Why Is My Leg Ulcer So Painful
4.9/5ulcerlegULCERulcersvery painfullegulcersulcer
The following advice may help your ulcer heal more quickly.
Also, are venous ulcers painful? Venous ulcers. Venous ulcers usually form below the knee and on the inner area of the ankle. There’s sometimes little or no discomfort, unless the ulcer is infected. In other cases, venous ulcers can be painful.
Then, do leg ulcers hurt when healing?
A venous leg ulcer is a chronic non-healing wound with broken skin and exposed tissue. Venous leg ulcers are usually found on the inside of the leg, just above the ankle. They are often painful, particularly when infected . However, with correct treatment the pain can often be resolved.
Are leg ulcers dangerous?
While the majority of vein illness symptoms are temporary and easily treated, venous leg ulcers are more severe and, when left untreated, can negatively affect your health. What separates venous leg ulcers apart from other diseases is the heightened risk of infection you have through an open sore.
What Is A Leg Ulcer And Why Do They Bleed
Leg ulcers do not start out as giant open sores. They usually start out as small wounds that were caused by a minor injury. Over time, the tiny wound does not naturally heal and the open wound becomes larger and larger.
Typically, a small wound to the leg will heal within a week or two. However, if you experience an underlying problem, such as vein insufficiency, damage can occur to the tissue surrounding the wound and it may not heal. This puts you at risk of developing serious infections that could become life-threatening.
Because leg ulcers do not heal properly and you are left with an open wound, you are at constant risk of reinjuring the area. All it would take is a simple bump or another minor injury to the area and the wound could start to bleed again.
What Causes Ulcers On Old Peoples Legs
arterial leg ulcers caused by poor blood circulation in the arteries. diabetic leg ulcers caused by the high blood sugar associated with diabetes. vasculitic leg ulcers associated with chronic inflammatory disorders such as rheumatoid arthritis and lupus. traumatic leg ulcers caused by injury to the leg.
Recommended Reading: Best Medicine For Ulcerative Colitis
Getting Diagnosed With A Leg Ulcer
If you have a wound or sore that isnt healing, make an appointment at your GP practice as it could turn into or be the beginnings of a leg ulcer. You might be given an appointment to see the nurse rather than the doctor as nurses are often responsible for caring for patients with leg problems.
Alternatively, there might be a Leg Club or specialist leg clinic in your area. You can attend these without having to be referred by your GP.
Remember to remove any nail polish from your toenails before your appointment.
When you see the nurse or doctor, they should:
- Ask about your symptoms and how long you have had problems
- Examine your lower legs
