Axial Arthritis And Ulcerative Colitis
Although more common in people with Crohns disease, axial arthritis can also affect those with UC. Over time, axial arthritis causes pain and stiffness in the lower spine and sacroiliac joints, which connect the lower spine and pelvis.
The main symptoms of axial arthritis are stiffness and pain in the lower back, hips, and buttocks that persist for three or more months at a time. Flare-ups typically come on slowly, gradually worsening over a period of several weeks or months. Symptoms tend to be at their worst in the morning and wear off with time and exercise. Prolonged rest or inactivity can make joint pain worse.
I canât bend or twist like I used to, wrote one MyCrohnsAndColitisTeam member. It hurts too bad. Being up and about helps, but getting up for those first few steps after sitting a while is so painful, and I canât fully stand upright sometimes for a minute or so. Itâs frustrating.
What Foods Should I Not Eat When I Am Having An Ulcerative Colitis Flare
Certain foods can exacerbate or aggravate an UC flare and should be avoided. They are more likely to trigger cramping, bloating, and/or diarrhea and are also not recommended in people diagnosed with a stricture, which is a narrowing of the intestine caused by inflammation or scar tissue, or in those who have had recent surgery. Examples include:
- Foods high in insoluble fiber that are hard to digest, such as seeds, raw green vegetables , whole nuts, whole grains, or fruits with a skin
- Lactose, which is milk sugar found in dairy products, milk, cream, cream cheese, and soft cheeses
- Non-absorbable sugars such as sorbitol, mannitol, and other sugar alcohols that are typically found in sugar-free gum, candy, ice cream, and certain types of fruits and juices such as pear, peach, and prune juice
- Sugary foods such as candy, pastries, and juices
- High-fat foods such as butter or margarine, coconut oil, or fatty, fried, or greasy food
- Spicy foods
- Alcohol such as beer, wine, or spirits
- Caffeinated drinks such as coffee or energy drinks
- Soda.
How To Tell A Back Strain From A More Serious Medical Condition
So, how can you be sure that the pain in your back isnt the result of some weekend gardening but rather a more serious medical condition? Most of the time when Dr. Crooks sees patients, theyve had their medical issue diagnosed and theyre dealing with the secondary effects of that problem in their musculoskeletal system.
However, he has seen patients whove come to him for back pain only to find something on an imaging study MRI such as a kidney stone or even cancer, which is more unusual.
Here are the most common medical conditions that can mimic musculoskeletal back pain and how you can help tell the difference:
Don’t Miss: Can Ulcers Cause Heart Palpitations
Vitamin And Mineral Supplements For Ibd
A person with IBD who eats a healthy, varied diet does not usually need to take vitamin supplements. But if they have a dietary deficiency, they may need tablets or occasional vitamin B12 injections. For example, a person on a low-fibre diet may need extra vitamin C and folic acid because they dont eat enough fruit and vegetables.A person with Crohns disease who experiences steatorrhoea may need calcium and magnesium supplements. Most children with IBD should take supplements to help them grow and develop normally.
What Are The Causes Of Ulcerative Colitis
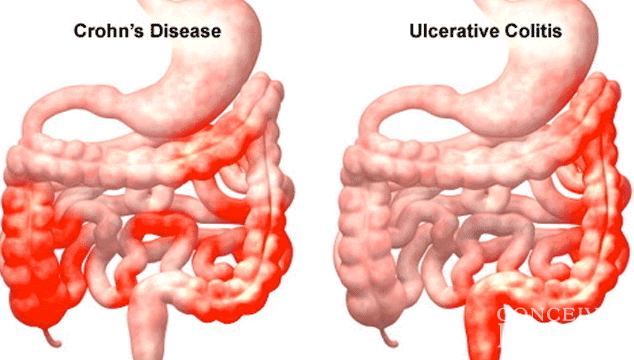
The exact cause of ulcerative colitis is unknown. The following have been suggested:
- Immune system
- Ulcerative colitis is thought to be a type of autoimmune disease, in which the body’s immune system malfunctions and attacks the tissues of the bowel.
Ulcerative colitis may occur at any age, but it is most common in young adults in the 15-30 age group or later on, in the 50-70 age group. Women are affected more than men.
Recommended Reading: Best Foods To Heal Stomach Ulcer
Crohns Disease And Ulcerative Colitis And Digesting Food
Your mouth and stomach break down food by mechanical and chemical means. When the food has reached a pulp-like consistency, it is slowly released into the first part of the small intestine . The food is then massaged along the length of the small intestine. Organs like the pancreas and the gall bladder make digestive enzymes to further break down the food into its simpler components.
