Treatment What Treatment Will I Be Offered For My Leg Ulcer
If your wound isnt healing because of venous hypertension and there are no problems with the blood supply to your legs, then you should be offered compression therapy.
Compression therapy improves blood supply by applying pressure to the leg. This can be done by bandaging the lower leg or by wearing supportive socks, stockings or tights. Compression therapy is very effective at reducing swelling, improving blood flow in the veins and healing or preventing sores or ulcers.
There are lots of different types of compression therapy so ask your nurse to find something that is right for you.
Compression can be a little uncomfortable when you first start treatment but should not cause you any pain. Any discomfort should reduce as the swelling goes down. If you do experience discomfort, talk to your nurse or doctor about it and they will advise you on ways of alleviating this.
In addition to the compression, your nurse should also advise you on wound care and dressings to keep your wound healthy.
What Treatment Might I Be Offered
Compression therapy if your wound isnt healing because of venous hypertension and there are no problems with the arterial blood supply to your legs, then you should be offered compression therapy. Compression therapy usually works very effectively and helps wounds to heal fast. It is thus essential to find a compression regime that is comfortable, provides the level of support you need and works. If this is inconsistently used or applied, this must be dealt with so that healing is not delayed
Compression therapy improves blood supply by applying pressure to the leg. This can be done by bandaging the lower leg or by wearing supportive socks, stockings or tights. To begin with it can be a little uncomfortable when you first start treatment but should not cause you any pain it should feel supportive to your leg. Any discomfort should reduce as the swelling goes down. If you do experience discomfort, talk to your nurse or doctor about it and they will advise you on ways of alleviating this.
How To Prevent Leg Ulcers
A leg ulcer is a breakage of the skin, allowing air and bacteria access to the exposed underlying tissues. While many people will recover quickly from an injury which breaks the skin, an ulcer is usually symptomatic of an underlying problem it can be slow or difficult to heal and may produce a discharge.
There are a number of factors which can affect the risk of developing leg ulcers. There are two main types of leg ulcers venous are due to pressure caused by an underlying problem with the veins, arterial are due to weak unhealthy skin caused by a lack of oxygen and blood flow after an arterial blockage.
Recommended Reading: Wound Care Treatment For Diabetic Foot Ulcer
The Traditional Idea Of Treating Leg Ulcers With Dressings And Compression Heal Venous Leg Ulcers But Do Not Cure Them
Prof Mark Whiteley explained that dressings, or even fads such as Manuka honey or sugar, can be useful for skin wounds. Also, compression can be useful for venous leg ulcers. However, no dressing or compression can cure a venous leg ulcer permanent.
The reason for this is quite simple. As it is the hidden varicose veins that cause the venous leg ulcer, the ulcer cannot be cured until this underlying problem is fixed. No matter what is placed on the surface, the underlying problem remains. Hence the ulcer will recur when the dressings or bandages are removed.
What Is The Treatment For A Venous Leg Ulcer
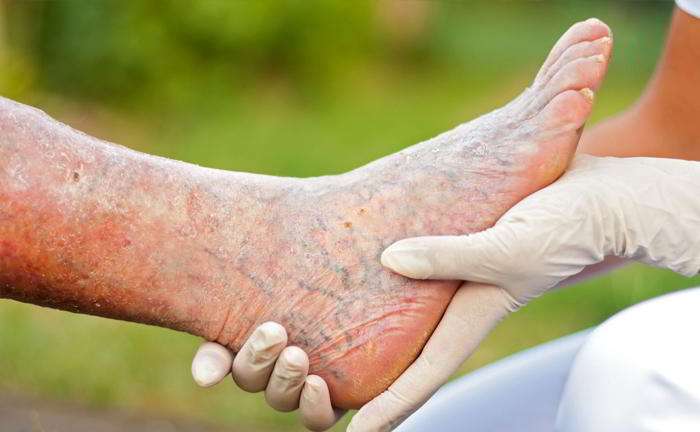
A venous leg ulcer usually wont get better without treatment from a healthcare professional. The aim of treatment is to make sure the wound heals while providing relief from symptoms such as pain in and swelling of your affected leg.
Your GP may recommend specialist wound care and compression therapy to help with healing. Treatment will usually be done by a district nurse who is specifically trained to manage leg ulcers.
Compression therapy applies pressure to your affected leg, which reduces the amount of blood pooling in the veins and helps to redirect the blood flow to your heart. It can help to reduce swelling and encourages delivery of oxygen and nutrients, critical for healing, to the wound.
Your GP may consider referral to a vascular surgeon to discuss a minimally invasive procedure for varicose veins. This will reduce the risk of recurrent ulcers.
Read Also: Can Ulcerative Proctitis Be Cured
Other Tips For Helping Leg Ulcers Heal Faster
In addition to always following the instructions provided for how to dress the wound and how to wear your compression bandage, there are other things you can do to help speed up the healing of your leg ulcer. Other things you can do include:
- Take any and all medication as prescribed for your leg ulcer
- Keep your leg elevated as much as possible. The leg should be elevated at a height that is level with your eyes.
