Ways To Treat Venous Leg Ulcer
Learn how to treat venous leg ulcers now.
1. Clean and Dress the Ulcer
One of the most important first steps is to clean and dress the ulcer. With any abrasion of the skin, you want to make sure the wound is cleaned.
Improper wound care can allow bacteria to gather in the wound, which then leads to infection. If your ulcer becomes infected, you might have to take antibiotics to kill the bacteria.
To clean the ulcer, run it under cold water with a damp washcloth before using an anti-infection cream. Since the wound breaks the skin, cover it with a bandage.
You should be able to find bandages and anti-infection creams at your local drugstore. Its also possible to make homemade bandages by taping down a pad of sterile gauze.
As the ulcer takes an increased amount of time to heal, be sure to intermittently replace the bandage and make sure the wound is still clean.
2. Compression Socks and Bandages
The most common treatments to address a venous leg ulcer are compression socks and bandages. Compression socks can also be found at your local drugstore.
These stockings gently compress the legs and narrow blood vessels, causing blood circulation to improve. It will also help decrease leg swelling. If you get a notice from your doctor that you have a medical reason for the compression socks, it may be possible to get a reimbursement from your insurance company.
3. Elevate the Legs
4. Moisturize to Reduce Itchy Skin
5. Stay Active Through Walking
Elevation Of The Legs
The legs should be placed in an elevated position, ideally at 30 degrees to the heart, while lying down. This, again, helps in the movement of venous blood to the heart.This also prevents the build-up of liquid in the legs that leads to swelling. A cushion or any other object of comfort can be used to keep the toes above the level of the hip while sleeping.
Why Is It Important To Seek Venous Ulcer Treatment
Venous ulcers dont heal on their own. The longer you live with them, the greater the likelihood of permanent tissue damage. The damage can spread or cause infections that can become life- or limb-threatening, such as gangrene.
In severe cases, it may be necessary to surgically remove your affected limb. Timely care from an experienced wound care provider significantly lowers this risk.
Recommended Reading: Quitting Smoking And Ulcerative Colitis
Dressings And Topical Agents
Dressings are usually applied to open ulcers. As well as offering protection, dressings may be chosen for other reasons, such as antimicrobial properties or absorption of exudate. As well as a wide range of types of dressings available, there are a number of topical products, used to reduce infection riskA way of expressing the chance of an event taking place, expressed as the number of events divided by the total number of observations or people. It can be stated as the chance of falling were one in four . This measure is good no matter the incidence of events i.e. common or infrequent., aid exudate absorption or promote wound healing by other means, as well as topical painkilling agents. Having reliable evidence to guide choices is important.
The authors of the Cochrane Review Dressings and topical agents for treating venous leg ulcers conducted a network meta-analysisThe use of statistical techniques in a systematic review to combine the results of included studies. Sometimes misused as a synonym for systematic reviews, where the review includes a meta-analysis. on dataData is the information collected through research. from 59 of the 78 studies included in the review . Unfortunately, it highlights continued uncertainty about whether particular dressings or topical agents improve the likelihood of healing. You can listen to a Cochrane podcast about this review.
Helping The Ulcer Heal
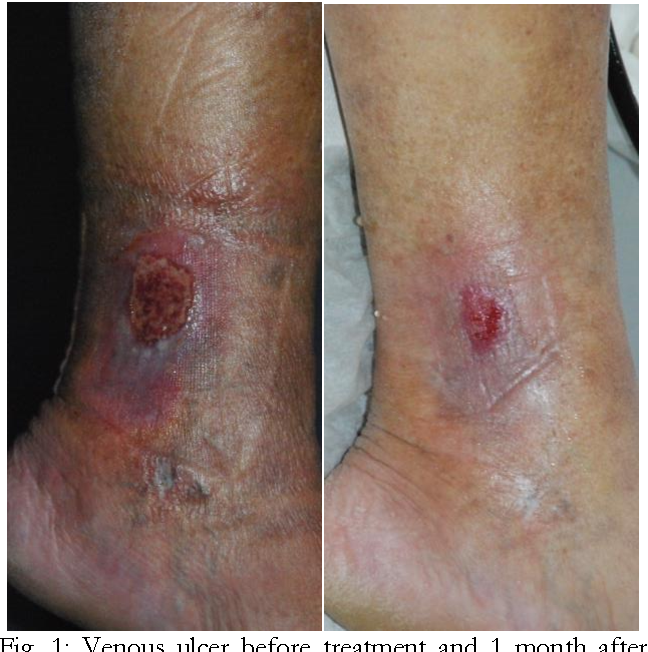
You May Like: Zinc Oxide For Stage 2 Pressure Ulcer
Why It Is Important To Do This Review
Wound cleansing is used as a component of venous leg ulcer management to prepare the wound before dressings and bandages are used. It has been suggested that failure to cleanse the wound and limb appropriately may have negative effects on healing time and infection risk. Wound cleansing is recommended in many international guidelines but an ongoing review of the evidence for this procedure is important in terms of its value, and the best approaches in terms of methods and solutions that, it has been suggested, are often based on ritualistic practice, with little consideration given to the potential research evidence to support or refute the chosen method or solution of cleansing . For this reason we aimed to include studies of cleansing versus no cleansing in addition to studies comparing different wound cleansing solutions and techniques with each other.
