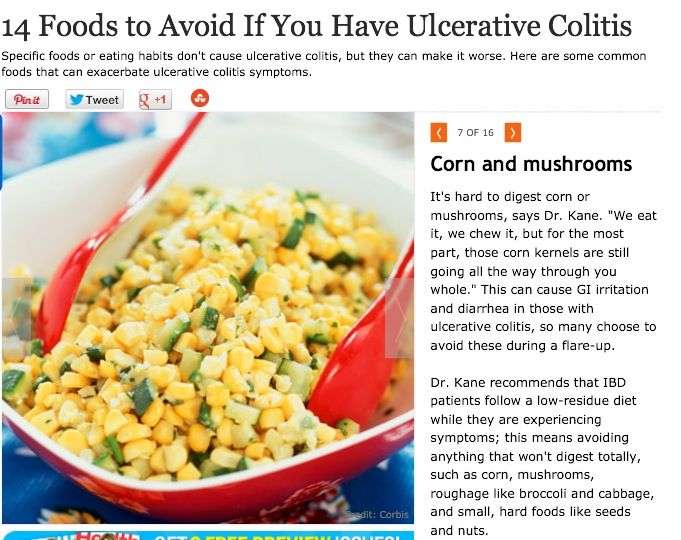
Foods To Avoid During Flares
Diet doesnt cause flares, but your food choices can make symptoms worse if your IBD becomes active.
How foods affect people who are flaring varies from person to person. But here are some of the foods that may worsen symptoms of a flare and cause complications:
- Fatty foods
- Sweets
- Sugary beverages
- Dairy products
- Beverages containing alcohol or caffeine.
- Sugar alcohols used to sweeten in sugar-free foods
- Raw fruits and vegetables
- Beans and lentils
- Whole nuts and seeds
- Whole grain and high-fiber breads and cereals
- Dried fruit
- Fruits with seeds and skins
What Foods Should I Avoid If I Have Ulcerative Colitis
While no single diet has been proven to treat the intestinal inflammation that causes ulcerative colitis, avoiding some foods may help alleviate symptoms during a flare-up. Trigger foods are not the same for everyone, so it is important to track what you eat and identify your own troublesome foods.
Avoid these foods during an ulcerative colitis flare-up, as they can be potential trigger foods:
- Foods high in insoluble fiber: whole grain foods , fruits with skin and seeds, some raw green vegetables, broccoli, cabbage, brussel sprouts, nuts, seeds, beans, lentils and peas
- Dairy products: milk, cream cheese and soft cheeses
- Non-absorbable sugars: sugar alcohols such as sorbitol and mannitol, which are found in sugar-free foods like gum, candy and ice cream
- High-sugar foods: pastries, candy, chocolate and juices
- High-fat foods: butter, margarine and cream, as well as greasy foods such as pizza and fried foods
- Alcoholic and caffeinated beverages: beer, wine, liquor, soda and coffee. Elimination of alcohol may not be required, but it should be consumed in moderation.
- Spicy foods
Diet Recommendations For Ulcerative Colitis Flare
- Follow a low residue diet to relieve abdominal pain and diarrhea.
- Avoid foods that may increase stool output such as fresh fruits and vegetables, prunes and caffeinated beverages.
- Try incorporating more omega-3 fatty acids in your diet. These fats may have an anti-inflammatory effect. They are found in fish, including salmon, mackerel, herring and sardines.
- Patients often find that smaller, more frequent meals are better tolerated. This eating pattern can help increase the amount of nutrition you receive in a day.
- Consider taking nutritional supplements if appetite is poor and solid foods are not tolerated well .
Don’t Miss: How Do Stomach Ulcers Heal
Foods To Eat With Ulcerative Colitis
Understanding inflammatory bowel diseases like ulcerative colitis can be difficult, especially knowing what foods to eat. An ulcerative colitis flare can be exacerbated when eating inflammatory foods. Likewise, one can easily become nutrient deficient if there is a lack of variety in the diet. Here we look into some recommended foods to eat when you have an ulcerative colitis flare.
Your nutrition affects your overall health and well-being. When you do not get the proper nutrients, you can experience ulcerative colitis complications like weight loss, malnutrition, and nutritional deficiencies. Before we dive into the foods that you should eat, here are a few tips that can help improve your health and reduce the frequency of flare ups.
