Does Ulcerative Colitis Make You Immunocompromised
Ulcerative colitis doesnt make you immunocompromised. Some of the medicines that treat it may change the way your immune system responds. This change is different for each medication. Some of these changes may increase the risk of certain infections or other issues. A discussion with your health care team before starting a medication is the best way to understand these risks and ways to prevent them.
Medication Options For Ulcerative Colitis
Medication is the first line of treatment for ulcerative colitis. Your doctors recommendation for which medication will work best for you is based on the severity of your disease, your overall health, and other individual factors.
There are six major classes of medication used to treat ulcerative colitis.
What Tests Are Used To Monitor Ulcerative Colitis
Doctors have a wide variety of tests that help diagnose and track inflammatory bowel diseases. Imaging tests and colonoscopies are done to check the bowels. Biopsies are sometimes taken to look at cells in the lining of the intestines. Blood tests are used to spot nutritional shortfalls and anemia, a common side effect of ulcerative colitis. Stool sample tests can detect infections in the intestines.
Read Also: What Pain Reliever Is Safe For Stomach Ulcer
Getting A Second Opinion
Patients have choices when it comes to their care team. You will want a team you can trust and can rely on. The first doctor or healthcare professional a patient meets with might not be the right one. Getting a second opinion may be necessary to find the right fit.
Second opinions might be needed to confirm a diagnosis, to change medications or manage complications, or before having surgery.
How To Manage Ulcerative Colitis At Home
Along with your treatment plan, your doctor may recommend making some dietary adjustments at home to help you manage the disease. While diet doesnt cause ulcerative colitis, nor does it cure the disease, some foods may play a role in making your symptoms worse.
Foods that trigger symptoms will vary for each person. So, the best thing to do is keep a food journal that tracks what you eat and how you feel afterward. This way you can identify your triggers. That said, The Cleveland Clinic says some common problem foods include high-sugar foods and drinks, greasy foods, alcohol, and carbonated beverages.
Don’t Miss: What Are Some Symptoms Of An Ulcer
Diet And Lifestyle Changes
Although diet and stress do not cause ulcerative colitis, there may be times when changes in your lifestyle may help control your symptoms and lengthen the time between flare-ups. The following changes may help to ease your symptoms:
- Limit milk/dairy products. If you are lactose intolerant , milk and dairy products can produce symptoms of excess gas and diarrhea.
- Restrict intake of certain high-fibre foods: such as nuts, seeds, and raw vegetables.
- Limit intake of caffeine, alcohol, carbonated drinks and fatty foods. .
- Eat small, frequent meals, rather than large meals..
- Exercise regularly to promote movement of the colon and reduce stress..
- Minimize stress. Yoga, meditation and slow, relaxed breathing techniques can help people with ulcerative colitis manage stress..
Ask your doctor or pharmacist if one of these formulations may be right for you. It is important to take the probiotic in the dose and duration recommended by the manufacturer to achieve the best results.
You May Need More Than One Treatment To Keep You In Remission
Everyone responds differently to UC treatments.
Some people will need more than one drug to manage their symptoms. For example, your doctor might prescribe both a biologic and an immunosuppressant medication.
Adding on another drug can increase the effectiveness of your treatment. But taking more than one medication can also increase the number of side effects you experience.
Your doctor will balance your need for symptom control with possible risks of treatment when choosing a medication for you.
40 to 60 percent of people with UC who use mesalamine, thiopurines, and anti-tumor necrosis factor antibodies will have remission that lasts for a year.
If a drug leads to remission, the person will continue to take it. If they stop, the symptoms may return.
Recommended Reading: Is Peppermint Tea Good For Ulcerative Colitis
How Your Doctor Will Assess Your Current Treatment Plan
Your doctor will likely want to rule out other possible causes of your symptoms. At your appointment, youll be assessed to see if the symptoms are the result of a UC flare, an infection, or another condition like irritable bowel syndrome , explains David P. Hudesman, MD, a gastroenterologist and the codirector of the inflammatory bowel disease center at NYU Langone Health in New York City.
Tests you may undergo include blood tests, stool studies, and a colonoscopy, he says.
