When To Call The Doctor
- Cramps or pain in your lower stomach area
- Bloody diarrhea, often with mucus or pus
- Diarrhea that cannot be controlled with diet changes and drugs
- Rectal bleeding, drainage, or sores
- Fever that lasts more than 2 or 3 days, or a fever higher than 100.4°F without an explanation
- Nausea and vomiting that lasts more than a day
- Skin sores or lesions that do not heal
- Joint pain that keeps you from doing your everyday activities
- A feeling of having little warning before you need to have a bowel movement
- A need to wake up from sleeping to have a bowel movement
- Failure to gain weight, a concern for a growing infant or child
- Side effects from any drugs prescribed for your condition
Can I Get Surgery For My Ulcerative Colitis
Surgery is an option if medications arent working or you have complications, such as bleeding or abnormal growths. You might develop precancerous lesions, or growths that can turn into colorectal cancer. A doctor can remove these lesions with surgery or during a colonoscopy.
Research shows that about 30% of people with ulcerative colitis need surgery sometime during their life. About 20% of children with ulcerative colitis will need surgery during their childhood years.
There are two kinds of surgery for ulcerative colitis:
Proctocolectomy and ileoanal pouch
The proctocolectomy and ileoanal pouch is the most common procedure for ulcerative colitis. This procedure typically requires more than one surgery, and there are several ways to do it. First, your surgeon does a proctocolectomy a procedure that removes your colon and rectum. Then the surgeon forms an ileoanal pouch to create a new rectum. While your body and newly made pouch is healing, your surgeon may perform a temporary ileostomy at the same time. This creates an opening in your lower belly. Your small intestines attach to the stoma, which looks like a small piece of pink skin on your belly.
After you heal, waste from your small intestines comes out through the stoma and into an attached bag called an ostomy bag. The small bag lies flat on the outside of your body, below your beltline. Youll need to wear the bag at all times to collect waste. Youll have to change the bag frequently throughout the day.
Can Imodium Make You Feel High
No, taking Imodium at the recommended dosage to treat diarrhea wont make you feel high. At this dosage, Imodium doesnt affect your brain. Instead, it only works inside your intestine.
However, Imodiums chemical structure is similar to that of opioids, such as morphine and heroin. If its misused and taken in extremely large doses, Imodium can affect your brain. And if it enters your brain, it may make you feel high.
Some people misuse Imodium in this way to make themselves feel high. But you shouldnt misuse Imodium, because doing so can have serious effects on your heart. .
If you have questions about how Imodium may affect you, talk with your doctor or pharmacist.
Don’t Miss: How To Ease Mouth Ulcer Pain
Who Diagnoses Ulcerative Colitis
If you have symptoms of ulcerative colitis, your regular healthcare provider will probably refer you to a specialist. A gastroenterologist a doctor who specializes in the digestive system should oversee the care for adults. For young patients, a pediatric gastroenterologist who specializes in children should manage the care.
Is It Important To Treat A Flare Early Or Is It Ok To Wait A Bit
Inflammation typically does not resolve without treatment and early intervention has a better outcome than waiting to treat. At an early stage of a flare, a more optimal baseline treatment is often enough to get the inflammation under control. If you wait, there is a greater risk that you might need drugs with greater side effects, such as oral steroids. By waiting, you will have to manage longer with your symptoms before getting relief. Living with constant or longer periods of inflammation might increase your risk for future complications, as inflammation might cause damage to the gut wall that accumulates in severity with each flare.
If you are experiencing worsening symptoms, you have probably already had the flare for some time without symptoms. Evidence shows that a stool test for inflammation in the colon, called fecal calprotectin, is often elevated for two to three months before any symptoms appear. Your colon might also start to show visual evidence of inflammation before you have symptoms, or at least indicate an increased risk for a flare.
Also Check: What’s The Signs Of An Ulcer
Misuse Withdrawal And Dependence
Imodium is a mu opioid agonist. At the recommended dosages for diarrhea, Imodium does not cross the blood brain barrier or produce a centrally acting opioid effect. However, when taken in extremely high doses, Imodium can enter the central nervous system and produce euphoria. Imodium is sometimes misused for this effect.
