What You Need To Know About Ulcerative Colitis And Colorectal Cancer
Posted by Minnesota Oncology Physicians on October 4, 2021
There is a significant link between ulcerative colitis and colorectal cancer. If you have UC, your risk of developing colorectal cancer is six times greater. And the longer you have had ulcerative colitis, the higher your risk for colon or rectal cancer becomes. Why are these two conditions of the intestines connected?
How Can We Decrease The Risk Of Crc In Ibd
The positive association between UC and CRC raises several practical questions. The causes behind the changing trends in UC-related CRC epidemiology are complex. One key element may be the early diagnosis and treatment of precancerous lesions by colonoscopic surveillance or sometimes prophylactic colectomy, while the third option is primary chemoprevention. Nowadays, prophylactic colectomy is obsolete. Nonetheless, the high colectomy rate, especially in Scandinavian countries has been associated with lower CRC risks. There are however, obvious changes in the patient management, also in Scandinavia. In the new population-based cohorts, a decrease in the colectomy rate can be observed.
Ulcerative Colitis And Colon Cancer: Risks Screenings And More
- In general, having ulcerative colitis can increase your risk for colorectal cancer.
- Recent research shows that colorectal cancer rates are dropping among people with inflammatory bowel diseases such as ulcerative colitis.
- People with ulcerative colitis should receive regular screenings for colorectal cancer.
- You can reduce your cancer risk with the help of medications and lifestyle changes.
Ulcerative colitis causes inflammation in the large intestine, including the colon.
The most obvious effects of the disease are symptoms such as diarrhea and abdominal pain. UC can also increase your risk for colorectal cancer.
Read on to find out how UC contributes to colorectal cancer risk and what you can do to protect yourself.
Recommended Reading: What Is The Cure For Ulcer
Risk Factors For Colorectal Cancer In Ulcerative Colitis
The most important risk factors for UC-associated CRC are disease duration and extent. The possible mechanisms include chronic inflammation and as the duration of chronic bowel inflammation increases, so does the risk for colorectal dysplasia and CRC. In some studies, this annual risk rises exponentially with a duration beyond 30 years. This has led some guidelines to recommend surveillance colonoscopy every 1 year to 3 years between years 8 and 20 and every 1 year to 2 years thereafter. In contrast, some of the recently published population-based studies could not demonstrate a clear-cut relation in UC duration,and cancer risk or the gradual increase of the risk was much lower.
In the landmark trial by Ekbom et al, more than 3000 UC patients were followed up and the risk for CRC increased gradually from 1.7-fold in proctitis and 2.8-fold in left-sided colitis to 14.8-fold in pancolitis, compared to the general population. Most studies including the meta-analysis by Eaden et al, have come to similar conclusions. The overall prevalence of CRC among patients with UC in all 116 studies was 3.7%, but when restricted to the 35 studies that stratified their analyses by extent of UC, the prevalence of CRC among patients with extensive involvement rose to 5.4%.
Duration Of Ulcerative Colitis

Your risk for colon cancer typically starts to increase once youve lived with UC for about 8 to 10 years, according to the Crohns & Colitis Foundation. The longer you have UC, the higher your cancer risk.
According to a 2019 literature review , colorectal cancer rates for people in North America increase dramatically after a person has lived with UC for 30 years.
Colorectal cancer rates in Asia increase dramatically after a UC duration of 10 to 20 years. Cancer rates for Asian people whove had UC for 10 to 20 years were four times higher than rates for Asian people whove had UC for 1 to 9 years.
Cancer rates for Europeans also increased as UC duration increased. However, the increase in cancer rates over time wasnt considered statistically significant. There wasnt enough data from Oceania to compare cancer rates over time.
This literature review had some noteworthy limitations. For instance, data wasnt included for people whod had colorectal polyps or a colectomy for UC.
Data for people with cancer outside of the colon or rectum, or those with a family history of colorectal cancer, was also excluded.
You May Like: Best Grain For Horses With Ulcers
Does Ulcerative Colitis Affect Your Cancer Risk
Having ulcerative colitis doesnt mean you will get colorectal cancer, but it does increase your risk.
Ulcerative colitis is a chronic inflammatory bowel disease that affects the lining of the rectum and colon. It can be limited to the rectum or extend throughout the colon. Ulcerative colitis that affects the entire colon is called pancolitis.
