Zinc To Speed Up The Healing
Zinc-rich foods like eggs, nuts, and legumes can prove to be very beneficial for both your diabetes and diabetic foot ulcers. Zinc promotes the production and secretion of insulin in the body and thus helps to keep blood sugar levels in check. Zinc also hastens the healing of the wound by maintaining the structural integrity of the dermal tissue.
Dressings And Topical Products
Alginate and other dressings
Alginate dressings are derived from seaweed and come in the form of calcium alginate or calcium sodium alginate or alginic acid. These alginate products form a highly absorbent gel that can absorb large volume of wound exudates to avoid skin maceration yet still maintain a moist environment. A Cochrane review and meta-analysis in 2013 showed no significant difference in ulcer healing with alginate products when compared with basic contact dressings or silver hydrocolloid dressings. Another systematic review in 2016 also found no difference in healing time between other synthetic active dressings and traditional dressings, including wet to dry saline moistened gauze, Vaseline gauze, and hydrofiber. As an exception, moderate-quality evidence suggested that hydrogel was more effective in healing DFUs.
Topical antiseptics and antimicrobials
Other topical products
Caring For Wounds And Foot Ulcers In Diabetic Patients
The Centers for Disease Control and Prevention reports that there are 30.3 million people living with diabetes in the United States. Diabetes comes with many serious complications, including chronic wounds, nerve damage and foot ulcers.
The American Podiatric Medical Association reports that 15 percent of diabetic patients will develop a foot ulcer. Further, diabetes is the leading cause of nontraumatic, lower-extremity amputations in the U.S. caused by infected wounds and foot ulcers that cannot heal. While difficult to treat, foot ulcers often can be prevented.
Controlling risk factors and monitoring the skin daily is key to minimizing the negative effects of diabetes, said Nancy Estocado, Advanced Wound Care Clinical Coordinator at Sunrise Hospital and Medical Center. For anyone with diabetes, understanding how to prevent and properly address wounds especially foot ulcers is integral to living a healthy life.
Read Also: Wound Vac For Pressure Ulcers
Diabetic Foot Ulcer Symptoms
Normally a wound or sore on the skin would cause pain. But the same loss of feeling in the feet that often contributes to the development of a diabetic foot ulcer means that theres often no pain associated with the ulcer. This can make it difficult for people to realize that an ulcer is even there in the early stages, when treatment is most effective.
Aside from pain, another sign to look for is discharge or drainage from the wound in the socks. Ulcers that have been present for some time and that have become infected may also cause an unpleasant odor.
Evidence Base For Wound Care Treatments

There is currently little evidence to justify the adoption of very many of the products and procedures currently promoted for use in clinical practice. Guidelines are required to encourage clinicians to adopt only those treatments that have been shown to be effective in robust studies and principally in RCTs. The design and conduct of such RCTs needs improved governance because many are of low standard and do not always provide the evidence that is claimed. There should be new guidance on the conduct of RCTs in this field, and it should embrace items such as those covered in the 21-item checklist of study quality reproduced as . Clinicians need to be able to assess the relative validity of published work, including its strengths and limitations in trial design, conduct, and reporting.
Recommended Reading: How Do I Know If I Have A Peptic Ulcer
What Is The Outlook For People With Diabetic Foot
Diabetic foot ulcers are fairly common in people who have had diabetes for a long time. Even with foot checks and careful blood glucose monitoring, some people with diabetes develop infections.
The outlook depends on factors such as:
- How early the wound was found.
- Presence of infection and how much it spreads.
- Treatment effectiveness.
If the infection cant be controlled and spreads too far, amputation may be necessary.
How Do You Treat A Cut On A Diabetic Foot
As we mentioned before, broken skin on the foot is more likely to become infected because of diabetes. This means that treatment for diabetic cuts or wounds should be almost immediate. So what are some treatments for a cut on a diabetic foot?
