Implications For Future Practice
Improving venous ulcer care requires increasing nurse wound care knowledge across settings and ensuring nurses work at the top of their scope of practice. For example, barring exclusion from a states nursing practice act, training in debridement of venous ulcers can be taught to nurses in many settings to facilitate care outside of wound care centers. In addition, nurses and patients can use monofilament devices for mechanical debridement.
The Centers for Medicare & Medicaid Services has paved the way for using telehealth during the pandemic, making it an ongoing viable option for helping patients adhere to treatment recommendations. It can be used for patient and family education and to perform screening and monitoring visits, effectively reducing barriers to care.
For more complex patients, home health nurses should be trained in advanced wound care to help reduce gaps in care during times of crisis and for patients unable to visit a wound care center. In addition, in-person or virtual patient self-care education is vital to ensure proper venous ulcer management if in-office or home health visits arent possible.
Risk Factors For Leg Ulcers
- Age peripheral circulation becomes less efficient with old age.
- Varicose veins the one-way valves that stop blood from travelling backwards in the vein stop working. The pooling of blood stretches and distorts the vein.
- Cigarette smoking tobacco is known to constrict the vessels of the circulatory system.
- Arterial disease vein problems are more likely if the person already has other diseases of the arteries.
- Certain disorders these include diabetes and arthritis.
- Pressure sores bed-bound people are at risk of pressure sores, which are areas of damage to the skin caused by constant pressure or friction.
- Medication some cardiovascular medications can contribute to leg oedema and altered circulation.
Signs And Symptoms Of Leg Ulcers
The most common symptoms that accompany leg ulcers are as follows:
- Swelling of the ankles
- Irritated or flaky skin
- Skin begins to harden and scale around the ulcers
These symptoms often vary in their severity. Although most leg ulcers usually disappear in a few days, some may be non-healing. It is always better to try and heal leg ulcers as soon as you can to prevent further complications. For that, you need to diagnose them first. The following are a few most common techniques used to diagnose leg ulcers.
Don’t Miss: How To Heal Mouth Ulcers
How To Effectively Treat Venous Ulcers
Regular bandages over the skin sores will make you more comfortable and help prevent the ulcers from becoming infected, but they wont heal them. The key to treating and healing venous ulcers is to prevent the blood from pooling in your veins so that the fluid does not ooze out and damage the surrounding tissues. There are a few ways you can treat the underlying problem that causes venous ulcers, including:
How Are Leg Ulcers Treated
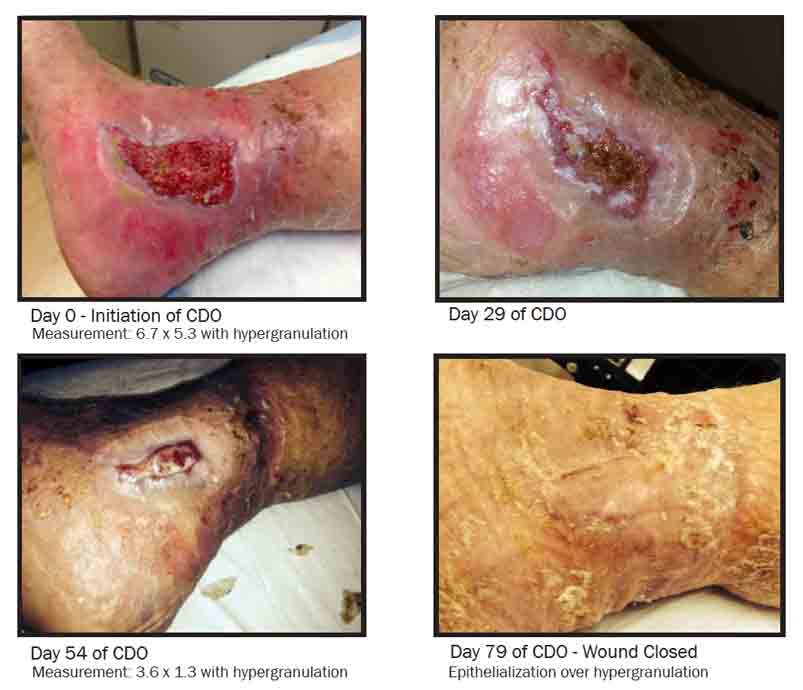
Treatment of leg ulcers typically involves compression bandages or stockings. Compression bandages or stocking provide pressure that may help restore the proper circulation of blood in your legs. Dressings, which are sterile bandages or wraps, may be placed on the sores to help aid in the healing process of leg ulcers. Your doctor may also prescribe antibiotics if your leg ulcer has become infected.
To help improve circulation in your legs, your doctor may also recommend that you raise your leg throughout the day for 30-minute intervals. Surgery may also be recommended as an alternative for restoring proper circulation in your legs.