Misuse of Imodium can lead to prolonged QT interval, Torsades de Pointes, or other ventricular arrhythmias, and heart attack. It can also lead to other symptoms of opioid overdose, such as CNS and respiratory depression.
Misuse of Imodium can lead to dependence on the drug and withdrawal symptoms after stopping the drug.
What Drugs Are Used To Treat Collagenous Colitis
Budesonide, mesalamine, cholestyramine, Boswellia serrata extract, probiotics, prednisolone and Pepto-Bismol® have been studied as treatment for collagenous colitis. Budesonide is an immunosuppressive steroid drug that is quickly metabolized by the liver resulting in reduced steroid-related side-effects.
Don’t Miss: What To Eat To Help Stomach Ulcers
Does Ulcerative Colitis Make You Immunocompromised
Ulcerative colitis doesnt make you immunocompromised. Some of the medicines that treat it may change the way your immune system responds. This change is different for each medication. Some of these changes may increase the risk of certain infections or other issues. A discussion with your health care team before starting a medication is the best way to understand these risks and ways to prevent them.
Prednisone Prednisolone And Methylprednisolone
Prednisone is taken by mouth and is available as:
- an immediate-release tablet
- a delayed-release tablet
- a liquid solution
Its available as a generic drug and as the brand-name drugs Prednisone Intensol and Rayos .
The forms of prednisolone that are FDA approved for UC are:
- immediate-release tablet
- liquid solution
- syrup
You can take any of these forms by mouth. Prednisolone is available as a generic drug and as the brand-name drugs Millipred and Prelone .
Methylprednisolone comes in two forms:
- oral tablet
- injectable medication
Its available as a generic drug and as the brand-name drugs Medrol and Depo-Medrol .
Side effects, complications, and interactions
When given in high doses, the side effects of these drugs are practically indistinguishable. The more common side effects can include:
- increased blood sugar levels
Immunomodulators are drugs that decrease the bodys response to its own immune system. The result is lowered inflammation throughout your body.
Immunomodulators may reduce the number of UC flare-ups you have and help you stay symptom-free longer.
Theyre generally prescribed to people whose symptoms havent been managed with 5-ASA drugs and corticosteroids. However, these drugs may take several months to start working.
The Food and Drug Administration hasnt approved immunomodulators for the treatment of UC.
However, theyre well supported in medical literature as useful options, and your doctor may still prescribe them. This is known as off-label drug use.
Also Check: Aloe Juice For Ulcerative Colitis
Common Questions About Loperamide
Loperamide is an anti-motility medicine. This means that it slows down food as it goes through your gut. Your body can then draw in more water from your intestines, so that your poos get firmer and you poo less often.
Loperamide usually starts to work within 1 hour to make your diarrhoea better.
Most people only need to take loperamide for 1 to 2 days.
You may need to take it for longer if your diarrhoea is because of a bowel condition such as Crohn’s disease, ulcerative colitis or short bowel syndrome.
If you’ve bought loperamide from a shop or pharmacy, do not take it for more than 48 hours without talking to a doctor.
If you’ve bought loperamide from a shop or pharmacy, do not take it for more than 48 hours without talking to a doctor.
Although diarrhoea is usually nothing to worry about, it can sometimes lead to dehydration. This can be serious if you do not get the correct treatment.
Diarrhoea can also sometimes be a warning sign of another problem. For this reason, it’s important to see a doctor to find out the cause of your diarrhoea if it continues beyond 7 days.
If you’ve bought loperamide for short-term diarrhoea, do not take it for longer than 48 hours without talking to a doctor.
Loperamide may be used for long-lasting diarrhoea and by people who have a colostomy if their doctor prescribes it.
Do not take loperamide to prevent diarrhoea, unless your doctor tells you to.
It’s not been officially approved and tested for preventing diarrhoea.
