Articles On Managing Ulcerative Colitis
Ulcerative colitis can make life hard to predict. A flare-up of symptoms is stressful and can leave you worn out for days, weeks, or even months. Even in remission, you might get tired a lot or have a hard time meeting friends or going to work. Itâs easy to see why living with this long-term inflammatory disease can affect your mental health.
There’s no evidence that stress actually causes inflammatory bowel disease , which includes UC and Crohnâs disease. But stress can definitely bring on a flare-up. And you’re more likely to feel anxious and depressed than your friends without UC. Your chances are even higher if you are a woman. Even rats with IBD in lab studies show signs of mood problems.
But there are steps you can take to lift your mood, even when your symptoms get you down.
Response To Acute Stress In The Presence Of Chronic Stress
The physiological and immune response to acute experimental stress is exaggerated by the presence of chronic psychological stress . Individuals with high chronic stress levels, such as those caring for a long term dependent or women with a strong family history of breast cancer, showed greater and more prolonged increases in sympathetic activation in response to acute stressors than controls. This was associated with a greater increase in NK cell numbers, albeit with an attenuated increase in their activity, in the chronically stressed subjects than in controls.
Table 1
Summary of the effects of adverse life events and acute experimental stress on systemic immune and inflammatory function in humans
What Is Inflammatory Bowel Disease
Inflammatory bowel disease causes parts of the intestine to get red and swollen . It’s a chronic problem, which means it lasts a long time or constantly comes and goes.
There are two kinds of IBD: Crohn’s disease and ulcerative colitis. These diseases have many things in common, but there are important differences:
- Crohn’s disease can happen in any part of the gastrointestinal tract from mouth to anus . Crohn’s disease damages the entire bowel wall.
- Ulcerative colitis happens only in the large intestine, also called the colon. It causes sores called ulcers on the inner lining of the colon.
What Are the Signs & Symptoms of Inflammatory Bowel Disease?
The most common symptoms of IBD are belly pain and diarrhea. Other symptoms include:
- blood in the toilet, on toilet paper, or in the poop
- fever
- weight loss
When symptoms happen, its called a flare-up.
IBD can make it hard for someone to get all the calories and nutrition they need. Some kids and teens may grow slowly or start puberty later than usual. It can cause other problems, such as rashes, eye problems, joint pain and arthritis, and liver problems.
Recommended Reading: Carbohydrate Diet For Ulcerative Colitis
Exercise To Reduce Inflammation
A study published in June 2019 in the journal Acta Clinica Croatica found that moderate exercise is beneficial for people with IBD because it can improve quality of life and reduce disease activity.
People with IBD tend to avoid physical activity because of their abdominal pain or other discomfort, says Dr. Axelrad. However, I encourage them to push through, because physical activity can improve fatigue and some disease activity.
Crohns and Colitis UK advises against strenuous activity, though, since intense exercise has been shown to exacerbate inflammatory symptoms. If you want to start a fitness regimen, consider taking up brisk walking, cycling, swimming, or a sport such as soccer or tennis.
What Are The Symptoms Of Ulcerative Colitis
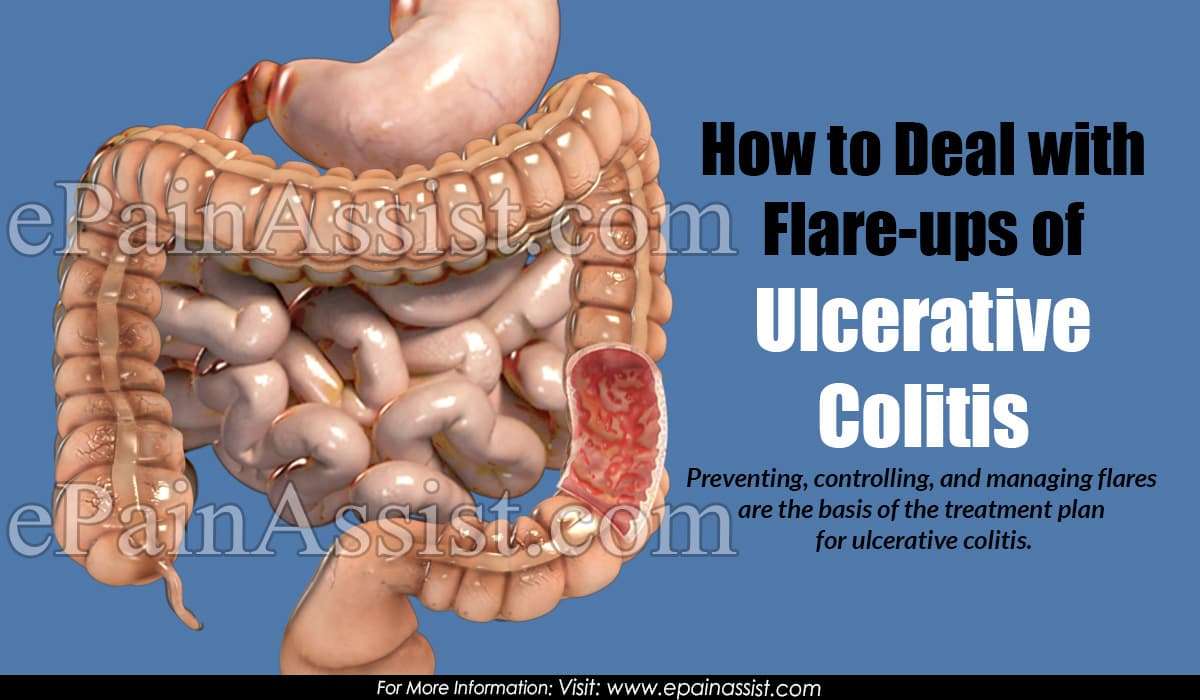
Ulcerative colitis symptoms often get worse over time. In the beginning, you may notice:
- Diarrhea or urgent bowel movements.