The most common symptoms of ulcerative colitis are diarrhea and blood in your stool. Some patients may have abdominal pain. In severe cases, it can cause fever. Experts arent sure what causes the disease.
We talked to Yinghong Wang, M.D., about the link between ulcerative colitis, cancer and cancer treatment.
How does ulcerative colitis affect cancer risk?
If you have ulcerative colitis, your immune system recognizes the lining of your colon as a foreign body and attacks it. Over time, this damages the colon. As your body tries to repair the damage, the inflammation and constant cell replacement can result in a mutation that leads to cancer.
The more extensive your colitis and the longer you have it, the greater your risk of colorectal cancer. Males are at higher risk. And if you have both primary sclerosing cholangitis, which is inflammation of the bile duct, that puts you at even greater risk for colorectal cancer.
What should I do to reduce my cancer risk if I have ulcerative colitis?
Surgery is a cure. Because your colon is gone, the disease is gone, too.
What should cancer patients with ulcerative colitis know?
Identification Of Primary Studies
All published reports citing the risk of CRC in UC were collected by conducting a literature search on Medline using the following keywords: colorectal cancer, ulcerative colitis, surveillance studies, dysplasia, risk factors, and children. A comprehensive search of reference lists of all review articles and of the retrieved original studies was performed to find studies not identified by the Medline search. This identified 194 independent studies dating back to 1925.
Also Check: Ulcerative Colitis How Much Blood Is Too Much
What Are The Causes Of Ulcerative Colitis
Ulcerative colitis is an inflammatory bowel disease affecting the inner lining of the large intestine leading to erosion and ulcers. It is a lifelong illness with no specific cause or cure. Patients have repeated cycles of flare-ups and remission with potential manifestations beyond the gut . There is a profound emotional and social impact on the affected patients.
What are the causes of ulcerative colitis?
The exact cause of ulcerative colitis is unknown, and the possible causes are as follows:
Chronic Inflammation In The Colon From Ulcerative Colitis
UC causes chronic inflammation that affects the cells lining the large intestine . Chronic inflammation, like that caused by ulcerative colitis, is an ongoing issue. And when left untreated it can lead to the development of cancer in the colon or rectum.
Chronic inflammation is known to:
- Damage your colon lining and destroy cells that repair other cells. Without repairs, damage can occur to DNA in your colon cells, contributing to ulcer development.
- Increase the level of molecules that promote cancerous tumor growth.
- Make you more susceptible to infections, which help cancer cells grow and multiply.
Recommended Reading: Ulcerative Colitis Pain Left Side Under Ribs
Log In To Taylor & Francis Online
- 48 hours access to article PDF & online version
- Article PDF can be downloaded
- Article PDF can be printed
Issue Purchase
- 30 days online access to complete issue
- Article PDFs can be downloaded
- Article PDFs can be printed
- Choose from packages of 10, 20, and 30 tokens
- Can use on articles across multiple libraries & subject collections
- Article PDFs can be downloaded & printed
From EUR 400.00
How To Reduce Your Risk
Here are a few other things you can do to lower your chances of developing colorectal cancer and improve your odds of finding it early if you develop it:
- Ask your doctor about taking medications such as sulfasalazine , vedolizumab , or mesalamine . These drugs help manage UC, and they may help lower your risk for colorectal cancer.
- Take your medications as your doctor prescribed to keep your UC inflammation well managed.
- See your gastroenterologist for check-ups at least once a year.
- Let your doctor know if any of your family members had colorectal cancer or have recently been diagnosed.
- Eat more fruits, vegetables, and whole grains such as brown rice or wheat bread.
- Limit red meat, such as burgers, steaks, and pork. Also limit processed meats, such as hot dogs, bacon, and sausage. Theyve been linked to colorectal cancer risk.
- Avoid alcohol or limit yourself to no more than one drink a day.
- Try to walk, ride a bike, or do other exercises on most days of the week.
Along with getting regular screenings, look for these symptoms of colorectal cancer and report them to your doctor right away:
- a change in your bowel movements
- blood in your stool
Recommended Reading: What Not To Eat When You Have Ulcerative Colitis
What Are The Treatment Options For A Flare
When you first develop ulcerative colitis it is usual to take medication for a few weeks until symptoms clear. A course of medication is then usually taken each time symptoms flare up. The medicine advised may depend on the severity of the symptoms and the main site of the inflammation in the colon and the rectum .