The ability to manage increasing demands on the health service is greatly influenced by the available resources . It is unlikely that there will ever be enough revenue to meet all healthcare challenges therefore the development of costeffective patient care delivery programmes is central to ensuring sustainability in healthcare delivery into the future . For individuals with leg ulceration this means all aspects of care should be effective, efficient and based on the best available evidence. This systematic review presents the evidence for approaches to wound cleansing for venous leg ulceration.
From Blood Flow To Compression Get A Holistic View Of Venous Stasis
Lower extremity venous disease affects millions of Americans and may ultimately lead to open, draining wounds that adversely affect quality of life. However, there are exciting developments in early diagnosis, prevention and treatment of venous leg ulcers . On the chronic venous insufficiency treatment side, there are more choices now than ever before in compression products, which is greatly improving the patient experience. But proper treatment also comes from a better understanding of venous leg ulcers, and better understanding comes from more education. This article covers six things to help empower and educate your team when treating chronic venous insufficiency and resulting VLUs.
Read Also: List Of Foods To Avoid With Ulcerative Colitis
What Causes Foot And Toe Ulcers How Do You Get An Ulcer
There are many possible causes. The most common include:
- Neuropathy from diabetes.
- Peripheral arterial disease.
- Walking in an odd way where you put too much pressure on one part of your foot or toe.
- Friction. Your foot or toe may rub against the toebox of your shoe.
Although they dont cause ulcers, foot and toe ulcers are often found alongside toe deformities such as hammertoe, mallet toe and clawtoe.
Avoid Sitting Or Standing For Long Hours
Being stationary for long hours leads to pooling of blood in the legs and development of venous leg ulcers.
Walking or moving the legs at regular intervals improves blood circulation and aids in pushing the blood in the veins up to the heart. Even moving the legs slightly helps in the circulation of blood.
You May Like: What Is The Treatment For Stomach Ulcers
What Is The Best Way To Heal A Leg Ulcer
Latest research confirms that the fastest way to heal the commonest type of leg ulcer is Early endovenous ablation of superficial venous reflux, in addition to compression therapy and wound dressings.
This method reduces the time to healing of venous leg ulcers, increases ulcer-free time and is highly likely to be cost-effective .
What Venous Ulcer Treatments Might I Need
The therapies that are best for you depend on the location and severity of the ulcer. Care typically includes frequent follow-up appointments to ensure treatments are working.
Venous ulcer treatments often include:
- Antibiotics if theres an infection.
- Compression bandages or stockings to improve circulation.
- Ointments that protect against germs.
- Pain relievers and other therapies to quiet overactive nerves.
- Procedures to remove debris and dead tissue.
- Referrals to specialists if you need help managing chronic conditions, such as diabetes.
- Special bandages and dressings to keep the ulcer covered.
- Wound cleaning daily to flush out bacteria and remove dead tissue.
Read Also: How Do You Test For An Ulcer In The Stomach
Symptoms Of Venous Leg Ulcers
Venous leg ulcers are open, often painful, sores in the skin that take more than a month to heal. They usually develop on the inside of the leg, just above the ankle.
If you have a venous leg ulcer, you may also have:
- discolouration and darkening of the skin around the ulcer
- hardened skin around the ulcer, which may make your leg feel hard or even resemble the shape of an upside-down champagne bottle
- a heavy feeling in your legs
- aching or swelling in your legs
- red, flaky, scaly and itchy skin on your legs
- swollen and enlarged veins on your legs
- an unpleasant and foul-smelling discharge from the ulcer
Cleveland Clinic Heart Vascular & Thoracic Institute Vascular Medicine Specialists And Surgeons
Choosing a doctor to treat your vascular disease depends on where you are in your diagnosis and treatment. The following Heart, Vascular & Thoracic Institute Sections and Departments treat patients with all types of vascular disease, including blood clotting disorders:
Section of Vascular Medicine: for evaluation, medical management or interventional procedures to treat vascular disease. In addition, the Non-Invasive Laboratory includes state-of-the art computerized imaging equipment to assist in diagnosing vascular disease, without added discomfort to the patient. Call Vascular Medicine Appointments, toll-free 800-223-2273, extension 44420 or request an appointment online.
Department of Vascular Surgery: surgery evaluation for surgical treatment of vascular disease, including aorta, peripheral artery, and venous disease. Call Vascular Surgery Appointments, toll-free 800-223-2273, extension 44508 or request an appointment online.
