Are Nutritional Needs Different For People With Ibd What Are The Specific Nutritional Needs For People With Crohn’s Disease And Ulcerative Colitis
Nutritional needs are specific to the individual and differ with disease state, body size and age. A nutritionist can help you estimate your individual needs. Calorie and protein needs are similar for Crohn’s disease and ulcerative colitis. In both diseases, needs increase during inflammation and immediately after to restore losses. The following are general statements about nutritional needs that may apply to you.
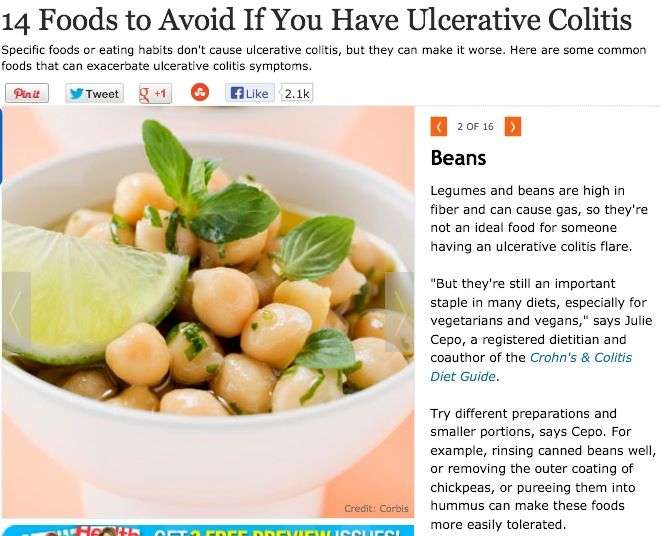
Not Completely Awful Treats
The following meals are really just treats for those times youre really craving something sugary and sweet and full of carbs.
These really arent great for us, but theyre a much better bad choice than some others we can make.
This is the type of stuff I cheat with and its plenty for me. I dont need to eat anything worse.
Ulcerative Colitis In Children
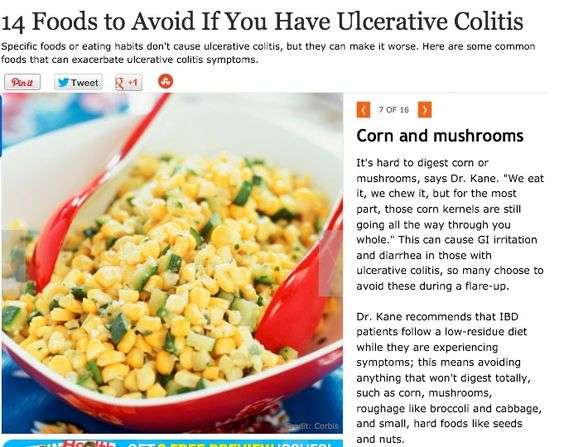
Without proper care, pediatric ulcerative colitis will result in slower than normal growth and/or stunted growth.Intestinal inflammation lowers a childs appetite, which mean less food is eaten resulting in fewer nutrients to support healthy growth. Supplements are often a good idea as is making sure that enough calories are consumed, which sometimes requires a high-calorie diet for some kids. Additionally, a therapy or counseling may be sought to help a child develop the tools to cope with their disease.
Recommended Reading: What Does Asacol Do For Ulcerative Colitis
Don’t Miss: Bowel Ulcers Signs And Symptoms
General Guidelines When Ulcerative Colitis Is In Remission
Some members of MyCrohnsAndColitisTeam find they can eat a wider variety of foods safely during remission periods when ulcerative colitis is not as active and symptoms are absent or mild. Still, every individual is different, and purportedly beneficial foods may trigger symptoms. Trial and tracking is the only way to know for sure.
If it is safe for you, these guidelines may help you stay your healthiest during remission:
- Get 25 grams to 35 grams of fiber per day to promote bowel regularity and reduce inflammation.
- Consume plenty of lean meats, which are a good source of B vitamins. Include fatty fish, tofu, and nut and seed butters.
- Include probiotic foods such as yogurt, tempeh, kefir, kimchi, miso, and sauerkraut.
While some members find kefir too sour for their liking, others report experiencing benefits from trying the fermented drink. Kefir has been helping me over the past week, wrote one. Been trying kefir the past few days. Will keep you posted. So far less pain, said another.