One possible reason for worsening symptoms is that youre not taking your medication exactly as prescribed. A study published in March 2019 in the journal PLoS One found that about 50 percent of patients with UC did not take their medications correctly. Those who were under 40, smoked, and drank alcohol were more likely not to adhere to their treatment plan properly. Research published in the journal Inflammatory Bowel Diseases found that more than 60 percent of patients admitted to not taking their medication as directed. Reasons included too many pills, too frequent dosing intervals, not wanting to use rectal applications, and simply forgetting.
Additionally, eating certain foods can provoke a return or worsening of symptoms, as can being under a great deal of stress.
Finding The Best Team
Most people who live with IBD will have a team of physicians that they are working with. You will want to get referrals or reach out to specialists as needed, or on a yearly basis for a check in.
Beyond asking a primary care physician and family or friends for recommendations, patients can also seek out nonprofit patient advocacy groups and professional physician societies to find a list of specialists. Patients will want to find a physician that has IBD or ulcerative colitis as their specialties of interest in order to get more targeted care.
You May Like: What Does A Venous Leg Ulcer Look Like
What Are The Signs And Symptoms Of Ulcerative Colitis
The most common signs and symptoms of ulcerative colitis are diarrhea with blood or pus and abdominal discomfort. Other signs and symptoms include the following:
- an urgent need to have a bowel movement
- feeling tired
- anemiaa condition in which the body has fewer red blood cells than normal
Less common symptoms include the following:
- joint pain or soreness
- eye irritation
- certain rashes
The symptoms a person experiences can vary depending on the severity of the inflammation and where it occurs in the intestine. When symptoms first appear,
- most people with ulcerative colitis have mild to moderate symptoms
- about 10 percent of people can have severe symptoms, such as frequent, bloody bowel movements fevers and severe abdominal cramping.
Testing For Ulcerative Colitis
Often, symptoms alone can provide doctors with the information they need to diagnose ulcerative colitis. Your doctor will perform a physical examination and take a complete medical history that includes a careful review of your symptoms. For this reason, it is important to be candid and specific with your doctor about the problems you are having.
There is no one specific laboratory test, X-ray or scope to diagnose ulcerative colitis, however, to help confirm the condition and rule out other problems, your doctor may send you to have one or more of the following tests:
Don’t Miss: How To Ease Stomach Ulcer Pain
Innovating The Standard Of Care Through State
The Crohns and Colitis Center offers the full range of state-of-the-art management of IBD as well as innovative medical therapies and treatment strategies. Our physicians are experienced in formulating a personalized, patient-centered therapeutic algorithm incorporating trajectory of disease as well as individual patient preferences. They also help patients obtain relief from persistent, difficult-to-manage symptoms. They are known around the world for their experience treating inflammatory bowel disease and have been involved in the formulation of many national and international treatment guidelines for their complex diseases.
Our physicians are also pioneers in the field and are actively involved in many clinical trials and research of promising new investigational medications, biological agents, and interventions to treat inflammatory bowel diseases. An average of 8-10 clinical trials are active in our center at any given time. All of our treating gastroenterologists are members of the Crohn’s and Colitis Foundation of America and American Gastroenterological Association, and regularly lecture at other institutions as well as many regional, national and international conferences on the management of inflammatory bowel diseases.
What Else Can I Do To Improve My Health With Ulcerative Colitis

If you smoke, set a goal to stop. Studies show that smoking worsens the symptoms of inflammatory bowel disease, especially Crohn’s. Smoking also adds to cancer risk.
Finding ways to ease stress may also help you control your symptoms. Stress doesn’t cause inflammatory bowel disease, but it can make your symptoms feel worse and may trigger flare-ups. Many people find that moderate exercise, relaxation techniques, or soaking in a warmth bath can help.
