flare Up
Sleep Apnea Can Cause Morning Breath
Morning breath may seem normal after a night of sleeping. Saliva production decreases during sleep, which gives odor-producing bacteria an opportunity to multiply and grow.
But the slowed production of saliva during sleep can sometimes be caused by leaving your mouth open for long periods of time. People with sleep disorders such as sleep apnea and snoring may have trouble breathing through the nose and are more likely to breathe through their mouths, which is a cause of bad breath.
When Should I See A Doctor If I Think I Have A Peptic Ulcer
- If you have burning pain in your upper stomach that is relieved by eating or taking antacids, call a health-care professional for an appointment. Donât assume you have an ulcer. Certain other conditions can cause similar symptoms.
- If you vomit blood or have other signs of gastrointestinal bleeding, go to an emergency department right away. Peptic ulcers can cause massive bleeding, which requires blood transfusion or surgery.
- Severe abdominal pain suggests perforation or tearing of an ulcer. This is an emergency that may require surgery to fix a hole in your stomach.
- Vomiting and abdominal pain also can be a sign of an obstruction, another complication of peptic ulcers. This also may require emergency surgery.
Recommended Reading: What Is Peptic Ulcer Disease
Epsom Salt For Mouth Ulcer:
Epsom salt is a recommended method to fight chronic halitosis and sores naturally. The affluence of healing properties in this item reduces the swelling of mouth ulcer superbly and the antibacterial compounds act as a germicide on the canker sores to resolve them from your skin surface. Letâs see how to use them to lessen the sensation of mouth sores swiftly-
Method
- Add Ãý tbsp of Epsom salt into 1 glass of hot water and gargle your mouth with this solution.
- After that, apply some cool healing methods on your sores like a few drops of raw honey or essential oil and let that method work there for several hours.
- This way, after a few applications, you will be free from any kinds of mouth sores soon.
Also Check: What To Eat When You Have Gastric Ulcer
Ways To Keep Your Heart Healthy If You Have Uc
Follow these steps to lower your risk of heart disease and ease your UC flares.
Also Check: Treating Leg Ulcers With Sugar
Drugs And Radiation Therapy
The most common drugs causing mouth sores include certain cancer chemotherapy drugs. Drugs containing gold, which were once used to treat rheumatoid arthritis and some other autoimmune disorders, can also cause mouth sores, but these drugs are rarely used because safer and more effective drugs are now available. Radiation therapy is also a common cause of mouth sores. Rarely, people may develop mouth sores after taking antibiotics.
What Are The Signs And Symptoms Of Ulcerative Colitis
First, lets review: What isulcerative colitis, anyway? This condition occurs when your large intestinethat includes your colon and your rectumis chronically inflamed. Somehow, your immune systems signals got scrambled, so the body ends up attacking healthy cells as if theyre foreign invaders. The resulting inflammation is the root cause of most of its symptoms, too.
While most people associate the digestive system and intestinal issues with UC, not all UC symptoms stem from the large intestine. Because the inflammation of UC is systemic, it can affect your entire body, leading to problems like joint pain, extreme fatigue, and morenot to mention the stress and anxiety that can come with dealing with a serious chronic disease.
Heres a quick list of the main symptoms:
-
Blood or pus in your stool
-
Frequent diarrhea
-
Tenesmus, or when you have a sudden and constant feeling that you need to have a bowel movement
-
Abdominal pain or discomfort
Read Also: Hind Gut Ulcers In Horses Treatment
> > > Scientists: Eat This White Mineral To Regrow Your Teeth And Gums Overnight
In addition to a poor diet, poor immune system, and a poor diet can all cause gum disease. These factors can lead to a weakened immune system and can make you vulnerable to a variety of conditions, including cancer. Therefore, a regular dentist is a must for maintaining a healthy immune system and avoiding the development of periodontal disease. This will help you maintain your teeth and avoid dental problems. If you suffer from periodontitis, see a dentist right away.
Do Ulcers In Horses Cause Colic
Necroscopic analysis of ulcerated horses, combined with other existing data, may provide a lead into the underlying etiology of many idiopathic colics. Many studies exist that show gastric ulcers are present in horses that colic, and articles continue to be published suggesting that gastric ulcers are causative.
Donât Miss: Medication For Ulcerative Colitis Flare Up
Don’t Miss: How To Treat An Eye Ulcer
Irritable Bowel Syndrome And Bad Breath
While SIBO more commonly causes bad breath, irritable bowel syndrome can cause bad breath too.
Irritable bowel syndrome is a common disorder of the digestive system. Most commonly, patients suffer recurrent abdominal pain and altered bowel habits such as constipation, diarrhea or both.
Other IBS symptoms include:
- Fever
- Weight loss
If you suffer from bad breath that can be described as sulfur burping, and also have diarrhea or vomiting, you should see a doctor immediately. These may be the first signs of irritable bowel syndrome.
