Antibiotic Use In Clinical Practice
Despite the scarcity of evidence supporting the effectiveness of antibiotics, they are still widely used in the treatment of chronic wounds. A Swedish audit showed 26.6% of chronic wound patients were receiving systemic antibiotics at the time of the study whereas a further 33.5% not receiving antibiotics at the time of the study, had done so in the previous 6 months. In total, therefore, 60.1% of chronic wound patients had received at least one antibiotic in the 6month period.
In the UK, investigation of the prescription of antibiotics for chronic wounds of all aetiologies in the community using the General Practice Morbidity Database for Wales for the year 2000 found that over two-thirds of patients with chronic wounds received at least one systemic antibiotic during the year, compared with less than one-third of age, sex and general-practice matched non-wound patients. Chronic wound patients received significantly more antibiotics than matched non-wound patients: means of 2.3 and 0.6 antibiotic prescriptions per person per year, respectively .
Infection Status Of Chronic Wounds
The interaction between ulcer and bacteria can be stratified into four levels: contamination, colonization, critical colonization and infection. Whilst, contamination and colonization by microbes are not believed to inhibit healing, the line between colonization and infection can be difficult to define. The term critical colonization has been used to describe the stage at which bacteria begin to adversely affect wound healing. Moreover, the underlying pathogenesis of chronic wounds may result in wounds of different aetiologies being differently affected by bacteria.,,
A range of clinical criteria have been used to define infection in chronic wounds. The Consensus Development Conference on Diabetic Foot Wound Care agreed that a DFU should be considered infected when there are purulent secretions or the presence of two or more signs of inflammation . Guidelines for the management of chronic venous leg ulcers produced by the British Association of Dermatologists and the Royal College of Physicians, recommend that infection should be considered if one of the following is present: pyrexia, increased pain, increasing erythema of surrounding skin, lymphangitis or rapid increase in ulcer size. It is accepted that chronic wounds by their very nature may not always display the classic symptoms of infection and it has been suggested that an expanded list, including signs specific to secondary wounds be employed to identify infection.
Also Check: Ulcerative Colitis And Lung Disease
Experimental Groups And Medications
Eighty four adult Albino Rats of both sexes , were used in this study for both wound healing and ulcer prevention experiment. Rats were divided into 7 equal groups each of six rats for each experiment. As For Ulcers, rats in group one were considered as control-negative and received orally 0.5ml of D.W. Group two received Amoxicillin-LDH Nano composite at dose of 40mg/kg B.wt., Group three administered Amoxicillin drug alone also at dose of 40mg/kg B.wt., Group four was treated with Doxycycline-LDH Nano composite at dose of 5mg/Kg B.wt., and Group five received Doxycycline alone at the same dose, Rats in group six were considered a Standard Group that received Ranitidine for ulcer study while using Fucidine ointment for wound healing. Rats in group seven were treated with LDH material by a dose of 5mg/kg B.wt.
All groups including the control-group were treated orally with stomach tube gavage daily for 7 continuous days for ulcer study. All drugs were made in the form of an ointment 10% based on Vaseline and were applied on the wound area for continuous 18 days.
Don’t Miss: What Foods Should You Avoid If You Have Ulcerative Colitis
Review Of Key Questions
For all EPC reviews, key questions were reviewed and refined as needed by the EPC with input from Key Informants and the Technical Expert Panel to assure that the questions are specific and explicit about what information is being reviewed. In addition, for Comparative Effectiveness reviews, the key questions were posted for public comment and finalized by the EPC after review of the comments.
Recommended Reading: Stomach Ulcer Blood In Stool
Medical History And Examination

Your GP or practice nurse will ask whether you have any other symptoms associated with venous leg ulcers, such as:
- swelling in your ankles
- discoloured or hard skin
They’ll try to determine the cause of the ulcer by asking about underlying conditions or previous injuries, such as:
Read more about how venous leg ulcers are treated.
Don’t Miss: How Do You Get Ulcers In Your Colon
Iodine And Silver Preparations:
Several new formulations of older topical agents should be considered to treat nonhealing wounds with or without evidence of clinical infection . Iodine, while toxic in high concentrations to tissue in vitro, can be beneficial at low doses. Cadexomer iodine releases low levels slowly into wounds and has been shown to be safe and effective at decreasing bacterial burden in the superficial compartment. Cadexomer iodine is available as an ointment and as an impregnated gauze dressing.
Silver preparations have been used on ulcers for many years. Nanocrystalline silver can deliver topical concentrations to the superficial compartment that are effective against a range of organisms, including yeast., Use of iodine and silver-containing preparations is summarized in .