Recommended Reading: Is Cranberry Juice Good For Ulcers
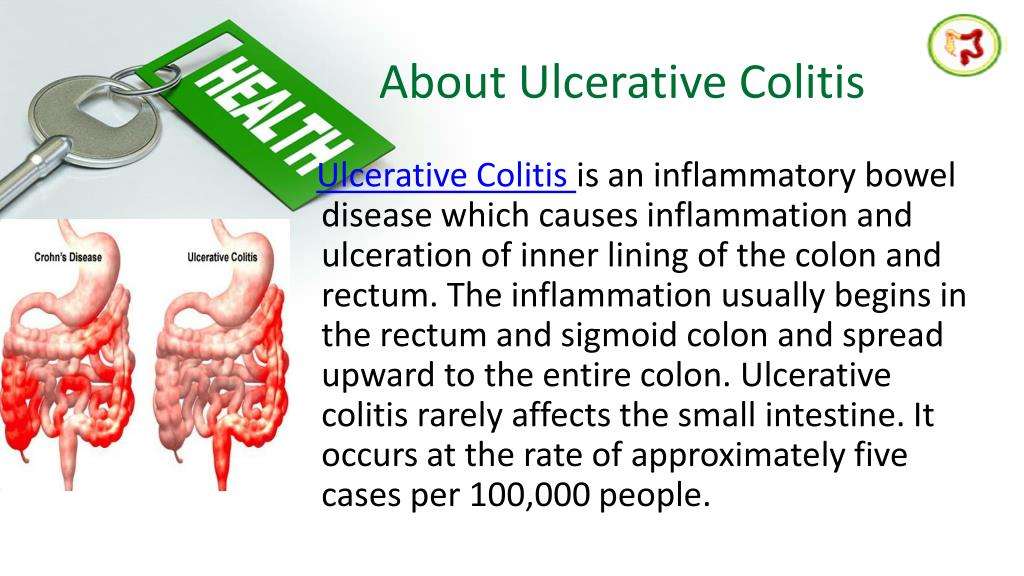
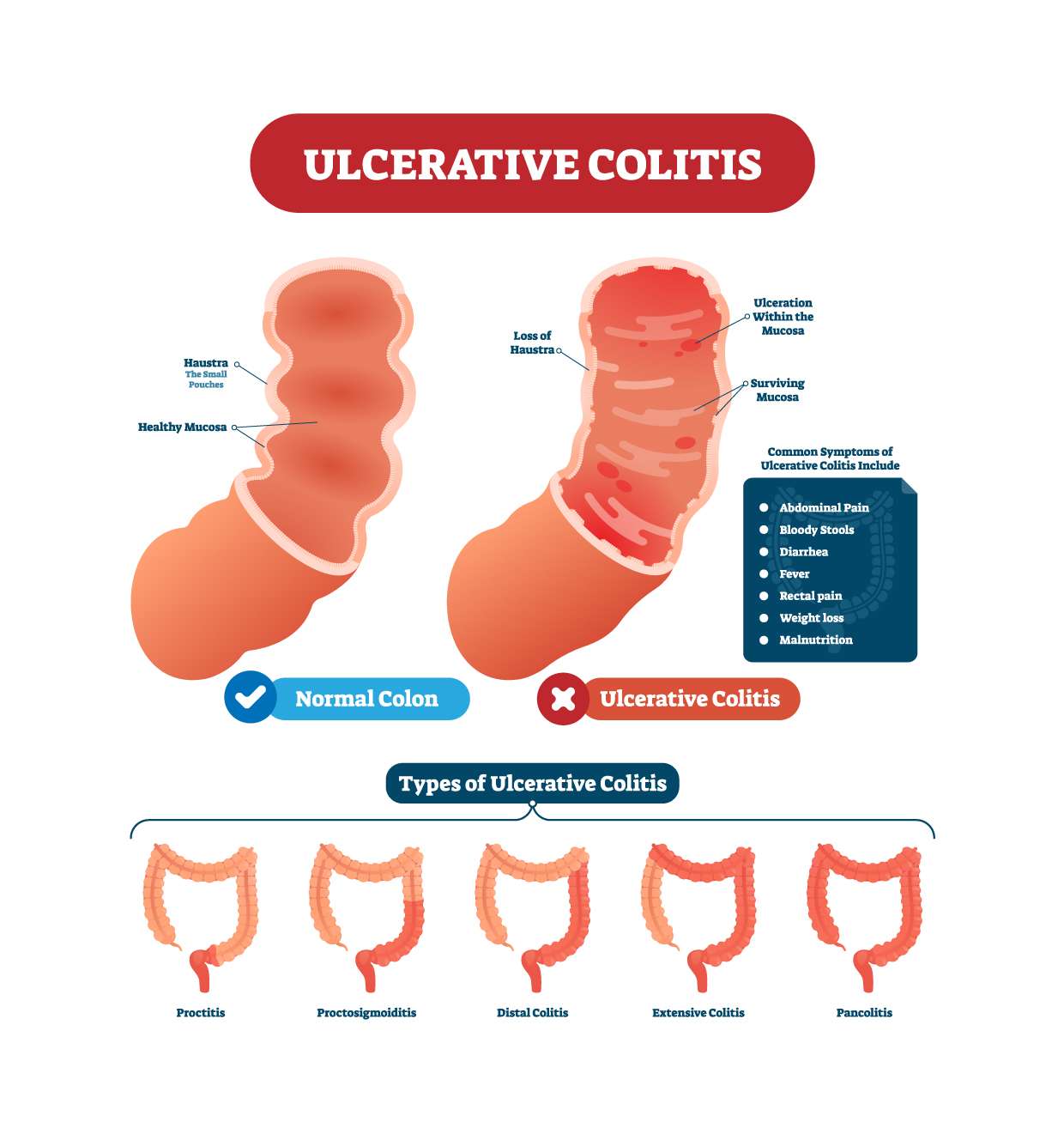
What Is Ulcerative Colitis
Ulcerative colitis causes irritation and ulcers in the large intestine . It belongs to a group of conditions called inflammatory bowel disease . It often causes diarrhea with blood, cramping and urgency. Sometimes these symptoms can wake a person up at night to go to the bathroom as well.
The inflammation in ulcerative colitis usually starts in the rectum, which is close to the anus . The inflammation can spread and affect a portion of, or the entire colon. When the inflammation occurs in the rectum and lower part of the colon it is called ulcerative proctitis. If the entire colon is affected it is called pancolitis. If only the left side of the colon is affected it is called limited or distal colitis.
The severity of UC depends on the amount of inflammation and the location. Everyone is a little different. You could have severe inflammation in the rectum or very mild inflammation in the entire colon .
If you have ulcerative colitis, you may notice a pattern of flare-ups , when symptoms are worse. During times of remission, you might have little to no symptoms. The goal with therapy is to remain in remission as long as possible .
Living With Ulcerative Colitis
Getting the right treatment for ulcerative colitis can make a big difference to your symptoms, but there is more to living with IBD than just taking medication. Its important to:
- Eat a healthy diet and take supplements if necessary
- Drink plenty of fluids, but avoid caffeine, alcohol and fizzy drinks
- Have someone to talk to, whether its a friend, relative, or a local or online support group
- Discuss the situation with your employer so that you can make adjustments when necessary
- Find a way to manage stress and anxiety, which can make your symptoms worse. Exercise, yoga or mindfulness could help.
