What Causes Diabetic Wounds
- Elevated blood glucose: When blood sugars reach levels higher than 200 the immune system lowers. This can contribute to the formation of wounds. A small cut that may normally heal without problems may actually become a larger, deeper ulcer due to the dysfunction of the immune system.
- Poor circulation: A common problem in patients with diabetes, is poor circulation. Elevated sugars in the blood can damage the small blood vessels, especially the ones to the foot and toes. When your foot or toes are lacking enough blood, they do not receive proper nutrients. The skin can begin to break down and an ulcer can form. This is similar to a plant that is not receiving proper water- the ends become brown, crisp and dry out.
- Neuropathy: Another common condition that can lead to diabetic ulcers, is neuropathy. Neuropathy is a loss of sensation or feeling, typically in the toes and the feet. You may step on something sharp and not feel it. This can result in a small cut that later becomes a deep wound. If you put a lot of pressure in the same place on your foot, daily, this can also result in a special type of ulcer called a pressure ulcer.
HOW CAN I PREVENT GETTING A DIABETIC WOUND?
HOW CAN I HEAL MY WOUND FASTER?
Key Principles Of Compression Bandaging:
Compression bandaging should not be used if there is arterial disease and leg ulcers. More damage can occur in the ulcer or within the blood circulation system.
- There should be graduated compression greatest at the ankle while decreasing as it is applied up the leg. Compression is measured in millimeters of mercury . Although everyones needs are different, the general rule is 32 to 42 mm Hg at the ankle and ending with 12 to 17 mmHg below the knee.
- Overly tight bandaging should be avoided. This may cause too much constriction resulting in persistent pain.
- Compression to the ulcerated area alone is ineffective.
- The bandage must be applied from the toe to the knee, molding around the ankle, up to the level just below the knee.
- The bandage must not be applied directly to the ulcer or to skin which is damaged or inflamed. A dressing or a paste bandage must act as a buffer.
- After healing, further compression may be necessary to prevent recurrence. At this point a compression stocking may be appropriate.
- Co-operation on the part of the patient is absolutely vital when using a compression bandage. For example, the elevation of the legs just above the heart helps the compression treatment.
Treatment What Treatment Will I Be Offered For My Leg Ulcer
If your wound isnt healing because of venous hypertension and there are no problems with the blood supply to your legs, then you should be offered compression therapy.
Compression therapy improves blood supply by applying pressure to the leg. This can be done by bandaging the lower leg or by wearing supportive socks, stockings or tights. Compression therapy is very effective at reducing swelling, improving blood flow in the veins and healing or preventing sores or ulcers.
There are lots of different types of compression therapy so ask your nurse to find something that is right for you.
Compression can be a little uncomfortable when you first start treatment but should not cause you any pain. Any discomfort should reduce as the swelling goes down. If you do experience discomfort, talk to your nurse or doctor about it and they will advise you on ways of alleviating this.
In addition to the compression, your nurse should also advise you on wound care and dressings to keep your wound healthy.
Also Check: Foods To Avoid With Peptic Ulcer
What Is The Treatment For A Venous Leg Ulcer
A venous leg ulcer usually wont get better without treatment from a healthcare professional. The aim of treatment is to make sure the wound heals while providing relief from symptoms such as pain in and swelling of your affected leg.
Your GP may recommend specialist wound care and compression therapy to help with healing. Treatment will usually be done by a district nurse who is specifically trained to manage leg ulcers.
Compression therapy applies pressure to your affected leg, which reduces the amount of blood pooling in the veins and helps to redirect the blood flow to your heart. It can help to reduce swelling and encourages delivery of oxygen and nutrients, critical for healing, to the wound.
Your GP may consider referral to a vascular surgeon to discuss a minimally invasive procedure for varicose veins. This will reduce the risk of recurrent ulcers.