Topical treatments applied locally by an enema or suppository are widely used for treating ulcerative colitis, particularly aminosalicylate and steroid medicinesâ see below. They are a treatment option if ulcerative colitis affects only the lower part of the bowel .
Medication options include the following:
You May Like: What Is A Good Diet For Ulcers
Getting Screened For Cancer
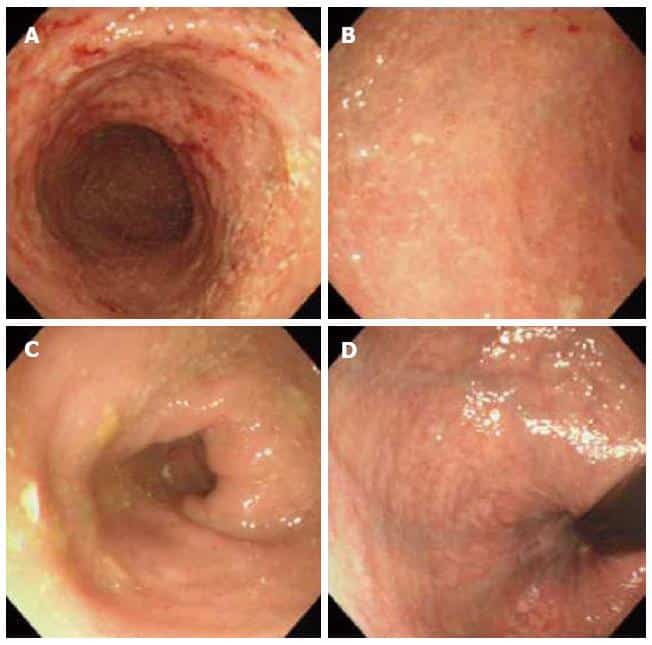
Because your risk for colorectal cancer increases over time if you have UC, its important to receive regular screenings for colorectal cancer.
People with UC should talk to their doctors about getting a colonoscopy, the main test used to detect this cancer.
Getting regular colonoscopies can help lower your risk for developing colorectal cancer or dying from colorectal cancer.
For people with IBDs who underwent regular screenings, the odds of developing colorectal cancer dropped by 42 percent. The odds of dying from the cancer dropped by 64 percent.
Read Also: Is Oatmeal Ok For Ulcerative Colitis
Why Regular Colorectal Cancer Screenings Are So Important
Colorectal cancer is curable, especially in the early stages. The best chance of complete remission comes with finding polyps early that need to be removed before they turn into cancer. This makes the entire process easier on you, less invasive, reduces the chance of it spreading to other organs, and is less expensive than late-stage cancer treatment.
To find colorectal cancer early, you need to stick with a regular cancer screening schedule. If you have ulcerative colitis or other medical conditions that put you at risk for colorectal cancer, your primary care doctor may recommend starting cancer screenings younger than the average age of 45. Screening for colon and rectal cancer can be done with an at-home stool test using a test such as a colonoscopy or a sigmoidoscopy. The right test for you, based on the severity of the UC, will be determined by your physician.
What To Do If Youre Diagnosed With Colorectal Cancer When You Have Ulcerative Colitis
There are experts in cancer care called oncologists, like those at Compass Oncology, who will assess all of your health conditions to make a recommended colorectal treatment plan. Your treatments may be a bit different than someone who doesnt have UC. Be sure to ask a lot of questions. There are no silly questions when it comes to your healthcare.
If you live in the Portland-Vancouver area and receive a colorectal cancer diagnosis, our team of GI cancer oncologists will guide you through the treatment process. Request an appointment for a consultation. Second opinions are available.
Don’t Miss: Can Ulcerative Colitis Cause Heart Problems
Does Pancolitis Affect Children
Children can develop ulcerative colitis, including pancolitis. In fact, theres reason to believe that rates of IBD in children are actually increasing, according to a 2015 study published in JAMA Pediatrics.7 Researchers hypothesize that formula feeding, high amounts of dietary fat, and exposure to antibiotics early in life may all play a role in these rising rates.