You may also use our MyConsult second opinion consultation using the Internet.
The Heart, Vascular & Thoracic Institute also has specialized centers and clinics to treat certain populations of patients:
Recommended Reading: What Foods Irritate Stomach Ulcers
Treating An Infected Ulcer
An ulcer sometimes produces a large amount of discharge and becomes more painful. There may also be redness around the ulcer. However redness may be harder to see on black or brown skin.
These symptoms and feeling unwell are signs of infection. You should contact your GP or leg ulcer specialist as soon as possible.
If your ulcer becomes infected, it should be cleaned and dressed as usual.
You should also elevate your leg most of the time. You’ll be prescribed a 7-day course of antibiotics.
The aim of antibiotic treatment is to clear the infection. But antibiotics do not heal ulcers and should only be used in short courses to treat infected ulcers.
How The Intervention Might Work
Compression bandaging is the gold standard for the management of ambulatory people with venous leg ulceration. Compression bandaging attempts to reverse the effects of venous insufficiency and the evidence suggests that there is an increased rate of wound healing using compression therapy . However, before application of the compression bandaging, it may be important to ensure the wound bed is free from contaminants and devitalised tissue, and wound cleansing could be central to achieving this . It has been suggested that failure to cleanse the wound bed sufficiently may lead to delayed healing, attributed to a number of important factors, including the presence of foreign bodies, necrotic or sloughy tissue and bacterial burden or biofilm and attached to the wound bed) . It is suggested that these factors lead to the increased production of metalloproteases within the wound . These enzymes are produced during wound healing, but when present for prolonged periods or in excess amounts, metalloproteases may become detrimental to healing tissue . Wound cleansing in the form of swabbing, irrigation, or washing the wound bed may contribute to reducing or eliminating some of these factors, thereby enhancing wound healing potential.
You May Like: What Foods To Eat With Ulcerative Colitis
When To Seek Medical Care
Will I Need Any Tests
Testing lets your healthcare provider know how severe the ulcer is. You may also undergo regular testing to determine whether venous ulcer treatments are working.
Tests for venous ulcers include:
- Ankle-brachial index, which takes blood pressure readings of your arms and legs.
- Doppler study to listen to blood flowing through your veins.
- Imaging studies, such as a CT scan to identify damaged or nonfunctioning valves.
Don’t Miss: Is Greek Yogurt Good For Ulcerative Colitis
What Is A Leg Ulcer
A leg ulcer describes a break in the skin, which allows air and bacteria to get into the leg. This is often caused by an injury, usually a minor one that cuts or grazes the skin.
In healthy people such an injury heals up quickly within a week or two. However, if the person has an underlying health problem, the skin does not heal and the area of breakdown can increase in size. This is what is meant by the term chronic leg ulcer.
All leg ulcers are a problem because they cause pain, disability and social isolation. In younger people, they can lead to time off work and sometimes loss of employment. All leg ulcers should be referred to a specialist team for assessment and treatment if they do not heal within 2 weeks.
Signs Of An Infection
A venous leg ulcer can be susceptible to bacterial infection. Symptoms of an infected leg ulcer can include:
A number of factors can increase your risk of developing a venous leg ulcer, including:
- obesity or being overweight this increases the pressure in the leg veins
- if you have difficulty walking this can weaken the calf muscles, which can affect circulation in the leg veins
- previous deep vein thrombosis blood clots that develop in the leg can damage valves in the veins
- varicose veins swollen and enlarged veins caused by malfunctioning valves
- previous injury to the leg, such as a broken or fractured bone, which may cause DVT or impair walking
- previous surgery to the leg, such as a hip replacement or knee replacement, which can prevent you from moving about
- increasing age people find it harder to move around as they get older, particularly if they suffer from arthritis
You May Like: Best Dressing For Stage 2 Pressure Ulcer On Buttocks
Infographic Excerpt: Other Home Remedies To Heal Leg Ulcers
Leg ulcers are majorly caused by injuries. While these often heal on their own, they also may warrant medical compliance and remedies to ease the discomfort.
The following infographic provides information about a few other remedies that can ease leg ulcers and promote healing. Check them out.
Illustration: StyleCraze Design Team
Leg ulcers resemble sores that develop when bacteria enter underlying tissues through injured or broken skin. While skin injuries are the most common risk factor for leg ulcers, certain underlying medical conditions like diabetes, arterial disease, and venous disease may also lead to leg ulcers. Some common signs and symptoms that often accompany leg ulcers include irritated or flaky skin, swelling, heaviness, discoloration, and leg pain on prolonged standing. You may use natural ingredients like Gotu kola, turmeric, aloe vera, coconut oil, tea tree oil, and yarrow in home remedies to heal leg ulcers in mild to moderate cases.