Clinical And Pathologic Features
The diagnostic workup should include chest radiograph and CT scan. PFTs should be obtained, if possible, because they can provide a baseline in the course of treatment. Endoscopy complements imaging studies in the detection of upper airway obstruction or stenosis and in obtaining material for microbiology and histologic studies. A complete blood count with differential as well as a metabolic panel should be performed. Erythrocyte sedimentation rate and C-reactive protein may be helpful in following disease activity during treatment. Between 50% and 70% of patients with ulcerative colitis and 10% to 30% of patients with Crohn disease show atypical antineutrophil cytoplasmic antibodies , characterized by a fine granular and perinuclear pattern. Serologic testing for ANCAs may be helpful in patients with suspected underlying IBD. ANAs can help identify drug-induced lupus syndrome in patients with serositis. Since thromboembolic disease is a known cause of morbidity and mortality in IBD patients, the physician should maintain a low threshold to consider and exclude pulmonary embolism in this population.
This section discusses the different compartments of the respiratory tract involved by IBD, including unique considerations of the particular location, clinical presentation, and its pathologic features .
Airway Disease
Bronchoscopically, the large airways show variable, but often severe, inflammation. Scarred bronchial granulomas are sometimes seen in patients with CD.
How Ulcerative Colitis Is Treated
Treatment for ulcerative colitis aims to relieve symptoms during a flare-up and prevent symptoms from returning .
In most people, this is achieved by taking medicine, such as:
- aminosalicylates
- corticosteroids
- immunosuppressants
Mild to moderate flare-ups can usually be treated at home. But more severe flare-ups need to be treated in hospital.
If medicines are not effective at controlling your symptoms or your quality of life is significantly affected by your condition, surgery to remove your colon may be an option.
During surgery, your small intestine will either be diverted out of an opening in your abdomen or be used to create an internal pouch that’s connected to your anus called an ileoanal pouch.
What Is The Prognosis For People Who Have Inflammatory Bowel Disease
IBD is a lifelong condition, but it shouldnt shorten your life expectancy. With proper treatment, you can prevent flares and have long periods of remission.
Managing a lifelong condition like IBD can be challenging. Its not unusual for people with IBD to become anxious or depressed. Seeing a mental health counselor can help.
You May Like: How To Treat An Ulcer After Gastric Bypass
Symptoms Of Ulcerative Colitis
The symptoms of ulcerative colitis vary in severity based on the individual, but a few symptoms are clear warning signs of the disease.
- Diarrhea. Ongoing diarrhea that is usually bloody and shows no reaction to over-the-counter medications is one of the most common symptoms of ulcerative colitis. These urgent bowel movements can even disturb a person from their sleep.
- Abdominal or rectal pain. You may feel pain and cramping in the belly and rectal areas due to inflammation and the formation of ulcers.
- Weight loss. If left untreated, chronic inflammation, diarrhea, and other symptoms can lead to a loss of appetite, weight loss, and poor nutrition. In children, the detrimental effect on nutrition can lead to poor growth as well.
Apart from these main symptoms, other signs of the disease are:
- Fatigue
- Red or painful eyes
Whats The Difference Between Ulcerative Colitis And Crohns Disease
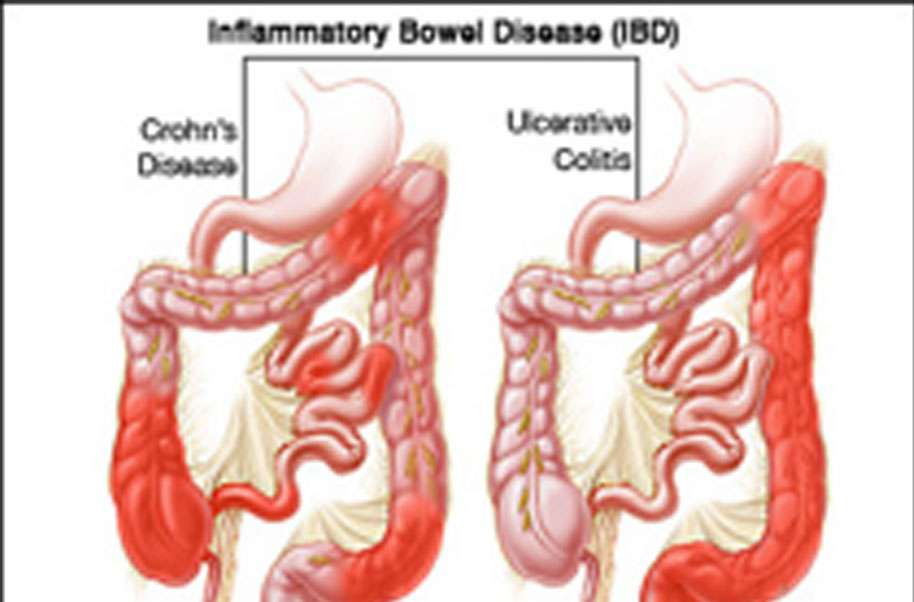
UC and Crohns disease are the most common forms of IBD. Both conditions are thought to be the result of an overactive immune system.