The small intestine is lined with microscopic , finger-like projections that lie close to tiny blood vessels . Nutrients pass into the bloodstream through these villi. The rest of the food is pushed into the large bowel, which absorbs excess water. The waste is then temporarily stored in the colon before it is eliminated from the anus.The two ways in which Crohns disease and ulcerative colitis disturb the digestion and absorption processes are:
- Crohns disease an inflamed ileum impairs absorption of vitamin B12 and bile salts. Inflammation along the length of the small intestine impairs absorption of all food nutrients. Inflammation of the large bowel impairs water absorption, causing diarrhoea.
- Ulcerative colitis digestion and absorption are generally not affected. Inflammation of the large bowel impairs water absorption, causing diarrhoea.
Other factors that may affect your nutritional status include:
This Factsheet Is About Ulcerative Colitis
Ulcerative colitis is a disease of the rectum and the large bowel, . Ulcerative colitis is thought to affect around 1 in 420. The peak age of incidence between 15-25 years old with a smaller peak occurring between the age of 55 and 65 years old. But it can occur at any age.
INFLAMMATORY BOWEL DISEASE
Ulcerative colitis is one of a group of conditions that are known as Inflammatory bowel diseases, which also includes Crohns disease. Inflammatory bowel disease is different to Irritable Bowel Syndrome , which can cause similar symptoms but does not involve inflammation. The term colitis means the large bowel has become inflamed and if this becomes severe enough ulcers may form in the lining of the large bowel.
Don’t Miss: Ulcerative Colitis Diet During Flare
Foods That May Fight Uc
Some research shows that certain nutrients may help fight the irritation and swelling in your gut caused by UC. Scientists have studied how linoleic acid affects people with the condition. Although everyone needs this good fat, donât overdo it, since there is some evidence it may play a role in inflammation if you get too much.
Other studies show that an omega-3 fatty acid called EPA may fight inflammation. This is another âgoodâ fat that blocks certain chemicals in your body called leukotrienes. Fish oil is a good source of EPA. In some studies, folks with UC saw some benefits when they took high doses. Many people, though, didnt like the fishy taste. There is also some evidence that adding fish oil to aminosalicylates may be helpful, but this isnât proven. DHA is another omega-3 found in fish oil that can fight inflammation and is used by some people with UC.
Some research also shows that yogurt with gut-healthy bacteria, called probiotics, eases inflammation. Scientists are still studying how they may help people with UC and similar conditions. Some people also believe that a diet low in FODMAPs a type of highly-fermentable carbs found in meats, fruits, dairy, and lots of other foods may help ease UC symptoms. But the evidence is unclear if it does. And without close monitoring, any diet that restricts certain foods may lead to poor nutrition and other problems.
Show Sources
Dont Miss: Wound Vac For Pressure Ulcers
Ulcerative Colitis And Cancer Of The Colon
The chance of developing cancer of the large intestine is higher than average in people who have had ulcerative colitis for several years or more. It is more of a risk if you have frequent flare-ups affecting the whole of the large intestine. For example, about 1 in 10 people who have ulcerative colitis for 20 years which affects much of their large intestine will develop cancer.
Because of this risk, people with ulcerative colitis are usually advised to have their large intestine routinely checked after having had the condition for about 10 years. This involves a look into the large intestine by a flexible telescope every now and then and taking small samples of bowel for examination. It is usually combined with chromoscopy – this is the use of dye spray which shows up suspicious changes more easily. Depending on the findings of this test and on other factors, you will be put into a low, intermediate or high risk category. ‘Other factors’ include:
- The amount of intestine affected.
- Whether you have had complications such as polyps. These are small, non-cancerous growths on the inside lining of the colon or rectum.
- Whether you have a family history of cancer.
The National Institute for Health and Care Excellence recommends the next colonoscopy/chromoscopy should depend on the degree of risk of developing colon or rectal cancer. After the next test, your risk will be calculated again.
Don’t Miss: Best Food For Peptic Ulcer
What To Eat When You Dont Feel Like Eating
If youre worried about triggering a flare, eat small, frequent meals throughout the day, says Palcsik, and avoid foods that contain sugar alcohols.
People who feel nauseated in the mornings can likely tolerate a protein shake and cooked, pureed, or canned fruit, she adds. Soft, fleshy fruit like watermelon and applesauce are other good options. Palcsik recommends pairing one high-protein food with a carbohydrate thats low in insoluble fiber.
A few stomach-friendly breakfast ideas:
- 1 cup of low-fat cottage cheese with a fruit cup
- 2 scrambled eggs with ½ cup of unsweetened applesauce
- 1 cup of oatmeal with a peeled peach
- Smoothie made with 1 cup of low-fat Greek yogurt, 1 cup of unsweetened almond milk, 1 cup of frozen peaches, and ½ banana
- 2 hard-boiled eggs with 1 cup of cooked wheat grains
Energy And General Health
If youre following a restricted or relatively bland diet to help cope with a flare of ulcerative colitis symptoms, or youre on a liquid-only diet as your body heals from surgery, you may be getting fewer calories and nutrition. As a result, you might not have as much energy as you typically do.
