Clinical Characteristics And Outcomes Of Primary Sclerosing Cholangitis And Ulcerative Colitis In Japanese Patients
-
Contributed equally to this work with: Junichiro Kumagai, Takashi Taida, Sadahisa Ogasawara, Tomoo Nakagawa
Roles Conceptualization, Data curation, Formal analysis, Investigation, Methodology, Writing original draft, Writing review & editing
Affiliation Department of Gastroenterology, Graduate School of Medicine, Chiba University, Chiba, Japan
-
Contributed equally to this work with: Junichiro Kumagai, Takashi Taida, Sadahisa Ogasawara, Tomoo Nakagawa
Roles Conceptualization, Data curation, Writing review & editing
Affiliation Department of Gastroenterology, Graduate School of Medicine, Chiba University, Chiba, Japan
-
Contributed equally to this work with: Junichiro Kumagai, Takashi Taida, Sadahisa Ogasawara, Tomoo Nakagawa
Roles Conceptualization, Formal analysis, Investigation, Methodology, Project administration, Visualization, Writing original draft, Writing review & editing
Affiliation Department of Gastroenterology, Graduate School of Medicine, Chiba University, Chiba, Japan
-
Contributed equally to this work with: Junichiro Kumagai, Takashi Taida, Sadahisa Ogasawara, Tomoo Nakagawa
Roles Data curation, Writing review & editing
Affiliation Department of Gastroenterology, Graduate School of Medicine, Chiba University, Chiba, Japan
Cancer Epidemiology In Primary Sclerosing Cholangitis
PSC is associated with a major lifetime risk of gastrointestinal cancers. Compared with the general population, patients with PSC have double the risk of cancer in general and 40 times the risk of a primary hepatobiliary cancer. Various studies have shown that patients with PSC have a significantly increased risk of developing cholangiocarcinoma , gallbladder carcinoma , hepatocellular carcinoma , and colorectal carcinoma . We discuss each of these in forthcoming sections.
Lifetime incidence of various cancers associated with primary sclerosing cholangitis and their respective risks compared with the general population. Estimations of lifetime incidence are made from limited available data , and thus may often underestimate true lifetime risk. 1The risk in patients with PSC-IBD is 4× the risk in patients with UC alone and 10× the risk in the general population. PSC: Primary sclerosing cholangitis PSC-IBD: Inflammatory bowel disease co-existing with primary sclerosing cholangitis UC: Ulcerative colitis.
Risk Of Malignancy In Psc
There is a high risk of malignancy in both PSC and IBD alone. However, their combination confers a significantly greater risk and requires shorter screening intervals for both CRC and hepatobiliary malignancy. Unfortunately, because of the relatively recent description of this phenotype, there is no strong evidence to inform malignancy screening guidelines. As a result, several of the screening recommendations are from guidelines describing PSC and IBD alone and are extrapolated to include screening in PSC-IBD patients.
You May Like: What Happens In Ulcerative Colitis
What Is The Connection Between Psc And Ulcerative Colitis
About two-thirds of people with PSC have ulcerative colitis, a type of inflammatory bowel disease . People with PSC also may have another type of IBD called Crohns disease.
Its not entirely clear why so many people with PSC also have IBD. Researchers at UChicago Medicine are investigating the interaction between environmental triggers, the immune system and the gut microbiome to help understand the connection between the two diseases.
What is known is that people with PSC and ulcerative colitis have inflammation throughout their colon. They also have a higher risk for cancer in the colon, bile duct and gallbladder.
At the IBD Center and Center for Liver Diseases at UChicago Medicine, our specialists have extensive experience managing both conditions and can help people with PSC and IBD manage their special health risks.