They also share many symptoms, including:
- cramps
- diarrhea
- fatigue
However, UC and Crohns disease do have distinct differences. Understanding the key differences between them can help you obtain a proper diagnosis.
Location
These two conditions affect different portions of the GI tract.
Crohns disease may affect any part of the GI tract, from the mouth to the anus. Its most often found in the small intestine. UC only affects the large intestine and rectum.
Response to treatment
Similar medications are prescribed to treat both conditions. Surgery is also a treatment option. Its a last resort for both conditions, but it can be a cure for UC, whereas its only a temporary therapy for Crohns.
Recommended Reading: Ulcerative Colitis Surgery Recovery Time
Specialized Diets To Manage Crohns And Ulcerative Colitis
In some cases, following a strict and specific diet protocol can do wonders for managing and reversing the massive inflammation seen in these inflammatory bowel conditions. In particular, two specific diets that have been found to be especially effective components of treatment are:
The Specific Carbohydrate Diet
This diet restricts specific carbohydrates that encourage the overgrowth of harmful bacteria in the gut. These harmful bacteria and their byproducts trigger and amplify inflammation in your gut. The SCD diet eliminates carbohydrates that contain two or more linked sugar molecules such as:
- Potatoes
- All grains including wheat, rice, corn, millet, quinoa, etc.
- Any processed meats or meats containing additives
- Dairy
- Most legumes
- Processed sugar, artificial sweeteners and sugar alcohols
- All processed foods
Eliminating complex carbs can yield impressive and significant results in many Crohns and ulcerative colitis patients.
The Elemental Diet
This diet allows your digestive tract to take a break without sacrificing your nutritional intake by consuming nutritionally complete liquids that are pre-digested. These premade formulas contain all of the carbs, fat, proteins, and nutrients your body needs in a super digestible form that doesnt require your digestive tract to break them down essentially allowing your gut to focus entirely on healing and repairing inflammation.
How Is Ibd Treated
Several types of medicines may be used to treat IBD. Some vaccinations are also recommended for patients with IBD to prevent infections. For some patients, surgery may be required to remove damaged portions of the GI tract, but advances in treatment with medicines mean that surgery is less common than it was a few decades ago. Since Crohns disease and ulcerative colitis affect different parts of the GI tract, the surgical procedures are different for the two conditions.
Don’t Miss: Signs And Symptoms Of Peptic Ulcer
Whats The Difference Between Ulcerative Colitis And Colitis
Colitis refers to inflammation of the inner lining of the colon. Colitis causes symptoms such as abdominal pain and cramping, bloating, and diarrhea.
An inflamed colon can be caused by several conditions. UC is one possible cause. Other possible causes of colitis include:
- infection
- Crohns disease
- an allergic reaction
To diagnose the cause of colitis, a doctor will order a series of tests. These tests will help them understand what other symptoms youre experience and rule out conditions based on what youre not experiencing.
Treatment for colitis will depend on the underlying cause and other symptoms you have.