What Problems Are Associated With Chronic Diarrhea
Healthcare providers will assess a patients symptoms to determine whether or not they are exhibiting acute or chronic diarrhea. Acute diarrhea is defined as watery stool lasting 2 weeks, whereas chronic diarrhea is watery stool lasting longer than 4 weeks. Acute diarrhea is often caused by a virus, but sometimes it is caused by bacteria, in which case it will be treated with antibiotics. Chronic diarrhea, on the other hand, may be due to CD or UC.1,2
Chronic diarrhea often directly impacts a patients nutritional status. Patients experiencing chronic diarrhea are at risk of becoming malnourished, because not enough nutrients can be absorbed by the digestive tract. While it is possible that certain food types can agitate the digestive tract causing chronic diarrhea, it is important for patients to contact their healthcare provider before self-imposing any dietary restrictions.
Patients experiencing chronic diarrhea due to IBD should work with their healthcare providers to develop a treatment plan. One form of management is the use of medications called anti-diarrheals.
Read Also: Can You Get An Ulcer In Your Intestines
What Causes Ulcerative Colitis Flareups
When youre in remission from ulcerative colitis, youll want to do everything you can to prevent a flareup. Things that may cause a flareup include:
- Emotional stress: Get at least seven hours of sleep a night, exercise regularly and find healthy ways to relieve stress, such as meditation.
- NSAID use: For pain relief or a fever, use acetaminophen instead of NSAIDs like Motrin® and Advil®.
- Antibiotics: Let your healthcare provider know if antibiotics trigger your symptoms.
Side Effects And Interactions
The more common side effects of biologics can include:
- headache
Biologic drugs may interact with other drugs and biologic agents, including:
- natalizumab , which can be used to treat Crohns disease or multiple sclerosis
- tocilizumab , anakinra , abatacept , which are primarily used to treat arthritis
- warfarin
- theophylline , an asthma medication
- live vaccines such as the varicella zoster vaccine
Recommended Reading: What Over The Counter Medicine For Ulcers
Before Taking This Medicine
You should not use Imodium A-D if you are allergic to loperamide, or if you have:
-
stomach pain without diarrhea
Ask your doctor before using Imodium A-D to treat diarrhea caused by Clostridium difficile.
Ask a doctor before using this medicine if you are pregnant or breastfeeding.
You should not breast-feed while you are using loperamide.
Cured My Uc Through Imodium Ad And Diet
Meet Ben:
I dont use Facebook or Twitter, my life was hell. I hope some people get relief trying what I am doing. I hope this helps.
Some more about Ben:
Raising a family, weight lifting, going to the beach. I live in Melbourne Beach Florida. I am a workaholic that is just now figuring out how to live. Recently I learned about laws of attraction and am applying it to all aspects of life.
Symptoms:
None, from what I have read even in remission your colon should be inflamed, mine is not.
You May Like: What To Eat When You Have Ulcers And Acid Reflux
Imodium With Rehydration Solutions
When treating diarrhea, its important to make sure that youre getting plenty of fluids.
Diarrhea causes you to lose more fluid and electrolytes than usual. And youll need to replace these substances in your body to avoid dehydration .
Children and older people are particularly at risk for dehydration with diarrhea.
Drinking a rehydration solution is a good way to replace fluids and electrolytes lost through diarrhea. Rehydration solutions are drinks that contain both glucose and electrolytes. Pedialyte and Gatorade are examples of rehydration solutions that contain electrolytes. You can buy these drinks at drugstores and grocery stores.
The American College of Gastroenterology recommends rehydration solutions for anyone with watery diarrhea thats severe. But they especially recommend these drinks for children and older people with diarrhea.
What Role Does Diet And Nutrition Play In Ulcerative Colitis
Diet does not cause the development of ulcerative colitis nor can any special diet cure the disease. However, the foods you or your child eat may play a role in managing symptoms and lengthening the time between flareups.
Some foods may make symptoms worse and should be avoided, especially during flareups. Foods that trigger symptoms are different from person to person. To narrow down what foods affect you, keep track of what you eat each day and how you feel afterward .
Problem foods often include:
- High sugar foods and drinks.
- Carbonated beverages.
- High-fiber foods.
- Alcohol.