How Is Ulcerative Colitis Diagnosed
To diagnose ulcerative colitis in children, teenagers and adults, your healthcare provider has to rule out other illnesses. After a physical exam, your provider may order:
- Blood tests: Your blood can show signs of infection or anemia. Anemia is a low level of iron in your blood. It can mean you have bleeding in the colon or rectum.
- Stool samples: Signs of infection, parasites , and inflammation can show up in your poop.
- Imaging tests: Your healthcare provider may need a picture of your colon and rectum. You may have tests including a magnetic resonance imaging scan or computed tomography scan.
- Endoscopic tests: An endoscope is a thin, flexible tube with a tiny camera. Specialized doctors can slide the endoscope in through the anus to check the health of the rectum and colon. Common endoscopic tests include colonoscopy and sigmoidoscopy.
Recommended Reading: Ozanimod Ulcerative Colitis Phase 3
Could My Symptoms Be Ibs
Irritable Bowel Syndrome is a different condition from IBD, although some of the symptoms are similar. Like Crohn’s and Colitis, IBS can cause abdominal pain, bloating and bouts of diarrhoea or constipation. However, it does not cause the type of inflammation typical of Colitis, and there is no blood loss with IBS.
Some people with Colitis may develop IBS-like symptoms, for example experiencing diarrhoea even when their Colitis is inactive. These symptoms may need slightly different treatment from their usual IBD symptoms. IBS is more common in people with IBD than in the general population.
If you develop diarrhoea with bleeding and abdominal pain, your doctor may suspect you have Colitis, particularly if you are a young adult or have a family history of Crohn’s or Colitis. You will need tests and physical examinations to confirm a diagnosis. See Tests and Investigations for IBD.
You may need to have tests repeated from time to time to check on your condition and how your treatment is working.
Some drug treatments may also require a series of blood tests and, occasionally, x-rays or scans to check for any potential side effects. Your specialist will avoid giving you any unnecessary tests or investigations.
You may need more regular colonoscopies when you have had Ulcerative Colitis for a long time to check for any signs of cancer.
What Causes Body Odor Associated With Ibd
Recent research suggests that excess sulfur is often present in the digestive systems of people diagnosed with inflammatory bowel disease. This excess sulfur could be to blame for unpleasant smells such as those described above.
Sulfur is an element that occurs naturally in many of the foods and drinks we consume. Everyone has bacteria in their digestive tract that turn the sulfur present in food into hydrogen sulfide. This process is called fermentation. The body excretes this toxic product when it passes gas. However, too much hydrogen sulfide in the body can also cause frequent bathroom trips, urgent diarrhea, and cramping or abdominal pain.
In most people, there are intestinal cells that line the colon that take care of excreting this chemical. However, people with IBD seem to produce more hydrogen sulfide than normal, leaving these intestinal cells overwhelmed. Whats more, chronic inflammation in the bowel seems to inhibit their functioning.
IBD is also associated with the malabsorption of some foods. This means that as food progresses through the gastrointestinal tract, more of it gets passed undigested from the small intestine into the colon . Bacteria in the colon then have to digest it. This process produces more gas than digestion would in a person with a normally functioning bowel, which can lead to bloating and additional flatulence.
Read Also: What Foods Should I Eat With Ulcerative Colitis
Can The Immune Response To Covid
byKate Kneisel, Contributing Writer, MedPage Today March 1, 2022
A 50-year-old male patient presented to an outpatient clinic in the spring of 2020 with fever and dyspnea he told clinicians that the symptoms had persisted for the past 3 days.
Physical examination findings included a fever of 37.8°C , respiratory rate of 24 breaths/min, and heart rate of 105 beats/min. There was no organomegaly, and the patient was a non-smoker.
Initial laboratory test findings included:
- White blood cell count: 6.4 × 109/L
- C-reactive protein : 4.6 mg/L
- Ferritin: 162 ng/mL
- D-dimer: 842 ng/mL
Findings of a polymerase chain reaction test for SARS-CoV-2 were negative. However, the patients wife and two children had positive PCR test results and the patients CT chest scan revealed diffuse ground-glass opacities consistent with viral pneumonia. Clinicians diagnosed him with COVID-19, and he was started on a now-debunked 7-day regimen of hydroxychloroquine and azithromycin. Once he was clinically stable, he was released with instructions to return for a follow-up assessment.
On follow-up assessment 1 week later, the patient reported no improvement in symptoms. His stool calprotectin level was 1800 g/g . Endoscopy revealed a diffuse, micro-ulcerated, granulated appearance that clinicians noted continued uninterrupted from the dentate line to the sigmoid colon, as well as distortion of the submucosal vascularization.
Discussion
Also Check: What Does A Mouth Ulcer Look Like