Treatment By Disease Severity And Location
Mild-moderate distal colitis
- Oral aminosalicylates, topical mesalamine, or topical steroids
- Combination of oral and topical aminosalicylates is better than either alone
For refractory cases, oral steroids or IV infliximab can be used
Mild-moderate extensive colitis
- Oral sulfasalazine 4-6 g/day or alternative aminosalicylate 4.8 g/day
- Oral steroids for patients refractory to above therapy + topical therapy
- 6-MP or azathioprine for patients refractory to oral steroids, but not so severe as to require IV therapy
- Infliximab in patients who are steroid refractory/dependant on adequate doses of 6-MP/thiopurine or who are intolerant to these medications
Severe colitis
- Infliximab if urgent hospitalization is not needed
- If patient is toxic, should be admitted to the hospital for IV steroids
- Failure to improve in 3-5 days is indication for colectomy or IV cyclosporine
Indications for Surgery
- Absolute: Hemorrhage, perforation, documented or strongly suspected cancer
Also, surgery is recommended for severe colitis refractory to medical therapy
Ways To Reduce Complications
Early intervention and frequent surveillance of ailments is key to reducing complications and improving outcomes. It’s important to maintain proper nutrition and avoid emotional stress, though neither stress nor sensitivity to certain foods causes the disease. Avoiding steroids can also be helpful if you and your doctor have an alternative way of treating UC flares.
While the cure for UC has yet to be found, when the disease is treated properly, some complications may disappear altogether. Work with your doctor and other members of your healthcare team to get optimal control of the disease as soon as possible.
Additional reporting by Jordan M. Davidson.
Why Does Kidney Disease Cause Weight Gain
Kidney disease doesnt just affect the kidneys, it affects the whole body. In the early stages, it can cause weight loss, while in the later stages it can cause weight gain. These variations are the result of different aspects of the disease. Heres some information to help you understand the issue of kidney disease and weight gain, courtesy of Dr. Allen Lauer, of Associates in Nephrology.
You May Like: What To Do For A Kidney Infection
Don’t Miss: Icd 10 Stage 4 Sacral Ulcer
Data Collection And Study Endpoints
We collected data on patient demographics and on the medications used for IBD treatment, including 5-aminosalicylic acid , corticosteroids, immunomodulators , and anti-tumor necrosis factor -α agents . Medication use was defined as all relevant medications prescribed within 1 year of the diagnosis of IBD. We also collected information on comorbidities identified with ICD-10 codes, including hypertension , DM , dyslipidemia , congestive heart failure , ischemic heart disease , hyperuricemia, and gout . The definitions of these comorbidities were validated previously. The metabolically healthy condition was defined as the absence of DM, hypertension, and dyslipidemia. An underlying disease was defined as the presence of at least one of the following: DM, hypertension, dyslipidemia, congestive heart failure, ischemic heart disease, hyperuricemia, and gout.
What Is Ulcerative Colitis
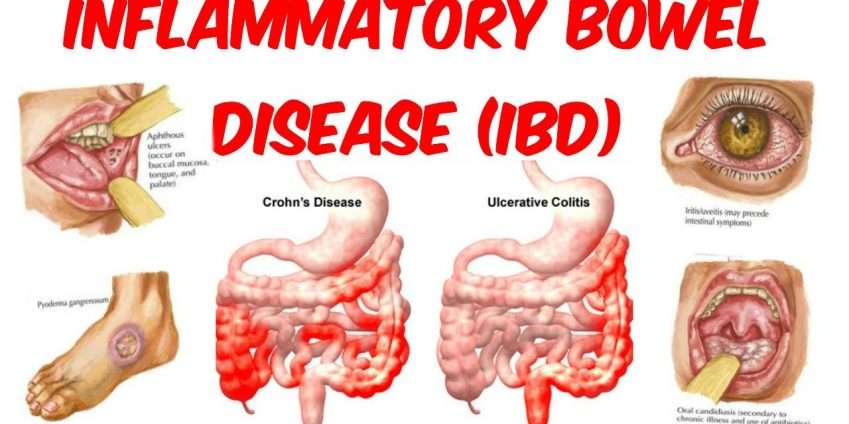
Ulcerative colitis is a chronic inflammation of the large intestine . The colon is the part of the digestive system where water is removed from undigested material, and the remaining waste material is stored. The rectum is the end of the colon adjacent to the anus. In patients with ulcerative colitis, ulcers, and inflammation of the inner lining of the colon lead to symptoms of abdominal pain, diarrhea, and rectal bleeding.