Read Also: Can Ulcerative Proctitis Be Cured
Deep Vein Thrombosis Prophylaxis
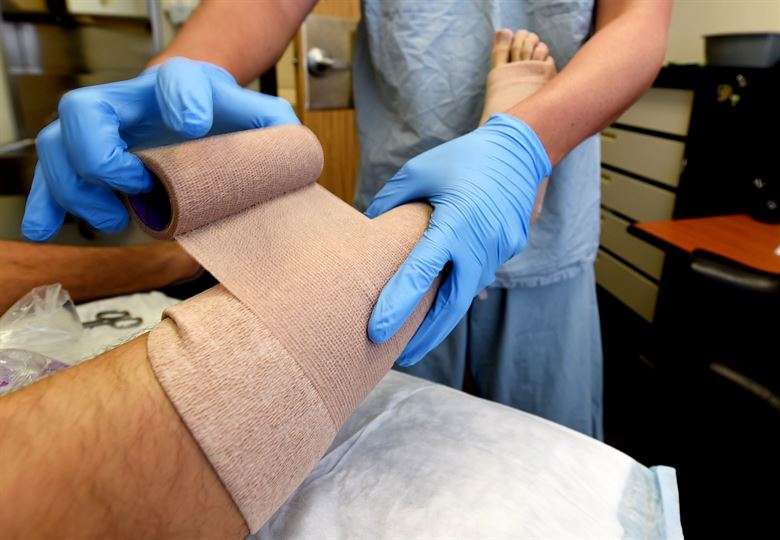
The role of mechanical devices graduated compression stockings and intermittent pneumatic compression is dependent on the risk of venous thromboembolism in the medical or surgical patient. They may be used in combination with drug therapy or alone, especially if drugs are contraindicated because of an unacceptable bleeding risk. These mechanical devices are contraindicated in patients with severe peripheral vascular disease, severe leg deformity and severe peripheral neuropathy.
Evidence supports the use of graduated compression stockings as thromboprophylaxis for abdominal, cardiac, thoracic, vascular, major general or gynaecological surgery, neurosurgery and total hip replacement. Similarly, there is evidence for the use of intermittent pneumatic compression for total hip replacement, hip fracture surgery, total knee replacement, vascular, cardiothoracic surgery, neurosurgery, and for major gynaecological surgery. Graduated compression stockings should be measured for the individual and worn for as long as possible until the patient is fully mobile.20
Recommended Reading: Ulcer On Eye From Contact Lens
Recommended Reading: Does Turmeric Help Ulcerative Colitis
Basic Principles Of Compression Therapy
Depending on the position of the body, compression therapy improves venous return . The consistent pressure applied to the veins results in a decrease in vessel diameter, in reduced transmural pressure, and thus in a flow rate that is almost twice as high. In a lying position, pressure values as low as 15 mmHg are sufficient to constrict superficial and deep veins, which subsequently leads to an acceleration in blood flow. To achieve this while standing up, significantly higher pressure values are required . Compression with a stiff, rigid material provides stable support for the leg muscles, thereby increasing the effects of the muscle pump, which in turn results in improved venous return . The latter leads to edema reduction as well as pain relief. The question as to whether leg ulcer patients might potentially benefit from additional compression of the thighs cannot be unequivocally answered based on current literature. Although strong nonelastic thigh bandages may reduce venous return , there are as yet no reports on accelerated ulcer healing. Moreover, additional thigh compression is likely to result in poorer adherence, which has similarly been described for the use of thromboembolic devices and compression stockings for the prevention of PTS . Thus, although thigh compression may indeed be applied in individual cases, it is currently not recommended as standard treatment for venous leg ulcers.
The Range Of Bandages
There is now a considerable range of compression and related bandages available for the treatment of leg ulcers. They provide a range of pressures that vary to suit a range of circumstances. There have been a number of reviews of compression bandaging systems .
Eagle identifies the following bandage systems: multi-layer systems, long-stretch single bandages, short-stretch bandages providing minimal stretch, cotton crepe and tubular bandages.
With all compression bandage systems, padding using orthopaedic wool is used to redistribute pressure from bony prominences and to help provide even distribution of pressure under the compression bandages where the shape of the leg may militate against even graduated pressure.
