How To Treat And Prevent Ulcers
There is no cure for CD, and in the past, treatment focused on alleviating symptoms. Now, says Binion, its believed that mucosal healing, defined by the absence of ulcers, is crucial to disease management and overall quality of life. When patients are able to heal ulcers, that actually has very, very important prognostic implications they will be well, he explains.
To achieve this, healthcare providers will very likely prescribe medications, the type of which depend on the location and severity of your CD. Common drugs include corticosteroids, which lessen inflammation, and immunosuppressants, which help control the immune systems ability to trigger inflammation. Crohns patients are often warned against using non-steroidal anti-inflammatory drugs like ibuprofen, however, as research suggests they may aggravate the disease.
Surgery may be necessary if your CD doesnt respond well to medical therapy. One common procedure to alleviate ulcers and associated complications is a resection, which removes a damaged part of the intestine and connects the healthy ends.
Mucosal healing and remission in general can be aided by a healthy lifestyle, including eating a nutritious diet, getting plenty of physical activity and avoiding smoking. Tobacco use, says Greywoode, puts you at increased risk of having more severe diseaseand having complications related to your disease.
Also Check: How Long Does An Ulcerative Colitis Flare Up Last
What Causes Ulcerative Colitis
Ulcerative colitis is thought to be an autoimmune condition.
This means the immune system, the body’s defence against infection, goes wrong and attacks healthy tissue.
The most popular theory is that the immune system mistakes harmless bacteria inside the colon as a threat and attacks the tissues of the colon, causing it to become inflamed.
Exactly what causes the immune system to behave in this way is unclear.
Many experts think it’s a combination of genetic and environmental factors.
Diagnosis Of Mouth Ulcers
A case of aphthous stomatitis that is not very troublesome or painful does not necessarily require a specific visit to a physician. However, it should be discussed at the next visit to the gastroenterologist who is treating the IBD.
If the ulcers become large, very painful, or do not heal, a dentist or physician should be consulted. A gastroenterologist can determine if the ulcers are in fact aphthous stomatitis, in most cases simply by their appearance and if further testing or any treatment is needed.
Mouth ulcers can be caused by other conditions that may need treatment so they should always be seen by a physician for a diagnosis.
If the ulcers do appear troublesome, the physician may order tests such as a complete blood cell count erythrocyte sedimentation rate and iron, folate, and B-12 levels. A culture or biopsy of the lesions may also be taken.
Read Also: What Is The Treatment For Diabetic Foot Ulcers
Symptoms Of Mouth Ulcers
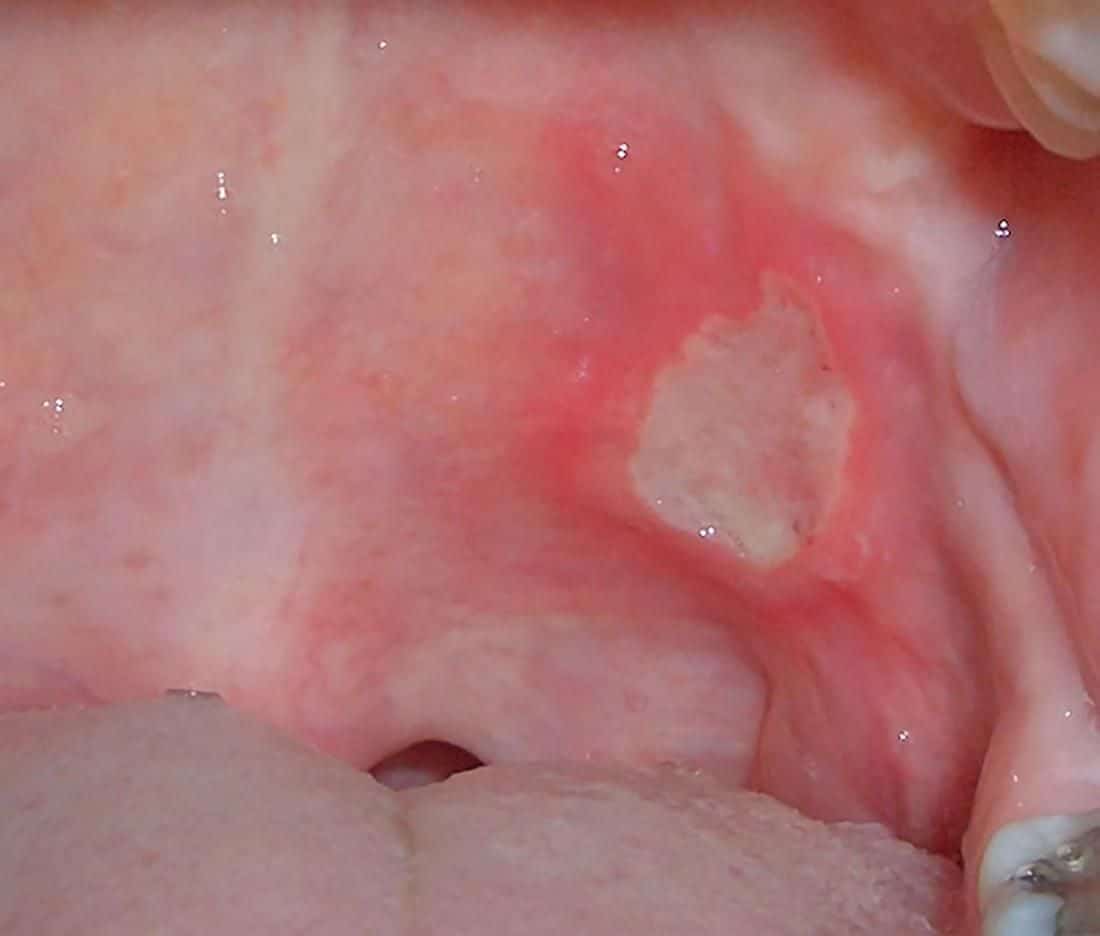
Aphthous ulcers are shallow ulcers in the mucosa of the mouth. They may appear anywhere in the mouth but are frequently found on the inside of the lower lip or cheeks, or on the sides or base of the tongue. They may last from 1 to 2 weeks to months. The ulcers may appear whitish or yellow with a red base, with a grayish layer that develops when they begin to heal. They may also be described as looking like a blister.
Diagnosis Of Crohns Mouth Ulcers