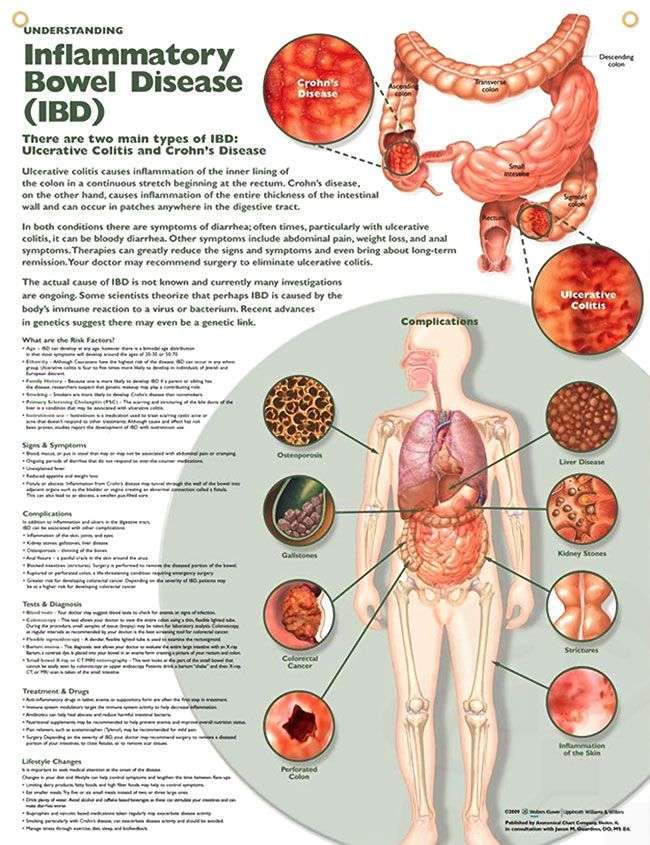
Ulcerative colitis is closely related to another condition of inflammation of the intestines called Crohn’s disease. Together, they are frequently referred to as inflammatory bowel disease . Ulcerative colitis and Crohn’s diseases are chronic conditions. Crohn’s disease can affect any portion of the gastrointestinal tract, including all layers of the bowel wall. It may not be limited to the GI tract . UC only affects the lining of the colon . Men and women are affected equally. The most commonly begin during adolescence and early adulthood, but they also can begin during childhood and later in life.
UC found worldwide but is most common in the United States, England, and northern Europe. It is especially common in people of Jewish descent. Ulcerative colitis is rarely seen in Eastern Europe, Asia, and South America, and is rare in the black population. For unknown reasons, an increased frequency of this condition has been observed recently in developing nations.
Don’t Miss: Ulcer On Eye From Contact Lens
Extraintestinal Manifestations And Complications
Aphthous ulcersPyoderma gangrenosum
UC is characterized by immune dysregulation and systemic inflammation, which may result in symptoms and complications outside the colon. Commonly affected organs include: eyes, joints, skin, and liver. The frequency of such extraintestinal manifestations has been reported as between 6 and 47%.
UC may affect the mouth. About 8% of individuals with UC develop oral manifestations. The two most common oral manifestations are aphthous stomatitis and angular cheilitis. Aphthous stomatitis is characterized by ulcers in the mouth, which are benign, noncontagious and often recurrent. Angular chelitis is characterized by redness at the corners of the mouth, which may include painful sores or breaks in the skin. Very rarely, benign pustules may occur in the mouth .