- Do a simple test called a Doppler ultrasound. This test compares blood flow in your ankle with that in your arm to find out if there are blood flow problems in your lower leg. You may have to come back to have your Doppler test on another day or at another clinic.
You may also be offered some other tests to check for other health problems that can affect your legs such as diabetes and anaemia.
If your GP practice thinks you have problems with your veins or arteries, they may refer you for more tests at your local hospital or specialist clinic.
You may hear different words to describe your wound such as ulcer, leg ulcer, sore, laceration, chronic wound and maybe others. Ask your nurse to explain their choice of word and what this may mean for you.
Can Leg Ulcers Be Prevented
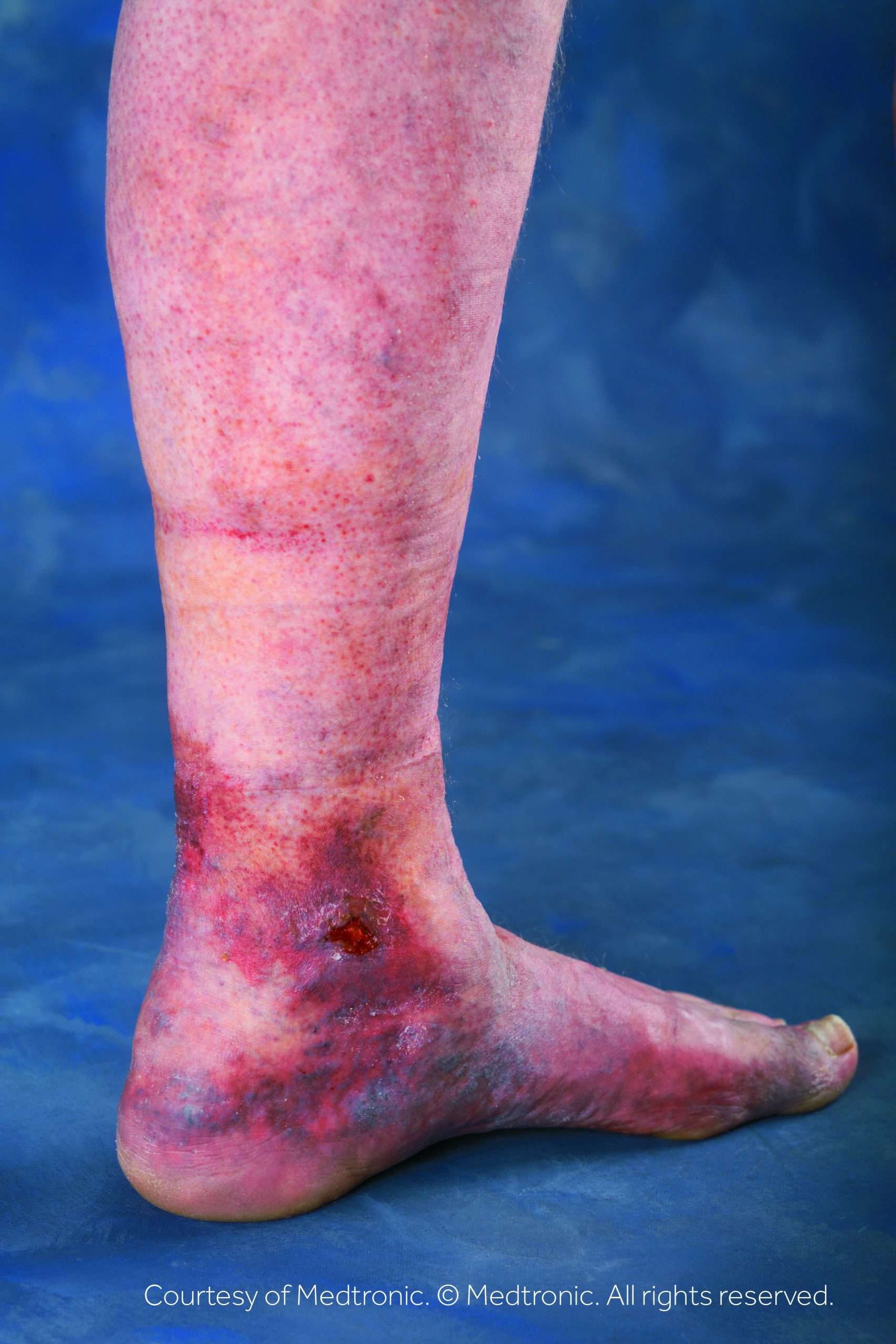
To prevent and promote healing of ulcers:
- Avoid injury, particularly when pushing a supermarket trolley. Consider protective shin splints.
- Walk and exercise for at least an hour a day to keep the calf muscle pump working properly.
- Lose weight if you are overweight.
- Stop smoking.
- Check your feet and legs regularly. Look for cracks, sores or changes in colour. Moisturise after bathing.
- Wear comfortable well-fitting shoes and socks. Avoid socks with a tight garter or cuff. Check the inside of shoes for small stones or rough patches before you put them on.
- If you have to stand for more than a few minutes, try to vary your stance as much as possible.
- When sitting, wriggle your toes, move your feet up and down and take frequent walks.
- Avoid sitting with your legs crossed. Put your feet up on a padded stool to reduce swelling.
- Avoid extremes of temperature such as hot baths or sitting close to a heater. Keep cold feet warm with socks and slippers.
- Consult a chiropodist or podiatrist to remove a callus or hard skin.
- Wear at least Grade 2 support stockings if your doctor has advised these. This is particularly important for the post-thrombotic syndrome, leg swelling or discomfort, and for long-distance flights.
- Have a vascular ultrasound assessment and consult a vascular surgeon to determine whether any vein treatment should be carried out.
- Horse chestnut extract appears to be of benefit for at least some patients with venous disease.
Also Check: Foods To Eat To Heal An Ulcer
How Are Venous Ulcers Treated
Venous ulcers need proper care and treatment to prevent infection and to heal. The Lakeland pain management doctors at the Vein Clinic work with each patient to determine the cause of the ulcer and develop an individualized treatment plan. The treatment goals are to relieve pain, speed recovery, and heal the wound. Treatment may include focusing on the circulatory or vein problems causing the ulcers.
The most common treatment to reduce the swelling is a compression bandage or stocking, which can help improve blood circulation in the legs, boosting the bodys ability to heal the sore. Some compression bandages may require the patient to wear them continuously, with a doctor replacing them every few days. Others are worn only during the day, with the patient putting them on and removing them.