Characteristics Of Uc Cases And Controls
In the present study, 327 people were included. Mean age of cases and controls was 39.5 ± 10.0 and 41.5 ± 11.8 y, respectively. Totally, 52% of study participants were female and 48% were male. Participants with UC were less likely to be physically active and university graduates. No significant differences in mean age and BMI were observed between cases and controls. There was also no significant difference in the distribution of subjects when considering them in terms of sex, smoking status, marital status, and history of diabetes. Comparing participants across quartiles of IPD score, we failed to find any significant difference in mean age and BMI as well as sex, marital status, smoking status, history of diabetes, education, and physical activity .
Table 1. Characteristics of patients with ulcerative colitis and controls across quartiles of inflammatory potential of the diet score.
You May Like: What Are Leg Ulcers Caused By
Does Ulcerative Colitis Lower Life Expectancy
Most people with this condition can have a full life expectancy. However, complications can increase the risk of an early death , according to one 2003 Danish study. Very severe ulcerative colitis could impact your life expectancy, especially within the first couple of years after your diagnosis.
Read Also: What Are Leg Ulcers Caused By
Whats The Best Diet For Ulcerative Colitis And Crohns Disease
The best diet is the one that doesnt keep making you sicker and further over-stimulating your immune system.
The best diet for ulcerative colitis is:
- Meat
- Well-Cooked Vegetables
- Fruit Smoothies
Truthfully, thats the whole thing. Theres a lot in the practice of the above, but those are the foods to build your lifelong eating patterns around.
If you want a name for the diet, its the Autoimmune Protocol Diet or the Paleo Autoimmune Protocol Diet. I abbreviate the latter Paleo-AIP here on the blog and in my books.
Read Also: How To Prevent Sacral Pressure Ulcers
A Caveat On The Ground Flax Seeds
This one is kind of a rule bend. Flax seeds are not allowed on a strictly Paleo-AIP eating template.
Ive personally been using them forever and my immune system is fine with them. I feel the additional fiber is quite beneficial for me.
But Ive tested this in my own body extensively. This is an empirical thing.
Not everyone can handle them.
Heres the finished shake. Its really quite good.
How Can I Prevent Inflammatory Bowel Disease
While there isnt anything you can do to prevent IBD, certain dietary and lifestyle changes may control the symptoms. You can:
- Eat smaller meals every two to four hours.
- Find healthy ways to manage stress, such as meditation, movement like tai chi, listening to music or going for a walk.
- Get plenty of sleep and stay physically active.
- Keep a food diary to identify foods that trigger IBD flares. You may find you have a food intolerance, such as lactose intolerance. If so, your body has a harder time digesting certain foods, which causes stomach upset.
- Reduce foods that irritate the intestines, such as those that are fibrous, spicy, greasy or made with milk. During flares, choose soft, bland foods that are less inflammatory.
- Cut back on caffeinated, carbonated and alcoholic beverages. Drink more water to prevent dehydration.
Ulcerative colitis is an inflammatory chronic disease of the colon and rectum where ulcers develop inside the lining of the large intestine. It is an inflammatory bowel disease along with Crohns Disease which causes a multitude of painful and unpleasant symptoms. Since dietary habits can contribute to ulcerative colitis symptoms, lets look at the worst foods for those with ulcerative colitis.
Also Check: Symptoms Of Having Ulcers In Your Stomach
What To Eat During Flare
Low-fiber foods are easiest to digest and are less irritating to the gut, especially with symptoms like abdominal pain or diarrhea. Choose:
- Grains/starches: White foods, instead of wheat or whole-grain, and those with less than 2 grams of fiber per serving
- Cooked vegetables: Well-cooked vegetables such as green beans, carrots, mashed potatoes without skin, steamed asparagus tips and pureed squash.Use fresh or frozen.
- Canned or soft fruits: Peeled apples, ripe bananas, cantaloupe, honeydew, watermelon, and canned fruit in fruit juice or light syrup
Be sure to eat enough protein — Inflammation causes increased protein needs. Choose:
- Tender, well-cooked meats: Poultry, salmon or other fish, lean beef and pork prepared without added fat
- Deli meats: Low-sodium and low-fat varieties
- Eggs: Well-cooked
- Tofu
- Smooth nut and seed butters: Peanut, almond or sunflower seed
Drink plenty of fluids — Aim for eight cups a day, and consider using oral rehydration beverages as needed. Try to limit caffeinated, sugar drinks and beverages made with sugar substitutes.
Limit added fats and oils — Focus on oils instead of solid fats, and limit intake to less than eight teaspoons per day.
Consume adequate calcium, vitamin D, probiotics, and prebiotics — Sources include:
A Healthy Crohns Disease Diet
Not everyone with Crohns disease has the same food triggers, Taylor says, so you might need to do some sleuthing to figure out what works for you. Try keeping a food journal jotting down what you ate and any symptoms you notice to look for clues about the foods that make your stomach unhappy.