Its important that you try your best to eat enough each day to meet your bodys nutrition and energy needs. Not only to help manage ulcerative colitis but to maintain your overall health.
Complications from IBD, such as infections, may be more likely if your body is weakened from malnourishment, vitamin deficiencies, and dehydration.
Preventing nutritional deficiencies may help prevent flares: In 2017, research from Beth Israel Deaconess Medical Center indicated that people with ulcerative colitis who are in remission may be more likely to experience a relapse of symptoms if they are deficient in vitamin D.
Recommended Reading: Natural Ways To Heal Stomach Ulcers
Duration Of Ulcerative Colitis
Your risk for colon cancer typically starts to increase once youve lived with UC for about 8 to 10 years, according to the Crohns & Colitis Foundation. The longer you have UC, the higher your cancer risk.
According to a 2019 literature review , colorectal cancer rates for people in North America increase dramatically after a person has lived with UC for 30 years.
Colorectal cancer rates in Asia increase dramatically after a UC duration of 10 to 20 years. Cancer rates for Asian people whove had UC for 10 to 20 years were four times higher than rates for Asian people whove had UC for 1 to 9 years.
Cancer rates for Europeans also increased as UC duration increased. However, the increase in cancer rates over time wasnt considered statistically significant. There wasnt enough data from Oceania to compare cancer rates over time.
This literature review had some noteworthy limitations. For instance, data wasnt included for people whod had colorectal polyps or a colectomy for UC.
Data for people with cancer outside of the colon or rectum, or those with a family history of colorectal cancer, was also excluded.
Ulcerative Colitis In Children
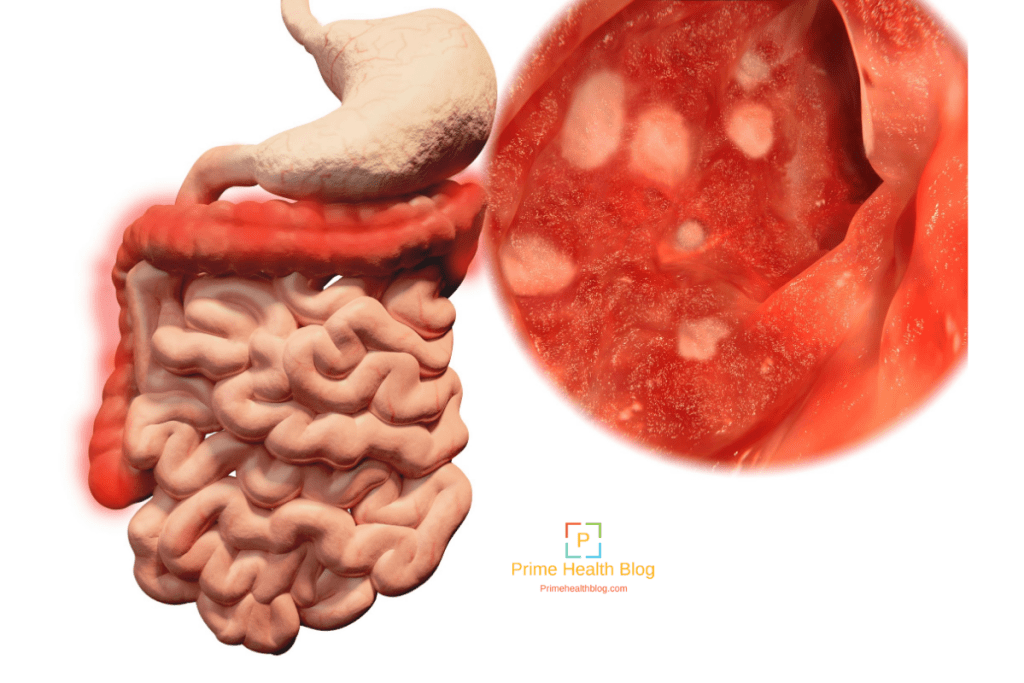
According to one study of IBD in the United States, 1 in 1,299 children between ages 2 and 17 years old were affected by the condition in 2016. Crohns disease was twice as common as UC, and boys were more likely to have IBD than girls.
For children with IBD, a diagnosis is more likely after 10 years old.
UC symptoms in children are similar to symptoms in older individuals. Children may experience bloody diarrhea, abdominal pain and cramping, and fatigue.