In treating venous ulcers, it is essential to keep the site infection-free. Special medication may be applied under the bandages or stockings to help during the healing process.
If a venous ulcer becomes infected by bacteria, the doctor may prescribe antibiotics to kill the infection. A moist dressing may be used to help the ulcer heal more quickly.
Other treatment options for home care include:
Most venous ulcers heal after 3 or 4 months of treatment. However, some can take longer or require a skin graft to close up the opening in the skin. Some may never clear up completely.
What Treatment Might I Be Offered
Compression therapy if your wound isnt healing because of venous hypertension and there are no problems with the arterial blood supply to your legs, then you should be offered compression therapy. Compression therapy usually works very effectively and helps wounds to heal fast. It is thus essential to find a compression regime that is comfortable, provides the level of support you need and works. If this is inconsistently used or applied, this must be dealt with so that healing is not delayed
Compression therapy improves blood supply by applying pressure to the leg. This can be done by bandaging the lower leg or by wearing supportive socks, stockings or tights. To begin with it can be a little uncomfortable when you first start treatment but should not cause you any pain it should feel supportive to your leg. Any discomfort should reduce as the swelling goes down. If you do experience discomfort, talk to your nurse or doctor about it and they will advise you on ways of alleviating this.
Don’t Miss: How To Check A Horse For Ulcers
How Can I Prevent Or Reduce My Risk Of Foot And Toe Ulcers
It may be possible to reduce your risk of getting ulcers, and even stop them from coming back. Try to:
- Manage your diabetes. If you have diabetes you should wear appropriate footwear and never walk barefoot.
- Every day, examine your legs as well as the tops and bottoms of your feet and the areas between your toes. Look for any blisters, cuts, cracks, scratches or other sores. Also check for redness, increased warmth, ingrown toenails, corns and calluses. Use a mirror to view your leg or foot if necessary, or have a family member look at the area for you. See a healthcare provider immediately if you notice any problems.
- Wear appropriate shoes and socks. Talk to your podiatrist about what you need.
Prevention Of Ulcer Recurrence
Factors that are associated with ulcer nonhealing and recurrence: Overweight body mass index, history of deep venous thrombosis, large ulcer area, noncompliance with compression therapy, and triple-system venous disease involving superficial, perforating, and deep veins . The strategies to prevent the ulcer recurrence should target these factors. These could be implemented as regular clinical evaluations, patient education and life-long compression therapies. Patient’s education should be regarding skin care, elevation of the affected limb when immobile, compliance to compression therapy, encourage mobility, and exercise. To encourage, early self-referral at signs of possible skin breach.
Compression therapy
Use of compression stockings reduces ulcer recurrence and is thus highly recommended in patients of venous leg ulcers. Patients are encouraged to wear the strongest compression they can tolerate for life-long, if not contraindicated otherwise .
You May Like: What Is Acute Ulcerative Colitis
What Are The Types Of Ulcers
There are two types of ulcers that can affect your feet and toes:
- Neurotrophic ulcers.
- Arterial ulcers.
Diabetics can get neurotrophic ulcers. Neurotrophic ulcers can be found anywhere on your feet, but theyre usually on pressure points on the bottoms of your feet. The base, or middle of the ulcer, can look different from person to person. It changes because the appearance depends on your circulation. A neurotrophic ulcer can appear pink, red, brown or black or a combination of these colors. The borders of the ulcers are punched out while the surrounding skin is often calloused.
Anyone can get an arterial ulcer. The word arterial means relating to arteries. Arteries are blood vessels that transport blood from your heart to the rest of your body, including your feet and toes. Arterial ulcers appear on your heels, the tips or your toes, between your toes where they rub against one another and anywhere your bones may protrude and rub against bed sheets, socks or shoes. They also occur commonly in the nail bed if your toenail cuts into the surrounding skin or if you had recent aggressive toenail trimming or an ingrown toenail removed.
Risk Of Bias In Included Studies
Allocation
Risk of selection bias is assessed based on generation of randomisation sequence and allocation concealment. Many studies were at unclear risk of bias for one or both of these, most commonly for allocation concealment. High risk of bias for randomisation was documented for only one study where errors were noted to have compromised the process. However only a minority were considered to have a low risk of bias. The remainder did not report the processes used clearly enough for us to determine the risk of bias. The number of studies considered to be at low risk for allocation concealment was even lower, with only 12 considered to be clearly at low risk of bias.
