Treatment For A Stomach Ulcer
Special diets are now known to have very little impact on the prevention or treatment of stomach ulcers. Treatment options can include:
- medication including antibiotics, to destroy the H. pylori colony, and drugs to help speed the healing process. Different drugs need to be used in combination some of the side effects can include diarrhoea and rashes. Resistance to some of these antibiotics is becoming more common
- subsequent breath tests used to make sure the H. pylori infection has been treated successfully
- changes to existing medication the doses of arthritis medication, aspirin or other anti-inflammatory medication can be altered slightly to reduce their contributing effects on the stomach ulcer.
- reducing acid tablets are available to reduce the acid content in the gastric juices
- lifestyle modifications including quitting cigarettes, since smoking reduces the natural defences in the stomach and impairs the healing process.
Recommended Reading: Is Mango Good For Ulcerative Colitis
Favorite Resource For Diet Advice
This book by A. Hillary Steinhart, MD, provides dietary strategies and recipes to help manage inflammatory bowel disease. The head of the combined division of gastroenterology for Mount Sinai Hospital and the University Health Network in Torontos Mount Sinai Hospital, Dr. Steinhart worked with the clinical dietitian Julie Cepo to offer well-researched dietary advice for people to maintain health during flare-ups as well as periods of remission. The book is packed with 150 recipes, from risotto to stew, to help anyone with IBD eat well and prevent malnutrition.
Doctors assured Danielle Walker that her diet was not a factor in her ulcerative colitis flares. But after years of suffering and multiple hospitalizations, Walker realized that she needed to make dietary changes. At the two-year remission mark, the mom, wife, and self-trained chef began blogging about her experience and sharing recipes to help others struggling with IBD. You can buy Walkers cookbooks on her website, which is loaded with nutritional resources including a blog and videos.
Read Also: Early Symptoms Of Ulcerative Colitis
How Is Acute Severe Ulcerative Colitis Treated
ASUC is a challenging condition to treat. Once you’re admitted to the emergency room, you’ll get a series of tests, including blood tests, stool tests, and an exam of your bowel called a sigmoidoscopy. You’ll also get intravenous fluids to boost hydration.
The average hospital stay for ASUC treatment ranges from 4.6 to 12.5 days. During this time, your health care providers may include a gastroenterologist, colorectal surgeon, dietitian, pharmacist, and stomal therapist. The goal of hospitalizing you is to end the flare, get your symptoms under control, and put the disease into remission. Your doctors will want to make sure that rectal bleeding and diarrhea have stopped and normal bowel movements have returned. Rehospitalization is common.
Intravenous steroid medications are the most common treatment for ASUC. For 30% to 40% of ASUC patients, steroid treatments donât work â and taking steroid medications for more than 10 days increases your risk of complications.
If the steroids donât help within 3 to 5 days, your health care team will start âmedical rescue therapyâ with immunosuppressive drugs like cyclosporine or infliximab.
You might get an operation to remove part of your colon, called a colectomy, if your ASUC doesnât respond to steroids, immunosuppressants, or other medical treatments.
You May Like: What Are The Signs Of A Stomach Ulcer
Oral Vs Rectal Treatments
Most physicians prescribe ulcerative colitis patients oral versions of 5-ASAs or corticosteroids, since this is a patient-preferred delivery method of medication. However, even if they have a specially designed release mechanism, they might not reach and treat the area where the disease is most active.
For example, when you apply sunscreen to your skin, you need to make sure that you cover every exposed part to protect it from the sun. Similarly, when applying these treatments to your rectum and lower colon, you need to make sure that the product covers all of the inflamed areas.
Oral tablets might not be the optimal way to reach the end of the colon, where stool and the fact that ulcerative colitis patients have diarrhea, might interfere with its effectiveness. Unfortunately, this is also the area in the colon where a flare usually starts. The best way to reach this particular area is by inserting the drug directly into the rectum.
Rectal preparations are particularly good at treating urgency and bleeding, symptoms that often are very bothersome. A positive response often occurs within days of treatment.