Stacey et al define compression bandages as follows:
– Sustained compression – this includes any bandage system that can maintain sub-bandage pressures for a least one week
– Multi-layered compression – this group includes bandages with more than 50% stretch
– Multi-layered compression – this group includes bandages with less than 50% stretch
– Reduced compression – this group contains systems that deliver 15-25 mmHg sub-bandage pressure for patients with narrow ankles or an ankle brachial pressure index between 0.8 and 0.5
– Compression stockings – primarily used for prevention of recurrence or in the care of varicose veins
– Intermittent pneumatic compression – systems capable of delivering high compression for short periods of time.
Read Also: Can Ulcerative Proctitis Be Cured
How To Heal Venous Leg Ulcers
This article was co-authored by . Marsha Durkin is a Registered Nurse and Laboratory Information Specialist for Mercy Hospital and Medical Center in Illinois. She received her Associates Degree in Nursing from Olney Central College in 1987.wikiHow marks an article as reader-approved once it receives enough positive feedback. In this case, 90% of readers who voted found the article helpful, earning it our reader-approved status. This article has been viewed 23,737 times.
A venous skin ulcer is a shallow wound that occurs when veins dont return the blood back to the heart the way theyre supposed to. These ulcers usually form on the sides of the lower leg, above the ankle, and below the calf. They can heal over time with proper care, but without it, they can return and/or cause serious complications.XTrustworthy SourceNational Health Service Public healthcare system of the UKGo to source It’s very important to see a doctor or wound care nurse when you have an ulcer, then to keep them dressed and bandaged, take the right medications, and alter some of your habits at home.
Limitations Of The Study
To this moment we were unable to present long term results longer observation than two months . Although study outcomes were consistent in each treatment group, the absence of blinding and use of placebo are a limitation of this study that may affect the generalization of the findings. In future we would like to provide quasi compression therapy in control groups and present complete results. We did not use intention-to-treat analysis either.
You May Like: Early Stage Venous Leg Ulcer
Looking After Yourself During Treatment
The following advice may help your ulcer heal more quickly.
- Try to keep active by walking regularly. Sitting and standing still without elevating your legs can make venous leg ulcers and swelling worse.
- Whenever you’re sitting or lying down, keep your affected leg elevated.
- Regularly exercise your legs by moving your feet up and down, and rotating them at the ankles. This can help encourage better circulation.
- If you’re overweight, try to reduce your weight with a healthy diet and regular exercise.
- Stop smoking and moderate your alcohol consumption. This can help the ulcer heal faster.
- Be careful not to injure your affected leg, and wear comfortable, well-fitting footwear.
You may also find it helpful to attend a local healthy leg club, such as those provided by the Lindsay Leg Club Foundation, for support and advice.
Diagnosis And Treatment Of Venous Ulcers
LAUREN COLLINS, MD, and SAMINA SERAJ, MD, Thomas Jefferson University Hospital, Philadelphia, Pennslyvania
Am Fam Physician. 2010 Apr 15 81:989-996.
Patient information: See related handout on venous ulcers, written by the authors of this article.
Venous ulcers, or stasis ulcers, account for 80 percent of lower extremity ulcerations.1 Less common etiologies for lower extremity ulcerations include arterial insufficiency prolonged pressure diabetic neuropathy and systemic illness such as rheumatoid arthritis, vasculitis, osteomyelitis, and skin malignancy.2 The overall prevalence of venous ulcers in the United States is approximately 1 percent.1 Venous ulcers are more common in women and older persons.36 The primary risk factors are older age, obesity, previous leg injuries, deep venous thrombosis, and phlebitis.7
Venous ulcers are often recurrent, and open ulcers can persist from weeks to many years.810 Severe complications include cellulitis, osteomyelitis, and malignant change.3 Although the overall prevalence is relatively low, the refractory nature of these ulcers increase the risk of morbidity and mortality, and have a significant impact on patient quality of life.11,12 The financial burden of venous ulcers is estimated to be $2 billion per year in the United States.13,14
You May Like: Psc Liver Disease Ulcerative Colitis
Recommended Reading: Air Mattress For Pressure Ulcer Prevention
Leg Ulcer Compression Therapy For Leg Ulcers And Foot Ulcers During The Coronavirus
If there are problems with a leg ulcer healing, this is usually because there are problems with the blood return from the leg to the heart.
If there is a good blood supply to the legs, then you should offer compression therapy to improve the blood return.