Blinding
Many studies were at high or unclear risk of performance bias. Although only a minority were clearly at high risk, many more had an unclear risk. Only 10 studies were considered to be at low risk. For detection bias, we observed a similar pattern although more studies clearly had outcomes determined by blinded observers 20 were considered to be at low risk of detection bias.
Incomplete outcome data
Twentysix studies were considered to be at high risk of attrition bias. However, a larger number had a low risk of bias and only ten were considered to be at unclear risk.
Selective reporting
Only four studies were at high risk of selective reporting bias a further 16 had an unclear risk in this domain the remainder were considered to be at low risk of bias.
Other potential sources of bias
Read Also: Is Nausea A Symptom Of Ulcer
How Do I Take Care Of My Ulcers
Your healthcare provider may teach you how to care for your ulcers at home. Some instructions may include:
- Wash the affected area with mild soap.
- Keep the wound clean and dry.
- Change the bandages as directed.
- Take prescribed medications as directed.
- Drink plenty of fluids. Ask your healthcare provider how much water you should drink every day.
- Follow a healthy diet, as recommended by your healthcare provider.
- Exercise regularly, under your healthcare providers care.
- Wear appropriate shoes.
- Wear compression wraps as directed.
Why Might A Wound On The Leg Not Heal And Turn Into A Leg Ulcer
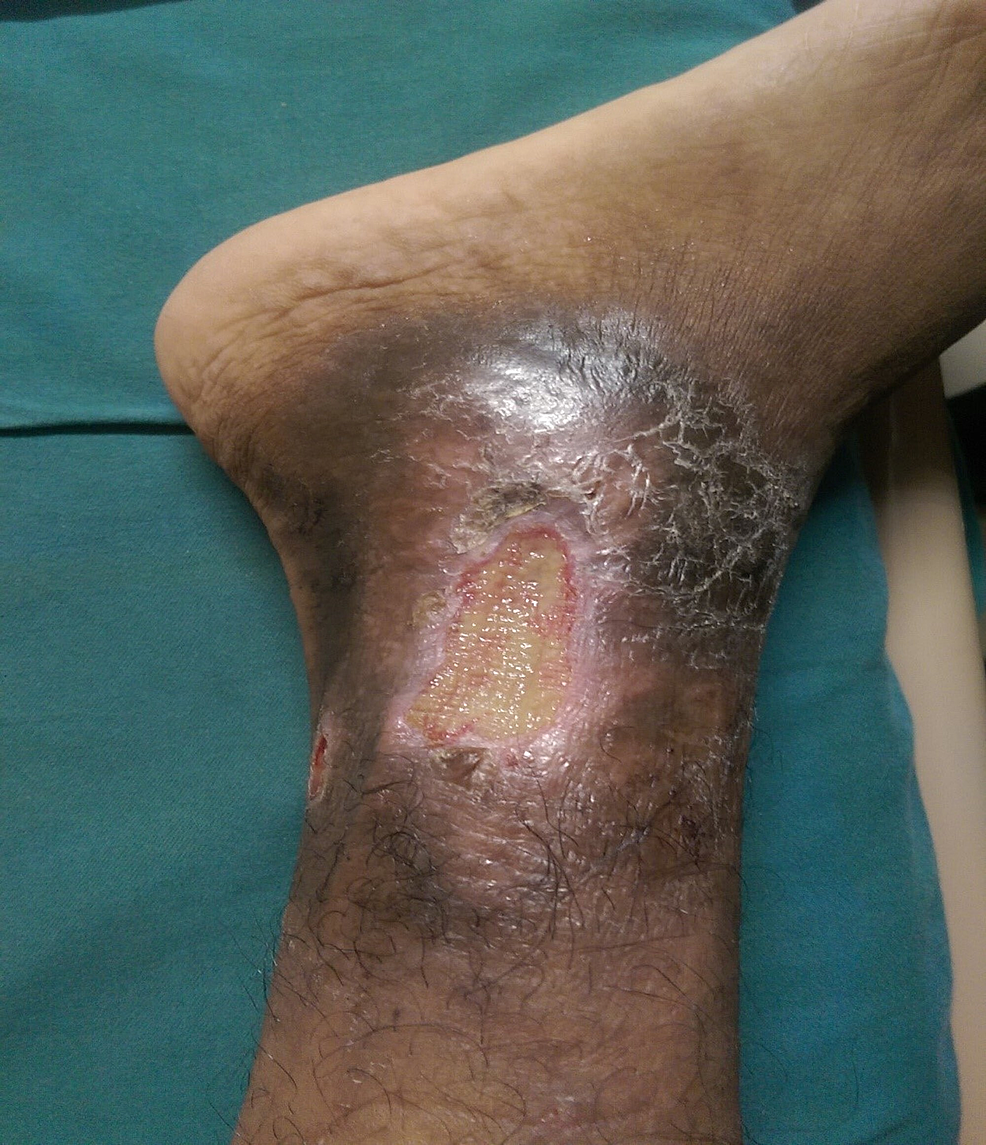
This is because the wound is on the leg and is much more difficult to heal than wounds on another part of the body. We spend a lot of time on our feet and if we have any swelling, this will interfere with healing. If you stand a great deal, or you are carrying excessive weight, this will not help your circulation. Any wound, except those caused by arterial disease will benefit from some form of compression therapy
Read Also: What Not To Eat With Bleeding Ulcers
How The Intervention Might Work
Animal experiments conducted over 40 years ago suggested that acute wounds heal more quickly when their surfaces are kept moist rather than left to dry and scab . A moist environment is thought to provide optimal conditions for the cells involved in the healing process with faster revascularisation , and development of granulation tissue , as well as allowing autolytic debridement , which is thought to be an important part of the healing pathway .