What Side Effects Of Ibd Can Cause Malnutrition

There are several reasons why people with IBD may be at risk for malnutrition. The following list includes some side effects that contribute to malnutrition.
- Inadequate food/fluid intake may by caused by nausea, abdominal pain, loss of appetite or altered taste sensation
- Increased losses â intestinal inflammation during acute flares results in increased protein losses, losses from fistula fluids, diarrhea and bleeding
- Increased nutritional needs â inflammation or infection increases metabolic requirements
- Malabsorption with Crohn’s disease may be caused by severe intestinal inflammation, resection of small intestine and medications, such as prednisone and sulfasalazine
Read Also: Surgical Management Of Ulcerative Colitis Ppt
Nutrition Tips For Inflammatory Bowel Disease
Inflammatory Bowel Disease is a term used for two specific and separate diseases: Crohn’s disease and ulcerative colitis. Nutritional recommendations are different for each disease and for each individual patient. It is important to discuss the treatments that are right for you with a registered dietitian and with your doctor.
What About Fodmap Foods
You also may have heard of something called the low-FODMAP diet . FODMAPs are carbohydrates that are poorly absorbed by the small intestine and when they land in the colon where the colonic bacteria ferment the undigested sugars resulting in gas production. Some research shows that following this diet can help reduce symptoms in people with UC. According to researchers at Monash University in Australia:
High FODMAP foods include:
Also Check: Does Stomach Ulcer Cause Pain
Can Certain Foods Really Cause Inflammation
The link between what we eat and chronic inflammation in the body isnt fully understood. What is known is that there does seem to be some connection.
Lets jump into the science: The liver produces something called C-reactive protein as a response to inflammation in the body. In short, higher levels of CRP mean more inflammation, and certain foods have been shown to increase levels of CRP in the blood.
Now, the specifics of what foods cause this increase is somewhat up for debate, but its possible that things like processed sugar can trigger the release of inflammatory messengerslike CRPa sign that they may potentially be contributing to an inflammatory state.
On the other hand, foods like fruits and vegetables may help fight oxidative stress, which is a trigger for inflammation. Certain diets, like the Mediterranean diet, already include many foods that are considered to be anti-inflammatory such as whole grains, legumes, a rainbow assortment of fruits and vegetables, and fish.
More Information About Ulcerative Colitis
According to George Washington University, colitis is a chronic digestive disease characterized by inflammation of the inner lining of the colon. Infection, loss of blood supply in the colon, Inflammatory Bowel Disease and invasion of the colon wall with collagen or lymphocytic white blood cells are all possible causes of an inflamed colon.
The following diseases fall into the colitis/IBD category they all can be treated with a combination of medication and improvements to your eating habits:
Also Check: Budesonide Vs Prednisone For Ulcerative Colitis
Dietary Habits Of Uc Cases And Controls
No significant difference was observed between cases and controls in terms of dietary habits including regular meal pattern, chewing efficiency, fluid consumption during meals, fried foods intake, and fatty meals intake. This was also the case when we compared the distribution of subjects in terms of above-mentioned variables across quartiles of IPD score .
Table 2. Distribution of patients with ulcerative colitis and controls in terms of dietary habits across quartiles of inflammatory potential of the diet score.
What Are Some High
Whole-grain breads, cereals, and pasta, whole vegetables and vegetable sauces, whole fruits, including canned fruits, yogurt, pudding, ice cream, or cream-based soups with nuts or pieces of fruits or vegetables, tough or coarse meats with gristle and luncheon meats or cheese with seeds, peanut butter, salad dressings with seeds or pieces of fruits or vegetables, seeds or nuts, coconut, jam, marmalade.
Read Also: Can You Donate Blood If You Have Ulcerative Colitis
What About Vitamins And Minerals
It is a good idea for all people with IBD to take a standard multivitamin every day. People with IBD who are doing well do not need any extra vitamins or minerals. If you have Crohn’s disease is in the ileum or the ileum has been removed you may need to take B12, calcium, or vitamin D. You may need iron supplements if you have blood loss during inflammation or reduced iron absorption as a result of inflammation. Diarrhea or vomiting can cause loss of potassium and magnesium. If you are lactose intolerant and avoid dairy products, this can lead to low calcium. Ask your doctor if you need to be tested for any of the above.
