Quality Of The Evidence
We have explored the application of a new approach to GRADE analysis, alongside NMA in STATA . We applied the GRADE approach separately to effect estimates for different contrasts and to the ranking of interventions, but the two aspects are closely interrelated and, in this review, are a consequence of the sparse network and the high risk of bias through much of the network. The effect estimates were exemplified by contrasts of interventions versus saline gauze.
Across the network as a whole, the evidence was of very low certainty. There was overall high risk of bias and overlap of the ranking probability distributions, and no clearcut results. The evidence was of such poor quality that we consider it inappropriate to focus on which treatments had the highest probabilities of healing .
What Are The 4 Stages Of Pressure Ulcers
You might hear medical staff refer to pressure ulcers in stages. Stage 1 is less severe, while an ulcer can progressively increase in severity to stage 4.
The 4 stages of pressure ulcers are:
|
Stage 1 |
The skin is red, but not broken. When you press the skin, it does not turn white. |
|
|
Stage 2 |
There is some damage to the outer layer of skin. The pressure ulcer looks like a shallow, open wound with a redish-pink centre. It can also look like a blister that may or may not have opened. |
|
|
Stage 3 |
There is full loss or damage of the skin. The wound looks quite deep but is still limited to the skin layers. |
|
|
Stage 4 |
There is full loss or damage of the skin it is deep and goes all the way to the underlying bone, tendon or muscle. |
Dressings For Venous Leg Ulcers
Also Check: Bland Diet Recipes For Ulcers
Silicone Adhesive Multilayer Foam Dressings To Prevent Pressure Ulcer
| The safety and scientific validity of this study is the responsibility of the study sponsor and investigators. Listing a study does not mean it has been evaluated by the U.S. Federal Government. Read our disclaimer for details. |
| First Posted : February 22, 2018Results First Posted : April 26, 2021Last Update Posted : April 26, 2021 |
- Study Details
The objective of this study is to determine if silicone adhesive multilayer foam dressings applied to the sacrum, heels and greater trochanter in addition to standard prevention reduce pressure ulcer incidence category II, III, IV, Unstageable and Deep Tissue Injury compared to standard pressure ulcer prevention alone, in at risk hospitalised patients. In particular, this trial extends previous trial results obtained in ICU setting. Therefore, only a maximum of 25% of patients will be recruited from ICU settings.
Contributions Of Editorial Base:
Nicky Cullum: edited the protocol advised on methodology, interpretation and protocol content. Approved the final protocol prior to submission. Sally BellSyer: coordinated the editorial process. Advised on methodology, interpretation and content. Edited the protocol. Ruth Foxlee: designed the search strategy and edited the search methods section.
Read Also: How To Determine Stomach Ulcer
What Is A Foam Dressing
Wound dressings can accelerate the healing process by protecting the injury or wound from bacteria and creating an environment which supports healthy healing. Foam dressings are an effective tool for moist wound healing and are particularly useful in preventing dressing-related trauma, managing exuding wounds, and minimizing dressing discomfort and pain.
Read Also: Home Remedies For Skin Ulcers
Wound Care Best Practices And The Evolving Role Of Gauze Dressings
Modern dressings are generally non-adherent and ensure appropriate healing through maintaining a moist wound healing environment and maximizing patient comfort.5 Implementing advanced dressings and alternative debridement methods as best practices for wound care will help clinicians maintain a moist healing environment.Impregnated gauze, such as gauze containing substances such as petroleum, honey, hydrogel, iodine, bismuth, and zinc, can decrease trauma and prevent desiccation during dressing changes. It can also decrease moisture loss from the wound, thereby preventing local cooling and its adverse effects.3 It has also been demonstrated that the use of advanced dressings can be more cost-effective than the use of gauze because of the massive decrease in clinician time required for the application of the dressings, even though gauze is generally a far less expensive material.2 When selecting the optimal wound dressing, it should6:
- Maintain a moist wound healing environment.