In addition to the problem foods listed above, infants, children and teenagers can also experience issues with:
- Salt.
- Dairy products.
Keep a careful eye on your childs diet and nutrition. Their appetite may decrease during a flareup and they might not eat enough to stay healthy, and grow. Also, the inflammation caused by ulcerative colitis may keep their digestive tract from absorbing enough nutrients. This can also affect your childs health. For these reasons, you may have to increase the amount of calories your child consumes.
Its best to work with your provider and nutritionist to come up with a personalized diet plan if you or your child has ulcerative colitis.
Don’t Miss: How To Heal Mouth Ulcers Fast
Is There A Cure For Nsaid
Pathogenesis of NSAID-induced colitis is still controversial. Local and/or systemic effects of NSAIDs on mucosal cells might lead to an increased intestinal permeability, which is a prerequisite for colitis. Treatment of NSAID-induced colitis should be to discontinue the drug, or at least, to reduce the dose as much as possible.
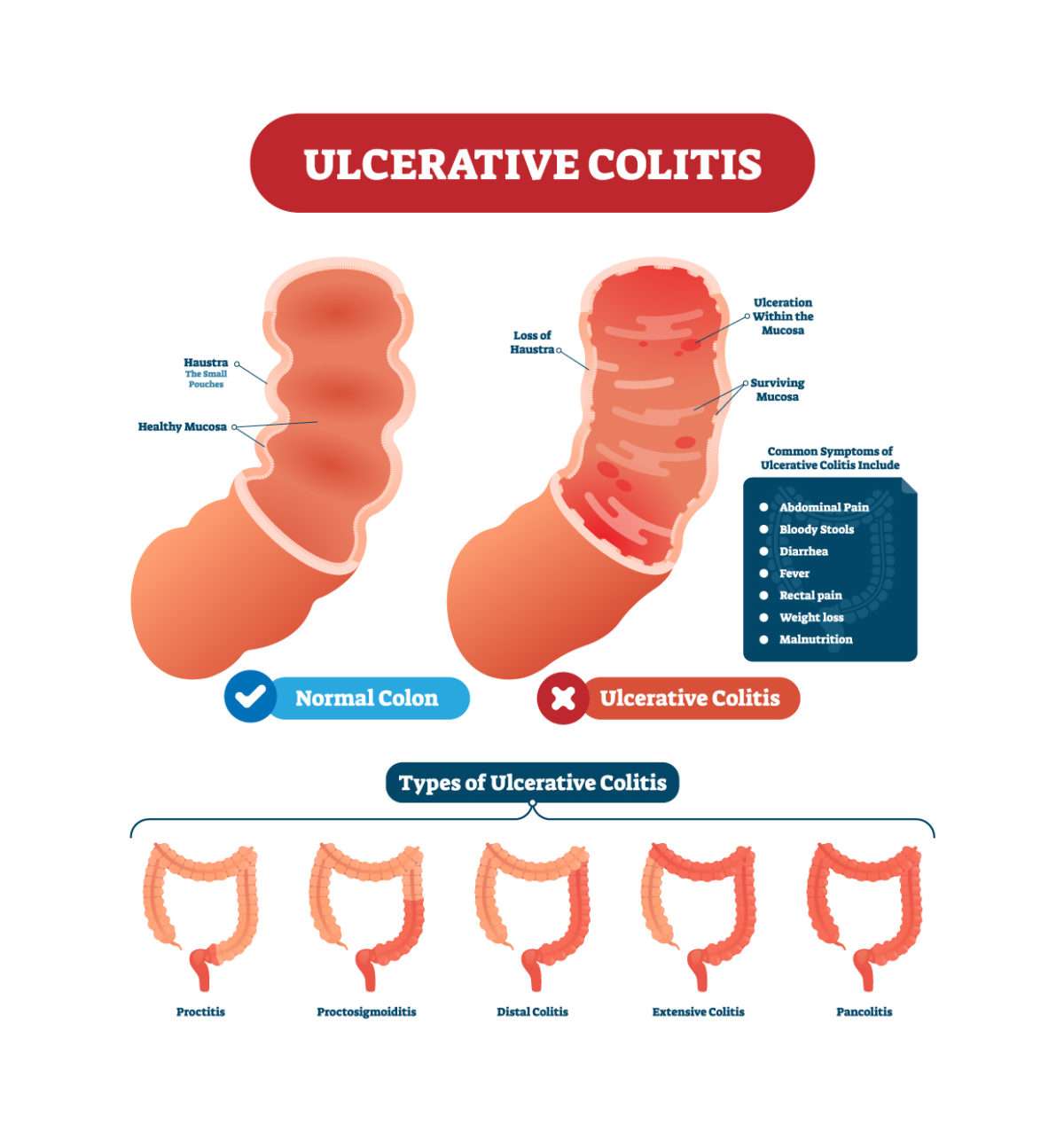
Complications Of Ulcerative Colitis
Although people with ulcerative colitis commonly have minor liver dysfunction, only about 1 to 3% have symptoms of liver disease, which vary from mild to severe. Severe liver disease can include inflammation of the liver , inflammation of the bile ducts , which narrow and eventually close, and replacement of functional liver tissue with scar tissue . Inflammation of the bile ducts may appear many years before any intestinal symptoms of ulcerative colitis. The inflammation greatly increases the risk of cancer of the bile ducts and also seems to be associated with a sharp increase in the risk of colon cancer.
Also Check: Foam Dressing For Pressure Ulcer
What Are The Symptoms Of Ulcerative Colitis
Ulcerative colitis symptoms often get worse over time. In the beginning, you may notice:
- Diarrhea or urgent bowel movements.
- Abdominal cramping.
- Liver disease.
- Loss of fluids and nutrients.
Symptoms are similar in pediatric ulcerative colitis and may also include delayed or poor growth. Some ulcerative colitis symptoms in children can mimic other conditions, so it is important to report all symptoms to your pediatrician.
How Is Ulcerative Colitis Diagnosed