What Other Conditions Are Related To Ulcerative Colitis
Ulcerative colitis is a type of IBD, but its not the same as irritable bowel syndrome .
Although the disorders share some of the same symptoms, such as abdominal pain and diarrhea, inflammation and ulcers do not occur with IBS.
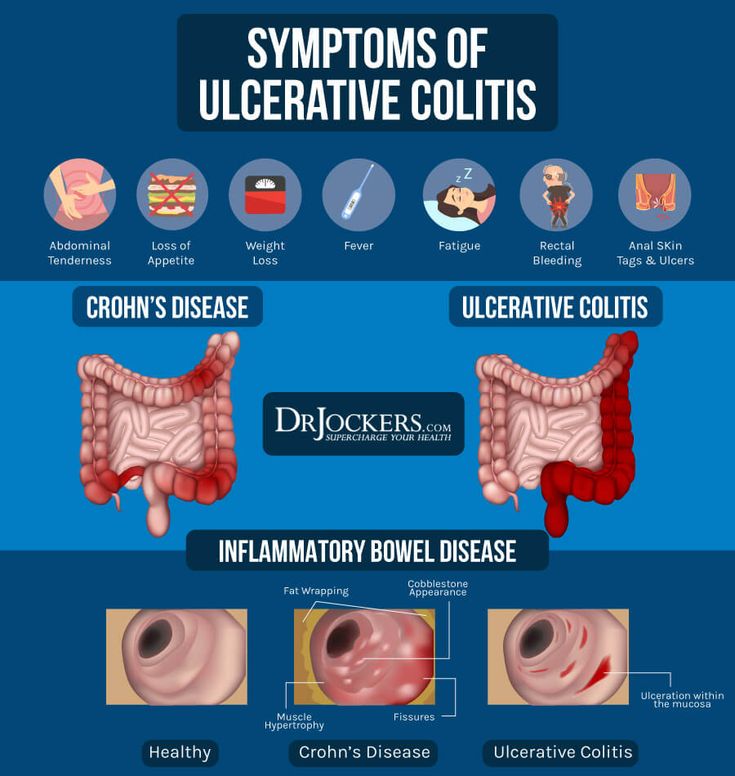
Another disease often mentioned alongside ulcerative colitis is Crohns disease. Ulcerative colitis and Crohns are different types of IBDs that affect the digestive tract in different ways.
The two diseases have a lot of common symptoms, but certain symptoms may make your doctor suspect one disease versus the other.
While diarrhea, rectal bleeding, and abdominal pain are common in both diseases, Crohns disease more often causes nausea, weight loss, and vomiting. The types of abdominal pain are often somewhat different.
Read Also: Where Is Stomach Ulcer Pain
Types Of Ulcerative Colitis
The type of ulcerative colitis you have depends on where it is in your body:
- Ulcerative proctitis is usually the mildest form. Itâs only in the rectum, the part of your colon closest to your . Rectal bleeding may be the only sign of the disease.
- Proctosigmoiditis happens in your rectum and the lower end of your colon . Youâll have bloody diarrhea, belly cramps, and pain. Youâll have the urge to poop, but you wonât be able to.
- Left-sided colitis causes cramps on that side of your belly. Youâll also have bloody diarrhea, and you might lose weight without trying. Youâll have inflammation from your rectum up through the left side of your colon.
- Pancolitis often affects your entire colon. It can cause severe bouts of bloody diarrhea, belly cramps, pain, fatigue, and major weight loss.
- Acute severe ulcerative colitis is rare. It affects your entire colon and causes severe pain, heavy diarrhea, bleeding, and fever.
Are Chia Seeds Good For Intestines
Chia seeds can also act as a cleansing agent for your digestive system since they turn into a sticky gel-like substance when soaked in water. This is a great way to get rid of toxins. If you are suffering from digestive problems, chia seed can help you out.
The seeds are rich in omega-3 fatty acids, which have been shown to help with digestive issues such as constipation, bloating, gas, and diarrhea. In addition, they are high in protein, fiber, vitamins A, C, D, E, K, B12 and K2, as well as B-vitamins B1 and B2.