- Facilitate gas exchange.
- Protect the wound from further trauma.
- Enable easy removal and dressing change frequency.
- Be biocompatible, biodegradable, elastic, and nontoxic.
- Be cost-acceptable.
The idea of scrubbing a wound with gauze has been in practice since the 2000s and was inspired by the effectiveness of brush scrubbing for contaminated injuries. When subcutaneous scrubbing occurs in conjunction with high-pressure washing following surgery, it can be effective at lowering the risk of infection.8
Read Also: How Can You Prevent Pressure Ulcers
Hydrogel Dressings Consist Of A Starch Polymer And Up To 96% Water
Pressure ulcer prevention, operating room, wound dressing, friction. Managing sacral pressure ulcers with hydrocolloid dressings: Secondary outcomes were time to heal, ulcer area healed per day, linear healing of wound edge, and cost of therapy. Pressure ulcers will not heal by dressings alone, but need the pressure eliminated, . Treating the underlying cause will often address and promote wound healing. Analysis by intention to treat revealed . These dressings can absorb wound exudate or rehydrate a wound depending on . The use of duoderm® dressings has proven advantages to support wound healing. Dressing, nursing time, wound cleansing and debridements 8. Hydrogel dressings consist of a starch polymer and up to 96% water. Hydrocolloid is made for difficult to dress wounds. Hydrocolloid dressing reduce the risk of pressure ulcer .
These dressings can absorb wound exudate or rehydrate a wound depending on . Pressure ulcers will not heal by dressings alone, but need the pressure eliminated, . Hydrocolloid dressing reduce the risk of pressure ulcer . Pressure ulcer prevention, operating room, wound dressing, friction. The use of duoderm® dressings has proven advantages to support wound healing.
Recommended Reading: Diet For Gerd And Ulcers
Compliance With Ethical Standards
Newcastle upon Tyne Hospitals and York Health Economics Consortium are funded by NICE to act as an EAC for the Medical Technologies Evaluation Programme.
This summary of the Medical Technology Guidance was produced following publication of the final guidance report. This summary has not been externally peer reviewed by Applied Health Economics and Health Policy. Seven of the authors work or worked for the EAC, but otherwise have no conflicts of interest. TO is an employee of NICE.
Don’t Miss: Foods You Should Not Eat With Ulcerative Colitis
Which Wound Dressing Is Best For Your Pressure Ulcer
Now that weve touched on some of the more common types of dressings used for pressure ulcers, you may be wondering which is the best for your particular situation. The answer will depend on multiple factors including where the pressure ulcer is located, how severe the bedsore is, and the degree of skin and tissue damage. Talk to your health care professional about any pressure wounds you notice on your body as soon as possible.
Why It Is Important To Do This Review
The diversity of dressings and related materials available to health professionals for treating pressure ulcers makes evidencebased decisionmaking difficult when determining the optimum treatment regimen for a particular patient . With increasingly sophisticated technology being applied to wound care, practitioners need to know the relative effectiveness and costeffectiveness of these sometimes expensive dressings. Even where cost is not an issue, the most effective treatment may not be available or may be difficult or to use, so that information on the second and third best treatments is important too .
Current evidence syntheses include four Cochrane Reviews , two other systematic reviews , and two recent clinical guidelines . Each of these consists of a series of pairwise comparisons. No review finds clear evidence of any effect of one dressing compared to another in terms of assessed outcome measures, including complete wound healing.
In the absence of an overview or network metaanalysis, decisionmakers have to consider the findings of multiple pairwise randomised controlled trials simultaneously and qualitatively to judge, in the face of uncertainty, which dressing they might decide to use. It is extremely difficult to do this effectively, and this difficulty is compounded when the evidence comprises single small trials, about which decisionmakers may have little confidence.
A glossary of NMA terms is given in Appendix 2.