Synthesis Of Ldh Doxycycline/ldh And Amoxicillin/ldh
Mg 2.6H2O and Al 3.9H2O were dissolved in 100mL distilled water. Sodium hydroxide was added dropwise until complete precipitation at pH 10.0. The precipitate suspension was stirred for 20h at 65°C, filtered, washed several times with double-distilled water and finally dried at 40°C.
Doxycycline-LDH was synthesized by repeating the same procedures and adding 0.005mol of doxycycline to the medium before precipitation. The doxycycline-LDH-precipitate suspension was stirred at room temperature for 20h, filtered, washed, and dried at 40°C. Amoxicillin-LDH was synthesized by adding a solution of amoxicillin to Mg: AL LDH for 24h at room temperature. The precipitate was filtered, washed and dried at 40°C. All steps are shown in Scheme .
You May Like: Ulcerative Colitis What Vitamins Can I Take
Recommendations For Antibiotic Treatment
Numerous recommendations exist regarding the use or avoidance of antibiotics for chronic skin wounds, and these differ according to ulcer aetiology. Importantly, there is a much lower tolerance of suspected infection in diabetic foot ulcers due to the risk of amputation and subsequent morbidity and mortality. Thus, the early use of antibiotics at signs of infection is generally advocated,, with some even advocating their use in uninfected ulcers. In contrast, recommendations with regard to venous ulcers advocate antibiotic use solely in the presence of clinical signs or symptoms of infection.,
Also Check: What Causes Mouth Ulcers On Gums
Guideline: Prescribing For Leg Ulcers
13 August 2020
The guideline
NICE has released guidelines with advice on antimicrobial prescribing for leg ulcers. It sets out a strategy for optimising antibiotic use and reducing unnecessary prescriptions, pointing out that while most leg ulcers will be colonised by bacteria, few become clinically infected.
Key points on prescribing for GPs
Dont take a sample from a leg ulcer for microbiological testing at first presentation.
Only offer antibiotics if there are signs of infection, including redness or swelling extending beyond the ulcer, localised warmth, increased pain or fever.
Offer antibiotics based on the severity of symptoms, the risk of the patient developing complications and previous antibiotic use.
When prescribing for an infected ulcer, advise the patient to seek help if their symptoms worsen or do not improve over the next two or three days.
Prescribe oral flucloxacillin 500mg-1g, four times a day for seven days as first line.
If there is penicillin allergy, prescribe oral doxycycline 200mg on the first day, then 100mg once a day for the next six days.
Prescribe oral co-amoxiclav 500/125mg, three times a day for seven days as second line.
Reassess an infected leg ulcer if there is no improvement after two or three days or if the patient becomes systemically unwell or has severe pain.
Practical issues
Also Check: Can Diverticulitis Cause Ulcerative Colitis
Recommended Reading: What Foods To Avoid With Peptic Ulcer
Risk Of Bias In Included Studies
Details of the risk of bias assessment for each included RCT are shown in the tables of . A crosstabulation of individual trial data with each risk of bias domain is shown in . shows the overall information on risk of bias.
1. Adequacy of randomisation
Ten RCTs were judged as using a satisfactory method of sequence generation and were deemed to be at low risk of bias for this domain. Specific methods included random number tables , computerised randomisation , and a remote, independent randomisation service . The remaining 35 RCTs did not specify the method of randomisation and were classified as having an unclear risk of bias.
2. Adequacy of allocation concealment
Six RCTs reported the use of an adequate method of allocation concealment such as sequentially numbered, sealed, opaque envelopes , sequentially numbered drug containers of identical appearance and a centralised, remote allocation service all were classified as low risk. Information from two RCTs suggested that the group allocation process could have been visible and so they were judged to be at high risk of bias . None of the other trials provided a clear description of allocation concealment and so were graded as unclear.
3. Blinding of participants
4. Blinding of outcome assessors
5. Incomplete outcome data addressed
6. Incomplete outcome data addressed
7. Incomplete outcome data addressed
8. Comparability at baseline
You May Like: Hindgut Ulcers In Horses Treatment
Establishing Extent Of Infection
Early recognition of the area of involved tissue can facilitate appropriate management and prevent progression of the infection . The wound should be cleansed and debrided carefully to remove foreign bodies or necrotic material and should be probed with a sterile metal instrument to identify any sinus tracts, abscesses, or involvement of bones or joints.
Plantar foot ulcers with a deep space infection.
Figure 3.
Plantar foot ulcers with a deep space infection.