Don’t Miss: Is Imodium Safe For Ulcerative Colitis
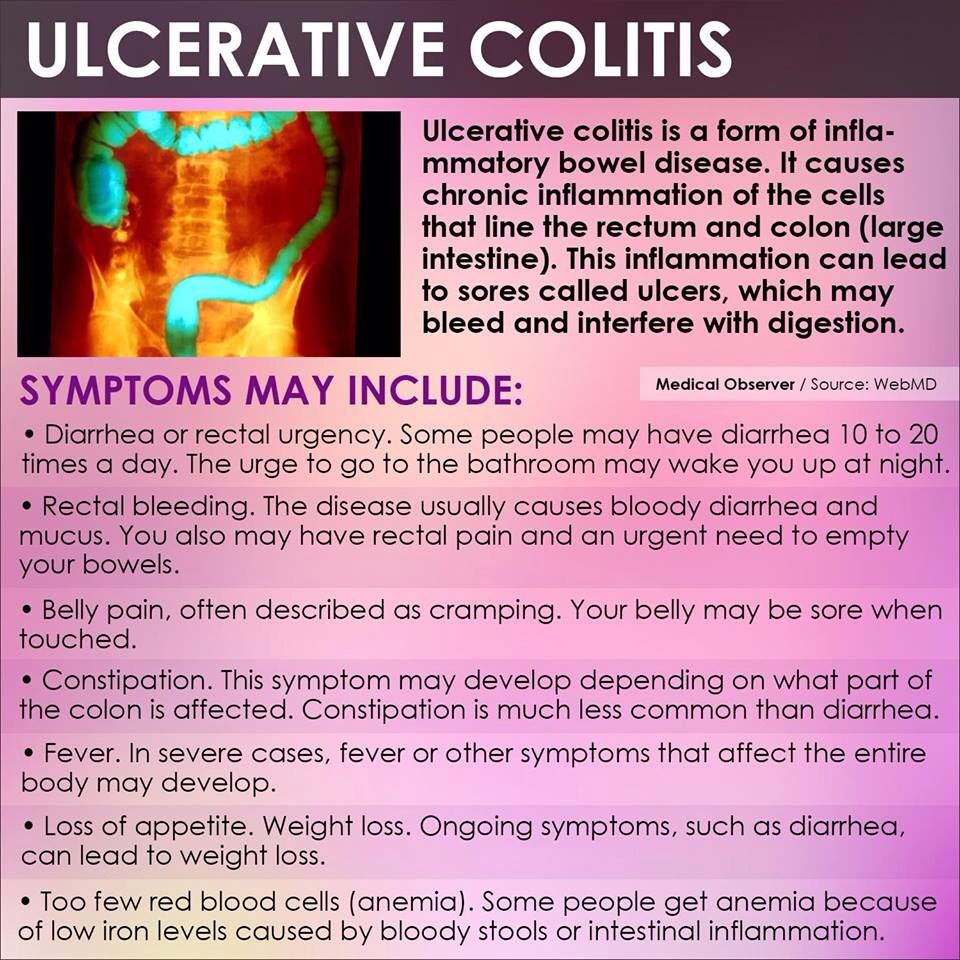
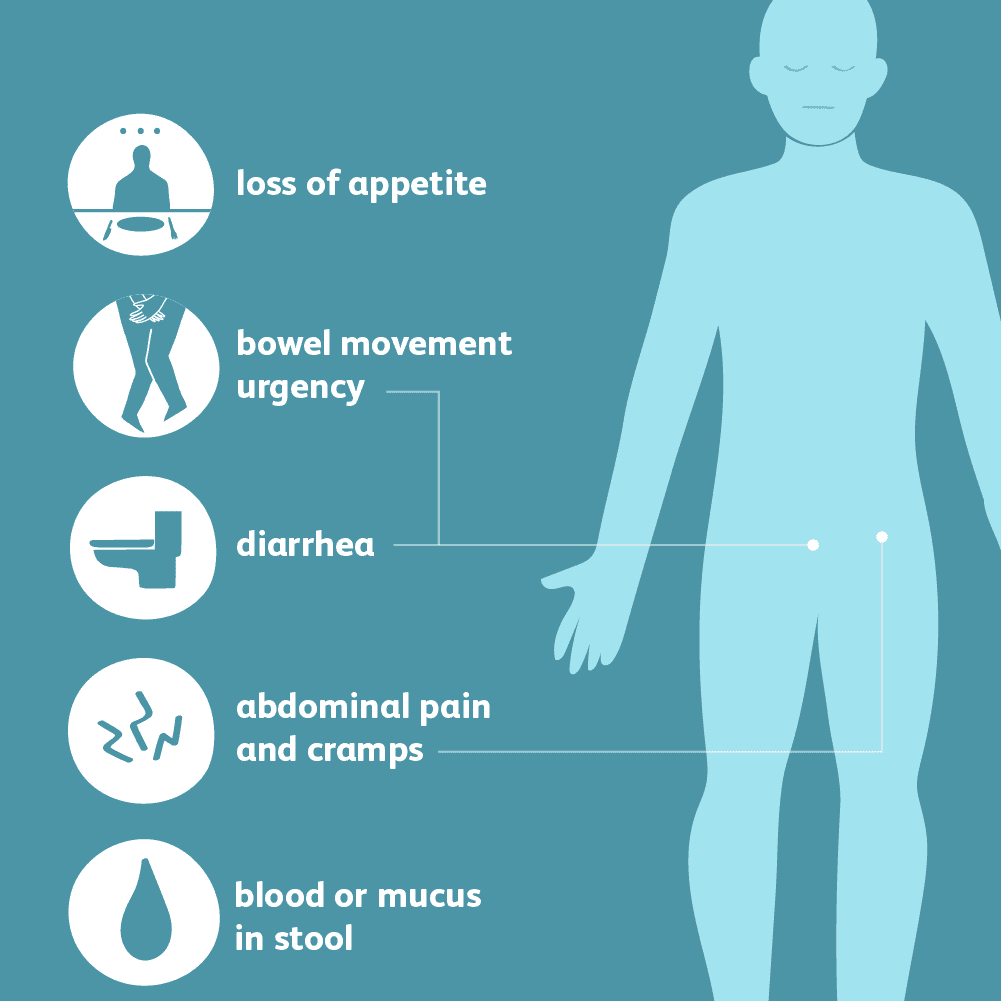
Common Symptoms Of Ulcerative Colitis
While UC symptoms can vary over time and from person to person, the most common symptoms are diarrhea with blood and abdominal discomfort.
However, your symptoms may vary depending on where inflammation occurs in your GI tract and how severe it is.
Other signs and symptoms include:
- An urgent need to have a bowel movement
- Nausea or loss of appetite
- Anemiaa condition in which the body has fewer red blood cells than normal
What Causes Ulcerative Colitis Flareups
When youre in remission from ulcerative colitis, youll want to do everything you can to prevent a flareup. Things that may cause a flareup include:
- Emotional stress: Get at least seven hours of sleep a night, exercise regularly and find healthy ways to relieve stress, such as meditation.
- NSAID use: For pain relief or a fever, use acetaminophen instead of NSAIDs like Motrin® and Advil®.
- Antibiotics: Let your healthcare provider know if antibiotics trigger your symptoms.
You May Like: Cures For Ulcerative Colitis Flare Up
Uc Symptoms Can Get Worse Over Time
Because UC is a chronic disease, symptoms can change or get worse over time. Many people go through periods when they experience few or no symptoms, known as remission, as well as periods of flare-ups when they experience frequent and/or more intense symptoms.
If youre still experiencing symptoms, even while being treated for UC, it could be a sign that your symptoms are not under control.
Experiencing uncontrolled symptoms could mean its time to consider a new treatment.
How To Talk To Your Child About Ulcerative Colitis
Its important to help your child feel comfortable to share changes in symptoms, or when theyve missed a medication dose. Here are some ways to help them cope with symptoms and to feel confident about opening up to you:
- Ask them for updates on how they feel both mentally and physically.
