Compression Versus No Compression/usual Care/simple Dressings
Various guidelines have recommended that some compression is better than no compression . A Cochrane review in 2009 compared compression with either primary dressing, noncompressive bandages and usual care that always did not include compression and concluded that venous ulcers healed faster with compression and some form of compression is better than no compression in healing VLU.
How The Intervention Might Work
Generally, compression therapy is thought to work by applying an external pressure to the leg which assists venous return and reduces venous reflux . Partsch has suggested that compression:
reduces oedema by reducing capillary filtration, moving fluid from compressed tissues to noncompressed tissues and improving lymphatic drainage and
reduces the pressure in the veins by increasing venous blood flow and reducing venous pooling .
The use of compression to treat venous leg ulcers is not without risk. Whilst Mosti has suggested that compression may increase arterial inflow , if the applied pressure exceeds the local arterial perfusion pressure then arterial inflow will be reduced, which risks ischaemia.
National clinical guidelines in the UK and USA recommend that all patients presenting with a leg ulcer be screened for arterial disease using Doppleraided measurement of the ABPI . Clinically significant arterial disease is often defined as an ABPI of below 0.8. Patients with venous leg ulceration who have an ABPI of between 0.5 and 0.8 may be eligible to receive modified compression .
Limitations Of The Study
To this moment we were unable to present long term results – longer observation than two months . Although study outcomes were consistent in each treatment group, the absence of blinding and use of placebo are a limitation of this study that may affect the generalization of the findings. In future we would like to provide quasi – compression therapy in control groups and present complete results. We did not use intention-to-treat analysis either.
Read Also: What Are Some Symptoms Of An Ulcer
Compression Therapy In The Treatment Of Venous Leg Ulcer
03 September, 2002
VOL: 98, ISSUE: 36, PAGE NO: 39
Michael Stacey, University of Western Australia, Fremantle
Vincent Falanga, Boston University, USA William Marston, University of North Carolina, USA Christine Moffat, Thames Valley University, London Tania Phillips, Boston University School of Medicine, USA R. Gary Sibbald, University of Toronto, Canada Wolfgang Vanscheidt, Universitèts-Hautklinik, Freiburg, Germany Christina Lindholm, Karolinska Hospital, Stockholm, Sweden
The appropriate management of venous leg ulcers is a continuing challenge for health care professionals, despite the publication of numerous useful management guidelines and systematic reviews . Approximately 1-2% of the general population suffer from a poorly healing ulcer of the lower extremity in their lifetime .
More effective management strategies are required which are based on the results of randomised controlled trials , improved organisational structures and multidisciplinary cooperation. It is also vital that any evidence-based recommendations are widely disseminated and easily implemented to maximise benefits to patients.
What Is The Best Treatment For Venous Stasis Ulcers

Evidence-based treatment options for venous ulcers include leg elevation, compression therapy, dressings, pentoxifylline, and aspirin therapy. Surgical management may be considered for ulcers that are large in size, of prolonged duration, or refractory to conservative measures.
Why are venous ulcers so painful?
The associated symptoms of a venous leg ulcer are caused by blood not flowing properly through your veins. This is known as venous insufficiency, and can cause: leg pain, which can be continuous or may come and go. varicose eczema
You May Like: Indian Diet For Ulcerative Colitis
Why It Is Important To Do This Review
Venous leg ulcers have a large impact on peoples lives and incur high costs to health services and compression therapy is currently the first line treatment. Since the publication of the original Cochrane Review of compression bandages and stockings for venous leg ulcers , the number of relevant randomised controlled trials has more than doubled the range of compression modalities has increased and the classification of compression modalities has been refined. In order to offer uptodate evidence for decision makers, we have decided to update the previous version of this review, , and to split it into separate reviews of different compression modalities. We will then bring the results together into an overview, which will incorporate a network metaanalysis , in order to rank the different treatments on their individual probabilities of being the most effective compression modalities for healing venous leg ulcers. This particular review provides evidence about the comparison of compression bandages or stockings versus no compression.