- Abdominal cramping.
- Liver disease.
- Loss of fluids and nutrients.
Symptoms are similar in pediatric ulcerative colitis and may also include delayed or poor growth. Some ulcerative colitis symptoms in children can mimic other conditions, so it is important to report all symptoms to your pediatrician.
Read Also: Can I Eat Oatmeal With Ulcerative Colitis
The Role Of Crf In Mediating Stress Related Gastrointestinal Changes In Animal Models
CRF is a 41 amino acid neuropeptide which exerts its effects via two adenylate cyclase coupled receptors, CRF-R1 and CRF-R2. It has a pivotal role in mediating the effects of stress on the gastrointestinal tract in animal models, some of which may be relevant to stress induced increases in IBD activity in humans.
Central injection of CRF in the rat induces behaviour normally seen in response to stressful stimuli. It also reproduces the motility changes usually seen in response to stress, with decreased gastric emptying and increased colonic motility. The use of selective CRF receptor antagonists has proven that central CRF increases colonic motility via stimulation of CRF-R1 and delays gastric emptying via stimulation of CRF-R2.
CRF levels are increased in caecal biopsies from rats with experimental colitis induced by intramural injection of peptidoglycan-polysaccharide polymers. In the chronically inflamed caecum, abundant immunoreactive CRF was found in inflammatory cells, mesenchymal cells, and myenteric plexi in contrast, in non-inflamed caecum only minimal CRF containing cells were found. Whether CRF has a role in mediating stress related gastrointestinal changes in humans with IBD is unknown. However, there is some evidence of a functional role for CRF in the pathogenesis of IBD as CRF levels are increased in lamina propria mononuclear cells in colonic biopsies from patients with active UC.
Understanding Stress And Anxiety In Ibd
Video Length1:25
Understanding Stress and Anxiety in IBD While stress and anxiety has not been shown to cause Crohn’s disease or ulcerative colitis, they can certainly have an impact on your disease. Learn more!
- Transcript
|
|
|
|
|
Don’t Miss: Bland Diet Recipes For Ulcers
Impact On Sexual Health By Depraved Physical Health Due To Ulcerative Colitis
- In ulcerative colitis there is frequent emptying of the stomach which leads to impaired uptake of nutrients .
- Due to impaired uptake of nutrients the deficiency of various minerals,vitamins like vitamin d, vitamin b, vitamin c, aspartic acid etc, Basic proteins and essential amino acids take place.
- Excessive bleeding in stools lead to poor red blood cell count, low iron levels and hence poor body status.
- Low sperm motility
- Low levels of testosterone and estrogen.
- Blood is the connective tissue in the body and prominent in circulation of oxygen therefore poor red blood cell levels hamper the oxygen supply in male genitals, lead to impaired erections and badly affect sexual health.
- Similarly in females low oxygen level due to poor circulation impaired the health status of female genital status.
Stress: Pathways And Pathophysiology
More than 80 years ago, Hungarian endocrinologist Hans Hugo Bruno Selye first defined the medical term stress as the physiological adaptive responses of organisms to adverse threats , which are endogenous or exogenous, psychological or physical, real or perceived . To maintain homeostasis under threat, organisms have evolved an extremely complex system, called the stress system, which involves physiological and behavioral adaptations via appropriate central and peripheral neuroendocrine responses. When exposed to long-term or severe stress, the organisms may reach a state called cacostasis, in which many vital physiological functions are impaired, and may develop many acute and chronic diseases . Stress-induced disorders occur in multiple systems throughout the body, among which the gastrointestinal tract is a sensitive system.