Inflammatory Bowel Disease In Childhood
The age of onset of pulmonary involvement may vary in a wide range. The incidence of symptomatic bronchopulmonary involvement in children suffering from IBD seems to be much lower than in adults . The spectrum of lung pathologies is quite similar, and available reports comprise nodules consisting of non-caseating granulomas , cavitating lesions , pleuritis , lymphocytic infiltrations and organizing pneumonia in patients with CD and UC .
Don’t Miss: Does Smoking Cause Ulcers After Gastric Bypass
What Causes Ulcerative Colitis
Ulcerative colitis is thought to be an autoimmune condition.
This means the immune system, the body’s defence against infection, goes wrong and attacks healthy tissue.
The most popular theory is that the immune system mistakes harmless bacteria inside the colon for a threat and attacks the tissues of the colon, causing it to become inflamed.
Exactly what causes the immune system to behave in this way is unclear.
Most experts think it’s a combination of genetic and environmental factors.
The Worst Foods For Those With Ulcerative Colitis
Ulcerative colitis is an inflammatory chronic disease of the colon and rectum where ulcers develop inside the lining of the large intestine. It is an inflammatory bowel disease along with Crohns Disease which causes a multitude of painful and unpleasant symptoms. Since dietary habits can contribute to ulcerative colitis symptoms, lets look at the worst foods for those with ulcerative colitis.
You May Like: What To Eat With An Ulcerative Colitis Flare Up
How A Professional Can Help
Living with ulcerative colitis can be frustrating, and its better if you dont have to go at it alone. Working with a gastroenterologist and a registered dietitian can help. Medications can ease symptoms, and diet changes can help to control flares. Its especially important to include a registered dietitian if youre trying an elimination diet since they will work with you to prevent any nutritional deficiencies.
Since everyone with UC has different triggers, figuring out what works best for youand the trial and error that goes along with itwill be much easier with the help of health professionals.
You May Like: Foods That Cure Ulcerative Colitis
Complications Caused By Nutritional Deficiencies
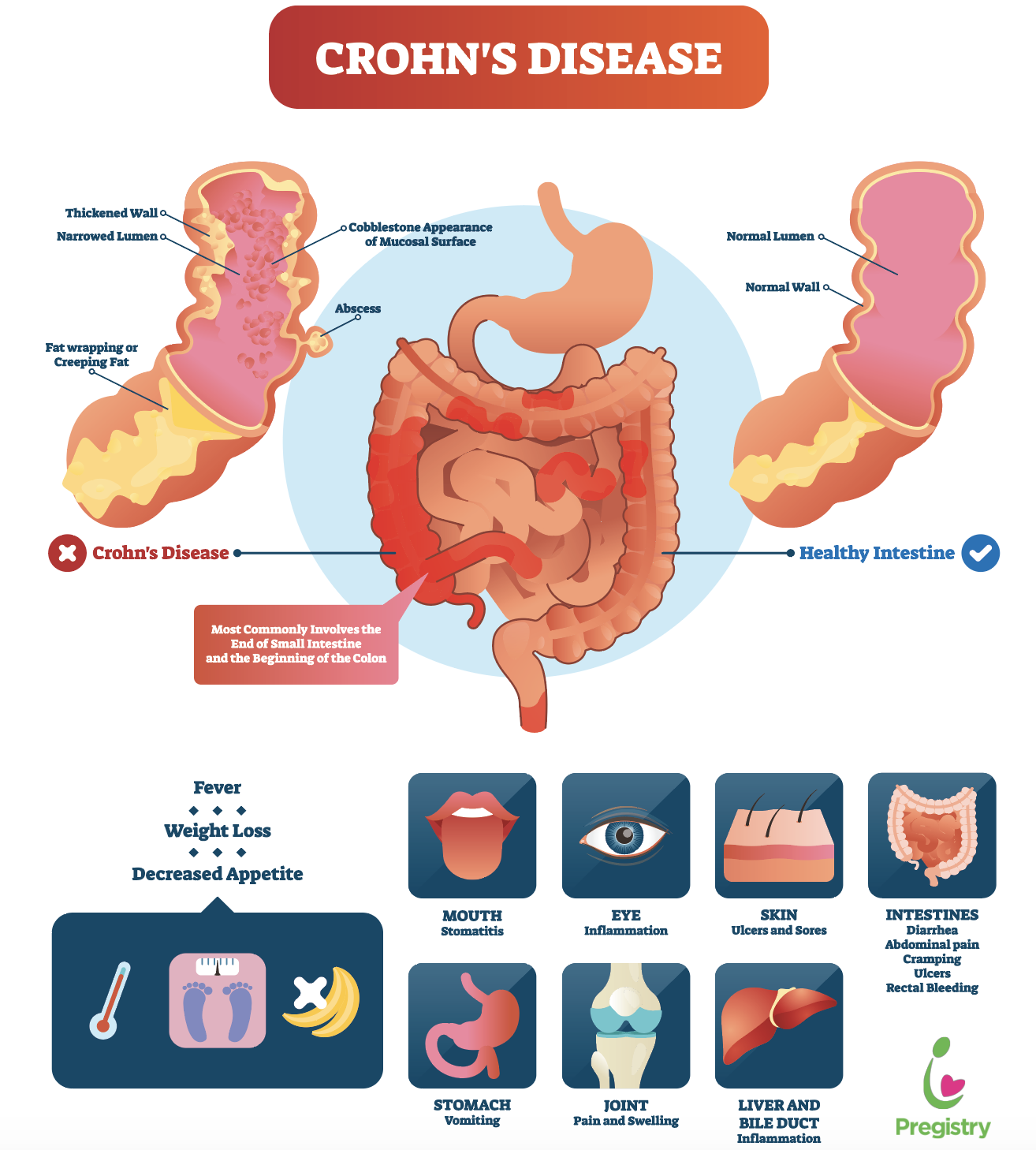
Some of the complications of malnutrition include:
- Dehydration diarrhoea causes your body to lose fluid, which can lead to dehydration. Severe dehydration can damage your kidneys.
