Extraintestinal Manifestations And Complications
UC is characterized by immune dysregulation and systemic inflammation, which may result in symptoms and complications outside the colon. Commonly affected organs include: eyes, joints, skin, and liver. The frequency of such extraintestinal manifestations has been reported as between 6 and 47%.
UC may affect the mouth. About 8% of individuals with UC develop oral manifestations. The two most common oral manifestations are aphthous stomatitis and angular cheilitis. Aphthous stomatitis is characterized by ulcers in the mouth, which are benign, noncontagious and often recurrent. Angular chelitis is characterized by redness at the corners of the mouth, which may include painful sores or breaks in the skin. Very rarely, benign pustules may occur in the mouth .
UC may affect the eyes. Inflammation may occur in the interior portion of the eye, leading to uveitis and iritis. Uveitis can cause blurred vision and eye pain, especially when exposed to light . Untreated, uveitis can lead to permanent vision loss. Inflammation may also involve the white part of the eye or the overlying connective tissue , causing conditions called scleritis and episcleritis. Uveitis and iritis are more commonly associated with ulcerative colitis, whereas episcleritis is more commonly associated with Crohn’s disease.
What Are Ulcerative Colitis Symptoms
Ulcerative colitis is an inflammatory bowel disease that can be life-threatening when the symptoms flare up. Its important for you to go to the hospital for treatment when your symptoms are too severe.
The condition doesnt have a cure, but it can have periods where the symptoms become extreme and flare-up or where they go into remission.
At least 25% of all cases of ulcerative colitis lead to hospitalization. You may need to be hospitalized many times throughout your life for this condition, particularly during flare-ups.
The main way to manage the disease is by taking an oral corticosteroid, typically in the form of a daily pill. You need to seek medical attentionand will likely be hospitalizedwhenever your body isnt responding to this treatment.
Ulcerative colitis usually begins with inflammation at the base of your colon. Over time, this inflammation can spread up the organ until the entire large intestine is affected.
This leads to many different symptoms, including:
Over long periods of time, ulcerative colitis can lead to further complications, including:
When Are Your Symptoms Severe Enough For Hospitalization?
Youll experience your ulcerative colitis symptoms on and off throughout your life. You should always contact your doctor when you have concerns about your symptoms or if new ones develop.
You should seek inpatient treatment at a hospital whenever:
Foods That May Fight Uc
Some research shows that certain nutrients may help fight the irritation and swelling in your gut caused by UC. Scientists have studied how linoleic acid affects people with the condition. Although everyone needs this good fat, donât overdo it, since there is some evidence it may play a role in inflammation if you get too much.
Other studies show that an omega-3 fatty acid called EPA may fight inflammation. This is another âgoodâ fat that blocks certain chemicals in your body called leukotrienes. Fish oil is a good source of EPA. In some studies, folks with UC saw some benefits when they took high doses. Many people, though, didnt like the fishy taste. There is also some evidence that adding fish oil to aminosalicylates may be helpful, but this isnât proven. DHA is another omega-3 found in fish oil that can fight inflammation and is used by some people with UC.
Some research also shows that yogurt with gut-healthy bacteria, called probiotics, eases inflammation. Scientists are still studying how they may help people with UC and similar conditions. Some people also believe that a diet low in FODMAPs a type of highly-fermentable carbs found in meats, fruits, dairy, and lots of other foods may help ease UC symptoms. But the evidence is unclear if it does. And without close monitoring, any diet that restricts certain foods may lead to poor nutrition and other problems.
Show Sources
You May Like: Foods That Heal Stomach Ulcers
How Does Pediatric Ulcerative Colitis Affect My Childs Mental/emotional Health
Like many conditions, ulcerative colitis can have a negative psychological effect, especially on children. They can experience physical, emotional, social and family problems. Because of the medications and/or general stress from the situation, your child may experience:
- Worry about appearance and physical stamina.
- Vulnerability because their body doesnt function normally.
- Poor concentration.
- Misunderstandings with friends and family.
Children need mutual support from all family members. Its helpful for the entire family to learn about the disease and try to be empathetic. Seek out a psychiatrist and therapist to help your child manage such challenges of their ulcerative colitis.