Compression Therapy For Venous Leg Ulcers
Benefits of Wearing Stockings
- Provides symptomaticrelief of swelling and pain
- Encourages a healthierand more efficient bloodflow
- Heals venous wounds
- Keeps wounds safe from infection
Compression therapy for venous leg ulcers and varicose veins refer to prescription snug-fitting material stockings. Much more advanced than a bandage, they are designed for the purpose of reducing reflux, increasing the blood flow of an individual and pushing the veins blood back upward through the vein capillaries. In doing this, the patient can relieve symptoms from vein disease such as edema or even prevent deep vein thrombosis.
Your insurance company may requestcompression stockings to be used for treating your varicose veins and venous ulcers as the first line of actionprior to the authorization of coverage for medical treatment. Therefore, youare advised to schedule a consultation with our specialist at a vein clinicnearest to you to find out whether compression therapy for leg ulcers and varicose veins is right for you along with whatsize compression stockings you need.
Consult with our vein specialist to find out if this is the right treatment for you.
Recommended Reading: How Do You Know If You Have Ulcerative Colitis
Stage : Identifying The Research Question
In the review, we aim to answer the following research questions:
What kinds of adjunct PA/exercise interventions have been used to affect VLU healing and recurrence?
What methods have been used to evaluate the key outcomes of interest regarding PA/exercise interventions applied for people with VLU?
What is the effect of PA/exercise interventions on patient/clinical outcomes ?
Single Component Versus Multicomponent Bandage Systems And Single Layer Versus Multilayer
Studies have emphasized the fact that multi-layering increases stiffness of bandages and increases sub bandage pressure , thereby being inelastic practically. It ensures even distribution of SBP . SBP of 30-40 mm Hg is recommended for healing of VLU . Multicomponent multilayered compression is superior to a single component, single layer compression bandage systems.
Recommended Reading: Stage 2 Pressure Ulcer Treatment Dressing
Medical And Surgical Treatment
A number of adjunctive medical therapies are currently in use without unequivocal support in the literature, but discussion of these is beyond the scope of this article. There is also increasing realisation that chronic wounds, such as venous ulcers, benefit from an overall approach aimed at optimising the wound bed. This approach, termed wound bed preparation, includes a number of aspects critical to wound care, such as elimination of excessive exudate and bacterial burden, debridement and elimination of necrotic tissue, angiogenesis and the formation of a wound matrix that promotes re-epithelialisation.
There is also emerging evidence that skin substitutes may be beneficial in the treatment of hard-to-heal venous leg ulcers when used in conjunction with multi-layer compression bandaging . Other biological agents, such as growth factors and protease inhibitors, are currently being evaluated for their efficacy in the management of venous leg ulcers.
Many patients with leg ulcers suffer pain that can adversely affect their quality of life and may influence speed of healing. Reduced compression should be used until pain and oedema resolves, then high-compression bandaging can be introduced. In most cases, appropriate dressings or oral analgesics can effectively manage pain, although skin grafting may be required in cases of intractable pain.
Deep Vein Thrombosis Prophylaxis
The role of mechanical devices graduated compression stockings and intermittent pneumatic compression is dependent on the risk of venous thromboembolism in the medical or surgical patient. They may be used in combination with drug therapy or alone, especially if drugs are contraindicated because of an unacceptable bleeding risk. These mechanical devices are contraindicated in patients with severe peripheral vascular disease, severe leg deformity and severe peripheral neuropathy.
