Pressure Ulcers: Prevention Evaluation And Management
DANIEL BLUESTEIN, MD, MS, Eastern Virginia Medical School, Norfolk, Virginia
ASHKAN JAVAHERI, MD, Stanford University School of Medicine, Stanford, California, and Veterans Affairs Palo, Alto Health Care System, Palo Alto, California
Am Fam Physician. 2008 Nov 15 78:1186-1194.
Pressure ulcers, also called decubitus ulcers, bedsores, or pressure sores, range in severity from reddening of the skin to severe, deep craters with exposed muscle or bone. Pressure ulcers significantly threaten the well-being of patients with limited mobility. Although 70 percent of ulcers occur in persons older than 65 years,1 younger patients with neurologic impairment or severe illness are also susceptible. Prevalence rates range from 4.7 to 32.1 percent in hospital settings2 and from 8.5 to 22 percent in nursing homes.3
SORT: KEY RECOMMENDATIONS FOR PRACTICE
Compared with standard hospital mattresses, pressure-reducing devices decrease the incidence of pressure ulcers.
| Clinical recommendation | |
|---|---|
|
There is no evidence to support the routine use of nutritional supplementation and a high-protein diet to promote the healing of pressure ulcers. |
|
|
Heel ulcers with stable, dry eschar do not need debridement if there is no edema, erythema, fluctuance, or drainage. |
|
|
Ulcer wounds should not be cleaned with skin cleansers or antiseptic agents because they destroy granulation tissue. |
SORT: KEY RECOMMENDATIONS FOR PRACTICE
How Are Pressure Injuries Treated
Pressure injuries can be treated in many ways depending on the stage. Once the stage and severity of the wound is determined, it must be cleaned, usually with a saline solution. After the wound is cleaned, it needs to be kept clean, moist, and covered with an appropriate bandage. There are several different types of bandages your doctor may use to dress the wound. These include:
- Water-based gel with a dry dressing
- Foam dressing
- Hydrocolloid dressing
- Alginate dressing
Sometimes debridement is needed. This is a process of ridding the wound of dead tissue. Debridement is an important part of the healing process. It changes the wound from a long-lasting one to a short-term wound. There are several types of debridement. These methods include:
- Ultrasound: Using sound waves to remove the dead tissue.
- Irrigation: Using fluid to wash away dead tissue.
- Laser: Using focused light beams to remove the dead tissue.
- Biosurgery: Using maggots to eliminate bacteria from the wound.
- Surgery: Using surgery to remove the dead tissue and close the wound.
- Topical: Medical-grade honey or enzyme ointments.
What Increases The Risk Of Developing Pressure Ulcers
People who are confined to a bed or chair for example due to stroke, spinal injury or dementia are at greater risk of developing extensive pressure ulcers. Other risk factors include:
- immobility being confined to bed after an illness or surgery, or due to paralysis
- diabetes and other health conditions that can affect blood supply
Read Also: How Effective Is Humira For Ulcerative Colitis
What Is A Pressure Injury
Pressure injury is a newer term for what people might know as a pressure sore, pressure ulcer, decubitus ulcer, bedsore or skin breakdown. The term changed because not all stages of injuries caused by pressure are actually open sores or ulcers. However, the meaning is similar. A pressure injury is an area of the skin or underlying tissue that is damaged when prolonged pressure cuts off blood flow to the area for too long.
- To learn more about skin care, visit .
Stages Of Pressure Ulcers
Casey Gallagher, MD, is board-certified in dermatology and works as a practicing dermatologist and clinical professor.
If a loved one has been severely injured or is extremely ill, they may need to spend a significant amount of time in bed. Prolonged immobility, while beneficial to recovery, can become problematic if it places persistent pressure on vulnerable skin. Unless preventive steps are taken, pressure ulcers, also known as decubitus ulcers or bedsores, can develop.