Osteomyelitis is a common and serious complication of diabetic foot infection that poses a diagnostic challenge. A delay in diagnosis increases the risk of amputation.13 Risk factors associated with osteomyelitis are summarized in Table 1.3,1316 Visible bone and palpable bone by probing are suggestive of underlying osteomyelitis in patients with a diabetic foot infection.1314 Laboratory studies, such as white blood cell count and the erythrocyte sedimentation rate , have limited sensitivity for the diagnosis of osteomyelitis. Osteomyelitis is unlikely with normal ESR values however, an ESR of more than 70 mm per hour supports a clinical suspicion of osteomyelitis.13 Definitive diagnosis requires percutaneous or open bone biopsy. Bone biopsy is recommended if the diagnosis of osteomyelitis remains in doubt after imaging.3
Wound lacking purulence or any manifestations of inflammation
You May Like: How Much Aloe Vera Juice For Ulcers In Horses
Symptoms Of Venous Leg Ulcers
Venous leg ulcers are open, often painful, sores in the skin that take more than a month to heal. They usually develop on the inside of the leg, just above the ankle.
If you have a venous leg ulcer, you may also have:
- swollen ankles
- discolouration and darkening of the skin around the ulcer
- hardened skin around the ulcer, which may make your leg feel hard or even resemble the shape of an upside-down champagne bottle
- a heavy feeling in your legs
- aching or swelling in your legs
- red, flaky, scaly and itchy skin on your legs
- swollen and enlarged veins on your legs
- an unpleasant and foul-smelling discharge from the ulcer
Signs And Symptoms Of Wound Infection12

RNAO Evidence Levels:
Venous ulcers, like most chronic wounds, can become infected with superficial or spreading bacteria. The validated mnemonics NERDS and STONEES classify the signs and symptoms of localized infection and spreading infection . Increased localized pain is a significant predictor of deep compartment infection.
Presence of Superficial Bacteria
- N New areas of breakdown
- E Exudate present
- E Erythema and/or Edema
In addition to recognizing the signs and symptoms of infection in venous leg ulcers, it may be helpful to obtain a culture and sensitivity using a validated method of sampling to quantify bacteria in wounds. Tissue biopsies are considered the gold standard but unfortunately are not practical in many settings. Fortunately, a linear relationship between quantitative tissue biopsy and swab for C& S taken using the Levine method of sampling has been validated and is recommended for assessing any open wound. Swabs for C& S are important in determining the type of bacteria and the appropriate antibiotics, but are not necessary to confirm the presence or absence of infection. The C& S results may not reflect the presence or absence of biofilm.
Levine Method for obtaining C& S laboratory swab
Recommended Reading: Antibiotics For Colitis Flare Up
Also Check: Why Does Ulcerative Colitis Happen
F Grading The Evidence For Each Key Question
At the completion of our review, at least two reviewers will independently assign evidence grades. Conflicts will be resolved through consensus or third-party adjudication. We will grade the strength of evidence based on the quantity, quality, and consistency of the best available evidence, addressing KQs 1, 2, and 3 by adapting an evidence grading scheme recommended in the Methods Guide.13 We will apply evidence grades to the bodies of evidence about each intervention comparison for each outcome. We will assess the risk of bias of individual studies according to study design characteristics, such as confounding and selection and information biases. We will assess the strength of the best available evidence by assessing the limitations to individual study quality , consistency, directness, precision, publication bias, and the magnitude of the effect.
We will classify evidence pertaining to the KQs into four basic categories: 1) high grade 2) moderate grade 3) low grade and 4) insufficient grade .
How Venous Leg Ulcers Are Treated
Most venous leg ulcers heal within 3 to 4 months if they’re treated by a healthcare professional trained in compression therapy for leg ulcers. However, some ulcers may take longer to heal, and a very small number never heal.
Treatment usually involves:
- cleaning and dressing the wound
- using compression, such as bandages or stockings, to improve the flow of blood in the legs
Antibiotics may also be used if the ulcer becomes infected, but they don’t help ulcers to heal.
However, unless the underlying cause of the ulcer is addressed, there’s a high risk of a venous leg ulcer recurring after treatment. Underlying causes could include immobility, obesity, previous DVT, or varicose veins.
Recommended Reading: What Causes Ulcers In Your Mouth
Referral To A Specialist
In some cases, your GP or nurse may decide to refer you to a specialist in conditions affecting the blood vessels .
For example, you may be referred to a vascular specialist if your GP or nurse is unsure about your diagnosis, or if they suspect your ulcer may be caused by artery diseases, diabetes or rheumatoid arthritis.
After taking your medical history and examining you, the vascular specialist may need to arrange further investigations to plan your treatment.
After The Ulcer Has Healed
Once you have had a venous leg ulcer, another ulcer could develop within months or years.