Compression therapy improves blood return by applying pressure to the lower leg and is very effective at helping leg wounds heal faster, reducing swelling and preventing ulcers coming back. This can be done by bandaging, compression hosiery or by wrap systems. There are lots of different types of compression therapy so there will be something that suits your patient.
Compression can be a little uncomfortable when the treatment is first started but should not cause your patient any pain. Any discomfort should reduce as the swelling goes down. If your patient does experience discomfort, encourage them to talk to you so you can suggest ways to reduce the discomfort.
Compression Stockings For Treating Venous Leg Ulcers
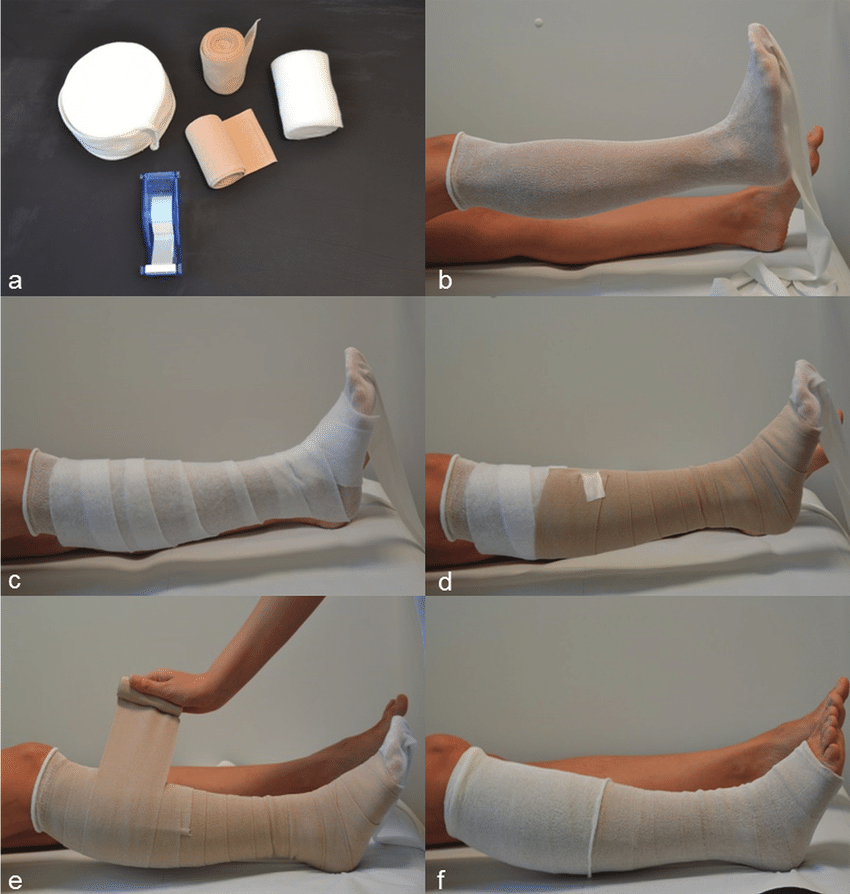
J. P. Benigni
1Cardiology Unit, HIA Bégin, 69 Avenue de Paris, 94160 Saint Mandé, France
2URDIA, Université des Saints Pères, 15 Rue des Saints Pères, 75006 Paris, France
Abstract
1. Background
Compression increases ulcer healing rates compared with no compression .
Thus to improve the healing process it is recommended to treat venous or mixed venous with high pressure. A pressure between 30 and 40mmHg should be obtained at the ankle .
Multicomponent systems are more effective than single-component systems. Multicomponent systems containing an elastic bandage appear more effective than those composed mainly of inelastic constituents. Two-layer stockings appear more effective than the short-stretch bandage . In fact, there are no clear differences in the effectiveness of different types of high compression.
Putting on the bandages requires a great experience and the respect of the bandage stretching rules. A pressure level from 30 to 40mmHg may not be easy to achieve. The main criticism that can be made against the use of a multilayer bandage or short stretch is linked to bandage slippage. Slippage is a cause of adverse effects: pain, aggravation of ulcer ulceration, and necrosis .