Also Check: What Can I Take For Ulcerative Colitis
Factors That Influence Sacral Ulcer Management
While wound management is a key part of sacral ulcer management, treating patients holistically is the key to success. Apart from ischemia, other factors that impede normal healing include poor nutrition, infection, edema, persistent moisture, fecal and urinary soiling, and shearing forces. One can look for, prevent, or minimize each of these risk factors. Of course, the patient should be frequently repositioned to avoid further tissue damage and to promote healing.
When selecting a dressing, the wound should be kept moist but not contain excessive amounts of exudate. Wound care professionals should consider the type of ulcer and any comorbid conditions that could complicate treatment . Arterial wounds generally require a moisture-retaining dressing, while wounds that arise from venous insufficiency usually require a dressing that absorbs excess moisture. All surfaces of the wound, including any tunnels, should be packed with the appropriate dressing.
How To Treat Pressure Ulcer
When Pressure ulcers are in the early stages, people may be able to treat them at home. Frequently changing positions can help the ulcers heal and keep new ones from forming.
Pressure ulcers can be prevented by periodically repositioning yourself to avoid stress on the skin. Other strategies include taking good care of the skin, maintaining good nutrition and fluid intake, quitting smoking, managing stress, and exercising daily.
MaxioCel, an advanced wound dressing product, provides faster healing to patients suffering from chronic wounds, such as pressure ulcers, diabetic foot ulcers, venous leg ulcers, cavity wounds, and skin abrasions to name some.
MaxioCel range of advanced chitosan dressings has the potential to address this gap and be a real game-changer. With a range of MaxioCel products, millions of patients who need advanced wound care products are being treated every year. MaxioCel with its 360-degree care combined hemostatic, pain management, and scar improvement properties, fulfills a large gap in the market.
Juwariah Khan
Donât Miss: Can Ulcerative Colitis Lead To Crohn Disease
Recommended Reading: Best Treatment For Stomach Ulcers
What Are The Benefits Of This Treatment
It can take several months of bedrest for a severe wound to heal on its own. All pressure must be off the area while in bed, which can be very hard to do on an ongoing basis. If pressure is put on the area while in bed, it can delay healing or make the wound worse. Plus, there is an increased risk of infection with any open wound. The longer the wound is open, the longer the higher risk continues. If an infection develops, there is a risk that it can spread and become life-threatening.
The obvious benefit of this treatment is that the wound can heal much quicker than it would without the treatment. Your doctor can explain all your benefits, but here are a few of the benefits:
- Much less time needed for bedrest
- Lowered risk for infection
- Increased independence to enjoy meaningful activities
- Lowered healthcare costs
Can Pressure Sores Be Prevented Or Avoided
The best way to prevent pressure sores is to avoid spending long periods of time in a chair, wheelchair, or bed. If youre unable to move on your own, make arrangements for somebodysuch as a family member, friend, or caregiverto help you move.
If you must spend a lot of time in a chair, wheelchair, or bed, check your entire body daily. Look for spots, color changes, or other signs of sores. Pay attention to the pressure points where sores are most likely to occur. Again, if youre unable to look on your own, ask someone to help you.
Another way to avoid pressure sores is to keep your skin healthy. This includes keeping it clean and dry. Wash it with mild soap and warm water. Dont use hot water. Apply lotion often.
Even small amounts of exercise can help prevent pressure sores. Thats because exercise improves blood flow, strengthens your muscles, and improves your overall health. Talk to your doctor if physical activity is difficult. They can suggest certain exercises. Your doctor also may refer you to a physical therapist. They can show you how to do exercises that fit with your current health condition.
Lastly, if you smoke, quit. Smoking increases your risk of pressure sores.
Don’t Miss: Best Things To Eat With Ulcerative Colitis
Stage 4 Bedsore Therapy
Stage 4 bedsore treatment is more accurately described as stage 4 bedsore management for most elderly patients. Although stage 4 bedsore treatment can be aimed at actually healing the open wound, many elder patients are not healthy enough to fully recover from a stage 4 bedsore. As a result, there are many medical processes in place that focus entirely on minimizing pain and discomfort for an elderly person with stage 4 bedsores.