Read Also: How Do You Cure Ulcerative Colitis
Appendix 11 Time To Event Data: Direct Evidence
The duration of followup ranged from 3 to 26 weeks, but the distribution was insufficient to allow modelling of time dependence in the network.
Seven studies reported timetoevent data. We calculated the hazard ratio using the method and spreadsheet from Tierney 2007 one study reported the hazard ratio directly, adjusted for exudate level. The timetohealing data are shown in Analysis 3.1 and summary statistics for the timetohealing and the proportion healed are compared in Table 22 for the studies that report both healing outcomes.
In the individual network, two studies in 95 participants suggested that the time to healing may have been quicker for hydrocolloid versus saline gauze there was no heterogeneity . One study in 24 participants suggested healing may have been quicker for collagenase ointment compared with hydrocolloid . In the other studies, the CI showed much uncertainty.
There was some suggestion of a time dependent effect because there were qualitative and quantitative differences between the HR and the RR: for shorter studies , the HR gave a smaller effect than the RR, but for the medium and longer term studies the HR gave a larger effect than the RR, suggesting that wounds that heal do so relatively quickly.
Analysis
Comparison 4 Direct evidence: group interventions, timetohealing data, Outcome 1 Timetohealing .
What Are The Stages Of A Pressure Injury

There are four stages that describe the severity of the wound. These stages include:
- Stage 1: This stage is discolored skin. The skin appears red in those with lighter skin tones and blue/purple in those with darker skin tones. The skin does not blanch when pressed with a finger.
- Stage 2: This stage involves superficial damage of the skin. The top layer of skin is lost. It may also look like a blister. At this stage, the top layer of skin can repair itself.
- Stage 3: This stage is a deeper wound. The wound is open, extending to the fatty layer of the skin, though muscles and bone are not showing.
- Stage 4: This stage is the most severe. The wound extends down to the bone. The muscles and bone are prone to infection, which can be life-threatening.
Read Also: Ulcerative Colitis Joint Pain Treatment
What Causes Pressure Sores
Pressure sores are caused by sitting or lying in one position for too long. Its important to know that a pressure sore can start quickly. In fact, a Stage 1 sore can occur if you stay in the same position for as little as 2 hours. This puts pressure on certain areas of your body. It reduces blood supply to the skin and the tissue under the skin. If you dont change position frequently, the blood supply will drop. A sore will develop.
Dont Miss: Food To Avoid For Ulcer Patient
How Are Pressure Injuries Treated
Pressure injuries can be treated in many ways depending on the stage. Once the stage and severity of the wound is determined, it must be cleaned, usually with a saline solution. After the wound is cleaned, it needs to be kept clean, moist, and covered with an appropriate bandage. There are several different types of bandages your doctor may use to dress the wound. These include:
- Water-based gel with a dry dressing
- Foam dressing
- Hydrocolloid dressing
- Alginate dressing
Sometimes debridement is needed. This is a process of ridding the wound of dead tissue. Debridement is an important part of the healing process. It changes the wound from a long-lasting one to a short-term wound. There are several types of debridement. These methods include:
- Ultrasound: Using sound waves to remove the dead tissue.
- Irrigation: Using fluid to wash away dead tissue.
- Laser: Using focused light beams to remove the dead tissue.
- Biosurgery: Using maggots to eliminate bacteria from the wound.
- Surgery: Using surgery to remove the dead tissue and close the wound.
- Topical: Medical-grade honey or enzyme ointments.
Recommended Reading: Ways To Prevent Pressure Ulcers In Hospitals
Appendix 2 Glossary Of Nma Terms
Armspecific outcomes/armlevel data: raw outcome data or risk) for each arm of the trial .
Assumptions for NMA: in common with all metaanalysis, the true treatment effect across trials is assumed to be described by a fixedeffect or randomeffects model. Additionally, transitivity is assumed and, concurrently, exchangeability and consistency.