Microbiome Of Children Under 10 Years Of Age
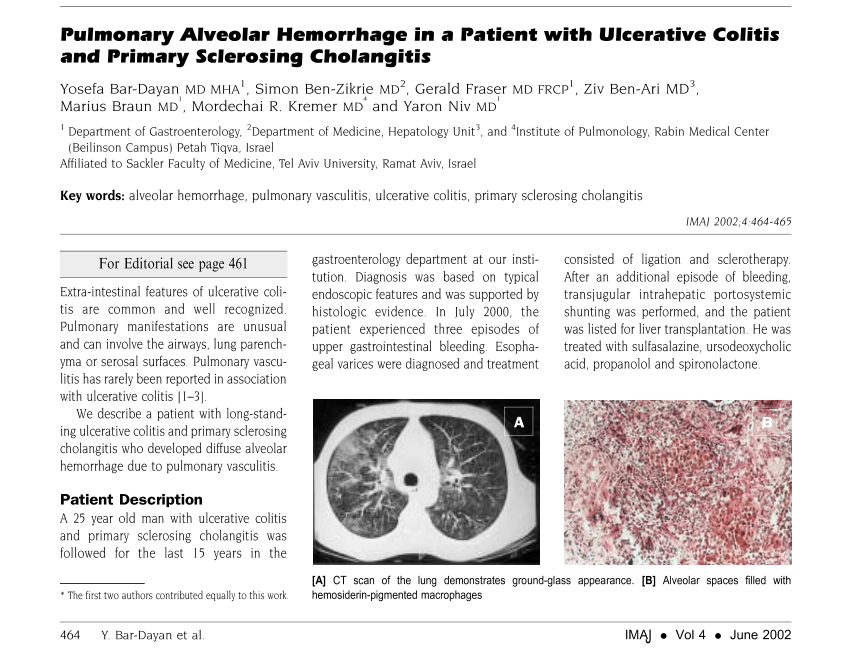
Children under 10 years of age were subsampled according to age at sample collection therefore, we subsampled them at < 10 years of age at diagnosis – PSC group , UC group , PSC+UC group , and Control Group . The predominant phyla were Firmicutes and Bacteroidetes , and Firmicutes was more abundant in the PSC group and Bacteroidetes was more prevalent in the UC group. The relative abundances of Proteobacteria and Actinobacteria were significantly higher in the PSC+UC and UC groups, compared to the control group.
The most abundant bacterial genus found in children < 10 years old was Bacteroides , which was more prevalent in the UC group and less prevalent in the PSC+UC group, but the results were not statistically significant. Interestingly, the relative abundance of Bifidobacterium was significantly higher in the UC group than in controls . The abundance of Streptococcus in the PSC group was statistically higher than that in the control group . In addition, the abundance of the genus Veillonella was significantly greater in the PSC and PSC+UC groups than in controls , and Escherichia-Shigella showed significantly higher values in the PSC+UC group than in controls .
Don’t Miss: Compression Therapy For Venous Leg Ulcers
Magnetic Resonance Scans And Protocol
Magnetic resonance cholangiograms for cases and negative controls were obtained between 2005 and 2010, within 3 months of recruitment into this study. MRC followed a standard protocol with the same 1.5T GE Signa Echospeed MR scanner for each, acquiring axial and coronal T2-weighted gradient echo and thick and thin slice heavily T2-weighted gradient echo MRC sequences. All positive controls had MRC sequences within a 10-year period of the cases and negative controls, although the MR scanners used varied for this group.
Disease Statusactive Vs Remission/controlled Disease
To evaluate the influence of active or remission/controlled disease status on the intestinal microbiome, we explored the distances between patients and their respective healthy control according to the disease status . In the PSC+UC group , the distances between patients in active disease status and their respective healthy control were significantly higher than the distances between patients in remission disease status from their controls . We observed a similar tendency for the UC group however, it was not statistically significant .