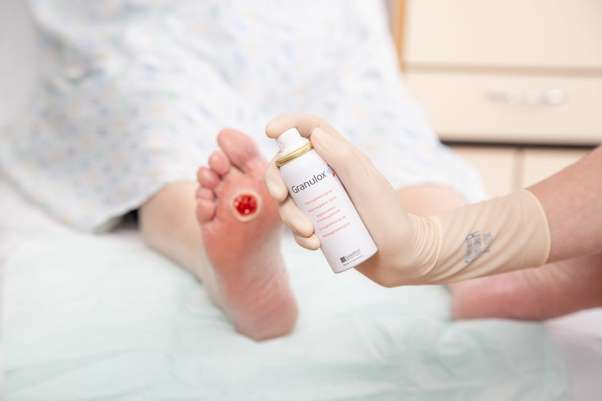
The most common treatment for open wounds or ulcers in people with diabetes is using a cleanliness regimen and dressings to promote rapid wound healing and prevent infection. Cleaning the wound/ulcer meticulously with soap and water removes all dead tissue such as slough from the surface making it a less perfect environment for bacterial growth and improves the healing process. A wet dressing can use material from previous incisions which have healed as well as dry non-adherent dressings available over-the-counter at pharmacies, grocery stores, to help maintain a moist environment around the wound/ulcer which can speed up the healing process and prevent infections around the affected area.
Here are some basic steps on how to treat a wound on a diabetic foot:
Recommended Reading: Does Smoking Cause Ulcers After Gastric Bypass
Make Sure You Dont Have An Infection:
- This is an area where your podiatrist can work with an infectious disease doctor. If you have any redness around your wound or drainage from the center of your wound, you likely have an infection of the current. In the short term, it is essential to start taking antibiotics and to get antibiotic medication onto this site. This can be life-threatening if allowed to continue for lengthy periods of time without improving.
- If you have redness or drainage developing around your ulcer, dont waste any time, this is the single most urgent thing you can do, dont be someone who loses their leg because they waited one or two days too long.
Treatment For Vascular Ulcers
Its important to note that not all skin ulcers are caused by diabetes, and that even people who dont have diabetes can suffer from chronic wounds. Even people without diabetes can be susceptible to vascular ulcers. Vascular ulcers are caused by problems with the vascular system .
These types of ulcers can happen to people who suffer from veins or arteries that dont function properly, causing blood flow in the legs to be limited. This can lead to an increased risk of wounds that may not heal normally and can become infected.
The Wound Care Center at Harrington also provides full service care for these types of wounds, including on-site X-rays, MRI and lab work.
To make an appointment at the Harrington Wound Care Center, call 248-8105. You can also learn more on our website here.
Don’t Miss: How To Check A Horse For Ulcers
What Happens If A Diabetic Gets A Cut On Their Foot
A wound is an injury to the skin or other external part of the body that breaks its surface. A wound may be caused by blunt force trauma, a cut from a sharp object, or pressure. Diabetes can increase your risk for wounds because it affects blood circulation and nerve function in your feet. It also makes you more prone to infection than someone without diabetes. If you get a cut on your foot, elevated protein levels will make your cells vulnerable to forming scar tissue which blocks red and white corpuscles called platelets from joining together to form clots during the healing time.
If a diabetic gets a cut on their foot, it can lead to ulceration that may eventually result in amputation of the limb, when not treated correctly. There wound treatment is very important for people with diabetes.
Diabetic wounds are often very difficult to heal. There are a lot of reasons why they may not heal well, but one common cause is that the person has poor diabetes management including high blood glucose levels and poor blood flow in their feet. This means that even if someone cuts themselves or gets an open wound on their foot, it’s harder for them to get better at healing because there is less blood flowing through the area around the cut or wound site.