- Anaemia reduced iron in the diet combined with losing blood from the bowel can lead to anaemia .
- Weight loss reduced appetite and poor absorption of food nutrients can cause weight loss.
- Reduced growth inadequate nutrition during childhood and adolescence can impair a childs growth and physical development.
You May Like: What’s The Difference Between Colitis And Ulcerative Colitis
Tips For Meal Prepping
Now that you have a sense of what to eat for ulcerative colitis, its time to get in the kitchen. Meal prepping some simple ingredients can make your life easier and prevent a UC flare. Here are some simple strategies:
- Buy pre-chopped fruits and veggies. Having produce in your fridge that dont require any preparation will make you more likely to add them to your plate at mealtime.
- Go frozen. Frozen fruits, veggies, and whole grains are generally as nutritious as fresh produce. Buy frozen fruit for smoothies, frozen veggies for soups and casseroles, and frozen grains to heat up in the microwave as a side dish.
- Pick up ready-made proteins. Stock up on simple options, like a rotisserie chicken or canned beans.
- Make a big batch of soup. Not only is soup soothing, its also an easy way to add a ton of veggies to your diet and is super easy to make in big batches.
- Stock up on healthy fats. Load up your cabinet with nuts, oils, and seeds for snacking, cooking, or adding texture to a recipe.
Recommended Reading: How To Check A Horse For Ulcers
Inflammatory Bowel Disease Nursing Care Plans
Inflammatory bowel disease is an idiopathic disease caused by a dysregulated immune response to host intestinal microflora. It results from a complex interplay between genetic and environmental factors. Similarities involve chronic inflammation of the alimentary tract and periods of remission interspersed with episodes of acute inflammation. There is a genetic predisposition for IBD, and patients with this condition are more prone to the development of malignancy.
The two major types of inflammatory bowel disease are ulcerative colitis and Crohn disease .
Ulcerative colitis : A chronic condition of unknown cause usually starting in the rectum and distal portions of the colon and possibly spreading upward to involve the sigmoid and descending colon or the entire colon. It is usually intermittent , but some individuals have continuous symptoms. Cure is effected only by total removal of colon and rectum/rectal mucosa.