- Use language they can understand. Medical terminology can be scary and confusing, so be sure to explain things at their level.
- Dont diminish the severity of their symptoms. Make sure they feel like they can keep you informed of any changes in how theyre feeling. This can be especially true for psychological symptoms like anxiety and depression.
- Make sure children know that their condition isnt their fault and that they arent alone. Online support groups, forums, and even specialized summer camps can be a good way to share other childrens stories.
- Be an advocate for your child with all medical professionals to let them know that you have their back.
- Remember to take care of yourself as a caregiver. Its easy to let your own needs slide when caring for others.
Don’t Miss: How To Treat Ulcers In Horses
What Role Does Diet And Nutrition Play In Ulcerative Colitis
Diet does not cause the development of ulcerative colitis nor can any special diet cure the disease. However, the foods you or your child eat may play a role in managing symptoms and lengthening the time between flareups.
Some foods may make symptoms worse and should be avoided, especially during flareups. Foods that trigger symptoms are different from person to person. To narrow down what foods affect you, keep track of what you eat each day and how you feel afterward .
Problem foods often include:
- High sugar foods and drinks.
- Carbonated beverages.
- High-fiber foods.
In addition to the problem foods listed above, infants, children and teenagers can also experience issues with:
- Dairy products.
Keep a careful eye on your childs diet and nutrition. Their appetite may decrease during a flareup and they might not eat enough to stay healthy, and grow. Also, the inflammation caused by ulcerative colitis may keep their digestive tract from absorbing enough nutrients. This can also affect your childs health. For these reasons, you may have to increase the amount of calories your child consumes.
Its best to work with your provider and nutritionist to come up with a personalized diet plan if you or your child has ulcerative colitis.
Do I Need To Be Screened For Colon Cancer
Yes. Everyone needs to be screened for colon cancer beginning at 50 years old. But if you have IBD, your risk of colon cancer is higher. You might need to be screened at a younger age or more often than people without IBD.
- Talk to your doctor about when to begin colon cancer screening, what tests to get, and how often to have them.
- Your doctors suggestions will depend on your family health history, how long you have had IBD, whether your colon is affected by your IBD, and how severe it is.
- If you have had IBD for 8 to 10 years, your doctor may recommend a colonoscopy with biopsies every 1 to 2 years. This test checks for early warning signs of cancer.
Also Check: How Do You Check For A Stomach Ulcer
Read Also: Can Tylenol Cause Stomach Ulcers
What Causes Ulcerative Colitis
Researchers think the cause of ulcerative colitis is complex and involves many factors. They think its probably the result of an overactive immune response. The immune systems job is to protect the body from germs and other dangerous substances. But, sometimes your immune system mistakenly attacks your body, which causes inflammation and tissue damage.
Ulcerative Colitis Risk Factors
Most people with UC dont have a family history of the condition. However, about 12 percent of people with UC do have a family member with IBD, according to research from 2014.
UC can develop in a person of any race, but its more common in white people. If youre of Ashkenazi Jewish descent, you have a greater chance of developing the condition than most other groups.
Young people with IBD may also be dealing with acne at the same time. Some older studies have suggested a possible link between the use of the cystic acne medication isotretinoin and UC. However, newer research has yet to find a definitive causal relationship.
Theres no solid evidence indicating that your diet affects whether you develop UC. You may find that certain foods and drinks aggravate your symptoms when you have a flare-up, though.
Practices that may help include:
- drinking small amounts of water throughout the day
- eating smaller meals throughout the day
- limiting your intake of high fiber foods
- avoiding fatty foods
- lowering your intake of milk if youre lactose intolerant
Also, ask a doctor if you should take a multivitamin.
Also Check: What Can Cause Ulcers In Your Mouth
Crohns & Colitis Uk Local Networks
Our Local Networks of volunteers across the UK organise events and provide opportunities to get to know other people in an informal setting, as well as to get involved with educational, awareness-raising and fundraising activities. You may find just being with other people and realising that you are not alone can be reassuring. Families and relatives may also find it useful to meet other people with Crohn’s or Colitis. All events are open to members of Crohns & Colitis UK
How Can You Use This Information
You dont need to become an expert in the tools your doctor uses to determine the severity of your condition. However, it is helpful to understand how this information is used.