Treatment Of Active Infection
Wound infection is a known predictor of poor wound healing and amputation. The appropriate recognition of infection and treatment with antibiotics in diabetic foot infection is imperative to improve outcomes. Conversely, inappropriately treating with antibiotics, often in the setting of fear of missing an infection, to reduce bacterial burden or prophylaxis is associated with several adverse effects, including antibacterial resistance. The IDSA has outlined specific guidelines for the treatment of diabetic foot infections. The IDSA recommends treatment of wounds with at least two signs or symptoms of inflammation or purulent secretion. It is recommended that, before antibiotic therapy, a deep tissue culture via biopsy or curettage after debridement be obtained. Swab specimens should be avoided, especially in inadequately debrided wounds. Antibiotic therapy should be targeted to aerobic Gram-positive cocci in mild to moderate infections. Severe infections should be treated with broad-spectrum empiric antibiotics pending cultures. IDSA recommends 1- to 2-week antibiotic course for mild infections and 23 weeks for moderate to severe infections, but antibiotics can usually be discontinued once clinical signs and symptoms of infections have resolved. To avoid antibacterial resistance and other adverse outcome of therapy, it is best practice that treatment of clinical diabetic foot infections be completed with narrow=spectrum antibiotics for the shortest duration possible.922
Q: When Should I Call A Podiatrist For An Appointment
A: Pain is never normal, especially if it has been going on for longer than one week. This means that most insurance plans will cover a visit if you feel you have a problem developing with your feet.
The longer you wait, the more serious the pain may become, which can lead to hospitalization or further foot problems.
It would help if you had it evaluated and treated to avoid long-term problems.
Q: Is Podiatrist Toenail Trimming Covered By Insurance
Yes, this service may be covered for people with help issues that cannot help themselves. If your foot is in pain or has a health issue, a podiatrist is recommended to evaluate you, and this is a covered option.
If you have foot pain, please call our office and schedule a no-obligation consultation with our podiatrists to assess your eligibility for foot care.
Etiology Of Foot Ulceration
The etiology of diabetic foot ulcers usually has many components.4,7 A recent multicenter study8 attributed 63 percent of diabetic foot ulcers to the critical triad of peripheral sensory neuropathy, trauma, and deformity. Other factors in ulceration are ischemia, callus formation, and edema. Although infection is rarely implicated in the etiology of diabetic foot ulcers, the ulcers are susceptible to infection once the wound is present. Many of the risk factors for foot ulcer are also predisposing factors for amputation, because ulcers are primary causes leading to amputation.5,7,9 Recognized risk factors for diabetic foot ulceration are listed in Table 1.4