Stage 4 bedsore management may involve the following:
Berman, Kevin. Pressure Ulcer.Medline Plus. Atlanta: 2012. < > .
Bluestein, Daniel and Ashkan Javaheri. Pressure Ulcers: Prevention, Evaluation, and Management.American Academy of Family Physicians. 2008. < > .
FREE Case Evaluation
Caring For A Pressure Sore
Stage I or II sores will often heal if cared for carefully. Stage III and IV sores are harder to treat and may take a long time to heal. Here’s how to care for a pressure sore at home.
Relieve the pressure on the area.
- Use special pillows, foam cushions, booties, or mattress pads to reduce the pressure. Some pads are water- or air-filled to help support and cushion the area. What type of cushion you use depends on your wound and whether you are in bed or in a wheelchair. Talk with your health care provider about what choices would be best for you, including what shapes and types of material.
- Change positions often. If you are in a wheelchair, try to change your position every 15 minutes. If you are in bed, you should be moved about every 2 hours.
Care for the sore as directed by your provider. Keep the wound clean to prevent infection. Clean the sore every time you change a dressing.
Avoid further injury or friction.
- Powder your sheets lightly so your skin doesn’t rub on them in bed.
- Avoid slipping or sliding as you move positions. Try to avoid positions that put pressure on your sore.
- Care for healthy skin by keeping it clean and moisturized.
- Check your skin for pressure sores every day. Ask your caregiver or someone you trust to check areas you can’t see.
- If the pressure sore changes or a new one forms, tell your provider.
Take care of your health.
You May Like: How To Heal Mouth Ulcers
How Pressure Ulcers Develop
Pressure ulcers can develop when a large amount of pressure is applied to an area of skin over a short period of time. They can also occur when less pressure is applied over a longer period of time.
The extra pressure disrupts the flow of blood through the skin. Without a blood supply, the affected skin becomes starved of oxygen and nutrients, and begins to break down, leading to an ulcer forming.
Pressure ulcers tend to affect people with health conditions that make it difficult to move, especially those confined to lying in a bed or sitting for prolonged periods of time.
Conditions that affect the flow of blood through the body, such as type 2 diabetes, can also make a person more vulnerable to pressure ulcers.
Learn more about the causes of pressure ulcers.
Treatment Of Stage 3 And Stage 4 Pressure Ulcers
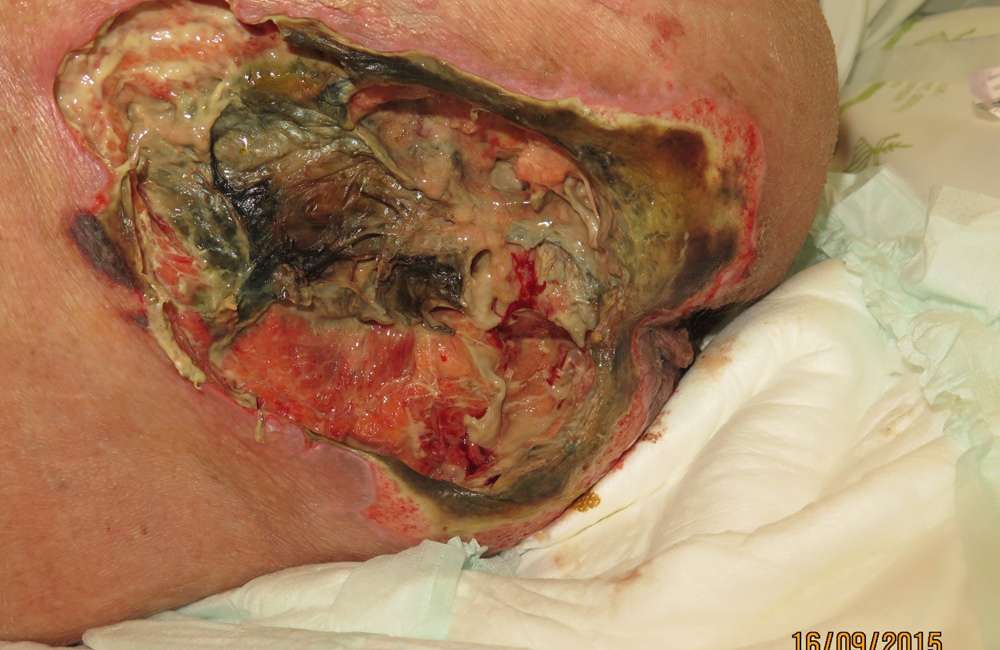
The goal of treatment for stage 3 and 4 pressure ulcers, is to properly debride and dress the wound cavity, create or maintain moisture for optimal healing, and protect the wound from infection. The goal of properly unloading pressure from the area still applies. At these pressure ulcer stages, more emphasis should be placed on proper nutrition and hydration to support wound healing. If the extent of the pressure ulcer or other factors prohibit it from healing properly, surgery may be necessary to close the wound.