To diagnose ulcerative colitis in children, teenagers and adults, your healthcare provider has to rule out other illnesses. After a physical exam, your provider may order:
- Blood tests: Your blood can show signs of infection or anemia. Anemia is a low level of iron in your blood. It can mean you have bleeding in the colon or rectum.
- Stool samples: Signs of infection, parasites , and inflammation can show up in your poop.
- Imaging tests: Your healthcare provider may need a picture of your colon and rectum. You may have tests including a magnetic resonance imaging scan or computed tomography scan.
- Endoscopic tests: An endoscope is a thin, flexible tube with a tiny camera. Specialized doctors can slide the endoscope in through the anus to check the health of the rectum and colon. Common endoscopic tests include colonoscopy and sigmoidoscopy.
Also Check: How Serious Is A Stomach Ulcer
What Types Of Testing Can Be Done To Identify The Cause Of Chronic Diarrhea
Chronic diarrhea is a sign that nutrients are not being well enough absorbed during the digestive process. Patients who have chronic diarrhea will often undergo blood tests to guide replacement of fluids, electrolytes, and minerals. A blood test can also identify whether the diarrhea is being caused by anemia or a bacterial infection.1
Patients with chronic diarrhea may also undergo fecal testing in order to accurately diagnose the cause. The presence of white blood cells indicates inflammation in the body, potentially due to IBD. If parasites or bacterial cultures are present in the stool sample, this could be the cause of diarrhea.
What Causes Ulcerative Colitis
Researchers think the cause of ulcerative colitis is complex and involves many factors. They think its probably the result of an overactive immune response. The immune systems job is to protect the body from germs and other dangerous substances. But, sometimes your immune system mistakenly attacks your body, which causes inflammation and tissue damage.
You May Like: Food To Avoid For Ulcer Patient
What Is The Best Diet For Ulcerative Colitis
Theres no single diet that works best for ulcerative colitis. If the disease damages the lining of the colon, your body might not absorb enough nutrients from food. Your healthcare provider may recommend supplemental nutrition or vitamins. Its best to work with your provider and nutritionist to come up with a personalized diet plan.