UC may affect the eyes. Inflammation may occur in the interior portion of the eye, leading to uveitis and iritis. Uveitis can cause blurred vision and eye pain, especially when exposed to light . Untreated, uveitis can lead to permanent vision loss. Inflammation may also involve the white part of the eye or the overlying connective tissue , causing conditions called scleritis and episcleritis. Uveitis and iritis are more commonly associated with ulcerative colitis, whereas episcleritis is more commonly associated with Crohn’s disease.
Safety And Tolerability End Points And Analyses
Safety and tolerability were evaluated in all patients in the safety population according to their exposure to study drug. Exposure was calculated using the number of days the patient received study drug, based on first and last dose dates. For patients not enrolled in the ongoing GEMINI LTS study at the data cut-off date, 16weeks were added to the date of the last dose to account for the known duration of detectable vedolizumab serum concentrations. In phase 2 studies, a dose was defined as any amount of infusion, and in phase 3 studies, as 75% of the infusion by volume. Total vedolizumab exposure for a patient was calculated as the sum of exposures in all applicable studies. For patients who received only placebo, exposure to vedolizumab was calculated as 0days.
Infusion-related reactions were defined as AEs occurring on the day of or one calendar day after the infusion that were assessed by the investigator as infusion-related. In addition, blood samples for antivedolizumab antibody assessment were collected within 30min before dosing in the phase 3 studies and within 2h in the phase 2 studies. Immunogenicity was determined as described elsewhere.
Read Also: How To Eat With A Stomach Ulcer
Review Of The Literature
Table summarizes the main literature reporting renal histology in patients affected by IBD. Overall, in accordance with the first report by Hubert et al. in 1984, following studies confirmed IgA nephropathy as the most common type of histological diagnosis. Few patients had granulomatous tubulo-interstitial nephritis that, at the time, were correlated with the exposure to aminosalicylate, but a clear pathological mechanism was not proposed. To the best of our knowledge, a relapse of renal manifestation, characterized by dual renal pathology, has never been previously reported.
Table 1 Main clinical studies reporting renal histology in Inflammatory Bowel Disease
S Boulajaad1* M Haida1 Ait Errami1 S Oubaha2 Z Samlani1 And K Krati1
*Corresponding author:Received: Accepted:Keywords
Cite this as
Copyright
Abstract
The extradigestive manifestations of chronic inflammatory bowel disease most often affect the articulations, skin, eyes, liver and bile ducts. Renal involvement is rare, and manifests as kidney stones, glomerulonephritis, tubulointerstitial nephritis, and secondary amyloidosis. In this context of chronic inflammatory bowel disease, in particular ulcerative colitis, renal involvement is very often secondary to nephrotoxicity of the basic treatment of digestive pathology, and very rarely an authentic extradigestive manifestation of intestinal disease.
We report a case of IgA nephropathy as an extra-digestive manifestation of ulcerative colitis.
The objective of this study is not to neglect the IgA nephtopathy as an extradigestive manifestation of IBD which, even though rare, remains a condition to be looked for by clinicians during the follow-up of IBD.
Main article text
Read Also: Support Surfaces For Pressure Ulcer Prevention
Are There Any Special Dietary Requirements For Persons With Ulcerative Colitis
Although it seems plausible that a specialized diet might benefit patients with ulcerative colitis, there is actually no evidence to support treatment with dietary modification. Despite extensive research, no diet has been found to slow progression, treat, or cure the disease. It is recommended that patients stay on a balanced, healthy diet rich in fruits, vegetables, grains, lean meats, beans, fish, eggs, nuts. Patients should also try to limit foods with saturated fatshigh cholesterol. During flare-ups, patients should continue to eat as tolerated. The Crohn’s and Colitis Foundation of America recommends a bland diet with soft food during a flare including hot cereals, boiled eggs, mashed potatoes, steamed vegetables, canned or cooked vegetables to minimize discomfort.
Does Drinking Water Help Uc
Its important to drink water when you have UC. Having enough fluids will replenish what you lose through diarrhea.
Water alone may not be enough. Your body also loses electrolytes like salt, potassium, and magnesium when you have diarrhea.
Drinking water plus electrolytes can help you stay hydrated. You can find that combination in the form of an oral rehydration solution at your local pharmacy. Sports drinks such as Gatorade and Powerade also contain electrolytes and fluid.