Evidence supports the use of graduated compression stockings as thromboprophylaxis for abdominal, cardiac, thoracic, vascular, major general or gynaecological surgery, neurosurgery and total hip replacement. Similarly, there is evidence for the use of intermittent pneumatic compression for total hip replacement, hip fracture surgery, total knee replacement, vascular, cardiothoracic surgery, neurosurgery, and for major gynaecological surgery. Graduated compression stockings should be measured for the individual and worn for as long as possible until the patient is fully mobile.20
Recommended Reading: Ulcer On Eye From Contact Lens
An Urgent Need To Improve Leg Ulcer Management
The expert working committee responsible for the EWMA document highlight this need, drawing attention to the variation in the quality of services offered to people with VLUs, despite the abundance of literature, as well as variations in the evidence and contradictory recommendations . Globally, education and training for healthcare professionals is crucial, they say, with the incorporation of Clinical Practice Guidelines in professional training and the expansion of guidelines to incorporate detailed educational and competency skills, in the clinical environment with senior management support as a strategy for putting evidence into practice.
We must hope that they succeed in their aim of keeping VLU management on the agenda as an international health priority, and that better primary research is being conducted so that new and updated Cochrane Reviews will be able to provide reliable evidence to inform practice.
*Since this article was published, there has been a new Cochrane Review published on subfascial endoscopic perforator surgery for treating venous leg ulcers, which concludes that its role remains uncertain.
Join in the conversation on Twitter with and @CochraneWounds or leave a comment on the blog.
References may be found here.
Sarah Chapman has nothing to disclose.
Description Of The Condition
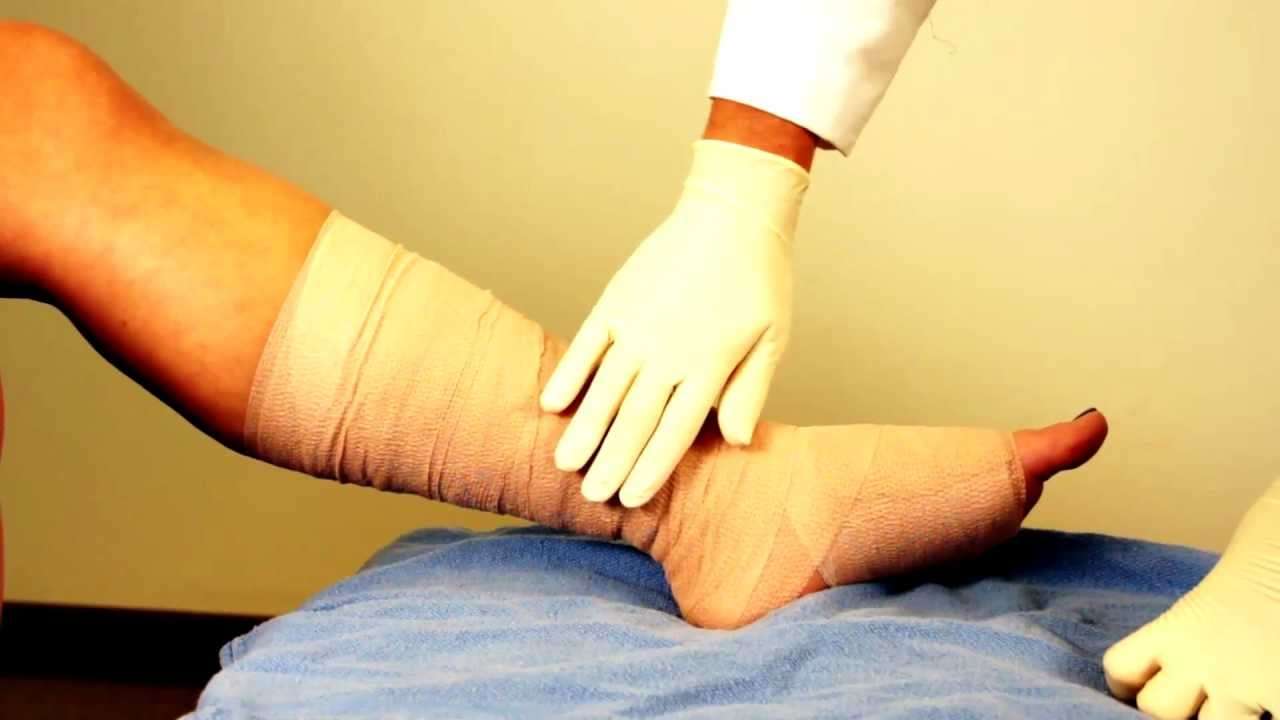
Leg ulcers are open skin wounds on the lower leg that can last weeks, months or even years. They occur as a consequence of arterial or venous insufficiency, or both. Less frequently, chronic leg ulceration may occur due to some other disease, such as rheumatoid disease or rarer conditions . Most leg ulcers are the result of venous disease , where blood flow in the veins can be impaired by vein damage, obstruction and calf muscle pump failure . These problems mean that blood no longer returns efficiently from the legs to the heart and the pressure within the veins rises . The precise chain of events that links high venous pressures with skin breakdown and subsequent chronic wounds is not fully understood.