The desire to maintain a moist wound environment is a key driver for the use of wound dressings and related topical agents. Whilst a moist environment at the wound site has been shown to aid the rate of epithelialisation in superficial wounds, excess moisture at the wound site can cause maceration of the surrounding skin , and it has also been suggested that dressings that permit fluid to accumulate might predispose wounds to infection . Wound treatments vary in their level of absorbency, so that a very wet wound can be treated with an absorbent dressing to draw excess moisture away and avoid skin damage, whilst a drier wound can be treated with a more occlusive dressing or a hydrogel to maintain a moist environment.
Some dressings are now also formulated with an ‘active’ ingredient .
Why Do Leg Ulcers Bleed
For most people, a small cut or injury on the leg isnt a big deal as the wound will usually heal itself in a few days. However, for some people leg wounds may not heal naturally and can occasionally start to bleed. When this happens the wound is considered to be a leg ulcer. Leg ulcers are a serious health problem that will only increase in size if proper treatment is not sought. Learn more about what a leg ulcer is, why you may experience more bleeding when you have one, and how it can be treated.
Don’t Miss: Ulcerative Colitis Treatment In India
What Is The Treatment For Leg Ulcers
Where possible, treatment aims to reverse the factors that have caused the ulcer. As an ulcer is often the result of both arterial and venous disease, careful assessment is needed first.
Venous leg ulcer, in the absence of arterial disease, is usually treated with exercise, elevation at rest, and compression. Compression must not be used if there is significant arterial disease, as it will aggravate an inadequate blood supply. Surgery, ultrasound-guided sclerotherapy or endovascular laser treatment of superficial and perforator leg veins may also help, particularly if the deep venous system is intact. Venous-return assisted calf compression devices may be of additional benefit.
A vascular surgeon should also assess patients with arterial leg ulcers as they may require surgery to relieve the narrowing of the arteries. Revascularisation is particularly important if the ABPI is less than 0.5.
It is also very important to treat underlying diseases such as diabetes and to stop smoking.
What Causes Venous Leg Ulcers
The root of the problem is increased pressure of blood in the veins of the lower leg. This causes fluid to ooze out of the veins beneath the skin. This causes swelling, thickening and damage to the skin. The damaged skin may eventually break down to form an ulcer.
The increased pressure of blood in the leg veins is due to blood collecting in the smaller veins next to the skin. The blood tends to collect and pool because the valves in the larger veins become damaged by a previous blood clot in the vein, or varicose veins. Gravity causes blood to flow back through the damaged valves and pool in the lower veins.
Don’t Miss: List Of Foods To Eat When You Have An Ulcer
Should Leg Ulcers Be Kept Dry
Low oxygen tension leads to high levels of oxygen at the capillaries and low levels of oxygen at the wound edges. This provides the ideal environment for wound healing because granulation and wound healing is stimulated. a wound, nurses should remember: If theres no blood supply keep it dry and seek expert advice.
Medical History And Examination
Your GP or practice nurse will ask whether you have any other symptoms associated with venous leg ulcers, such as:
- swelling in your ankles
- discoloured or hard skin
They’ll try to determine the cause of the ulcer by asking about underlying conditions or previous injuries, such as:
Read more about how venous leg ulcers are treated.
Don’t Miss: How Do You Heal Leg Ulcers