- Stay active. Simply walking each day can help prevent the leg ulcer from getting worse and reduce the amount of swelling you experience in your legs.
- Learn stationary leg exercises that you can do throughout the day. Some examples of stationary leg exercises include rotating your ankles, moving your feet up and down, or wiggling your leg. These exercises will help to improve blood flow to your legs.
- Try to lose weight
- Seek treatment for any other health problems, such as diabetes or heart disease
- Make improvements to your diet
- Work to make lifestyle changes, such as not drinking too much alcohol and not smoking
- Avoid bumping or touching the wound as it could reinjure the area and slow down the healing process
- Follow through with all regularly scheduled appointments with your doctor and healthcare team
Signs And Causes Of Venous Ulcers
Venous ulcers are non-healing or slow-healing wounds that form as a result of blood pooling in the legs and feet. This happens when the walls or valves in the veins of the lower extremities dont work effectively. This is called venous insufficiency.
Venous ulcers are more common in women and older people. Several factors increase your risk of developing venous ulcers, including:
- Long periods of immobility, such as bed rest
- Older age
Recommended Reading: Is Ulcerative Colitis Considered An Autoimmune Disease
What Causes Leg Ulcers To Develop
Leg ulcers develop because there is an underlying health problem or issue that is causing your body to be unable to naturally heal the skin. These health problems cause a condition known as lymphedema, a buildup of fluid in the tissues, to develop. If the skin is unable to heal naturally due to the buildup of fluid, it can result in the further breakdown of the surrounding skin which will cause the wound to increase in size.
Healthcare providers know the following health problems can result in lymphedema caused leg ulcers:
- Arterial disease
- Venous disease
Diagnosis And Treatment Of Venous Ulcers
LAUREN COLLINS, MD, and SAMINA SERAJ, MD, Thomas Jefferson University Hospital, Philadelphia, Pennslyvania
Am Fam Physician. 2010 Apr 15 81:989-996.
Patient information: See related handout on venous ulcers, written by the authors of this article.
Venous ulcers, or stasis ulcers, account for 80 percent of lower extremity ulcerations.1 Less common etiologies for lower extremity ulcerations include arterial insufficiency prolonged pressure diabetic neuropathy and systemic illness such as rheumatoid arthritis, vasculitis, osteomyelitis, and skin malignancy.2 The overall prevalence of venous ulcers in the United States is approximately 1 percent.1 Venous ulcers are more common in women and older persons.36 The primary risk factors are older age, obesity, previous leg injuries, deep venous thrombosis, and phlebitis.7
Venous ulcers are often recurrent, and open ulcers can persist from weeks to many years.810 Severe complications include cellulitis, osteomyelitis, and malignant change.3 Although the overall prevalence is relatively low, the refractory nature of these ulcers increase the risk of morbidity and mortality, and have a significant impact on patient quality of life.11,12 The financial burden of venous ulcers is estimated to be $2 billion per year in the United States.13,14
You May Like: Psc Liver Disease Ulcerative Colitis
Cleveland Clinic Heart Vascular & Thoracic Institute Vascular Medicine Specialists And Surgeons
Choosing a doctor to treat your vascular disease depends on where you are in your diagnosis and treatment. The following Heart, Vascular & Thoracic Institute Sections and Departments treat patients with all types of vascular disease, including blood clotting disorders:
Section of Vascular Medicine: for evaluation, medical management or interventional procedures to treat vascular disease. In addition, the Non-Invasive Laboratory includes state-of-the art computerized imaging equipment to assist in diagnosing vascular disease, without added discomfort to the patient. Call Vascular Medicine Appointments, toll-free 800-223-2273, extension 44420 or request an appointment online.
Department of Vascular Surgery: surgery evaluation for surgical treatment of vascular disease, including aorta, peripheral artery, and venous disease. Call Vascular Surgery Appointments, toll-free 800-223-2273, extension 44508 or request an appointment online.
You may also use our MyConsult second opinion consultation using the Internet.
The Heart, Vascular & Thoracic Institute also has specialized centers and clinics to treat certain populations of patients:
Treating Venous Leg Ulcers With Honey The Trial
Leg ulcers are nasty sores. They are long-lasting and can take a month to six weeks to heal and much longer in some cases. They usually, though not always, develop, just above the ankle on the inside part of the leg. Honey definitely has some medical qualities that can help heal wounds and sores. Watch the video to find out more.
My Notes:
We have known about venous leg ulcers for centuries. They occur when there’s a breakdown in the skin tissue below the knee area. Ever since the 17th century, people have treated these sores by applying compression bandages. The compression helps the leg cope with the constant pressure of fluids in the lower parts of the body. This is what’s known as hydrostatic pressure. It refers to the pressure that any fluid in a confined space exerts.
The symptoms of a venous leg ulcer include:
- Pain
- Persistent itching
- Swelling in the affected leg
In recent times there has been a lot more interest in general for alternative medicines. Honey is fast becoming one of those keen areas of interest. You can read more all the time about how people are using honey as a potential healing agent. Some suggest that a honey dressing as well as a compression bandage can help with venous leg ulcers.