Faecal Butyrate: Key Metabolite In Uc
Short chain fatty acids, including butyrate, proprionate, and lactate, are generated in the colon as result of bacterial fermentation of dietary fibre by luminal bacteria such as Bifidobacterium, Eubacterium, and Lactobacillus species. Roediger et al demonstrated significant inhibition of butyrate but not glucose oxidation by hydrogen sulphide in the ascending colon, splenic flexure, and in the rectosigmoid region. A direct anti-inflammatory effect for butyrate, the most extensively studied of the short chain fatty acids, may be attributable to its inhibition of nuclear factor B, thus preventing the transcription of proinflammatory cytokines. In this study, butyrate also attenuated dextran sulphate sodium induced colitis. Furthermore, butyrate has been demonstrated to reduce colonic permeability by enhancing peroxisome proliferator activated receptor activation. This is of special interest as PPAR- ligands show antineoplastic and anti-inflammatory effects in experimental colitis.
Patients with active extensive UC have decreased colonic butyrate oxidation. As remission of disease is associated with normalisation of butyrate oxidation, UC mucosa is not intrinsically altered in butyrate oxidation. Butyrate enemas have been shown to be of benefit in the management of distal UC.
Also Check: Natural Supplements For Ulcerative Colitis
General Guidelines When Ulcerative Colitis Is In Remission
Some members of MyCrohnsAndColitisTeam find they can eat a wider variety of foods safely during remission periods when ulcerative colitis is not as active and symptoms are absent or mild. Still, every individual is different, and purportedly beneficial foods may trigger symptoms. Trial and tracking is the only way to know for sure.
If it is safe for you, these guidelines may help you stay your healthiest during remission:
- Get 25 grams to 35 grams of fiber per day to promote bowel regularity and reduce inflammation.
- Consume plenty of lean meats, which are a good source of B vitamins. Include fatty fish, tofu, and nut and seed butters.
- Include probiotic foods such as yogurt, tempeh, kefir, kimchi, miso, and sauerkraut.
While some members find kefir too sour for their liking, others report experiencing benefits from trying the fermented drink. Kefir has been helping me over the past week, wrote one. Been trying kefir the past few days. Will keep you posted. So far less pain, said another.
What Foods Should You Eat With Ulcerative Colitis
If you have Ulcerative Colitis, very minor changes to what you eat can make a BIG difference in your symptoms. Consider keeping food logs or adjusting foods that trigger your symptoms. You may also want to work with your doctor or dietitian to work through an elimination diet. Generally, you should try to:
In terms of specific food recommendations, go with these:
| Food Type |
|---|
Recommended Reading: How Effective Is Humira For Ulcerative Colitis
Best Foods To Eat During An Ulcerative Colitis Flare
HomeUlcerative Colitis7 Best foods to eat during an ulcerative colitis flare-ups
Ulcerative colitis is a long-lasting condition that causes inflammation and ulcers in your digestive tract. It usually affects the innermost lining of your large intestine and the rectum. Symptoms of ulcerative colitis develop over time, rather than all of sudden.
The food you eat has a great impact on the severity of your Ulcerative colitis symptoms. If you have ulcerative colitis, you may already identify various foods as triggers. But figuring out what foods to eat is also equally important as the right foods will provide you key nutrients without irritating your digestive tract.
Faq: Dietary Management Of Ibd
Information regarding dietary treatments for IBD is often confusing. Many people receive information telling them to avoid entire food groups or specific foods. However, there is no need to avoid foods unless they worsen your symptoms. It is best to restrict as few foods as possible to increase the chances that you are getting a balanced, nutritious diet. This is important for maintaining the function of your digestive tract and your overall health.
Don’t Miss: Diet For Gerd And Ulcers
What To Eat With Colitis
Colitis or Inflammatory Bowel Disease is a common disease which can result in discomfort for most of its patients, who experience symptoms such as diarrhea, abdominal pain, flatulence or dehydration. Diet is an essential factor in treating colitis. Not only can it help us to recover but it also means we can avoid having to deal with any of its symptoms. For this reason, at OneHowTo we explain what to eat with colitis.