Figure 5 Principal Coordinate Analyses plots of Bray-Curtis distance between each patient and the respective control. According to the disease status of patients in the PSC + UC or UC groups, and according to the active or remission disease status shows significant differences for the PSC + UC group , but not for the UC group by the MannWhitney test. UC, Ulcerative Colitis group PSC + UC, Primary Sclerosing Cholangitis with concomitant Ulcerative Colitis.
Subsequent analysis, independent of age and disease groups remission/controlled patients and patients in activity , showed a significant higher relative abundance of Ruminoclostridium 5 and Ruminococcaceae UCG 002 in patients in remission/controlled disease compared to patients with active disease . In addition, Veillonella was increased in patients with active disease , and Escherichia-Shigella tended to increase in this group .
Recommended Reading: Signs Of Having An Ulcer
Can Primary Sclerosing Cholangitis Be Misdiagnosed
Diagnosing PSC requires expertise, so its possible that you may have PSC for many years before it is accurately diagnosed. One reason is that you may have PSC without any symptoms just certain signs in your bloodwork. That is why it is important to go to a center like the one at UChicago Medicine that has extensive experience diagnosing and managing patients with liver diseases like PSC.
Definitions For This Study
The extent of colitis was defined as the maximum documented extent histologically at any time during the course of the disease. Liver biochemistry was defined as normal if the serum alkaline phosphatase , gamma-glutamyl transferase and alanine transferase values were below the upper limit of normal for our institution at the time of recruitment and on all previous hospital records. An isolated mildly elevated bilirubin was accepted after assessment by a consultant hepatologist as attributable to Gilbert’s syndrome. The presence of CRD or CRC was identified at colonoscopy and confirmed histologically. CRD was classified at the time of this study, as either flat or associated with a raised lesion or mass or adenoma-like mass ), and confirmed histologically as arising within an area of documented colitis. In accordance with current SCENIC classification, these would be classified as endoscopically invisible dysplasia, endoscopically resectable non-polypoid and polypoid lesions. Two separate gastrointestinal pathologists blinded to clinical details reviewed the colonic biopsies and re-defined the degree of dysplasia using the WHO classification: low-grade CRD or high-grade CRD .
Read Also: Boost Vs Ensure Ulcerative Colitis
Surveillance For Hepatocellular Carcinoma
Historically, patients with PSC have been considered to have a relatively low risk for developing HCC, with an estimated lifetime incidence below 1.5%, a cut off established to justify regular HCC surveillance strategies based on cost-benefit analysis. However, reports on the incidence of PSC have been limited and vary considerably. In a retrospective study of 119 patients with PSC and cirrhosis, no patients developed HCC. Conversely, in a more recent study of 830 patients with PSC, 2.8% were found to have HCC, all of whom had underlying cirrhosis. Therefore, it is unclear whether HCC surveillance is indicated for all patients with PSC. At this time, the AASLD, EASL, and ACG do not provide specific recommendations on screening for HCC in patients with PSC, in part due to the fact that many patients with PSC do not have cirrhosis. Our practice is to conduct HCC surveillance with imaging every 6 mo for all patients with PSC-related cirrhosis, as is done for patients with cirrhosis due to other diseases. For patients without cirrhosis, surveillance for HCC is effectively a byproduct of routine CCA surveillance.
Characteristics Of Psc Associated With Ibd
While the presence of IBD with PSC appears to convey a specific IBD phenotype, the converse does not appear to be true. Microscopically, an early study noted no significant difference in the degree of histologic periductal fibrosis, periductal inflammation, portal edema or fibrosis in PSC vs. PSC-UC patients . Macroscopically, data conflict regarding the degree of intrahepatic and extrahepatic involvement in PSC-IBD vs. PSC alone . Clinically, PSC outcome measurements, including transplant-free survival rates, cirrhosis rates and mortality, did not differ significantly between PSC-IBD patients and those with PSC-alone . Notably, however, recent studies by Fevery and Weismüller report higher rates of liver-related morbidity and mortality in PSC-UC patients when compared to patients with PSC-CD or PSC alone. These data suggest the subtype of IBD may have an impact on the course of PSC disease progression .