In addition, they may experience issues compounded by the condition, such as:
- anemia due to blood loss
- malnutrition from poor eating
- unexplained weight loss
UC can have a significant effect on a childs life, especially if the condition isnt treated and managed properly. Treatments for children are more limited because of possible complications. For example, medicated enemas are rarely used as a treatment method in children.
However, children with UC may be prescribed medications that reduce inflammation and prevent immune system attacks on the colon. For some children, surgery may be necessary to manage symptoms.
If your child has been diagnosed with UC, its important that you work closely with their doctor to find treatments and lifestyle changes that can help. Check out these tips for parents and children dealing with UC.
Dont Miss: Best Protein For Ulcerative Colitis
Also Check: Artificial Sweeteners And Ulcerative Colitis
Not Just Crohn’s And Uc But 100s Of Diseases
In order to understand why you cant have both Crohns and UC in the same person I think its important to better understand what Inflammatory Bowel Disease actually is. When a patient is diagnosed with IBD they receive a diagnosis of Crohns disease or ulcerative colitis and sometimes a person will receive a diagnoses of IBD Unclassified which used to be known as indeterminate colitis.
So wouldnt that mean there are only 3 types of IBD? Nope. We receive one of those
3 diagnoses according to the way our body expresses its IBD but over the years we have come to realize that IBD falls along a spectrum and there really could be hundreds of different kinds of inflammatory bowel diseases.
Dr. Rubin helps describe this by saying, Weve labeled Crohns disease and ulcerative colitis as two diseases, but weve come to realize that there may be 50 to 100 different diseases that are all overlapping. The body can express itself in very specific and limited ways, so anything that results in overactive inflammation or some imbalanced immune response can look like one of these diseases.
To help you understand this you can take a look at the genes that are involved in IBD. Back in the early aughts the very first susceptibility gene to be associated with IBD, NOD2, was discovered. Since then over 200 genes have been discovered and that
more in-depth look into what IBD actually is.
Questions To Ask Your Doctor
- How will my inflammatory bowel disease be treated?
- Will I need surgery? Are there other options?
- What lifestyle changes can I make to help inflammatory bowel disease?
- What are some medicines used to treat inflammatory bowel disease and what are the possible side effects?
- Are my children at risk of inflammatory bowel disease?
Also Check: Indian Diet For Ulcerative Colitis
Don’t Miss: Do Probiotics Help Stomach Ulcers
Celiac Later In Life: Can You Become Gluten Intolerant
Research shows that celiac disease can strike at any age, even in people who have tested negative in the past. Whats behind the rise in celiac among seniors?
Jose L. Pelaez/Corbis
Celiac disease can strike at any age, even in people who once tested negative for the condition.
The digestive disease is being diagnosed more frequently in everyone including the elderly, says Joseph Murray, MD, a gastroenterologist at the Mayo Clinic in Rochester, Minnesota, and author of the book Mayo Clinic Going Gluten Free: Essential Guide to Managing Celiac Disease and OtherGluten-Related Conditions.
Celiac disease is an autoimmune condition that tends to run in families. People with celiac cant tolerate gluten, a protein found in wheat, barley, and rye, according to the National Institutes of Health . In these people, gluten damages the part of the small intestine that helps absorb nutrients. Signs and symptoms may include pain, diarrhea, malnutrition, anemia, and osteoporosis, the NIH says. In older people, cognitive impairment can also be a symptom, Dr. Murray says.
What Are The Treatment Options For Ulcerative Colitis
The primary goals of the treatment for ulcerative colitis are to achieve remission and maintain remission to prevent further flare-ups. If remission cannot be achieved, the next objective is to reduce the severity of the condition and frequency of flare-ups to enhance ones quality of life.
The principle of the treatment of ulcerative colitis is to reduce the inflammation and allow recovery of the lining of the colon and rectum. It helps with diarrhea, rectal bleeding, and stomach discomfort.
However, there is no one-size-fits-all therapy for ulcerative colitis. Because the condition is unique for everyone, the solution must be personalized.
Medical treatment
Various medications that are administered orally, intravenously, or as suppositories or topical agents are available for the treatment of ulcerative colitis. These medications include:
- Amino salicylates
Symptomatic treatment for diarrhea, abdominal pain, nausea, and others is administered to relieve the symptoms.
Surgery
A person may respond well initially to medical treatments. However, severe bleeding from ulcers or rupture of the bowel, or the development of toxic megacolon may indicate surgery.
Surgical excision and total removal of the affected section of the intestine are done. This surgery is called proctocolectomy.
Diet changes
Modifying the diet may be beneficial at times, especially during a flare. The doctor may suggest certain diets at various times, such as:
You May Like: How To Treat A Diabetic Ulcer