The most effective method of preventing this is to wear compression stockings at all times when youre out of bed.
Your nurse will help you find a stocking that fits correctly and you can manage yourself.
Various accessories are available to help you put them on and take them off.
Page last reviewed: 11 January 2019 Next review due: 11 January 2022
You May Like: What Not To Eat If You Have An Ulcer
Treating An Infected Ulcer
An ulcer sometimes produces a large amount of discharge and becomes more painful. There may also be redness around the ulcer.
These symptoms and feeling unwell are signs of infection.
If your ulcer becomes infected, it should be cleaned and dressed as usual.
You should also elevate your leg most of the time. You’ll be prescribed a 7-day course of antibiotics.
The aim of antibiotic treatment is to clear the infection. But antibiotics do not heal ulcers and should only be used in short courses to treat infected ulcers.
What Are The Symptoms Of Leg Ulcers
The main symptom of a leg ulcer is a deep sore on the leg. You might also have:
- bad-smelling fluid weeping from the wound
- injury to the leg
- an infection
Older people are more at risk of developing a leg ulcer. You are also more at risk if you have diabetes or high blood pressure, if you are obese, or if you are a smoker.
You May Like: Can You Drink Coffee With Ulcerative Colitis
Do Not Take A Swab Or Use Antibiotics For The Management Of A Leg Ulcer Without Clinical Infection
Lower leg ulcers, most commonly venous ulcers are often treated with oral antibiotics, even in the absence of evidence of clinical infection. There is no evidence to support this use, except if screening for carriage of multi-resistant organisms. Also a swab for microscopy and culture, in the absence of signs of infection is not recommended. Unnecessary antibiotics and swabbing will add to healthcare costs, antimicrobial resistance and patient allergy.
Supporting evidence
- OMeara S, Al-Kurdi D, Olugun Y, Antibiotics and antiseptics for Venus ulcers. Cochrane Database Systematic Review 2014 CD003557.
- Hansson C, Hoborn J, Moller A, Swanbeck G. The microbial flora in venous leg ulcers without clinical signs of infection. Repeated culture using a validated standardised microbiological technique. Acta Dermato Venereologica 1995 75:24.
An initial list of 10 low value interventions was compiled by the Lead Fellow of the Australasian Society for Infectious Diseases Inc following an online discussion in ASIDâs discussion forum, Ozbug. The Royal Australasian College of Physicians then facilitated a consultation of all ASID members via a survey distributed through the societys e-newsletter. In the survey, members were asked to rank the 10 suggested interventions and suggest additional items for consideration. A subsequent shortlist of items was created by selecting the top 7 interventions as ranked by the members from the initial list.
Should Leg Ulcers Be Kept Dry
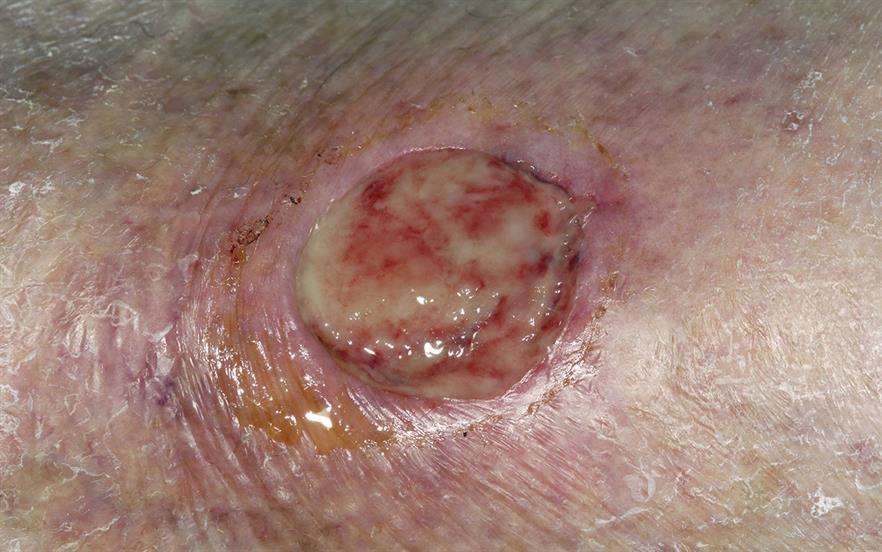
Low oxygen tension leads to high levels of oxygen at the capillaries and low levels of oxygen at the wound edges. This provides the ideal environment for wound healing because granulation and wound healing is stimulated. a wound, nurses should remember: If theres no blood supply keep it dry and seek expert advice.
Read Also: Best Alcohol To Drink With Ulcerative Colitis