Speak with your doctor to learn more about the available treatment options for leg ulcers.
Our heart and vein doctors at Heart Vein NYC have over 20 years of experience providing the New York City area with comprehensive, personalized vascular care for patients who suffer from leg ulcers or who have symptoms of a vascular condition. Contact our compassionate heart doctors if you believe you have a vascular problem and want to learn more about improving your vascular health. Call or schedule an appointment with Heart Vein NYC today.
You May Like: Air Mattress For Pressure Ulcer Prevention
Recalcitrant Ulcers: Factors Prolonging Healing
Acute wounds physiologically heal within 4 weeks on the other hand, chronic wounds need a longer time to close, with an average healing time of 612 months for VLU. Moreover, it has been estimated that recurrence occurs in about 70% of VLU within 5 years of closure .
Several events occur to delay wound closure, including ulcer characteristics, concomitant diseases, patient characteristics, diagnostic delays and inaccuracies, therapeutic interventions, and environmental factors.
A well-known risk factor for recalcitrant ulcers is advanced patient age. In fact, elderly patients generally have reduced mobility as well as lesser compliance for compression bandages and garment treatments compared to younger patients. The VLU microenvironment is also characterized by a compromised cellular and biochemical machinery, where senescent fibroblasts fail to respond to proliferative stimuli .
Preexisting or underlying venous diseases, including all anatomic levels of venous system disease or deep venous thrombosis, are among the major risk factors for delayed healing.
Patients with higher body mass index and nutritional deficiencies also have a poor healing prognosis .
Additionally, a history of venous ligation or vein stripping, a history of hip or knee replacement surgery, ankle brachial pressure index < 0.8, and the presence of fibrin covering greater than 50% of the wound area have been associated with prolonged healing .
Side Effects Of Leg Ulcers
- A green and foul-smelling discharge from the ulcers
- The skin around the ulcers begins to swell
- The sores become bigger
- Inflamed skin around the ulcers
Leg ulcers resemble sores that develop when bacteria enter underlying tissues through injured or broken skin. While skin injuries are the most common risk factor for leg ulcers, certain underlying medical conditions like diabetes, arterial disease, and venous disease may also lead to leg ulcers. Some common signs and symptoms that often accompany leg ulcers include irritated or flaky skin, swelling, heaviness, discoloration, and leg pain on prolonged standing. You may use natural ingredients like Gotu kola, turmeric, aloe vera, coconut oil, tea tree oil, and yarrow in home remedies to heal leg ulcers in mild to moderate cases.
You May Like: Is Green Tea Good For Ulcers
Treatment Of Venous Insufficiency Ulcers
In directly treating venous ulcers, the primary goals are keeping the ulcer site infection-free during the healing process and alleviating edema of the site. Debridement to remove dead tissue and surface contamination may be used to change the wound from chronic to acute, at which point it can progress through the regular stages of healing. Maggots or biotherapy may also be suggested as another method of removing necrotic tissue from the wound. Typically, oral antibiotics are only necessary if there is an infection in the surrounding tissue. The wound environment should typically be moist, with dressings changed as infrequently as possible due to the fact that changing dressings removes both healthy cells and debris. In extreme cases, surgical skin grafts can be used in order for abnormally large or painful venous ulcers to properly heal.
The following precautions can help minimize the risk of developing venous ulcers in at-risk patients and to minimize complications in patients already exhibiting symptoms:
What Is The Finest Cream For Leg Ulcers
Additionally, creams containing urea may be beneficial, since urea is a good moisturizer. Around a leg ulcer, the skin may get macerated and damaged, particularly if the lesion is actively oozing. A barrier film, such as Cavilon barrier film or LBF , protects and assists in the healing of the peri-wound skin.
Dont Miss: Signs And Symptoms Of Peptic Ulcer
You May Like: What Is Stomach Ulcer Pain Like
Tenets In The Treatment Of Cvlus
A systematic assessment of patient and CVLUs is essential to find the underlying etiology. The basic principles in managing CVLUs are to remove the etiological causes, to evaluate the wound and artery pulses, and to manage systemic conditions and wound infection with debridement, and to reduce excessive pressure on the wound. The first-line treatments of CVLUs are bed rest with leg elevation, wound care, debridement, and compression. Surgical approaches remain a high ligation with or without stripping or ablation of the great saphenous veins depending on venous reflux or insufficiency not all CVLUs are suitable for surgery due to comorbidities. Standard wound care should be used for an initial period of 4 wk and can fail to heal approximately 25% of CVLUs. Even advanced therapies do not heal > 60%. Wound failing to heal 50% ulcer area at 4 wk should be reevaluated and then considered for advanced therapies in the absence of underlying disease. When standard care of wound for 4 wk failed to heal CVLUs effectively, advanced wound care should be considered to use based on the available evidence. Unfortunately, many advanced approaches for CVLUs do not have strong evidence or a randomized prospective study to evaluate the efficacy.