Regional enteritis : May be found in portions of the alimentary tract from the mouth to the anus but is most commonly found in the small intestine . It is a slowly progressive chronic disease of unknown cause with intermittent acute episodes and no known cure. UC and regional enteritis share common symptoms but differ in the segment and layer of intestine involved and the degree of severity and complications. Therefore, separate databases are provided.
Also Check: Is Ulcerative Colitis A Gastrointestinal Disease
How Is Ulcerative Colitis Treated
Theres no cure for ulcerative colitis, but treatments can calm the inflammation, help you feel better and get you back to your daily activities. Treatment also depends on the severity and the individual, so treatment depends on each persons needs. Usually, healthcare providers manage the disease with medications. If your tests reveal infections that are causing problems, your healthcare provider will treat those underlying conditions and see if that helps.
The goal of medication is to induce and maintain remission, and to improve the quality of life for people with ulcerative colitis. Healthcare providers use several types of medications to calm inflammation in your large intestine. Reducing the swelling and irritation lets the tissue heal. It can also relieve your symptoms so you have less pain and less diarrhea. For children, teenagers and adults, your provider may recommend:
Children and young teenagers are prescribed the same medications. In addition to medications, some doctors also recommend that children take vitamins to get the nutrients they need for health and growth that they may not have gotten through food due to the effects of the disease on the bowel. Ask your healthcare provider for specific advice about the need for vitamin supplementation for your child.
You might need surgery that removes your colon and rectum to:
- Avoid medication side effects.
- Prevent or treat colon cancer .
- Eliminate life-threatening complications such as bleeding.
How Is Inflammatory Bowel Disease Diagnosed
If you have any of the symptoms of IBD, it’s important to see your doctor. The doctor will do an exam and ask about symptoms, your past health, your family’s health, and the medicines you take.
The doctor might order blood tests, stool tests, X-rays, and other tests, and will check your poop for blood.
The doctor might look at your stomach and intestines with an endoscope, a long, thin tube with a camera at the end. In a colonoscopy, the doctor puts the tube in through the anus to look for inflammation, bleeding, or ulcers on the colon. In an upper endoscopy, the doctor passes the tube down the throat to see the stomach and small intestine. During the procedure, the doctor might take small tissue samples. These will go to a lab for testing.
Also Check: How Do You Know You Have A Stomach Ulcer
Ulcerative Colitis Crohns Disease Or Something Else
The colon, also known as the large intestine, has three parts or section: ascending colon , transverse , descending colon , and the sigmoid colon just before the rectum.
Ulcerative colitis symptoms in each person will be different depending on where inflammation occurs and how bad it is. The most common symptoms include:
There are common complications that tend to come with UC, even though they are not actually a direct result of this chronic health condition. Fever, fatigue, and anemia are perhaps the most common additional symptoms. Additionally, inflammation beyond the colon often shows up as skin sores, skin rashes, mouth sores, joint pain, red and painful eyes, and sometimes even liver disease.
While both are referred to as inflammatory bowel disease or IBD, and Ulcerative colitis is related to Crohns disease, they are still different. Crohns disease, unlike ulcerative colitis, is not limited to the colon and is a chronic inflammatory disease of the intestines or the entire GI tract. Crohns often affects the small intestine and colon although occasionally it, too, is limited to the colon.
How Often Do I Need A Colonoscopy
Especially when you have symptoms or are just starting or changing medications, your doctor may want to periodically look at the inside of the rectum and colon to make sure the treatments are working and the lining is healing. How often this is needed is different for each person.
Ulcerative colitis also increases your chance of developing colon cancer. To look for early cancer signs, your healthcare provider may have you come in for a colonoscopy every one to three years.
Don’t Miss: Oral Antibiotics For Leg Ulcers
Ibd Is Not Irritable Bowel Syndrome
IBD should not be confused with irritable bowel syndrome or IBS. Although people with IBS may have symptoms similar to IBD, IBD and IBS are very different. IBS is not caused by inflammation and does not damage the bowel. Treatment is also different. Learn more about the difference between IBD and IBSpdf iconexternal icon.