The following precautions can help minimize the risk of developing pressure ulcers in at-risk patients and to minimize complications in patients already exhibiting symptoms:
- Patient should be repositioned with consideration to the individualâs level of activity, mobility and ability to independently reposition. Q2 hour turning is the standard in many facilities, but some patients may require more or less frequent repositioning, depending on the previous list.
- Keep the skin clean and dry.
- Avoid massaging bony prominences.
- Provide adequate intake of protein and calories.
- Maintain current levels of activity, mobility and range of motion.
- Use positioning devices to prevent prolonged pressure bony prominences.
- Keep the head of the bed as low as possible to reduce risk of shearing.
- Keep sheets dry and wrinkle free.
Recommended Reading: How To Treat Skin Ulcer On Leg
What Are The Causes Of Pressure Injuries
Pressure injuries are caused when a force is applied to the skin, causing damage to the tissue. Several types of force include:
- Pressure: Constant pressure on the skin results from remaining in the same position for a prolonged period of time.
- Shear: Shear damage or a dragging force can occur when the head of the bed is raised and the body slides down. The skin sticks to the sheets, but internal structures are damaged.
- Moisture: Fluids that remains on the skin can cause the skin to become overly wet, which increases the risk for pressure injury development.
What Are The Long
If the wound becomes infected, the infection can spread to other parts of the body. Several conditions that may occur if an infection spreads include:
- Cellulitis: An infection of the skin.
- Osteomyelitis: An infection of the bone.
- Bacteremia: An infection of the blood.
- Meningitis: An infection of the brain and spinal cord.
- Endocarditis: An infection of the heart.
Don’t Miss: What To Avoid With An Ulcer
Sacral Decubitus Ulcers Are A Certain Type Of Wound Located On The Lower Back At The Bottom Of The Spine
How to measure a sacral wound. Clock terms can also be used to describe the location of undermining. Use the body as a clock when documenting the length, width, and depth of a wound using the linear method. The braden risk assessment scale can be utilized to assess a patientâs risk of developing a pressure ulcer.
Get the wound depth using a cotton pledget or applicator dipped in a normal saline solution to measure the deepest part of the wound bed. Look closely at the wound and its edges, and then draw the wounds shape. Measure the wound how to measure wound size consistency is key.
Any adult who scores lower than 18 on the braden scale is high risk. For example, you might use words like jagged, red, puffy, or oozing to describe the wound.step 2, use a ruler to measure the length. Remove the applicator and hold it against the ruler to measure the depth of the wound margin based on.
This is particularly important when The total amount of tissue debrided should be listed separately from the wound measurements The six approaches for measuring wound area were simple ruler method , mathematical models , manual planimetry , digital planimetry , stereophotogrammetry and digital imaging method .
Step 1, draw the shape of the wound and write a brief description. Assessing and measuring wounds you completed a skin assessment and found a wound. In all instances of the linear method, the head is at 12:00 and the feet are at 6:00.