Articles On Types Of Dermatitis
Venous stasis dermatitis happens when thereâs a problem with your veins, usually in your lower legs, that keeps blood from moving through very well. As more fluid and pressure build, some of the blood leaks out of your veins and into your skin.
The condition is also called venous eczema or stasis dermatitis. Itâs more common in people who are 50 or older. Women are more likely to have it than men.
Medical treatments can help, and you can do many things on your own to get the problem under control.
Read Also: Can Coffee Cause Ulcerative Colitis
Also Check: Foods To Treat Ulcerative Colitis
What Should I Do At My Appointment
Remember to remove any nail polish from your toenails before your appointment.
When you see the nurse or doctor, they should:
- Ask about your symptoms and how long you have had problems
- Examine your lower legs
- Do a simple test called a Doppler Ultrasound. This test compares blood flow in your ankle with that in your arm to find out if there are arterial blood flow problems in your lower leg. You may have to come back to have your Doppler test on another day or at another clinic.
- You may also be offered some other tests to check for other health problems that can affect your legs such as diabetes and anaemia.
You may hear different words to describe your wound such as ulcer, leg ulcer, sore, laceration, chronic wound and maybe others. Ask your nurse to explain their choice of word and what this may mean for you.
Recommended Reading: Is Beer Bad For Ulcerative Colitis
Venous Leg Ulcer Causes
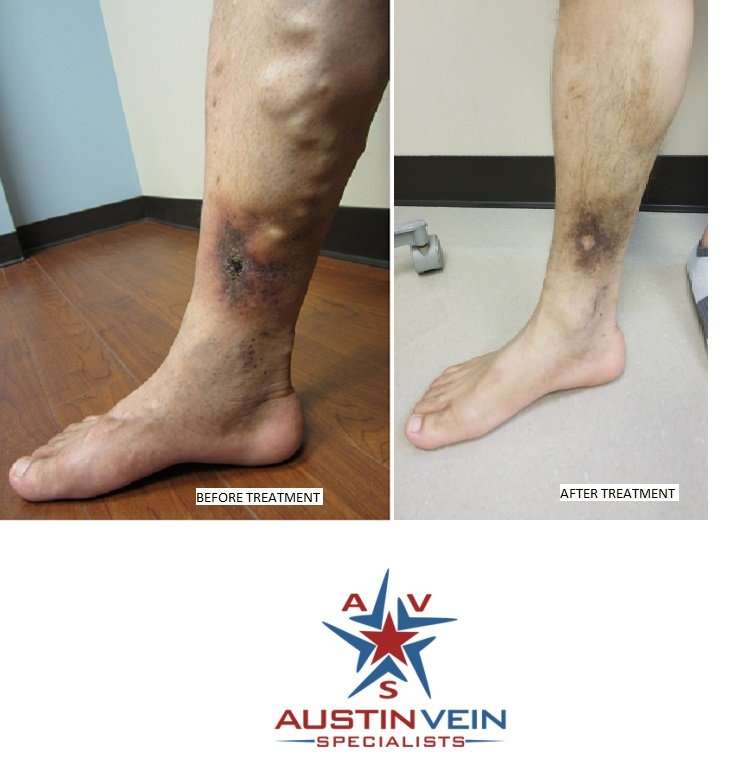
A venous leg ulcer is caused by low blood circulation due to damaged veins in your legs.
There are two main types of blood vessel:
- arteries oxygen-rich blood is pumped from your heart, through your arteries, to the rest of your body
- veins blood is returned to the heart through the veins once the oxygen has been removed
Vein problems occur when the valves inside the veins stop working properly.
In a healthy vein, blood flows towards the heart. Blood is prevented from flowing backwards by a series of valves that open and close to let blood through. If the valves weaken or are damaged, for example, following a deep vein thrombosis, the blood can flow backwards.
This may cause varicose veins visible on the surface of the leg, or the damage may lie in the deep veins, hidden from view. Pressure inside these veins is increased and this can damage the skin.
The constant high blood pressure in your legs causes fluid to leak from the veins. The fluid causes swelling and damages the skin, which becomes hard and inflamed, leading to an ulcer.