Mouth sores are the first symptoms of Crohns mouth ulcers. Evaluation can be performed with a tissue sample taken from the affected areas. It is examined for signs of inflammation and infection. Certain sores can appear in the mouth when inflammatory cells collect at one spot. These are commonly known as granuloma. Having granuloma is a clear indication that the mouth ulcers have been caused by Crohns disease.
Recommended Reading: Signs Of An Ulcer After Gastric Bypass
Biopsy Of Aphthous Ulcers In A Patient With Crohns Disease
The epithelium is a little bit acanthotic in the connective tissue. It looks like theres a little bit of inflammation, but when you go to a higher power you see these little structures. These are called granulomas.
This is a granulomatous condition with eosinophils scattered throughout. Our differential for diagnosis for granulomatous inflammation would be something thats either caused locally, or it could be a foreign material, an allergy, or a fungal infection.
We can do stains and polarize to see if any of these things show up. Not so much the allergy but the fungal or foreign material. If we do some stains for fungal and its negative, then weve got to start thinking of more systemic causes.
It can be either Crohns disease, sarcoid is also a granulomatous type condition, and TB. But these will be necrotic granulomas in the center.
Involvement Of Body Sites Other Than The Bowel In Inflammatory Bowel Disease
Both forms of inflammatory bowel disease can develop symptoms and signs in addition to the bowel disease. Changes in the skin and oral mucosa can develop with both, but are more commonly seen with Crohn disease. Sometimes these develop before the diagnosis of inflammatory bowel disease, leading the doctor to investigate for bowel problems. In some patients they may appear with flares of the bowel inflammation. Where the association is specific with diagnostic histology, it can be valuable in making the diagnosis.
Also Check: Icd 10 Stage 3 Pressure Ulcer Sacrum
When To Get Medical Advice
You should see a GP as soon as possible if you have symptoms of ulcerative colitis and you have not been diagnosed with the condition.
They can arrange blood or poo sample tests to help determine what may be causing your symptoms.
If necessary, they can refer you to hospital for further tests.
If you have been diagnosed with ulcerative colitis and think you may be having a severe flare-up, contact a GP or your care team for advice.
You may need to be urgently admitted to hospital for immediate care.
If you cannot contact your GP or care team, call NHS 111 or contact your local out-of-hours service.
Crohns Disease And Ulcers: What You Need To Know
Medically reviewed by Jenny Blair, MD
When you have Crohns disease , inflammation often causes ulcers to form in your digestive tract. These open sores may be mild or severe, and can lead to more serious complications, like fistulas and strictures. Theyre considered a hallmark of the condition.
We look for the presence of ulcers to help us make the diagnosis, says David Binion, MD, a gastroenterologist and co-director of the Inflammatory Bowel Disease Center at the University of Pittsburgh Medical Center in Pennsylvania. And the larger and deeper the ulcers, he adds, the more serious the ramifications. Its a warning sign in terms of whats coming down the road in years ahead.
Also Check: Is Greek Yogurt Good For Ulcerative Colitis
Oral Signs Of Crohn Disease
The oral mucosa is commonly affected in Crohn disease with up to one third of patients reported to have oral changes, and even higher in children. In some studies, the oral changes preceded the diagnosis of Crohn disease in 60%. There may be a male predominance.