When the brain receives stress input, multiple pathways containing the autonomic nervous system and hypothalamic-pituitary-adrenal axis are activated . Stress from different sources results in modifications of the brain-gut axis, which eventually leads to the progression of a wide range of gastrointestinal disorders. The frequently involved diseases include IBD, irritable bowel syndrome , peptic ulcers, food antigen allergic reactions, and gastroesophageal reflux disease. The potential mechanisms are summarized in the following sections .
You May Like: Stage 2 Pressure Ulcer Treatment Cream
Encountering Emotional Stressors And Facing Them
Possible Emotional Stressors
Other Peoples Perception of UCIts hard if you feel isolated because people around you dont understand how your condition affects you. The symptoms of UC can often be invisible on the outside and you could be worried that others may see you differently because of your condition.
Ways You Can Face Them
Refuse to Suffer in SilenceIf you’re concerned that others don’t understand what you’re going through, try your best to talk about it. Open up and crush the stigma. Educate others that may not understand the facts and let go of the people who refuse to understand. Keep the people who really want to understand and support you close.
Having Symptoms at Work or SchoolWorrying about how to manage your UC symptoms when youre not in the comfort of your own home can be hard. Especially if you arent getting what you need, like a flexible schedule or support from your boss. And while you may know your rights as a patient with a medical condition, sometimes there are negative impacts, like unsupportive people, that are outside your control.
Being in Social SituationsIt can feel easy to stay isolated and keep yourself at home. But every now and then everyone needs to get out and have fun. Thinking of your UC might hinder you from doing things like going to parties, seeing friends, or attending events.
Possible Emotional Stressors
Ways You Can Face Them
Ways To Manage Symptoms And Flares Of Ulcerative Colitis
A flare of ulcerative colitis can be painful and embarrassing not only for you, but for those around you. Once you have one flare, are you going to have more? That anxiety can make you feel even worse and trigger one. Lets investigate 6 ways to manage symptoms and flares of ulcerative colitis.
Read Also: Can Ulcerative Proctitis Be Cured
Can You Prevent Ulcerative Colitis
Because experts arent sure what causes someone to get ulcerative colitis, there isnt much you can do to prevent it. If youre at higher risk for the disease due to a family history or other factors, certain steps may help improve gut health. These same actions can also reduce your risk of a flare-up or worsening of symptoms if you have the disease.
Steps to prevent or manage ulcerative colitis:
-
eat a low-fat, nutritious diet
-
find healthy ways to manage stress
-
get plenty of sleep
-
keep a food diary to figure out which foods cause symptoms
-
maintain a healthy weight and stay physically active
-
use a pain reliever like acetaminophen instead of an NSAID
General Causes Of Ulcerative Colitis
The exact cause for ulcerative colitis continues to be not acknowledged. However, researchers link the sickness to:
- A combination of environmental factors.
- A system that is awry.
- Genetic predisposition.
- A microorganism or microorganism infection within the colon, that initiates uncontrolled inflammation that is closely joined to colitis.
The condition may additionally be aggravated by the sort of diet and stress. For example consumption of Trans fats in masses will increase the danger of the condition. These fats square measure chiefly in processed foods. On the opposite hand, the intake of Omega -3 fatty acids in massive quantities lowers the danger of developing the condition.
Read Also: How To Get Remission In Ulcerative Colitis
When To Seek Medical Advice
You should see your GP as soon as possible if you have symptoms of ulcerative colitis and you haven’t been diagnosed with the condition.
They can arrange blood or stool sample tests to help determine what may be causing your symptoms. If necessary, they can refer you to hospital for further tests.
Read more about diagnosing ulcerative colitis.
If you’ve been diagnosed with ulcerative colitis and think you may be having a severe flare-up, contact your GP or care team for advice. You may need to be admitted to hospital.
If you can’t contact your GP or care team, call NHS 24 111 service or contact your local out-of-hours service.
Southern Cross Medical Library
The purpose of the Southern Cross Medical Library is to provide information of a general nature to help you better understand certain medical conditions. Always seek specific medical advice for treatment appropriate to you. This information is not intended to relate specifically to insurance or healthcare services provided by Southern Cross. For more articles go to the Medical Library index page.
Don’t Miss: Foods You Can Eat With An Ulcer
How To Manage Ulcerative Colitis Flares
Although there isnt a cure for ulcerative colitis, there are plenty of treatment options to reduce inflammation and help you return to your daily routine. Depending on the severity of your flare-up and your individual needs, your healthcare provider can recommend treatment to help you manage ulcerative colitis flares.