Treatments for pancolitis are the same for children as they are for adults, and revolve around controlling ulcerative colitis inflammation. Dr. Bechtold explains that in many cases, the same medications can be used, just at a lower dosage. Kids with ulcerative colitis do need to be watched carefully, though, as colon inflammation can impact how nutrients are absorbed which can impair growth, according to a 2012 study published in the World Journal of Gastroenterology.8
The good news is no matter your age, people with pancolitis can go into long-term remission with the help of a dynamic, ongoing treatment plan, says Dr. Scwhimmer. The hope is always that the medications will keep inflammation down and the risk of cancer down as well.
You May Like: What To Take For Stomach Ulcer Pain
The Importance Of Colorectal Cancer Screening
Regular screening for colorectal cancer is important for people living with ulcerative colitis because it increases the likelihood of catching cancer in its earliest, most treatable stages.
Screening is done via a colonoscopy, a procedure in which a long, flexible tube with a camera is inserted into the rectum and used to look at the inside of the colon. This allows your doctor to identify and remove any polyps or other tissue that may be precancerous.
Recent technological advances have improved methods for identifying cancer or precancer in the large intestine during a colonoscopy. For instance, a chromoendoscopy may be used to identify polyps and precancerous changes in the large intestine. This involves using a blue contrast dye to highlight any changes to the lining of the intestine.
According to the Crohn’s and Colitis Foundation, those who have had UC symptoms for a period of eight or more years should have a colonoscopy every one to two years. The exception to this is those who have both UC and the liver disease PSC. In this case, surveillance through colonoscopy should begin as soon as a UC diagnosis has been given.
Read Also: How To Heal An Ulcer In Your Mouth
Endoscopic Surveillance In Ibd
Endoscopic surveillance remains an important but often disputed cornerstone of IBD management. Colonoscopic surveillance to detect dysplasia and/or cancer is routinely indicated in compliant UC patients in clinical practice. Surveillance colonoscopy may permit earlier detection of CRC, with a correspondingly improved prognosis however, unequivocal evidence is lacking that surveillance colonoscopy prolongs survival in patients with UC. Based on previous epidemiological data, international guidelines of the Crohn’s and Colitis Foundation of America and very recently the European Crohn’s and Colitis Organisation suggest a relatively strict surveillance policy. Whether these recommendations require adjustments in light of new epidemiological data that suggest a much lower CRC incidence remains questionable. Many factors need to be considered. Nonetheless, it is possible that the lower incidence rates reported in recent population-based studies are at least partly a consequence of the vigorous surveillance programs.
The diagnosis of dysplasia is demanding. During a period of active disease, it is almost impossible to differentiate between inflammation and true dysplasia. Furthermore, a significant interobserver variation was reported for the detection of dysplasia, and an agreement concerning low-grade dysplasia may be as low as 43%. Therefore, because of important prognostic implications, any case of dysplasia should be confirmed by an experienced pathologist.
Keep Up With Regular Physicals
Getting an annual physical is always smart, but it’s especially important if you have UC.
During the checkup, your healthcare provider will ask whether your treatments are going well and ensure that screening is performed at the appropriate intervals to catch any cancer in the early stages. Even if your UC symptoms are in remission , seeing a healthcare provider regularly can help ensure that you stay on the healthy track.
Recommended Reading: Ulcerative Colitis Surgery Pros And Cons
Extent And Duration Of Ibd
The extent of colonic inflammation is a risk factor for CRC. UC patients with extensive disease have a greater risk of developing CRC than do UC patients with only proctitis or proctosigmoiditis . IBD duration is one of the most important risk factors for CRC among IBD patients. CRC risk is significantly increased after 8 years of IBD and continues to increase in subsequent years .
Categories:Colorectal Cancer,Gastrointestinal Cancers
Did you know theres a significant link between ulcerative colitis and colorectal cancer? Ulcerative colitis patients have a six times greater risk of developing colorectal cancer than those of average risk. But, that being said, only about 5% of people with severe ulcerative colitis will end up developing this type of cancer. Plus, there are ways you can lower your risk.