Leg ulcers of mixed aetiology usually involve a combination of venous and arterial disease. Open skin ulceration that is due solely to limb ischaemia is less common.
The making of a differential diagnosis of the underlying aetiology of a specific leg ulcer is made by taking a clinical history, physical examination, laboratory tests and other assessments . Typically, the latter includes an assessment of the arterial blood supply to the leg using the anklebrachial pressure index , measured using a handheld Doppler ultrasound scanner.
Don’t Miss: Ulcers In Small Bowel Crohn’s
After The Ulcer Has Healed
Once you have had a venous leg ulcer, another ulcer could develop within months or years.
The most effective method of preventing this is to wear compression stockings at all times when you’re out of bed.
Your nurse will help you find a stocking that fits correctly and you can manage yourself.
Various accessories are available to help you put them on and take them off.
Page last reviewed: 11 January 2019 Next review due: 11 January 2022
Diagnosis And Treatment Of Venous Ulcers
LAUREN COLLINS, MD, and SAMINA SERAJ, MD, Thomas Jefferson University Hospital, Philadelphia, Pennslyvania
Am Fam Physician. 2010 Apr 15 81:989-996.
Patient information: See related handout on venous ulcers, written by the authors of this article.
Venous ulcers, or stasis ulcers, account for 80 percent of lower extremity ulcerations.1 Less common etiologies for lower extremity ulcerations include arterial insufficiency prolonged pressure diabetic neuropathy and systemic illness such as rheumatoid arthritis, vasculitis, osteomyelitis, and skin malignancy.2 The overall prevalence of venous ulcers in the United States is approximately 1 percent.1 Venous ulcers are more common in women and older persons.36 The primary risk factors are older age, obesity, previous leg injuries, deep venous thrombosis, and phlebitis.7
Venous ulcers are often recurrent, and open ulcers can persist from weeks to many years.810 Severe complications include cellulitis, osteomyelitis, and malignant change.3 Although the overall prevalence is relatively low, the refractory nature of these ulcers increase the risk of morbidity and mortality, and have a significant impact on patient quality of life.11,12 The financial burden of venous ulcers is estimated to be $2 billion per year in the United States.13,14
Don’t Miss: Blood Clots In Stool With Ulcerative Colitis
A Systematic Review Of Compression Treatment For Venous Leg Ulcers
- Accepted 14 August 1997
Stage : Identifying Relevant Studies
As suggested by the JBI , the search strategy for the review will follow a three-step search to identify both published and unpublished studies. First, an initial search of MEDLINE via OVID will be conducted, followed by an analysis of the keywords contained in the title and abstracts, as well as the subject headings used to describe the study. We will then use all identified keywords and subject headings to undertake search across all included databases. Last, the bibliographies of all identified studies, especially systematic reviews and literature reviews, will be screened for additional studies not identified through electronic database search.
Database search terms will be developed by the research team in conjunction with an experienced research librarian using a combination of keywords and controlled vocabulary . Electronic database searching will be conducted in Medline, CINAHL and The Cochrane Central from inception to present day, with English language being the only limitation applicable. We will also search ICTRP WHO, ClinicalTrials.gov. and Australian New Zealand Clinical Trials Registry for ongoing clinical trials. Grey literature will be retrieved through hand searching the first five pages of google scholar, and the reference list of relevant studies will also be screened for any unpublished studies. A copy of the preliminary search terms and search strategy for Medline is available in Appendix 1.