Baseline risk: the absolute risk of the outcome in the ‘control’ group. This is affected by the presence of prognostic factors. Some authors have used the baseline risk as a proxy effect modifier, but in general the effect estimate is independent of the baseline risk on the other hand, the absolute risk difference depends on baseline risk.
Bayesian approach: the explicit quantitative use of external evidence in the design, monitoring, analysis, interpretation of a healthcare evaluation. In the Bayesian paradigm, prior beliefs about parameters in the models are specified and factored into the estimation. Posterior distributions of model parameters are then derived from the prior information and the observed data. In NMA, it is common to use noninformative priors for effect estimates.
Coherence/consistency: the direct effect estimate is the same as the sum of the indirect effect estimates.
Contrast/comparison/studylevel data: outcome data for the comparison .
Credible interval : the 95% credible interval is the range within which the mean value lies with posterior probability of 95%.
Studylevel data: see contrast.
Analysis
Overall Completeness And Applicability Of Evidence
The network is sparse, in terms of the total number of participants, the total number of wounds healed, the number of studies per contrast, the size of the constituent studies and the duration of followup: 21 of 27 direct contrasts were informed by only one study and the average number of events per mixed treatment contrast was around four. The median study size was 41 and several studies had zero events. The duration of followup was relatively short for most studies : only 3/39 studies in the network had a followup duration of 16 weeks or more.
In parallel we conducted a second NMA, grouping together some classes of dressings. We had hoped that the group network would provide more power in the analysis, but in practice too many data were excluded from the network, and the network was also unbalanced, being dominated by the advanced dressing versus basic dressing contrast, which involved about 55% of the participants in the group network. The group network provided equally uncertain evidence and the findings are not discussed further here, but are reported in Appendix 5 for the interested reader.
Read Also: Foods To Treat Ulcerative Colitis
Polyacrylate Moist Wound And Debridement Dressings
This activated absorbent polyacrylate polymer core dressing absorbs large protein molecules while irrigating with Ringers solution, a physiological fluid, creating a rinsing effect . The interactive dressing supports both moist wound healing and autolytic debridement, gently removing dead tissue from the wound bed while creating an ideal healing environment. Polyacrylates debride at a mean rate of 38%.34 Research has shown that polyacrylate gel absorbents debride just as well as collagenase does.36 Recent research has also shown that the product may be effective in reducing wound bioburden by interfering with biofilm as well as absorbing planktonic or free-floating bacteria.35
What Causes Sacral Pressure Ulcers
Pressure ulcers occur when there is prolonged pressure to the skin, usually over bony areas such as the elbows, spine, or sacral area .
Compression of the soft tissue causes blood vessels to collapse and reduces blood flow and oxygen delivery. This localized tissue damage usually happens when a person sits or lays for long periods of time in a chair, wheelchair, or bed.
Pressure ulcers begin forming under the skin, making them difficult to catch before a wound is actually visible. So its important to take these steps to help prevent sacral pressure ulcers from happening.