The end goal of treatments for ulcerative colitis flare-ups is to maintain remission. You might always have ulcerative colitis, but if you care for yourself you can avoid intense flare-ups. Your healthcare provider might recommend a medication to reduce swelling, heal tissue, relieve symptoms, reduce pain, and avoid diarrhea:
You can’t completely avoid flare-ups. If you eat well and take your medicine as prescribed, its likely that your disease will stay in remission. See your healthcare provider regularly to make sure that youre always doing whats best for your body, even when its been a while since you had a flare-up.
Ulcerative colitis flares can affect how you travel, your personal relationships, your professional life, and more. The most important thing you can do is to face your fears and worries instead of letting them control your life.
What Is Ulcerative Colitis
This chronic inflammatory bowel disease causes unpredictable diarrhea and pain in the abdomen. Other common symptoms include: urgent and frequent bowel movements, bloody stool, abdominal pain, nausea and vomiting, and weight loss. You may have periods with no symptoms, and then suddenly, the pain and trips to the bathroom return.
Sometimes remission can last for weeks, months, or even years.
Once you receive a confirmed diagnosis by Colorectal Surgical Associates, proper treatment can begin which should give you some relief from this condition.
You May Like: What Does A Skin Ulcer Look Like
Acute Psychological Stress And Gastrointestinal Motility And Water And Ion Secretion
Figure 2
Pathways by which the enteric nervous system is likely to mediate stress induced increases in inflammatory bowel disease symptomatolgy and disease activity. CRF, corticotrophin releasing factor SP, substance P IL, interleukin.
Acute psychological stress has effects on gastrointestinal motility, and water and ion secretion. Thus in healthy human volunteers, acute short term stress in the form of painful stimuli, dichotomous listening tests, and stressful interviews enhanced colonic motility. Dichotomous listening tests and cold pain stress have also been shown to increase jejunal water and sodium and chloride ion secretion. Although these are non-inflammatory changes, they could contribute to stress induced increases in symptomatology in patients with IBD.
What Role Does Diet And Nutrition Play In Ulcerative Colitis
Diet does not cause the development of ulcerative colitis nor can any special diet cure the disease. However, the foods you or your child eat may play a role in managing symptoms and lengthening the time between flareups.
Some foods may make symptoms worse and should be avoided, especially during flareups. Foods that trigger symptoms are different from person to person. To narrow down what foods affect you, keep track of what you eat each day and how you feel afterward .
Problem foods often include:
- High sugar foods and drinks.
- Carbonated beverages.
- High-fiber foods.
- Alcohol.
In addition to the problem foods listed above, infants, children and teenagers can also experience issues with:
- Salt.
- Dairy products.
Keep a careful eye on your childs diet and nutrition. Their appetite may decrease during a flareup and they might not eat enough to stay healthy, and grow. Also, the inflammation caused by ulcerative colitis may keep their digestive tract from absorbing enough nutrients. This can also affect your childs health. For these reasons, you may have to increase the amount of calories your child consumes.
Its best to work with your provider and nutritionist to come up with a personalized diet plan if you or your child has ulcerative colitis.
Also Check: Signs And Symptoms Of Ulcerative Colitis Flare Up
My Experience With The Covid
With the vaccine behind me, I feel hopeful for the future for the first time in over a year.
Having an autoimmune disease is tough physically, mentally, and emotionally. Having an autoimmune disease during a pandemic? That is a completely new experience that I wasnt prepared for.
I have ulcerative colitis , a type of inflammatory bowel disease , and have been fighting a flare-up off and on throughout all of 2020. I like to say that I was quarantining before quarantining was cool.
I finally felt a glimmer of hope mixed with a twinge of uncertainty when the Centers for Disease Control and Prevention announced that a COVID-19 vaccine was finally available.
Was it going to work? Was it going to make my disease worse? So many questions were living rent-free in my brain.
I did so much research about the effects of the vaccine on people with IBD and initially found very little. I want to share my experience in the hope that it will help you make an educated decision on COVID-19 vaccination for yourself.
Eating Healthy Diet Will Surely Ease Flare
Eating healthy diet will absolutely ease flare-up of ulcerative colitis. Always confirm your diet is healthy and avoid consumption processed foods. Also, you must avoid sweet and spicy foods in your diet, as they cause irritation to your colon. Your diet ought to be composed of vegetables as a serious supply of super molecule. The vegetables ought to be recent and leafed inexperienced, as they are a decent supply of naphthoquinone. Naphthoquinone deficiency is associated to redness being severe. Additionally, avoid consumption beef however instead supply super molecule from chicken and turkey or baked fish. Beef causes stress in your colon.
Don’t Miss: How Do Stomach Ulcers Heal