Also Check: What Happens In Ulcerative Colitis
Dressings And Topical Agents
Dressings are usually applied to open ulcers. As well as offering protection, dressings may be chosen for other reasons, such as antimicrobial properties or absorption of exudate. As well as a wide range of types of dressings available, there are a number of topical products, used to reduce infection risk, aid exudate absorption or promote wound healing by other means, as well as topical painkilling agents. Having reliable evidence to guide choices is important, and not only for healthcare professionals. Patients responding to Cochrane Wounds online open consultation on research priorities, conducted between May and November 2016, asked in particular for evidence relating to specific dressings.
There are high quality, recent evidence syntheses, including a number of Cochrane Reviews, on particular dressing types and topical agents, but the evidence is low quality and does not provide robust support for any specific dressing or treatment. What is needed is a network meta-analysis , a simultaneous comparison of linked, multiple, competing treatments in a single statistical regression model. This is being done in a new Cochrane Review for the outcome of venous leg ulcer healing, for alternative dressings and topical agents .
Compression Therapy For Venous Leg Ulcers: Risk Factors For Adverse Events And Complications Contraindications A Review Of Present Guidelines
Radboud UMC, Nijmegen & Andriessen Consultants, Malden, The Netherlands
International Compression Club , Berndorf, Austria
Department of Angiology, Clinica MD Barbantini, Lucca, Italy
International Compression Club , Berndorf, Austria
Medical University Vienna, Vienna, Austria
International Compression Club , Berndorf, Austria
Medical & Regulatory Affairs, Lohmann & Rauscher GmbH & Co KG, Rengsdorf, Germany
Patient Outcome Group , European Wound Management Association , Frederiksberg, Denmark
International Compression Club , Berndorf, Austria
Radboud UMC, Nijmegen & Andriessen Consultants, Malden, The Netherlands
International Compression Club , Berndorf, Austria
Department of Angiology, Clinica MD Barbantini, Lucca, Italy
International Compression Club , Berndorf, Austria
Medical University Vienna, Vienna, Austria
International Compression Club , Berndorf, Austria
Medical & Regulatory Affairs, Lohmann & Rauscher GmbH & Co KG, Rengsdorf, Germany
Patient Outcome Group , European Wound Management Association , Frederiksberg, Denmark
International Compression Club , Berndorf, Austria
Read Also: What To Do When Ulcerative Colitis Flares
Compression Bandages Or Stockings Versus No Compression For Treating Venous Leg Ulcers
Key messages
Compared with not using compression, compression therapy that uses bandages or stockings to treat venous leg ulcers:
– probably heals venous leg ulcers more quickly
– probably increases the number of people whose ulcer has completely healed after 12 months
– probably reduces pain and
– may improve some aspects of peoples quality of life.
However, there is still uncertainty about whether or not compression therapy causes unwanted side effects, and if the health benefits of using compression outweigh its cost.
What are leg ulcers?
Leg ulcers are open skin wounds on the lower leg that can last weeks, months or even years. Most leg ulcers are caused by venous diseases that affect the circulation of blood in leg veins. Venous leg ulcers can cause distress and pain to patients, and can be very costly to the health service.
What did we want to find out?
Standard treatment options for venous leg ulcers often include compression therapy. This involves applying external pressure around the lower leg to help the return of blood from the legs to the heart. Compression therapy uses bandages, stockings or other devices.
We wanted to find out if compression therapy delivered by bandages and stockings compared with no compression:
– heals venous leg ulcers
– improves peoples quality of life
– has health benefits that outweigh the costs and
– reduces pain.
What did we do?
What did we find?
Venous leg-ulcer healing and unwanted effects
Other effects
Primary outcomes