Also Check: Primary Sclerosing Cholangitis Ulcerative Colitis
Best Practices For Venous Leg Ulcer Treatment
Venous leg ulcer treatment and management require frequent examination of at-risk patients and best practice wound care with a focus on prevention. Without effective treatment, venous leg ulcers can become extremely painful and result in cellulitis, osteomyelitis, and even death.1 To prevent these complications, health care professionals must actively work to identify venous leg ulcers, manage exudate, and choose wound dressings that enable an optimal healing environment. This can help promote rapid healing, reduce costs, and improve quality of life for patients.1
Identifying At-Risk Patients One of the most important components of venous leg ulcer management is prevention. Venous leg ulcers are caused by inflammatory processes that lead to endothelial damage, platelet aggregation, and intracellular edema. By taking steps to identify at-risk patients and regularly assessing them for signs of ulcers, health care professionals can reduce the incidence of the disease. Older adults, obese patients, those with mobility issues, and those who have previously had a venous leg ulcer are all significantly more likely to develop venous ulcers.1
Elevate Legs Leg elevation for 30 minutes three to four times a day can help reduce edema and thus may positively affect inflammation.1
Dress the Wound Dressings aid in the treatment of venous leg ulcers by protecting the wound, preventing adherence of compression bandages, and enabling an ideal healing environment.1,5
Risk Factors And Symptoms
The incidence of venous insufficiency rises with age, and is also linked to a family history of varicose veins, a sedentary lifestyle, or to jobs that require people to spend many hours on their feet. Venous insufficiency can also be caused by a partial blockage of the veins, for example by a blood clot .
The most common early symptom of venous insufficiency is chronically swollen ankles the feet and calves may also swell. The swelling can be accompanied by a dull aching, cramping, or feeling of heaviness in the legs and feet that becomes worse after prolonged standing.
As the condition progresses, people with venous insufficiency develop brown patches and deteriorating skin around the ankles. If venous insufficiency is not treated, venous ulcers may develop on the lower legs.
Doctors use an imaging test called a duplex ultrasound to determine if there is structural damage in the veins.
Recommended Reading: What Causes Venous Leg Ulcers
Venous Insufficiency Stage 3
Venous Stasis ulcers commonly occur during the third phase of venous insufficiency, open sores that fail to heal. Venous stasis ulcers commonly begin as a small sore on the surface of the skin but can quickly expand. The most common location for venous ulcers to appear is near the ankle, but they could appear anywhere on the lower leg. Venous ulcers that form above the ankle are often the result of skin trauma or scratching. While ulcerations can cause a significant amount of pain, many find the wound itself relatively painless unless infection sets in. With proper treatment, venous ulcers can heal, but healing can take a considerable amount of time.
After The Leg Ulcer Has Healed
Once a leg has suffered a venous ulcer, there is a one in four chance of further ulceration developing within the next two years. The most effective method of preventing this is to wear a graduated elastic medical compression stocking at all times when you are out of bed. Your nurse will help you find a stocking that fits correctly and which you can manage yourself.
Various accessories are available to help you put these on and take them off.
Also Check: Signs Of Ulcerative Colitis In Child
What Types Of Wounds Can Alginate Dressings Heal
Alginate dressings usually do best on wounds that are actively giving out bodily secretions as the gel forms a shield around the sore to help soak up the secretions while keeping all other foreign bodies out of the cut, which lowers risks of infections. Alginate is also useful for wounds that are bleeding profusely as there are calcium fibers in the bandages which can break down and help slow the bleeding of a sore is bleeding heavily. Alginate dressings have long been used to dress wounds including fissures, hyper granulating tissue, interdigital maceration, heloma mole, and other lesions. Alginate dressings have also successfully been used to cover wounds on the parts of the body that are utilized the most such as on the feet. When it comes to healing venous ulcers, more studies are needed to see if Alginate dressings are effective.
If you do have venous ulcers or varicose veins, take a look at our Vein Score tool! After entering your symptoms and zip code, you will receive and vein score and a list of local vein physicians.
Medically reviewed by Dr. Susanne Woloson on 5-01-2020.
*Disclaimer: We are a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for us to earn fees by linking to Amazon.com and affiliated sites.
Medically reviewed by Dr. Susanne Woloson on May 5, 2020
What Can Cause Leg Ulcers
Venous hypertension / insufficiency the most common cause of poor healing on the lower leg is venous hypertension. This is when the veins struggle to take the blood back up the leg, so the blood can pool at the ankle creating pressure in your veins
Peripheral arterial disease another reason why our lower leg wound might not be healing is because not enough blood is getting down to our feet to heal the wound. This is then the opposite of the problem described above with veins.
Diabetes peripheral arterial disease is a known complication of diabetes, which can lead to developing a leg ulcer or diabetic foot ulcer.
Also Check: Can Ulcerative Colitis Cause Eye Problems
Preventing A Venous Leg Ulcer
You can help to prevent a venous leg ulcer in several ways, such as wearing a compression stocking, losing weight and taking care of your skin.
People most at risk of developing a venous leg ulcer are those who have previously had an ulcer. Once a leg has suffered a venous ulcer, there is a one in four chance of further ulceration developing within the next two years.