Complications Of Ulcerative Colitis
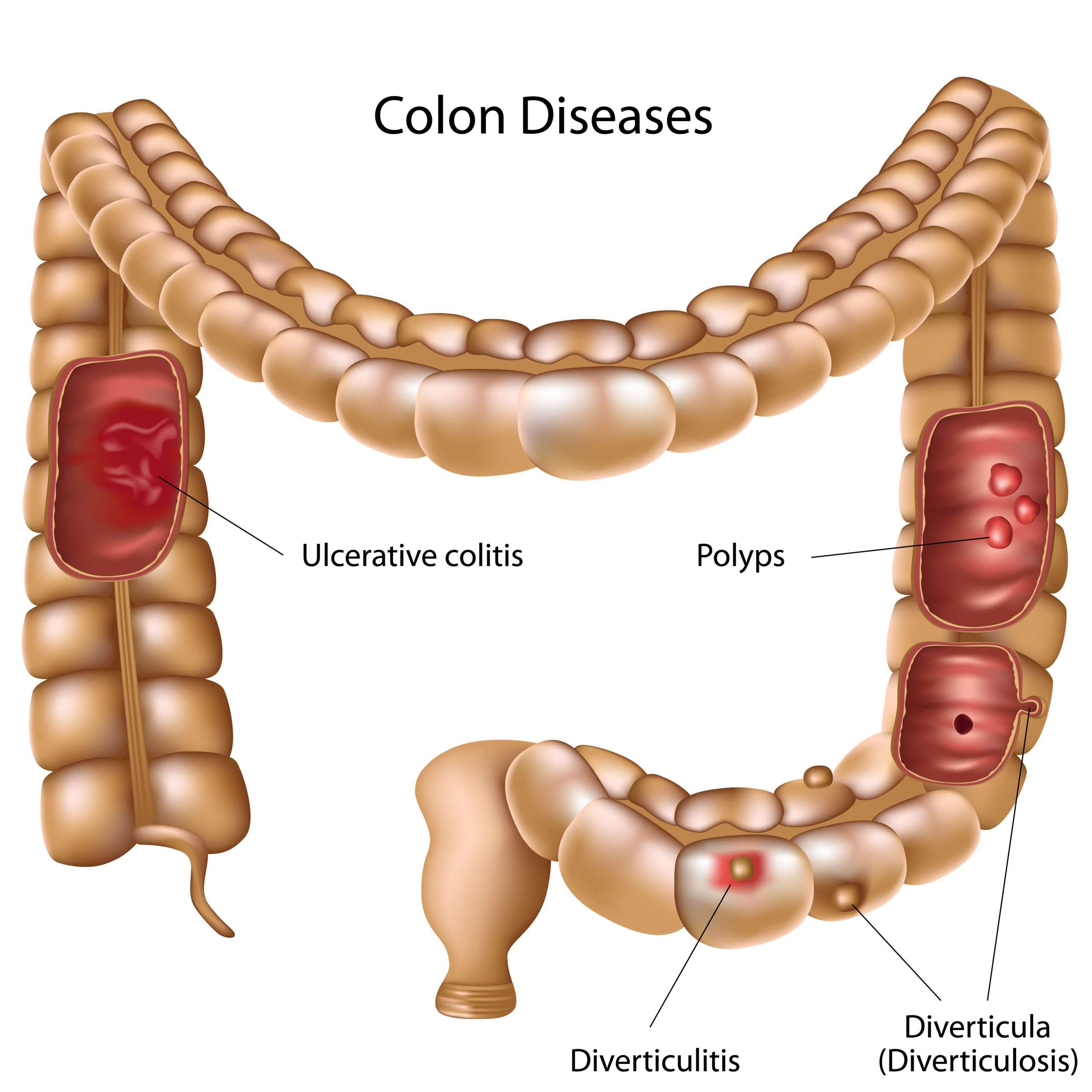
A small number of people with colitis can develop inflammation in other parts of the body, such as the liver, skin, joints and eyes.
Regular monitoring by a gastroenterologist, as well as colonoscopies, may help prevent complications from developing. But medications, including steroids and drugs designed to prevent inflammation and occasionally surgery may be needed.
Osteoporosis can develop as a side effect of long-term corticosteroid use.