When you arent having symptoms, though, try to eat a balanced diet. You dont want to regularly shun healthy foods like whole grains, veggies or beans. Malnutrition can be a problem for people with Crohns disease, so only avoid these foods during a flare-up, she says.
Managing this lifelong disease can be a challenge, and a dietitian can help you manage your diet.
Crohns is different for every person, so work with someone who can help you design an individualized plan, Taylor says. If you have a dietitian in your corner, theyll be available so that when you have a problem, they can steer you in the right direction.
Also Check: How To Eat With A Stomach Ulcer
What Role Does Diet And Nutrition Play In Ulcerative Colitis
Diet does not cause the development of ulcerative colitis nor can any special diet cure the disease. However, the foods you or your child eat may play a role in managing symptoms and lengthening the time between flareups.
Some foods may make symptoms worse and should be avoided, especially during flareups. Foods that trigger symptoms are different from person to person. To narrow down what foods affect you, keep track of what you eat each day and how you feel afterward .
Problem foods often include:
- High sugar foods and drinks.
- Carbonated beverages.
- High-fiber foods.
- Alcohol.
In addition to the problem foods listed above, infants, children and teenagers can also experience issues with:
- Salt.
- Dairy products.
Keep a careful eye on your childs diet and nutrition. Their appetite may decrease during a flareup and they might not eat enough to stay healthy, and grow. Also, the inflammation caused by ulcerative colitis may keep their digestive tract from absorbing enough nutrients. This can also affect your childs health. For these reasons, you may have to increase the amount of calories your child consumes.
Its best to work with your provider and nutritionist to come up with a personalized diet plan if you or your child has ulcerative colitis.
Diet Recommendations For Crohn’s Disease Flare

- Follow a low residue diet to relieve abdominal pain and diarrhea.
- If you have strictures, it is especially important to avoid nuts, seeds, beans and kernels.
- Avoid foods that may increase stool output such as fresh fruits and vegetables, prunes and caffeinated beverages. Cold foods may help reduce diarrhea.
- If you have lactose intolerance, follow a lactose-free diet. Lactose intolerance causes gas, bloating, cramping and diarrhea 30 to 90 minutes after eating milk, ice cream or large amounts of dairy. A breath hydrogen test may confirm suspicions of lactose intolerance.
- If you have oily and foul-smelling stools, you may have fat malabsorption. Treat fat malabsorption by following a low-fat diet. Discuss these symptoms with your doctor or nutritionist.
- Smaller, more frequent meals are better tolerated and can maximize nutritional intake.
- If your appetite is decreased and solid foods not tolerated well, consider taking nutritional supplements .
Don’t Miss: Foods For Ulcers And Gastritis
Track The Good And The Bad
There’s no single diet that will help everyone with UC. The condition can also change over time, so your plan will need to be flexible, too. The key is to find what works for you.
To stay organized, keep a food diary. Use your smartphone or a small notebook to record what you eat and drink and how they make you feel, both good and bad. It takes a bit of time and patience, but it will help you track your condition and fine-tune your diet plan.
When you prepare your meals, don’t forget that a well-balanced diet gives you enough protein, whole grains, and fresh fruits and vegetables.
You might not be able to eat everything in the grocery store or on the menus at the restaurants you like. But try to focus on the ones that you can enjoy without triggering your symptoms. Some simple tweaks in your meal prep can make it easier to eat some foods, like steaming veggies or switching to low-fat dairy.
Some people follow a low-residue diet or low-fiber diet every so often, getting about 10-15 grams of fiber a day. That can help you go to the bathroom less often.
Watch out for items that can be troublemakers if you have UC, including:
- Alcohol
What About Vitamins And Minerals
It is a good idea for all people with IBD to take a standard multivitamin every day. People with IBD who are doing well do not need any extra vitamins or minerals. If you have Crohns disease is in the ileum or the ileum has been removed you may need to take B12, calcium, or vitamin D. You may need iron supplements if you have blood loss during inflammation or reduced iron absorption as a result of inflammation. Diarrhea or vomiting can cause loss of potassium and magnesium. If you are lactose intolerant and avoid dairy products, this can lead to low calcium. Ask your doctor if you need to be tested for any of the above.
Recommended Reading: Is Ulcerative Colitis Caused By Stress
Foods To Avoid During Flares
Diet doesnt cause flares, but your food choices can make symptoms worse if your IBD becomes active.
How foods affect people who are flaring varies from person to person. But here are some of the foods that may worsen symptoms of a flare and cause complications:
- Fatty foods
- Beverages containing alcohol or caffeine.