1. Specific oral mucosal changes: orofacial Crohn disease
In children with Crohn disease, orofacial Crohn disease can be an important presentation preceding the bowel diagnosis.
2. Nonspecific changes in the mouth and surrounding facial skin associated with Crohn disease:
Results Based On Patient Complaints
The frequency of dry mouth , taste changes, and acidic taste sensation in patients was, respectively, 31.1% , 6.2% , and 6.2% .
The frequency of other taste problems was 4.3% . Two cases reported bitterness sensation, and five participants reported changes in the taste sensation after taking the drug.
Seventeen patients had subjective halitosis.
The frequency of oral manifestations before the diagnosis of the disease was 24.2% . The duration of the ulcers was short term in three participants , recurrent in 24 participants , and continuous in 11 patients . Oral ulcers of 21 patients were reduced after diagnosis and treatment, and they were not recovered among 18 patients . Among 28 patients , ulcers were presented during < 1 year before the diagnosis. Among eight patients , ulcers were presented over the past 2 years before the diagnosis. Oral manifestations precede gastrointestinal involvement in three patients for 3 years or more. The ulcers were still present among 28 patients who had oral manifestations before the diagnosis .2]. In addition, the frequency of oral manifestations before the diagnosis was 24.4% among patients suffering from ulcerative colitis and 23.8% among patients suffering from Crohn’s disease.
Oral aphthous ulcers on the oral mucosa.
You May Like: Foam Mattress For Pressure Ulcers
Symptoms Of Crohns Disease
The most common symptoms of Crohns disease are abdominal pain and diarrhea. Other signs of inflammation are often present, including fever and abdominal tenderness. Because symptoms can be worsened by eating, the intake of food is reduced, and this leads to loss of weight, and, less commonly, nutritional deficiencies. Slow, continuous loss of blood into the intestine that may not even be recognizable in the stool can lead to iron deficiency anemia.
How Common Are Mouth Sores In People With Crohn’s Or Colitis

No one knows how common mouth sores are in people with IBD. Studies report estimates ranging from 20% to 50% of patients. Mouth sores are more common in people with Crohn’s disease than ulcerative colitis, and children are more likely to have mouth sores than adults. Men and boys are more likely to have them than girls and women.1 Mouth sores are more likely if you also have inflammation in your esophagus or around your .4
Recommended Reading: What Can Cause Ulcers In Your Mouth
Epidemiology Of Oral Manifestations In Ibd
In 1969, Dyes and colleagues initially described oral lesions in two patients with CD. This was followed in the same year by Dudeneys report of another patient suffering from CD who had oral manifestation. Oral lesions in the absence of intestinal findings in CD were initially described in 1972 by Varley, and there have since been various reports on the incidence of oral lesions in CD. The highest rate was reported from a study in a pediatric age group, indicating a rate of 48%. The prevalence rate is estimated to be between 50% and 20% in most publications.
This variation in rate might be related to the different ages of patients studied, their ethnicity and genetic background, whether they were receiving treatment while being investigated, the experience level of the examiners, and the variation in definition of specific lesions.
In the majority of cases, intestinal involvement precedes the oral lesion. Oral lesions are more common in CD compared to UC, more prevalent in children compared to adults, and with a male dominance. The prevalence is also higher in CD patients with proximal gastrointestinal tract and/or perianal involvement.
Oral lesions may be the primary presenting signs preceding gastrointestinal symptoms in 5%-10% of affected patients. This figure has been reported to be as high as 60% in patients with CD.
Oral Mucosa Signs Of Inflammatory Bowel Disease
The changes of the face and oral mucosa associated with inflammatory bowel disease can be divided into four main categories:
The first three of these categories may be useful in directing the doctor to the bowel problem and making the specific diagnosis.
Don’t Miss: Natural Cure For Peptic Ulcer
Treatments For Oral Crohn’s
Most children and teenagers are worried by the appearance but whether you have gut lesions or not, some treatment can be given, and include:
- exclusion diet – this tries to reduce the intake of food which may make the swelling worse
- mouthwash or paste for mouth ulcers
- injections into the swelling on lips or cheeks to try to improve the appearance. This usually results in a good cosmetic result.
- it is not a good idea to have cosmetic surgery as the swelling returns quickly and lots of scarring may occur. Surgery may sometimes be necessary but should always be done with a doctor’s input.
We use cookies on our website, some of which are essential for our site to work and some help to improve the performance of our site. Click accept if you agree to all performance related cookies. To learn more about cookies, including how we use them, please view our privacy policy at cicra.org/privacy.