Cases of marked inflammation caused by UC can also lead to:
- nutritional deficiencies
- heavy bleeding due to deep ulcers
- perforation of the bowel
- problems with the bile ducts, affecting the liver
- fulminant colitis and toxic megacolon, conditions that cause the bowel to stop working
In the long-term, UC is associated with an increased risk of developing bowel cancer. After 10 years the risk of bowel cancer is 1 in 50, and after 20 years it increases to 1 in 12. This risk can be decreased by maintaining a healthy diet, exercising and avoiding alcohol and smoking.
Also Check: Home Remedies For Stomach Ulcer Pain
What Are The Complications Of Ulcerative Colitis
Complications of ulcerative colitis can include the following:
- rectal bleedingwhen ulcers in the intestinal lining open and bleed. Rectal bleeding can cause anemia, which health care providers can treat with diet changes and iron supplements. People who have a large amount of bleeding in the intestine over a short period of time may require surgery to stop the bleeding. Severe bleeding is a rare complication of ulcerative colitis.
- dehydration and malabsorbtion, which occur when the large intestine is unable to absorb fluids and nutrients because of diarrhea and inflammation. Some people may need IV fluids to replace lost nutrients and fluids.
- changes in bones. Some corticosteroid medications taken to treat ulcerative colitis symptoms can cause
- osteoporosisthe loss of bone
- osteopenialow bone density
Health care providers will monitor people for bone loss and can recommend calcium and vitamin D supplements and medications to help prevent or slow bone loss.
- inflammation in other areas of the body. The immune system can trigger inflammation in the:
Health care providers can treat inflammation by adjusting medications or prescribing new medications.
- megacolona serious complication that occurs when inflammation spreads to the deep tissue layers of the large intestine. The large intestine swells and stops working. Megacolon can be a life-threatening complication and most often requires surgery. Megacolon is a rare complication of ulcerative colitis.
Who Develops Ulcerative Colitis
About 2 in 1,000 people in the UK develop ulcerative colitis. It can develop at any age but most commonly first develops between the ages of 10 and 40. About 1 in 7 cases first develop in people over the age of 60 years. Non-smokers are more likely than smokers to develop ulcerative colitis. However, smoking brings other dangers to health which far outweigh this benefit.
Complications of ulcerative colitis include:
- primary sclerosing cholangitis where the bile ducts inside the liver become damaged
- an increased risk of developing bowel cancer
- poor growth and development in children and young people
Also, some of the medications used to treat ulcerative colitis can cause weakening of the bones as a side effect.
Read Also: I Have Ulcerative Colitis Can I Get Disability
Why Choose Mount Sinai
Mount Sinai has a unique and rich tradition of specialized and individualized treatment and scientific research and discovery in ulcerative colitis. The physicians/scientists in the Mount Sinai Health System are constantly conducting clinical trials and are developing new drug therapies to help patients manage their disease. Learn more about ulcerative colitis.
There are 3 basic tests for colon cancer a stool test , sigmoidoscopy , and colonoscopy . All 3 are effective in catching cancers in the early stages, when treatment is most beneficial.
The esophagus, stomach, large and small intestine, aided by the liver, gallbladder and pancreas convert the nutritive components of food into energy and break down the non-nutritive components into waste to be excreted.
Ulcerative colitis is categorized according to location. Proctitis involves only the rectum. Proctosigmoiditis affects the rectum and sigmoid colon. Left-sided colitis encompasses the entire left side of the large intestine. Pancolitis inflames the entire colon.
Symptoms Of A Duodenal Ulcer
If you have a duodenal ulcer, you might:
- have pain in the stomach or abdomen
- have indigestion
Very occasionally, an ulcer can cause serious complications. Go to the emergency department if:
- you have a sharp pain in your stomach that doesnt go away
- your vomit or stools look bloody or a black colour
If you are concerned about symptoms, you can use healthdirects online Symptom Checker to get advice on the next appropriate healthcare steps and when to seek medical attention.
Also Check: Can Ulcerative Colitis Cause Heart Problems
Ibd And The Benefits Of Vinegar Diet Changes
Thinkstock
Vinegar has been around for centuries. A variation of the Old French word vinaigre , vinegar literally translates as sour wine. With seemingly countless uses , vinegar is something of a wonder product. But what about its dietary health benefits?