- Sugar alcohols used to sweeten in sugar-free foods
- Raw fruits and vegetables
- Whole grain and high-fiber breads and cereals
- Dried fruit
- Fruits with seeds and skins
Fruit And Hemp Protein Smoothie
This particular smoothie recipe has been a daily staple for me for many years now:
- Nutiva Hemp Protein Powder
- Fresh fruit like mangoes, strawberries or blueberries
- Organic coconut oil
- Organic India Psyllium Husk Fiber
- Ground Flax Seeds
- Celtic Sea Salt
- Water and/or Hemp Milk
This combination of stuff blended together is about as close as Ive found to foods that are actively healing for the gut and UC.
This shake daily makes a HUGE difference in my bowel health and stools.
Ive been told the same thing by others with and without UC who have used the recipe with consistency as well.
Don’t Miss: Crohn’s Versus Ulcerative Colitis Pathology
Nutritious Foods To Combat Ulcerative Colitis Complications
People with ulcerative colitis commonly experience anemia and unintended weight loss. Anemia is a low red blood cell count caused by chronic blood loss. It can cause fatigue unless treated. For this reason, the nutrients folate, magnesium, calcium, and iron are of special importance for individuals with UC.
Furthermore, steroid medications such as prednisone may contribute to risk of osteoporosis, which puts emphasis on dietary intake of calcium, vitamin D, magnesium, and vitamin K. Here are the vital body functions that depend on each of these nutrients, along with food sources rich in each.
Calcium
Calcium is important for healthy bones, teeth, and the heart. The best food sources include dairy products, such as yogurt, milk, cottage cheese, and more. Nondairy sources of calcium include sardines , fortified soy milk and almond milk, tofu, kale, broccoli, and chia seeds.
Folate
Folate is crucial for cell division and DNA synthesis. It is found in avocados, black-eyed peas, spinach, Brussels sprouts, asparagus, and fortified breakfast cereals.
Iron
Iron is an important mineral that helps transport oxygen in red blood cells from the lungs to body tissues. It is found in fortified breakfast cereals, tofu, spinach, lentils, chickpeas, and cashews.
Magnesium
Magnesium is an important electrolyte that may be lost through sweating or diarrhea. Foods such as halibut, nuts, nut butters, spinach, potatoes with skin, black-eyed peas, and spinach are rich in magnesium.
Vitamin D
What To Do During A Flare
Medications are used to manage flares and induce remission as quickly as possible.
Doctors may prescribe a corticosteroid , antibiotic, 5-aminosalicylate, immunomodulator or biologic.
In addition, certain diet changes may help shorten flares. Some tips to keep in mind:
- Keep a food and symptom journal during flares to identify bothersome foods. This also ensures that foods are not avoided without cause.
- Eat small, more frequent meals as opposed to 3 large meals in a day .
- Ask your doctor whether to limit fiber until symptoms pass. Eating a maximum of 10 grams of fiber per day may reduce irritation and lower the risk of intestinal blockage. Once you are in remission, gradually increase your fiber intake, depending on how much you can tolerate, until you reach the recommended daily intake of 2530 grams.
- Drink plenty of fluids to avoid dehydration.
Don’t Miss: Does Aloe Vera Help Ulcerative Colitis
Why Working With A Qualified Care Team Is So Important When It Comes To Managing Ulcerative Colitis
People being treated for UC typically arent getting dietary or lifestyle advice, which is a huge disservice, says Cohen. But managing ulcerative colitis and preventing flare-ups can be done! You just might need a little help from the experts.
Because UC isnt one-size-fits-all and triggers are highly individual, enlisting the help of a care team like the clinicians at Parsley Health is wise. Providers can provide individualized supplement protocols based on lab testing, customized eating plans for periods of remission and flares, and communicate with your current GI doctor if necessary to streamline care.
Study Design And Participants
In the present cross-sectional study, the diet adequacy and food avoidance habits of UC patients in the UK were investigated. The study was conducted according to the guidelines laid down in the Declaration of Helsinki, and all procedures involving human subjects were approved by the ethics committee of a UK Higher Education Institution. Written informed consent was obtained from all participants.
A total of ninety-seven UC patients were recruited across the UK from the National Association for Colitis and Crohns Disease registers by e-mail, posts in UC forums and social media sites. The inclusion criteria were as follows: aged 1865 years and no history of UC-related surgery.
Initially, four participants participated in a pilot study to ensure that the questionnaire and 24 h dietary recalls were readable and not distressing.
Also Check: Total Contact Casting For Diabetic Foot Ulcers