There are several types of colitis which vary in causes and duration. However in all cases, aside from regular medication, your diet is critical. The types of colitis include:
- Ulcerative colitis causes ulcers in the colon and rectum and may also affect the intestines.
- Infectious colitis is caused an infection and is usually temporary.
- Amoebic colitis is caused by an amoeba parasitic infection.
- Colitis cystica profunda causes polyps to appear on the lower part of the colon.
- Pseudomembranous colitis occurs when the large intestine is infected with clostridium difficile bacteria and it spreads to the colon.
- Ischemic colitis is due to blockage in a colon artery stopping the area from getting enough oxygen.
- Idiopathic colitis has no known causes.
To avoid diarrhea, abdominal pain, flatulence and general discomfort, we have to watch what we eat. As for protein and dairy, for a colitis diet we must:
Did My Diet Cause Ibd
No. IBD seems to be caused by a mix of genes and things that damage the lining of the intestine. Together, these cause the immune system in the intestine to be exposed to the bacteria of the intestine more than usual. Inflammation in the intestine of a healthy person lasts for a short time, and then goes away. In people with IBD, the inflammation does not go away, and it stays inflamed.
Recommended Reading: Align Probiotic For Ulcerative Colitis
Herbal Remedies And Supplements
There are lots of supplements that claim to treat Crohns and Colitis. But there isnt enough evidence to recommend any herbal remedies or supplements. This is because its difficult to know whether the supplement is directly affecting a persons Crohns or Colitis or whether something else is causing a change in symptoms. Also, everyone is different so what helps one person may not help another.Some people find that some herbal remedies, such as aloe vera or curcumin , help them manage their symptoms when they use them together with their prescribed medicines. There have been reports of cannabidiol , an ingredient in cannabis, helping with symptoms like diarrhoea, pain and loss of appetite. But we dont know enough about how it works or how much is a safe amount to take. It isnt currently recommended and isnt available on prescription for people with Crohns or Colitis.There have been claims in the media about the benefits of kefir a fermented milk drink that contains probiotics. But there isnt any medical evidence to show that it helps people with Crohns or Colitis.If you want to take herbal remedies, its important to speak to your IBD team or dietitian first. Dont stop taking your prescribed medicine without talking to your IBD team, even if your symptoms improve.
I think it is so important to remember that the relationship with food and IBD is so different for everyone!
Tom
What Is An Ulcerative Colitis Diet
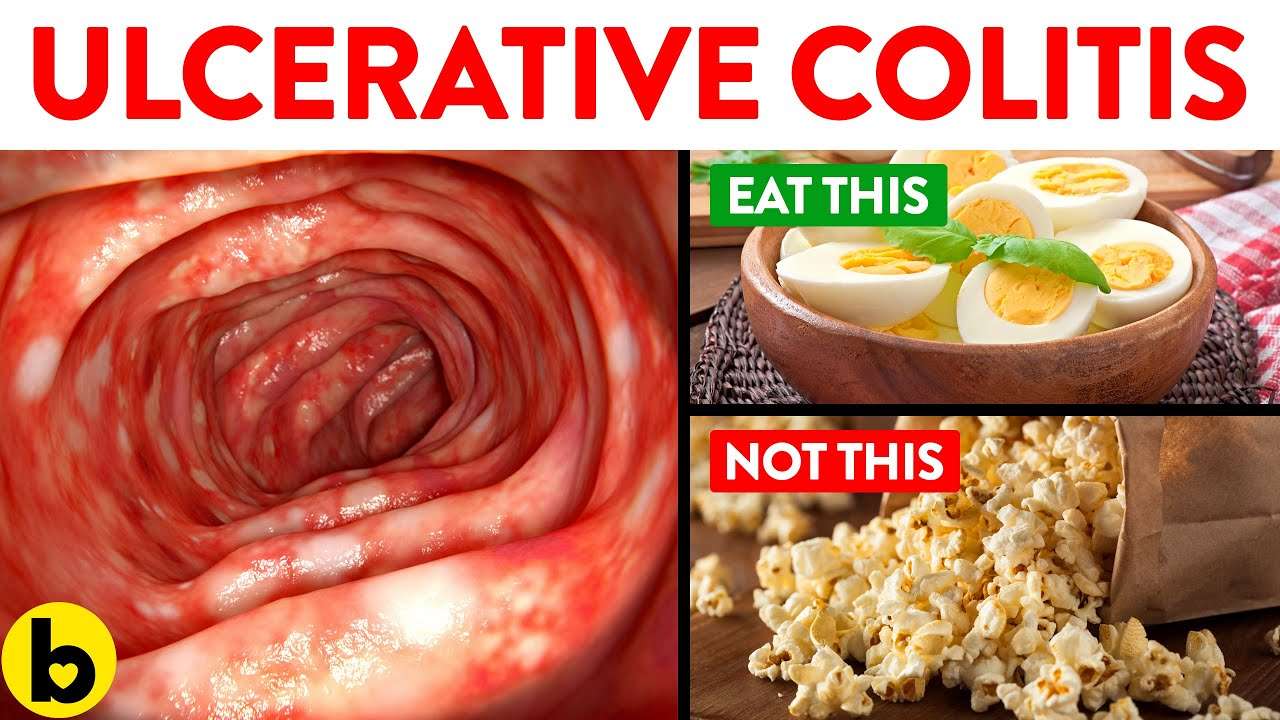
A person with ulcerative colitis may find they need to modify their diet to help manage their symptoms. There is not a single diet or meal plan that fits everyone with ulcerative colitis, and diets are individualized for each patient. Depending on symptoms different types of diets may be recommended, such as:
- A high-calorie diet: Many people with ulcerative colitis lose weight and can develop signs of malnutrition. A high calorie diet may prevent these problems.
- A lactose-free diet: People with ulcerative colitis may also have lactose intolerance.
- A low-fat diet: Ulcerative colitis may interfere with fat absorption and eating fatty foods may trigger symptoms. This is often recommended during an ulcerative colitis flare.
- A low-fiber diet : This can help reduce the frequency of bowel movements and abdominal cramps.
- A low-salt diet: This diet is used when patients are on corticosteroid therapy to help reduce water retention.
- A low FODMAP diet: FODMAPstands for Fermentable Oligo-Di-Monosaccha-rides and Polyols, which are types of sugars found in certain carbohydrates and sugar alcohols. This diet is used in people who have intolerance to FODMAPS.
- A gluten-free diet: People with ulcerative colitis may also be sensitive to gluten.
You May Like: Can Stomach Ulcer Cause Fever
Ulcerative Colitis: Let’s Talk
Colitis, Ulcerative Colitis, and Crohn’s are often used interchangeably – but in reality, they explain three different conditions. Colitis is the general inflammation of large intestine lining . It is synonymous with Irritable Bowel Disease and encompasses multiple conditions. Ulcerative Colitis: is a specific digestive issue, identified by ulcers on your large intestine.
Which Nutrients Are Important In Crohn’s And Colitis
Vitamins and mineralsYour body needs vitamins and minerals to work and stay healthy. Your Crohns or Colitis may stop you absorbing enough vitamins and minerals from your food. Vitamins and minerals that you may not absorb properly include iron, vitamin B12, vitamin D and calcium.Eating a healthy, balanced diet may help improve the level of vitamins and minerals in your body. If blood tests show you have low levels of vitamins and minerals, your doctor or specialist nurse may recommend you take supplements to restore your vitamin and mineral levels.Speak to your doctor, specialist nurse or dietitian if you think you may have low levels of any of these nutrients.
IronHaving low levels of iron is common in people with Crohns or Colitis. Possible causes include a lack of iron in the diet, blood loss and problems absorbing iron from food. Lack of iron can lead to anaemia, where there are fewer red blood cells to carry oxygen around the body.Common symptoms of anaemia include:
- feeling tired and lacking in energy
- feeling short of breath
- fast or irregular heartbeat
- pale skin.
Its important to speak to a dietitian before cutting down on fibre so you dont miss out on the health benefits. For example, they may suggest that some people cut down on fibre for a short time during a flare-up, before slowly adding it back in to the diet.Fibre-rich foods include:
- wind
- stomach rumbling and pain
- diarrhoea loose and runny stools.
- sipping a cold drink
Read Also: What Medicine Is Good For Ulcers