In January 2016 the Journal of Agricultural and Food Chemistry published an animal study that showed promising results for Inflammatory Bowel Disease. The study, led by Chinas Jilin University, looked at the effect of vinegar and its main component, acetic acid, on the gut bacteria and inflammatory markers of mice.
At the beginning of the study the mice were altered chemically to develop ulcerative colitis . Small amounts of vinegar or acetic acid were given to the mice and changes in inflammatory markers and gut bacteria were measured through colon inflammation and stool bacteria. Both substances, the vinegar and the acetic acid, improved the symptoms of UC as well as reducing inflammation in the colon and improving the gut bacteria .
While the study looks promising, further research is needed to see if these results can be repeated in human subjects.
So, what does that all mean for current IBD patients? First things first: discuss any changes you intend to make to your diet with your physician. If you get the go-ahead from your doc, then you can start to add vinegar to your diet.
Meet Our Writer
Jennifer Mitchell Wilson
Doctors Told How To Protect Yourself From Ulcerative Colitis
A campaign has been launched in Yekaterinburg, the goal of which is to educate the Urals people about inflammatory bowel diseases . Doctors told how to diagnose an incipient ailment and what actions to take to avoid it altogether.
Ulcerative colitis and Crohns disease are among the most severe diseases, but their detection rate is poor.According to doctors forecasts, almost 35 thousand patients with IBD live in the Sverdlovsk region, but only 500 cases are officially known. Doctors hope to help people diagnose the disease on their own in the early stages and prevent severe forms.
In IBD, the immune system begins to work against the body, resulting in a very specific inflammatory process. In ulcerative colitis, the disease mainly affects the mucous membrane, and in Crohns disease, all layers of the intestine, which makes its treatment more difficult.In this case, ulcers can occur at the site of inflammation, which lead to abscesses, and the prolonged course of IBD contributes to the development of intestinal cancer and increased mortality. In the case of Crohns disease, inflammatory processes begin in other organs as well joints, vision, skin, mucous membranes of the mouth are affected.
According to European statistics, 505 people out of 100,000 suffer from ulcerative colitis, and 322 people suffer from Crohns disease.
Don’t Miss: Differential Diagnosis For Ulcerative Colitis
Radiology Scans Or Diagnostic Imaging
Traditional upper GI endoscopy and colonoscopy are not be able to reach about two-thirds of the small intestine. Therefore, in addition to capsule endoscopy, various radiologic exams or diagnostic imaging may be performed to evaluate these parts of the intestines as well as to evaluate the actual wall of the bowel and surrounding areas outside the bowel.
X-rays
X-rays are the oldest way of imaging the inside of the body. X-rays are cost-effective and useful for detection of blockages in the small or large intestine.
Barium contrast studies
During a barium study, you will ingest a contrast material and have images taken with traditional X-ray technology. Barium is a chalky/milky liquid that you drink prior to the procedure. A series of X-rays are taken to observe the material flowing through the digestive system. These studies include:
Upper GI series examines the esophagus, stomach, and first part of the small bowel for patients with Crohns disease
Small bowel series and small bowel enteroclysis examines the entire small bowel. For a small bowel series, you will drink several cups of barium, and then have an X-ray taken every 1530 minutes as the barium travels down the small intestine and enters the large intestine. The time required varies but may take four to five hours. An enteroclysis is similar, except that the barium is placed directly into the small intestine through a tube introduced into the GI tract via the nose or mouth.
Cross-sectional imaging
Is There An Ulcerative Diet Listing Foods To Avoid And Foods That Relieve Symptoms
Proper nutrition is important for a person with ulcerative colitis. Foods do not cause ulcerative colitis, but certain food groups can cause symptoms to flare. Often it is a process of trial and error to find what foods need to be avoided. Although specific foods do not cause the disease, some types of food may trigger discomfort and diarrhea. Keep a food diary to help find foods that cause problems.
Counseling and education are important for both the patient and family a better understanding of how ulcerative colitis affects the body will allow the patient and physician to work together to control the symptoms.