Living with ulcerative colitis can be difficult, especially because flare ups are so unpredictable. Its important not to underestimate the emotional impact it can have. Youll have to make some big changes in your life so make sure that you have the support you need from your doctor at the London Gastroenterology Centre as well as your friends and family.
Don’t Miss: What Is A Vascular Ulcer
Colon Cancer And Ulcerative Colitis
When you have ulcerative colitis, you may be more likely to get colon cancer. Your chances go up if you dont get treatment for UC. Thats because unchecked inflammation can cause changes in the cells in your colon. These cells may turn into cancer down the road.
Your chances of getting colon cancer go up if youve had ulcerative colitis for 8 years or longer. The odds are also higher if:
- Your inflammation doesnt go away.
- Youre a man.
- You have a liver condition called primary sclerosing cholangitis.
- You have a family member whos had colon cancer.
Some research shows that people with UC may be less likely to get colon cancer now than in the past. Experts think its because doctors now have better ways to screen for colon cancer and they do it more often. It also helps that new medicines, like biologics, do a good job of curbing inflammation.
Signs Your Ulcerative Colitis Treatment Isnt Working
After a while on one treatment plan, you may find that your medication doesnt work as well as it used to. Dr. Philpott says that an increase in your bowel movements, trouble or pain passing stool, weight loss, fevers, blood in stool, and fatigue could be signs that its time to discuss a change with your doctor. But, she cautions, It is important to be aware that sometimes these symptoms can occur for a different reason. That is why your healthcare provider should do some tests when this occurs, to identify what is causing the problem.