Read Also: Foods That Irritate Stomach Ulcers
Surveillance For Gallbladder Carcinoma
In the general population, GBC is often diagnosed at late stages because of the paucity of symptoms at early stages. By the time a diagnosis is made, patients often have metastatic cancer and a 5-year survival rate of less than 5%. However, if detected incidentally or at an early stage , 5-year survival after simple cholecystectomy is near 100%. The same analogy can be made for patients with PSC however, patients with PSC are much more likely to have gallbladder neoplasms than the general population, as mentioned earlier, and a high proportion of such lesions harbor malignancy in PSC. Given these considerations, both the AASLD and EASL recommend yearly abdominal ultrasound in patients with PSC. Although ultrasound is the preferred modality due to its high accuracy, availability, and cost-effectiveness, GBC surveillance can also be performed with MRI/MRCP . As discussed earlier in this review, all patients with PSC with gallbladder polyps greater than 8 mm in size or gallbladder masses of any size should be evaluated for cholecystectomy while smaller lesions may be observed.
Patient Demographics And Clinical Features
Demographics and clinical features of UC patients in the extensive UC and CRD cohorts are outlined in Table , and features specific to UC patients with CRD are shown in Table . Positive and negative controls were well matched to cases . Overall, most patients were male, had extensive UC and were taking 5-ASA prior to MRC evaluation. Patients in the extensive UC cohort were younger with a shorter duration of UC at the time of recruitment compared with those in the CRD cohort. The colectomy rate was lower in patients with extensive UC compared to CRD , and the surgical indication for the extensive UC cohort was active disease. In the CRD cohort, dysplasia was the sole indication for surgery. Elevated total IgG and IgG4 subclass levels were detected more frequently in those with CRD compared with extensive UC, although the absolute values were not raised overall .
| Variables |
|---|
| Cardiovascular disease | Metastatic GB/biliary adenocarcinoma |
In the cohort of patients with sub-clinical PSC-UC, only those assessed as definite PSC had the outcomes of progression of MRC changes , development of cirrhosis and anorectal adenocarcinoma . However, both those assessed as possible PSC and definite PSC developed abnormal liver biochemistry and hepatobiliary malignancy .
Recommended Reading: Can Stress Cause Flare Up Ulcerative Colitis
Primary Sclerosing Cholangitis With Ulcerative Colitis Presents As A Unique Disease Phenotype
Patients with primary sclerosing cholangitis and ulcerative colitis had distinct disease symptoms compared with patients with PSC or UC alone. These findings, from a retrospective study, were published in the World Journal of Gastroenterology.
Patients with UC , Crohn disease , PSC without inflammatory bowel disease , PSC-UC , and PSC-CD had colonic biopsy and resection specimens collected between 1999 and 2013 at the Barnes-Jewish Hospital in the United States. Patients with and without PSC were matched for age and CD or UC disease duration.
Among patients with UC, the PSC-UC and UC groups did not differ significantly for sex, diagnosis age, or dysplasia rates. Fewer patients with PSC-UC were treated with steroids or had colectomies compared with patients with UC alone.
The biopsy data indicated that in patients with PSC-UC, disease was more likely to be confined to the right side of the colon , activity scores were lower in the rectum , there was less basal plasmacytosis in the left colon and rectum , and overall inflammation was lower across all sites , compared with UC alone, respectively.
Among patients with CD, the PSC-CD and CD groups were well balanced for age at diagnosis, CD disease duration, colectomy rates, and dysplasia rates. The PSC-CD group had more men , and fewer were treated with anti-tumor necrosis factor therapy compared with patients with CD alone. Comparison of biopsy specimens between patient groups did not reveal any significant differences.