Determining severity helps your doctor know how to best treat your IBD. Following changes in severity over time helps you and your doctor know if treatments are working.
There are two separate goals of treatment: improving your symptoms and healing your bowels. While the two usually go hand in hand, your health care provider may see improvement in your bowels before you experience an improvement of your symptoms, or vice versa. If youre not seeing improvement in symptoms or in your bowels, it may be time to discuss different treatment options.
It is important to discuss your treatment goals with your doctor, so you can work together to meet those goals.
You May Like: Boots To Prevent Pressure Ulcers
Medications For Ulcerative Colitis
Medications can calm the inflammation inside your colon. The first one youâll usually try is from a group called aminosalicylates. If that doesnt help, your doctor might prescribe a steroid like prednisone. A third option is an immune modifier, which lowers inflammation by changing the activity of your immune system. It can take up to 3 months before you feel the benefits.
Recurring Or Severe Symptoms Of Ulcerative Colitis
Doctors examine people when their typical symptoms return, but they do not always do tests. If symptoms have been more frequent or longer-lasting than usual, doctors may do sigmoidoscopy or colonoscopy and a blood count. Doctors may do other tests to look for infection or parasites.
When symptoms are severe, people are hospitalized. Doctors take x-rays to look for a dilated or perforated intestine.
Also Check: What Can Cause Ulcerative Colitis Flare Ups
Favorite Ulcerative Colitis Blogger
Sam Cleasby created her blog in 2013 to raise awareness of IBD and her struggles with self-esteem. Cleasby also has a radio show on BBC Radio Sheffield in which she shares about modern family life, including relationships, disability, nutrition, and kids. You can subscribe to her blog via email or follow her on or .
Pearls And Other Issues
There is an increased risk of colorectal cancer in patients with ulcerative colitis. The risk is cumulative, with a 2% chance of colorectal cancer after ten years of diagnosis, 8% after 20 years, and 20% to 30% after 30 years. Two factors associated with increased risk of colorectal cancer are the duration and extent of the disease.
Also Check: Another Name For Pressure Ulcer Is
What Is Ulcerative Colitis Exactly
Ulcerative colitis is one of the two main forms of inflammatory bowel disease . The other is Crohns disease. U.C. occurs when the immune system malfunctions, causing inflammation and ulcers to appear on the inner lining of the large intestine, according to the National Institute of Diabetes and Digestive and Kidney Diseases . Its not comfortable, to put it mildly, and not something that will clear up quickly.
Ulcerative colitis is a chronic illness that does not yet have a medical cure. That doesnt mean nothing can be done though, so dont despair if youre experiencing symptoms. Sidhartha Sinha, M.D., a gastroenterologist, assistant professor at Stanford Medicine, and researcher who specializes in IBD, tells SELF that while there arent medical cures for ulcerative colitis, there are medical treatments. And we have made great advancements in these treatments, he says. The last resort is a surgical option called colectomythe removal of the entire colonwhich can eliminate U.C. entirely.
Ulcerative Colitis Causes And Risk Factors
Ulcerative colitis happens when your immune system makes a mistake. Normally, it attacks invaders in your body, like the common cold. But when you have UC, your immune system thinks food, good gut bacteria, and the cells that line your colon are the intruders. White blood cells that usually protect you attack the lining of your colon instead. They cause the inflammation and ulcers.
Doctors arenât sure why people get the condition. Your genes may play a role the disease sometimes runs in families. Other things in the world around you may make a difference, too.
Things that can affect your risk of getting ulcerative colitis include:
- Age. Itâs most likely if youâre between 15 and 30 years old or older than 60.
- Ethnicity. The risk is highest in people of Ashkenazi Jewish descent.
- Family history. Your risk could be up to 30% higher if you have a close relative with the condition.
Food and stress donât cause it, but they can trigger a flare of symptoms.
Also Check: Can You Take Tylenol With A Stomach Ulcer