According to Kane, If you are feeling worse on the medication than off it, it is time to have a discussion with your doctor. Dont be afraid to speak up. Your doctor assumes everything is okay unless you say something, says Kane. She recommends you start by saying something like: Im not sure that my medicine is doing what its supposed to because and then going into detail about your symptoms. Your doctor will appreciate your honesty, she adds.
Philpott says its also important to be prepared going into your appointment. Things to discuss with your healthcare provider would be what the specific symptoms are, when they started, and if notice a fluctuation over time. For example, she says, if youre taking an injection and notice that symptoms start recurring when youre due for the next injection, thats important to note.
Also Check: Symptoms Of Having Ulcers In Your Stomach
How Do Drugs Used To Treat Ulcerative Colitis Work
- Aminosalicylates work in the lining of the large intestine, including the rectum, to decrease cellular inflammation and heal sores.
- Corticosteroids suppress the entire immune response instead of specific parts that cause inflammation. They act on the white blood cells to reduce the chemicals that increase inflammation. Steroid use can cause side effects such as poor bone health, muscle weakness, weight gain, skin bruising skin and increased risk of infection. Because of this, these medications cant be stopped abruptly and require medical supervision.
- Immunomodulators also suppress the immune response but may take several months to take effect, which is why they are often used when the drugs above either do not work or have only partially worked. Some immunomodulators are used to enhance the effectiveness of other medications. Immunomodulatory therapy requires monitoring, with periodic assessments of blood counts and blood tests to anticipate any negative side effects.
- block the JAK enzyme inside white cells. They prevent inflammation by reducing levels of substances called cytokines in the blood. These work well in severe cases of UC.
- Biologics and biosimilars are lab-made antibodies that stop certain proteins in the body from causing inflammation. These may be given orally or as shots and need careful medical supervision.
Ulcerative Colitis Vs Crohns Disease
Ulcerative colitis is similar to Crohns disease, another type of IBD. However, Crohns can affect any part of the gastrointestinal tract, while ulcerative colitis only causes inflammation of the large intestine.
It is important to distinguish between ulcerative colitis and other diseases that cause similar symptoms like Crohns disease, irritable bowel syndrome, celiac disease or cancer because these diseases require different therapies for effective treatment.
Early diagnosis of ulcerative colitis can lead to earlier therapy, which can help prevent serious complications, including hospitalization and surgery. Up to one in every four patients with ulcerative colitis will need surgery, but better medications are reducing that need.
You May Like: Oral Antibiotics For Leg Ulcers
Ulcerative Colitis Care At Uvm Medical Center
At the UVM Medical Center, we have a team of gastroenterologists who work together to provide advanced, personalized care. Our doctors are trained in the latest technology to diagnose and treat ulcerative colitis.
Each patient is unique, therefore our recommended treatment plans will be designed specifically for you. Your treatment plan will depend on the severity of your ulcerative colitis and your preferences. When you receive care at the UVM Medical Center, you will be seen & treated by some of the best doctors in the area.
You Dont Need To Change Your Diet Dramatically
Theres no evidence that following a strict diet can put you into remission or keep you there. In fact, cutting out certain foods could prevent you from getting the nutrients you need to stay healthy.
You may want to avoid certain foods like dairy products if they seem to aggravate your symptoms. However, talk with your doctor or a dietitian before making any major changes to your diet.
You May Like: Diet Plan For Ulcerative Colitis Flare Up
Its Important To Stay The Course
Never stop your ulcerative colitis medication unless directed by your doctor. Adhering to the treatment that was prescribed to you decreases your chances of a flare and reduces your risk of colon cancer. If youre in remission and have been doing well for a long time, then you might talk to your doctor about reducing your medication dosage and changing your dosing schedule.
Gastroenterologists & Certified Nutritionists Located In The Villages Leesburg & Wildwood Fl
Every year, around 70,000 Americans develop an inflammatory bowel disease like ulcerative colitis. At Gastroenterology & Nutrition of Central Florida, skilled gastroenterologists Nehme Gabriel, MD, and Raj Borade, MD, offer full-scale ulcerative colitis care, including medication and surgery, based on your needs. Call the office in The Villages, Leesburg, or Brownwood Paddock Square in Wildwood, Florida, or use online scheduling.
You May Like: What Not To Eat With Bleeding Ulcers