You May Like: Do Ulcers Cause Weight Loss
Crohns Disease And Ulcerative Colitis
A serious but rare complication of these forms of inflammatory bowel disease is fulminant or toxic colitis, formerly called toxic megacolon.
The signs and symptoms of this condition can include bloody diarrhea along with fever, racing heartbeat , low blood pressure , metabolic acidosis , low urine output , and acute kidney failure.
Toxic colitis is more common with ulcerative colitis than it is with Crohns disease.
Symptoms Of Kidney Dysfunction
The kidneys are a vital organ that act as a filter to eliminate waste and toxins, remove excess water, help balance blood pressure, and influence the production of red blood cells and bone health. When the kidneys aren’t functioning properly, symptoms can include:
- Weight loss
- Headaches
- Erectile dysfunction
A MyCrohnsAndColitisTeam member said, I have a lot of kidney pain at times, along with blood in my urine. My kidney doctor says there is no explanation for it. He thinks it’s just from the Crohns. It is very painful.
Read Also: How Do You Treat A Peptic Ulcer
What Are The Risk Factors For Ulcerative Colitis
A number of factors increase the risk of developing ulcerative colitis. Not all people with risk factors will get ulcerative colitis. Risk factors for ulcerative colitis include:
- Consumption of excess dietary fats, protein and refined sugar
- Family history of ulcerative colitis
- Infection of the intestines
- Jewish ancestry
- Quitting
- Retention of appendix
- Use of NSAIDs
Gi Issues Caused By Kidney Stones
Normally, kidney stones cause symptoms such as pressure and pain in your lower back, fever, frequent urination, discomfort urinating, and bloody or discoloured urine. However, sometimes kidney stones can cause gastrointestinal symptoms such as nausea, vomiting, and stomach discomfort.
If youre experiencing sudden low back pain and gastrointestinal discomfort, dont ignore the possibility that it might be kidney stones.
Recommended Reading: How To Cure Ulcerative Proctitis
Baseline Characteristics Of The Study Population
From January 2010 to December 2013, a total of 38812 patients with IBD were enrolled in the IBD cohort . Of these, 16606 patients were included in the IBD incidence group. The IBD cohort comprised 12585 patients with CD and 26227 patients with UC. The control group comprised 116436 age- and sex-matched subjects without IBD. Compared to the control group, the IBD cohort had significantly lower proportions of rural residents and individuals with incomes in the bottom 20% . Moreover, compared to controls, the IBD cohort had significantly lower prevalences of DM , hypertension , and dyslipidemia , and higher prevalences of congestive heart failure , ischemic heart disease , and gout and hyperuricemia . The CD and UC groups were not significantly different from controls in the trends of covariates, except for DM and dyslipidemia. Among the medications prescribed for IBD, 5-ASA, corticosteroids, immunomodulators, and anti-TNF-α agents were prescribed to 36288 , 22284 , 10356 , and 2103 patients with IBD, respectively. The immunomodulators and anti-TNF-α agents were used more frequently by patients with CD than by patients with UC .
Medications For Ulcerative Colitis
The goal of medication is to control inflammation and heal the intestinal lining known as mucosal healing.
Medications used to treat ulcerative colitis include:
- Aminosalicylates, such as sulfasalazine and mesalamine , which reduce inflammation
- to treat bacterial infections
- Antidiarrheals to control diarrhea
- Biologic agents that can rapidly induce remission in patients with severe ulcerative colitis, defined as more than six bloody stool episodes daily
- Corticosteroids
- Immunomodulators that suppress the bodys immune response, such as azathioprine and 6-mercaptopurine
After beginning medication therapy, follow-up blood and stool tests for markers of disease activity, such as fecal calprotectin can help monitor the response to various therapies.
Read Also: What Is Best Medicine For Ulcer
Complications Of Ulcerative Colitis And How To Avoid Them
Learn how to identify and avoid potentially life-threatening complications of ulcerative colitis.