The use of compression stockings seems to be the best option because of the pressure control it allows for and it is not operator dependant. However 3040mmHg compression stockings are often hard to put on, especially for the elderly. In this case a donning and doffing aid could be useful.
Read Also: Natural Ways To Heal Ulcerative Colitis
Four Categories Of Compression Hosiery
1) Support Wear:Contains a very mild compression of 8-5 mmHg
- Tired aching legs
- Mild swelling
- Prevention for people who are required to stand or sit in one position for long periods of time.
2) Medical Leg Wear:Available in compressions from 15-50 mmHg
- Management and prevention of venous leg ulcer minor to severe varicosities
- Minor to severe edema
- Post-surgery and sclerotherapy
- Pregnancy related edema and varicosities
- Lymphatic edema
- Management of Chronic Venous Insufficiency
3) Custom Wear:Available in compression of 15-90 mmHg
- Patients with abnormal limb shapes
- Patients who need an unlimited size range
- Patients who need specific garment options to improve compliance and fit
- Patients who need long-term management of lyphedema or vascular edema
4) Ulcer Care:Contains a compression of 40 mmHg
- Designed specifically for use with venous ulcerations
- Two-part system providing a total pressure of 40+ mmHg
- Liner holds dressing in place, is easy to put one, is worn 24 hours a day, facilitates donning of outer stocking
- Is used until the ulceration heals
- Outer stocking has zipper to facilitate donning and is worn during ambulation over the white liner
- Open toe stocking
A follow-up appointment is usually arranged after the hosiery has been fitted to ensure that the stocking is being used properly. Regular review may be required to check for any problems.Ideally, new hosiery should be re-ordered every four to six months.
Why It Is Important To Do This Review
Venous leg ulcers have a large impact on peoples lives and incur high costs to health services and compression therapy is currently the first line treatment. Since the publication of the original Cochrane Review of compression bandages and stockings for venous leg ulcers , the number of relevant randomised controlled trials has more than doubled the range of compression modalities has increased and the classification of compression modalities has been refined. In order to offer uptodate evidence for decision makers, we have decided to update the previous version of this review, , and to split it into separate reviews of different compression modalities. We will then bring the results together into an overview, which will incorporate a network metaanalysis , in order to rank the different treatments on their individual probabilities of being the most effective compression modalities for healing venous leg ulcers. This particular review provides evidence about the comparison of compression bandages or stockings versus no compression.
Read Also: What Causes Ulcers On The Feet
Referral To A Specialist
In some cases, your GP or nurse may decide to refer you to a specialist in conditions affecting the blood vessels .
For example, you may be referred to a vascular specialist if your GP or nurse is unsure about your diagnosis, or if they suspect your ulcer may be caused by artery diseases, diabetes or rheumatoid arthritis.
After taking your medical history and examining you, the vascular specialist may need to arrange further investigations to plan your treatment.
Compression Therapy For Venous Leg Ulcers: Risk Factors For Adverse Events And Complications Contraindications A Review Of Present Guidelines
Radboud UMC, Nijmegen & Andriessen Consultants, Malden, The Netherlands
International Compression Club , Berndorf, Austria
Department of Angiology, Clinica MD Barbantini, Lucca, Italy
International Compression Club , Berndorf, Austria
Medical University Vienna, Vienna, Austria
International Compression Club , Berndorf, Austria
Medical & Regulatory Affairs, Lohmann & Rauscher GmbH & Co KG, Rengsdorf, Germany
Patient Outcome Group , European Wound Management Association , Frederiksberg, Denmark
International Compression Club , Berndorf, Austria
Radboud UMC, Nijmegen & Andriessen Consultants, Malden, The Netherlands
International Compression Club , Berndorf, Austria
Department of Angiology, Clinica MD Barbantini, Lucca, Italy
International Compression Club , Berndorf, Austria
Medical University Vienna, Vienna, Austria
International Compression Club , Berndorf, Austria
Medical & Regulatory Affairs, Lohmann & Rauscher GmbH & Co KG, Rengsdorf, Germany
Patient Outcome Group , European Wound Management Association , Frederiksberg, Denmark
International Compression Club , Berndorf, Austria
You May Like: What Is A Gastric Ulcer And What Is Its Cause