The rightsholder did not grant rights to reproduce this item in electronic media. For the missing item, see the original print version of this publication.
Proper Dressing Infection Control And Offloading
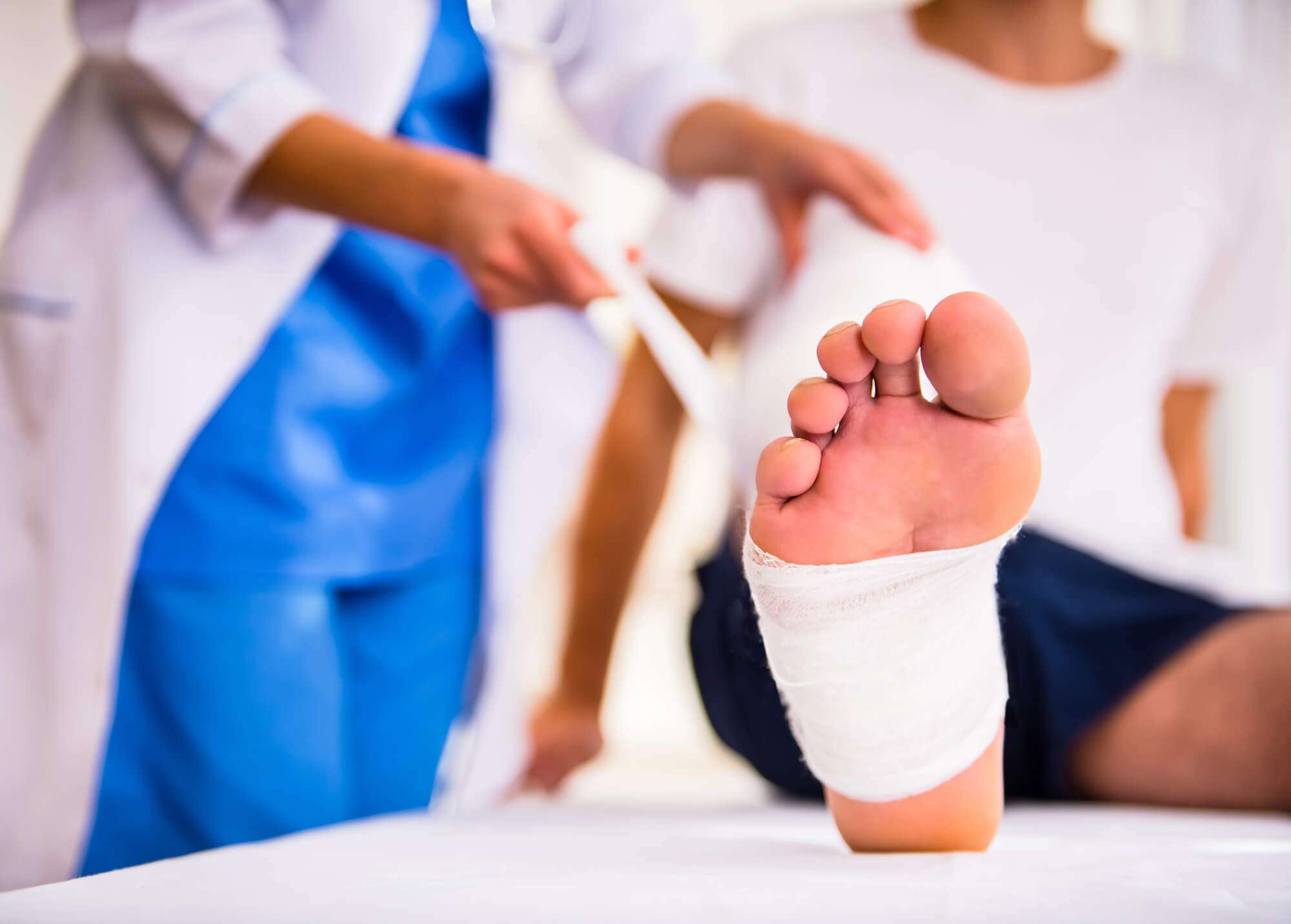
Its essential to use the proper types of wound dressing, infection control, and offloading to prevent your diabetic wound from regressing during or after treatment.
The best wound dressing maintains a healthy amount of moisture on the foot to create a favorable environment for the wound. It must be changed at least once or twice per day, depending on the stage and severity of the ulcer. Wound dressing helps control infection, as do antibiotics.
Offloading is also a very important but often overlooked component of diabetic foot ulcer treatment. When you offload, you remove pressure from your injured foot and give new, healthy cells the opportunity to thrive. Crushes, knee scooters, and wheelchairs all accomplish offloading.
How To Treat Diabetic Foot Ulcers
November 4, 2016 by Admin2
Diabetes is a deadly and life-threatening disease that can bring about unbearable pain and discomforts that are enough to affect the way we live. This includes loss of energy, increased hunger with no appetite, lack of interest and focus, loss of vision, and loss of efficiency for the body to heal wounds. One of the major effects of diabetes is the painful and grotesque wounds that form under your heels. This is called Diabetic foot ulcers and they are serious symptoms of diabetes that can lead to even more complications.
Diabetic foot ulcer is an open wound that occurs under or at the side of your foot and toes. These are painful and can sometimes leak out blood and pus. Diabetic ulcers are formed as a result of changes in the bony shapes of the foot. Other causes are peripheral neuropathy and diseases in the artery. Diabetic foot ulcers can also be caused by wearing tight footwear, rigorous exercises, and getting wounded in the foot.
More than 90% of diabetic patients experience diabetic foot ulcers, and 15% of these patients have been hospitalized due to inflammation and infection. While it is hard to heal diabetic foot ulcers, it is best not to leave them alone for flies and germs to gather around to prevent worsening the condition.
Here are ways you can treat your diabetic foot ulcers:
Which Ointment Is Best For Diabetic Wound
Hydrogen peroxide is used for very small wounds, but it’s more important to prevent infection when treating diabetic wounds. For a closed incision or wound, you would want to cover the entire surface of the skin with dry non-stick dressing and secure it with adhesive tape.