Also Check: Can Ulcers Cause Weight Loss
What Are The Most Effective Treatments For Ulcerative Colitis
There are a variety of factors that can determine whether a specific medication can be effective at treating UC. Here are the most common medications for UC:
- 5-amino salicylic acid . This is the first-line treatment for UC. Commonly used medications are sulfasalazine, mesalamine, balsalazide, and olsalazine. The particular 5-ASA medication prescribed to a person with UC depends on the area of the colon thats affected by the condition.
- Corticosteroids. Corticosteroids, such as prednisone and budesonide, are another treatment for UC. These drugs cause significant side effects when used for longer periods, so theyre used only for moderate to severe illness.
- Immunomodulators. These medications minimize inflammation by controlling the immune response. Some common examples include cyclosporine, which is only used in short durations, as well as azathioprine and mercaptopurine. These two medications can cause side effects in the liver and require close monitoring of the blood by a physician.
- JAK inhibitors. The JAK inhibitor tofacitinib was approved recently for use in UC. It blocks an enzyme that can trigger inflammation.
- Biologics. Infliximab, adalimumab , and golimumab work by neutralizing proteins produced by the immune system. Another biologic, vedolizumab , targets the gut and helps reduce inflammation.
Untreated UC may progress over time, potentially becoming difficult to treat later on.
Treating UC can help minimize the risk of developing serious complications, including:
Demographic Information And Risk Factors
94 patients who have been diagnosed with UC after the age of 65years were compared with 94 patients who have been diagnosed with UC between 40 and 64years. The demographic characteristics of both group are shown in Table . Median age at diagnosis was 71.5±5years and 50.1±6.7years in E-O and A-O, respectively . Male patients were more frequent in both groups . Family history for UC was similar in the two groups . Difference in smoking habits, althoughs not statistically significant was reported. Time between onset symptoms and UC diagnosis was similar in the two groups, 5.8±4.6months in the elderly and 6.2±4.7months in adults respectively. 34% of the elderly and 19% of the adults received a different diagnosis before UC diagnosis. The most frequent one was diverticular disease in the first group , while infectious colitis was the most common in the second group .
Table 1 Demographic characteristics of UC by age
Median follow among elderly patients up was 8.1years and 5.7years in the control group. Mortality was 20.5% in the elderly and 3.9% in adults. p< 0.0005. Main causes of death were cardiovascular disease , sepsis , extraintestinal neoplasia and respiratory failure in the elderly cardiovascular disease , sepsis and extraintestinal neoplasia in adults.
Read Also: First Signs Of Ulcerative Colitis
Which Type Of Doctor Treats Colitis
Gastroenterologists are the medical specialists that treat diseases of the gastrointestinal organs such as colitis.
- In some cases, colitis may be managed by primary care specialists or internal medicine specialists.
- Depending on the type of colitis, other specialists may be involved in the treatment, including:
- Infectious disease specialists or surgeons
- Pediatricians or pediatric gastroenterologists are involved in the care of infants, children, and teens with colitis
Tests Before Treatment Initiation
In addition to the tests used for diagnosis, some specific tests are recommended before treatment initiation. The European Crohns and Colitis Organisation recommends that pretreatment laboratory testing include electrolyte, renal function, iron level, immunization status, and vitamin D tests. See Monitoring for tests used to monitor treatment.
Anti-JC Virus Antibodies
Testing for antibodies to JC virus is recommended in patients with CD natalizumab should be used for CD treatment only in patients negative for anti-JC virus antibodies.
Thiopurine Therapy-Related Testing
Pharmacogenetic testing before treatment initiation may be helpful to guide therapeutic decisions, particularly because treatment failure due to individual differences in medication response is not uncommon in IBD. Thiopurine drugs are commonly used in treating IBD.
The American Gastroenterological Association recommends either phenotype or genotype testing in adults beginning thiopurine therapy.TPMT and NUDT15 gene variants as well as reduced TPMT enzyme activity are associated with a greater risk of myelosuppression in response to treatment with thiopurines due to accumulation of active thiopurines. Phenotype testing should not be performed in patients already receiving treatment with thiopurines because results will be falsely low. In addition, the current TPMT phenotype may not reflect the future phenotype, particularly in patients who received blood transfusions within 30-60 days of testing.
Also Check: What Foods Should I Avoid If I Have An Ulcer