Will I Have To Change My Diet
No specific foods are believed to provoke the symptoms of Crohns disease. Even so, it is always recommended to eliminate foods that seem to exacerbate symptoms. The most commonly recommended dietary change is to reduce intake of milk and dairy products, but this recommendation is based primarily on the possibility of lactose intolerance, a genetic abnormality of milk sugar digestion that is unrelated to Crohns disease. If the relationship between milk and symptoms is not clear, it probably is a good idea to do a formal lactose tolerance test to learn for certain whether milk and milk products should be eliminated from the diet. It would be a shame to eliminate milk from the diet unless necessary since milk is an excellent source of nutritious calories, protein, vitamin D, and calcium.
Read Also: Venous Stasis Ulcer Signs And Symptoms
Spectrum Of Oral Manifestations In Ibd
The spectrum of oral lesions described in the medical and dental literature is wide . Some of these lesions are related to IBD, while others represent nutritional deficiencies secondary to malabsorption or adverse reactions to medical therapies.
Figure 1
Oral lesions in patients with IBD can be divided into three categories. First, there are highly specific, pathognomonic entities, occurring almost always in association with IBD with characteristic morphology or/and histology. In second place, there are lesions that are highly suspicious for IBD, meaning that the probability of an underlying IBD, especially CD, is considered to be high. These two categories above may be useful in directing the physician into making the correct IBD diagnosis. Finally, the most common lesions encountered are nonspecific lesions that may occur in association with IBD, but also in its absence . Of note, in CD, the macroscopic and histological appearances of oral lesions often resemble the gastrointestinal tract lesions while in patients with UC oral lesions are histologically unrelated to lesions found in the colon.
Figure 7
The clinical signs of oral involvement in IBD by anatomical location are presented in Table .
Recurrent aphthous stomatitis
Any patient with recurring or insisting oral ulcers should be evaluated medically for the possible presence of later development of a more serious systemic disease.
Salivary duct and saliva in IBD
Linear IgA disease
Buccal abcesses in IBD
Types Of Mouth Ulcers
According to the ADA, the mouth ulcers developed from those affected by Crohns disease are similar to canker sores but technically different.
According to the Mayo Clinic, aphthous ulcers, commonly known as canker sores, are small, ovular, and have a red border. They form on the mucous membranes and are not contagious. Mouth ulcers in those with Crohns disease have similar presentation and symptoms.
There are a few varieties of mouth ulcers that can result from Crohns disease:
- Minor aphthous-like ulcers – cause a low amount of discomfort and are typically less than 5mm in size
- Major aphthous-like ulcers – are painful and typically greater than 5mm in size
- Herpetiform canker sores – occur when smaller lesions combine to form a bigger, irregular ulcer
Helpful tip: Mouth ulcers are different from cold sores caused by the herpes simplex virus and are contagious.
Read Also: Mayo Score 2 Ulcerative Colitis
Oral Lesions In Crohns Disease
Dudeneys report of oral Crohns disease in 1969 described it as a raised, edematous, pink granulation tissue in the buccal mucosa. It is now known that the lips are the most frequent site of oral Crohns disease lesions. Oral lesions may be painful, impair proper oral function, or lead to psychological disorders due to disfigurement. Oral manifestations of CD can be specific or non-specific, based on the presence of granulomas noted on the histopathology reports.
Vitamin And Mineral Deficiencies

If you have Crohns, you often have a greater chance of certain nutritional deficiencies that could potentially lead to mouth probs. Research estimates up to 85 percent of folks with Crohns deal with malnutrition symptoms.
A vitamin K deficiency can also cause bleeding gums. And being short on vitamin B12 or zinc can cause glossitis, a condition that leads to tongue swelling and redness.
Read Also: What Do I Take For An Ulcer
Oral Manifestation In Inflammatory Bowel Disease: A Review
Correspondence to: Gholam Reza Sivandzadeh, MD, Department of Internal Medicine, Gastroenterohepatology Research Center, Shiraz University of Medical Sciences, Namazi Hospital, Zand St., Shiraz 7193711351, Fars, Iran.
Telephone: +98-711-6473236 Fax: +98-711-6474316
What Else Should I Know About Crohns Disease
People with Crohns disease are at risk for colon cancer, which is related to chronic inflammation. So they should get a colonoscopy every 12 years, starting about 10 years after diagnosis.
Kids and teens with Crohns disease may feel different and not be able to do the things their friends can do, especially during flare-ups. Some struggle with a poor self-image, depression, or anxiety. They may not take their medicine or follow their diet. Its important to talk to your health care professional if youre concerned about your childs mood, behavior, or school performance.
Parents can help teens with Crohns disease can take on more responsibility for their health as they get older. Encourage teens to take their medicine, take care of themselves, and manage stress in positive ways. Yoga, meditation, breathing and relaxation techniques, music, art, dance, writing, or talking to a friend can help.
You also can find more information and support online at:
You May Like: I Think I Have Ulcerative Colitis
Don’t Miss: Can Stomach Ulcers Cause Cancer