Archives Of Plastic Surgery
The Available Reconstructive Options Are
Split thickness skin grafting
When the ulcer is superficial and vital tissues such as bone, vessels, nerves or tendons are not exposed, and the ulcer is not copiously discharging, skin grafting is the first option for surgical treatment. The slimy layer over the surface of ulcer is sharply debrided to get a healthy vascular bed for skin grafting.
Local flaps
Variety of local flaps can be used to reconstruct the defect created by excision of pressure ulcers. Local transposition, rotation, limberg flap are the available options .3]. Biceps femoris V-Y advancement for ischial pressure sore and perforator based V-Y advancement is another good options if the anatomy permits .
Sacral pressure sore , debridement and cover by local perforator based V-Y advancement flaps , 1-month post-operative , recurrence on the flap after 11 years due to loss of family support and subsequent improper care. Another patient with the same flap after 16-year of follow-up with a proper weight shifting and care showing stable coverage
Regional flaps
Medial planter flap for heel sore: A long-standing deep trophic ulcer of heel . The islanded medial planter flap was transposed to the defect and the resultant donor site was covered by split thickness skin graft . The 1-week and 3-month post-operative pictures showing stable coverage. Patient allowed full weight bearing from 6th week along with silicone footpad protection
Microvascular free flaps
You May Like: Ulcerative Colitis Caused By Alcohol
Symptoms Of Pressure Ulcers
The parts of the body most at risk of developing pressure ulcers are those that are not covered by a large amount of body fat and are in direct contact with a supporting surface, such as a bed or a wheelchair.
For example, if you are unable to get out of bed, you are at risk of developing pressure ulcers on your:
- shoulders or shoulder blades
- knees, ankles, heels or toes
- spine
- tail bone
If you are a wheelchair user, you are at risk of developing pressure ulcers on:
- your buttocks
- the back of your arms and legs
- the back of your hip bone
What Are The Stages Of A Pressure Injury
There are four stages that describe the severity of the wound. These stages include:
- Stage 1: This stage is discolored skin. The skin appears red in those with lighter skin tones and blue/purple in those with darker skin tones. The skin does not blanch when pressed with a finger.
- Stage 2: This stage involves superficial damage of the skin. The top layer of skin is lost. It may also look like a blister. At this stage, the top layer of skin can repair itself.
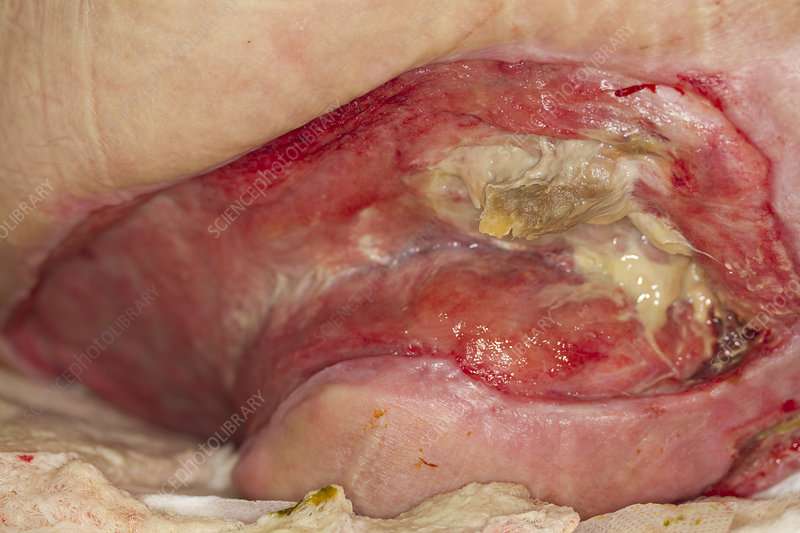
- Stage 3: This stage is a deeper wound. The wound is open, extending to the fatty layer of the skin, though muscles and bone are not showing.
- Stage 4: This stage is the most severe. The wound extends down to the bone. The muscles and bone are prone to infection, which can be life-threatening.
You May Like: Do Probiotics Help Stomach Ulcers