Is Ulcerative Colitis Curable
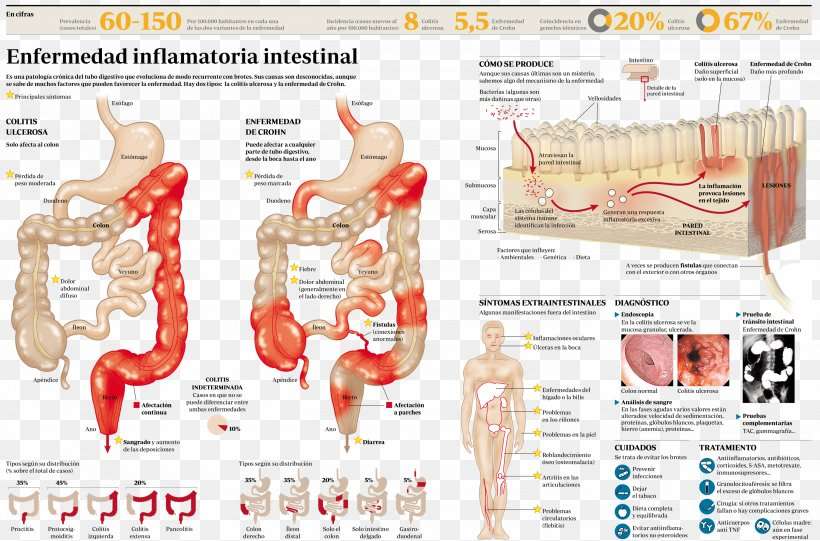
Currently, theres no nonsurgical cure for UC. Treatments for the inflammatory disease aim to extend periods of remission and make flare-ups less severe.
For people with severe UC, curative surgery is a treatment option. Removing the entire large intestine will end the symptoms of UC.
This procedure requires your doctor to create a pouch on the outside of your body where waste can empty. This pouch can become inflamed and cause side effects.
For that reason, some people choose to have only a partial colectomy. In this surgery, your doctor only removes the parts of the colon that are affected by UC.
While these surgeries can help ease or end symptoms of UC, they can have adverse effects and possible long-term complications. Read more about these issues to determine if surgery is an option for you.
Recommended Reading: Icd 10 Stage 4 Sacral Ulcer
How Common Is Ibd In The United States
In 2015 and 2016, about 3 million US adults reported being diagnosed with IBD .2 This was a large increase from 1999 .3
Some groups were more likely to report IBD, including those
- Aged 45 or older.
- Born in the United States.
- Living in poverty.
- Living in suburban areas.
This estimate does not include children younger than 18 years, who may also have IBD. Most people with IBD are diagnosed in their 20s and 30s.
The Main Types Of Drugs
The aim of drug treatment for Ulcerative Colitis is to reduce inflammation. The main types of drugs are:
Aminosalicylates reduce inflammation in the lining of the intestine. Examples include mesalazine , olsalazine , sulphasalazine and balsalazide .
Corticosteroids work by blocking the substances that trigger allergic and inflammatory responses in your body. They include prednisolone, prednisone, methylprednisolone, budesonide , hydrocortisone and beclometasone dipropionate .
Immunosuppressants suppress the immune system, and reduce levels of inflammation. The main immunosuppressants used in IBD are azathioprine , mercaptopurine or 6MP , methotrexate, ciclosporin and tacrolimus. They are often used in patients who relapse when they come off steroids.
Biological drugs are the newest group of drugs used to treat IBD. Anti-TNF drugs, such as infliximab , adalimumab and golimumab target a protein in the body called TNF, or tumor necrosis factor, preventing inflammation. Another type of biological drug is vedolizumab , which works by stopping white blood cells from entering the lining of the gut and causing inflammation.
You can find more information about some of the drugs used for Colitis: Adalimumab, Aminosalicylates , Azathioprine and Mercaptopurine, Biologic Drugs, Golimumab, Methotrexate, Infliximab, Steroids, Ustekinumab and Vedolizumab.
About a quarter of people diagnosed with Crohn’s or Colitis are children or adolescents at the time they are diagnosed.
You May Like: Doctors Specializing In Ulcerative Colitis