A Personal History Of Inflammatory Bowel Disease
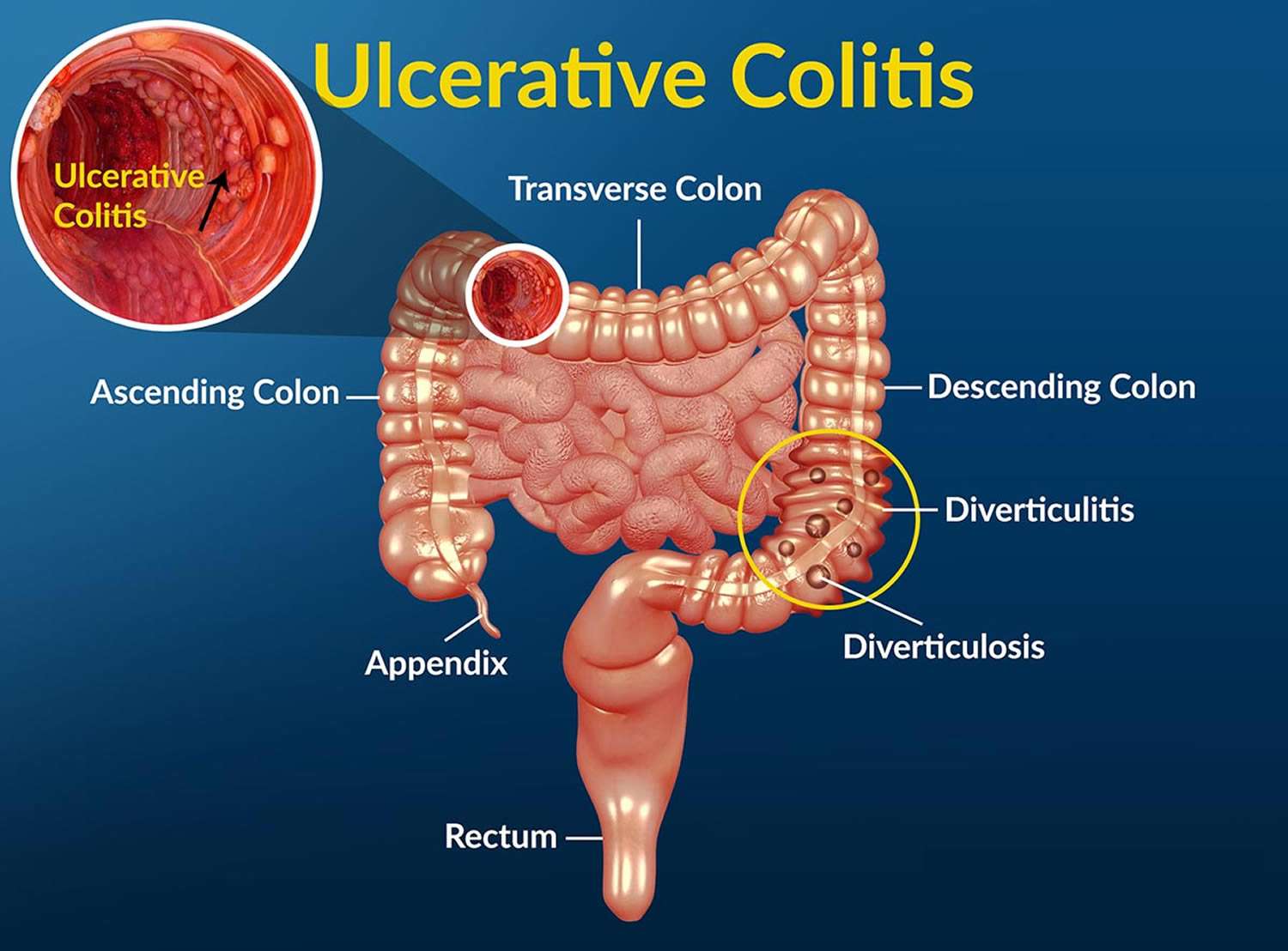
If you have inflammatory bowel disease , including either ulcerative colitis or Crohns disease, your risk of colorectal cancer is increased.
IBD is a condition in which the colon is inflamed over a long period of time. People who have had IBD for many years, especially if untreated, often develop dysplasia. Dysplasia is a term used to describe cells in the lining of the colon or rectum that look abnormal, but are not cancer cells. They can change into cancer over time.
If you have IBD, you may need to start getting screened for colorectal cancer when you are younger and be screened more often.
Inflammatory bowel disease is different from irritable bowel syndrome , which does not appear to increase your risk for colorectal cancer.
Also Check: How To Get Remission In Ulcerative Colitis
Recommended Reading: What Foods To Avoid If You Have A Stomach Ulcer