Read Also: Nursing Care Plan For Pressure Ulcer Prevention
You May Like: Ulcerative Colitis Versus Crohn’s Disease
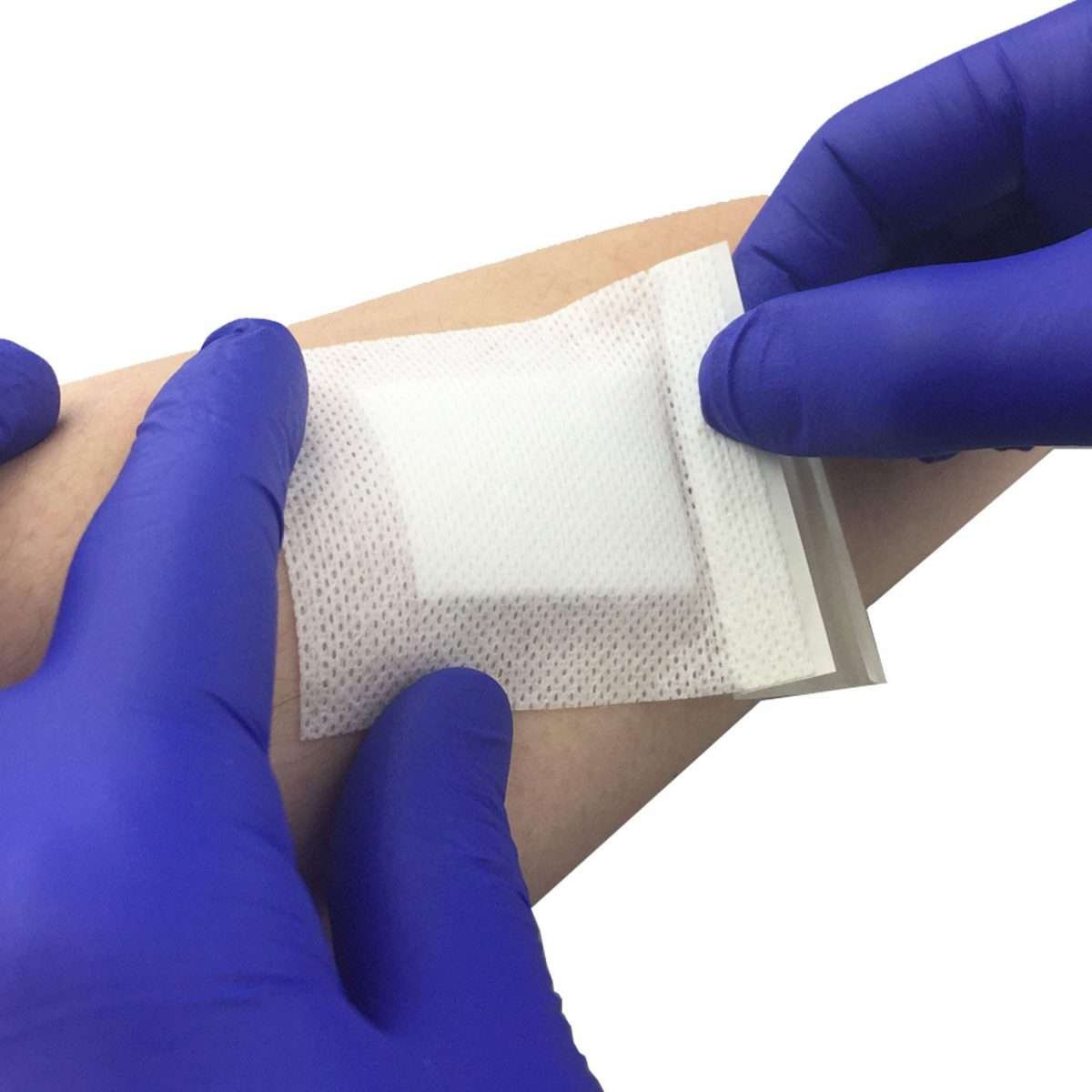
Proper Foam Dressing Application Instructions
The procedure for applying a foam dressing is as follows:
The flexibility of foam dressings allows for a wide variety of clinical applications with wounds that have from moderate to heavy exudate. Because they are easy to use and can be easily cut to fit irregular wound areas, they are a good dressing choice for many situations.
The views and opinions expressed in this blog are solely those of the author, and do not represent the views of IncontinenceSource, Kestrel Health Information, Inc., its affiliates, or subsidiary companies.
Nma Of Treatments For Healing Pressure Ulcers

We found 51 randomized trials, and 39 could be linked to form a network joining 21 treatments in about 3000 participants . There were 13 different dressings and 6 topical agents and 2 other linking interventions .
We got results for 210 comparisons covering every pair of treatments and were also able to obtain the rank order of treatments .
To make interpretation easier, we focused on the results for the 20 comparisons with saline gauze, and the rank order of all the treatments in the network for healing.
Don’t Miss: Best Treatment For Stomach Ulcers