For an open wound or ulcer, it’s important to cleanse using soap and water as well as to irrigate your wound twice per day in order to maintain a sanitary environment. Wet dressings may be recommended after cleaning which may include sterile gauze/adhesive tapes applied so that the material can absorb any fluids from the surrounding area.
Newer products such as hydrocolloid dressings which are able to create a moist healing environment on surfaces by absorbing wound fluid while protecting the area from infection, dirt, and other external contaminants are available over-the-counter at pharmacies or grocery stores.
If you have a non-healing ulcer after six months of treatment, consult your doctor for further help in promoting wound healing. They may prescribe antibiotics to prevent infections.
Here is a list of supplies required when treating sores on diabetics:
- Hydrogen peroxide
- Non-adherent dressings
- Wet non-adherent dressing
- Cotton balls or cotton swabs
- Gauze pads: regular and compression
- Gauze roll bandages/tubular gauzes
- Tape
- Scissors
Here are some ways you can avoid getting cuts or sores on your feet.
How Are Diabetic Feet Diagnosed
To diagnose diabetic foot, a healthcare provider will:
- Ask about your symptoms and how well youre controlling blood glucose.
- Examine your toes, feet and legs.
- Touch the toes, feet and legs with various tools to check whether you have numbness.
If a diabetic ulcer or blister is present, the healthcare provider will likely:
- Examine it for any signs of infection, such as redness, swelling, warmth, discoloration or discharge.
- Order tests to take pictures deeper than the skin, such as X-ray or MRI.
- Take a sample of the skin or discharge to test for infection.
Finding The Best Treatment For A Diabetic Foot Ulcer
Youre probably wondering if a person who has no history of diabetes is likely to have a foot ulcer and the answer is yes, its possible. Its important to contact a health professional no matter your current health condition as you do not want symptoms to get worse.
The Wound Institute of America is ready to accept new patients who want to have professional wound care from the number one wound care center in California. To make an appointment with Wound Institute of America or to learn more about your foot ulcer, call 919-4179. You can also learn more about foot ulcers and other wound care treatments on our website here.
Tea Tree Oil To Fight The Infection
Tea tree oil is rich in antibacterial properties. You can mix the tea tree oil in equal quantity with coconut oil and use it for dressing the diabetic foot ulcer. You can even keep the wound open for some time after applying the tea mixture of tea tree and coconut oil. This home treatment of diabetic foot hastens the process of healing of the wound.
Q: Does Medicare Pay For Diabetic Shoes And Custom Orthotics
A: Medicare will cover diabetic shoes and inserts with some patients.
- Patients must meet and have specific qualifying conditions that must be verified by the Physician managing their diabetes.
- If you have diabetes, you should have an annual foot evaluation performed by a foot doctor or podiatrist to determine if you are eligible for this benefit through Medicare and other insurance carriers.
Arguments Against Primary Amputation
Natural history of disease
The 5-year mortality in patients with diabetes and critical limb ischaemia is 30% and about 50% of patients with diabetic foot infections who have foot amputations die within five years . The mortality rate is similar to some of the most deadly cancers . Poor treatment can lead to lower extremity amputations. About half of these amputations can be prevented by proper care . It is vital that the diabetic condition in patients with infection is urgently controlled, otherwise the vicious cycle of infection leading to the instability of the diabetes and ketosis allows the spread of infection . Patients with a severe infection should be hospitalized immediately as these are often imminently limb-threatening and, in some cases life- threatening . When all or part of a foot has dry gangrene, it may be preferable especially for a patient who is a poor surgical candidate to let the necrotic portions auto-amputate. It may also be best to leave adherent eschar in place, especially on the heel, until it softens enough to be more easily removed, provided that there is no underlying focus of infection . Wet gangrene develops if infection supervenes and this spreads rapidly leading to a severely compromised limb, systemic sepsis and death if there is no intervention . However, the required emergency amputation still carries a high mortality of up to 50% because of severe sepsis and the effects of tissue necrosis .
Assessment and treatment