If you have an inflammatory bowel disease like ulcerative colitis , a gastroenterologist can prescribe medication and create a treatment plan for the inflammation and sores, called ulcers, that occur in the lining of the large intestine and rectum. But this autoimmune disorder is often associated with complications in other parts of the body that should be addressed as well.
Extraintestinal complications those that exist outside the intestines can even overshadow symptoms in your bowels, making UC tricky to diagnose. They are also highly prevalent, occurring in nearly half of UC patients and appearing more often in women, according to a review published in May 2019 in Current Gastroenterology Reports. While it remains unclear why UC complications can arise beyond the intestines, the review noted that genetic predisposition, irregular immune response, and changes to the gut microbiome are some common contributing factors.
Its easy to forget that ulcerative colitis is not just a disease of the intestines but a systemic or body-wide disorder of the immune system, says Jessica Philpott, MD, PhD, a gastroenterologist at Cleveland Clinic in Ohio.
Below are five conditions commonly linked to ulcerative colitis, along with some treatment options.
Read Also: What Causes Kidney Stone Pain
Ibd Medications And Kidney Problems
The medications you take for IBD can sometimes cause issues with kidney function. Mesalamine and immunosuppressive medications like cyclosporine can sometimes change kidney function by causing the blood vessels in the kidneys to constrict, but this effect is very rare.
However, studies have found that other medications, such as aminosalicylates, methotrexate, and azathioprine, do not negatively affect estimated glomerular filtration rate , which is used to measure kidney function.
Also Check: How Long Does Pain Last After Kidney Stone Surgery
Read Also: Does Turmeric Help Ulcerative Colitis
Living With Ulcerative Colitis And Kidney Disease
If you are living with UC and kidney disease, it is important to maintain a healthy lifestyle. Many MyCrohnsAndColitisTeam members have shared their tips on how they live with UC and kidney disease. I have regular appointments with my urologist/kidney specialist to check my blood and urine, one member noted. Another said, I exercise and stay at a good weight, while a third member wrote, I try to get enough potassium and vitamin D in my diet.
Other ways to manage UC and kidney disease include:
- Maintaining a healthy, well-balanced diet
Acute Kidney Injury In The Context Of Inflammatory Bowel Disease
Joana Cristóvão Marques1*, Rui Barata1, Joana Lemos Garcia2, David Navarro1, Mário Góis1,3, Helena Sousa1,3, Patrícia Cotovio1, Francisco Ribeiro1 and Fernando Nolasco1
1Nephrology Department, Hospital Curry Cabral, Centro Hospitalar Universitário de Lisboa Central, Lisboa, Portugal
2Gastroenterology Department, Instituto Português de Oncologia, Lisboa, Portugal
3Laboratory of Renal Morphology, Nephrology Department, Hospital Curry Cabral, Centro Hospitalar Universitário de Lisboa Central, Lisboa, Portugal
Read Also: What Not To Eat With Bleeding Ulcers
What Are Immunomodulator Medications
Immunomodulators are medications that weaken the body’s immune system. The immune system is composed of immune cells and the proteins that these cells produce. These cells and proteins serve to defend the body against harmful bacteria, viruses, fungi, and other foreign invaders. Activation of the immune system causes inflammation within the tissues where the activation occurs. Normally, the immune system is activated only when the body is exposed to harmful invaders. In patients with Crohn’s disease and ulcerative colitis, however, the immune system is abnormally and chronically activated in the absence of any known invader. Immunomodulators decrease tissue inflammation by reducing the population of immune cells and/or by interfering with their production of proteins that promote immune activation and inflammation. Generally, the benefits of controlling moderate to severe ulcerative colitis outweigh the risks of infection due to weakened immunity. Examples of immunomodulators include azathioprine , 6-mercaptopurine , cyclosporine , and methotrexate .
Azathioprine and 6-MP
Azathioprine and 6-MP are increasingly recognized by doctors as valuable drugs in treating Crohn’s disease and ulcerative colitis. Some 70% of patients with moderate to severe disease will benefit from these drugs. Because of the slow onset of action and the potential for side effects, however, 6-MP and azathioprine are used mainly in the following situations:
Other Issues in the Use of 6-MP
Methotrexate