Demographic And Clinical Characteristics
The basic demographic and clinical information including age, gender, race, age at PSC diagnosis and colonoscopic extent of UC are summarised in Table . Patients with PSC were divided into two groups: 167 with PSC-UC and 55 with PSC alone . The median age at presentation for the subgroup of PSC alone patients was 48 years. These patients were significantly older than the group of PSC-UC patients whose median age at diagnosis was 37 years. The male to female ratio was slightly lower in patients in PSC alone group, although the difference was not statistically significant. There was no significant difference in the age of the patients at the time of last follow-up in the two groups: mean age was 53.4 ± 13.1 years in the PSC alone group vs. 51.5 ± 12.8 years in the PSC-UC group.
| Variable |
|---|
| PSC/UC | 0.90 | 0.60 |
- 0: Low risk-Mayo PSC risk score 0 1: Medium risk-Mayo PSC risk score > 0 < 2 2: High risk-Mayo PSC risk score 2.
Read Also: Low Residue Diet For Ulcerative Colitis
Demographic And Clinical Variables
Demographic and clinical variables were studied from patient medical records including age, gender, smoking and alcohol history, and family history of IBD, PSC or liver/colon cancer in first degree relatives. The clinical variables were defined as follows- duration of UC defined as the time from the diagnosis of UC to the time of last clinical follow-up, family history of IBD-CD or UC in first degree relatives, smoking-smoking more than seven cigarettes a week, Alcohol use defined as more than two drinks a day, extent of UC Extensive colitis -endoscopic, macroscopic or microscopic evidence of disease proximal to the splenic flexure.
The following variables with regard to UC were obtained UC activity in the last 5 years of the follow-up period type of UC treatment used during the whole follow-up period severity of disease at last colonoscopy , assessed macroscopically and histologically and information on UC flares during the last 5 years of follow-up. We had earlier described the collection of these data into the database.
The Mayo Risk Score was calculated at entry using the revised PSC Mayo Risk Score. This score was developed to assess 1-year to 4-year probability of survival of patients with PSC and its advantage is that there is no requirement for liver histology.
Selection Of Cases And Controls
The study population consisted of patients with either Crohnâs disease or ulcerative colitis who enrolled in the University of Pittsburgh Medical Center Inflammatory Bowel Disease Research Registry from 2000 to 2009. The research registry facilitates retrospective research studies on IBD, as registry participants provide written informed consent to allow analysis of their identifiable medical record information. Enrollment and participation in the research registry was approved by the University of Pittsburgh Institutional Review Board.
The study involved a search of the Medical Archival Retrieval System at UPMC, a repository of electronic medical records . Using UPMC MARS, IBD registry patients were identified who had blood eosinophilia, defined by an absolute eosinophil count greater than normal , as defined by UPMC clinical laboratory), on a complete blood count at any time between 1996 and 2009. To focus our attention on individuals with likely eosinophilia-associated IBD, we sought to find subjects with significant and recurrent eosinophilia and defined cases as IBD patients who had AEC equal to or greater than 0.5 Ã 109/liter on at least 4 separate occasions, with at least 2 episodes occurring 4 or more weeks apart.
Recommended Reading: Blood Clots In Stool With Ulcerative Colitis
Gut Microbiome Of Children And Adolescents With Primary Sclerosing Cholangitis In Association With Ulcerative Colitis
- 1Department of Clinical and Toxicological Analysis, School of Pharmaceutical Sciences Universidade de Sao Paulo , São Paulo, Brazil
- 2School of Pharmaceutical Sciences, Universidade de Sao Paulo, São Paulo, Brazil
- 3Department of Gastroenterology and Hepatology, Child Institute, ICR-HC/FM, Universidade de Sao Paulo , São Paulo, Brazil
- 4Department of Hepatology and Liver Transplantation, Hospital Sirio Libanes/Hospital Municipal Infantil Menino Jesus, São Paulo, Brazil
- 5School of Arts, Science and Humanities, University of Sao Paulo, São Paulo, Brazil