Read Also: Best Treatment For Diabetic Foot Ulcer
What Should I Do At My Appointment
Remember to remove any nail polish from your toenails before your appointment.
When you see the nurse or doctor, they should:
- Ask about your symptoms and how long you have had problems
- Examine your lower legs
- Do a simple test called a Doppler Ultrasound. This test compares blood flow in your ankle with that in your arm to find out if there are arterial blood flow problems in your lower leg. You may have to come back to have your Doppler test on another day or at another clinic.
- You may also be offered some other tests to check for other health problems that can affect your legs such as diabetes and anaemia.
You may hear different words to describe your wound such as ulcer, leg ulcer, sore, laceration, chronic wound and maybe others. Ask your nurse to explain their choice of word and what this may mean for you.
Early Treatment For Leg Ulcers Leads To Better Outcomes For Patients
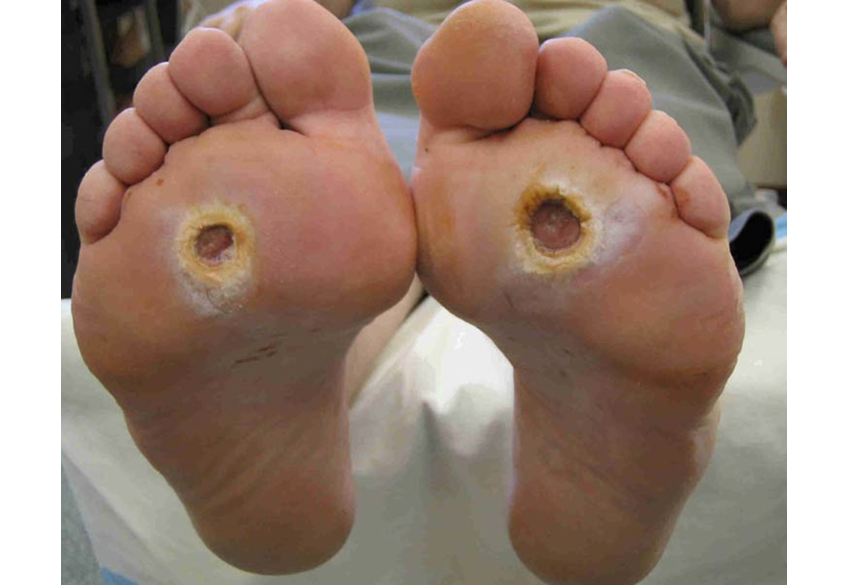
by Maxine Myers23 September 2020
Early surgical treatment of leg ulcers caused by varicose veins improves healing and reduces the risk of the condition coming back.
Venous leg ulcers are common and distressing, affecting around 1 in 300 adults in the UK. They are open, often painful, sores on the leg that take months to heal and can develop after a minor injury. People with enlarged veins known as varicose veins are at high risk of developing venous leg ulcers, as they have persistently high pressure in the veins leading to skin damage.
In a clinical trial, led by researchers at Imperial College London and clinicians at Imperial College Healthcare NHS Trust, 450 patients with venous leg ulcers were treated with early surgical interventions. This resulted in faster healing and a reduced risk of the condition coming back compared with current methods of treating patients with compression stockings and delayed surgical interventions.
The researchers behind the study, published in JAMA Surgery, suggest that current guidelines on treating leg ulcers should be revised to include early assessment of varicose veins and surgical treatment of leg ulcers to deliver clinical benefits and cost savings for the NHS. They suggest that this early treatment intervention could save the NHS an estimated £100 million per year.
The study was funded by NIHR Imperial College Biomedical Centre .
Recommended Reading: What Is A Gastric Ulcer And What Is Its Cause
Referral To A Specialist
In some cases, your GP or nurse may decide to refer you to a specialist in conditions affecting the blood vessels .
For example, you may be referred to a vascular specialist if your GP or nurse is unsure about your diagnosis, or if they suspect your ulcer may be caused by artery diseases, diabetes or rheumatoid arthritis.
After taking your medical history and examining you, the vascular specialist may need to arrange further investigations to plan your treatment.
What Is A Venous Skin Ulcer
A skin ulcer is a type of wound that develops on the skin. A venous skin ulcer is a shallow wound that occurs when the leg veins don’t return blood back toward the heart the way they should. This is called venous insufficiency.
These ulcers usually form on the sides of the lower leg, above the ankle and below the calf.
Venous skin ulcers are slow to heal and often come back if you don’t take steps to prevent them.
A venous skin ulcer is also called a stasis leg ulcer.
Read Also: Ulcerated Nodular Basal Cell Carcinoma
Healthcare Advice For Leg Ulcers
There are some lifestyle changes you can make that will help boost healing:
- Maintain a healthy weight
- Eat a well-balanced diet that includes 5 portions of fruit and vegetables a day and protein rich foods such as eggs, fish, chicken or pulses
- Take light to moderate exercise such as cycling or walking for about thirty minutes at least three times a week
- Avoid standing or sitting for long periods of time
- Put your feet up elevate your legs above your heart.
- Every so often, move your feet around in circles, then up and down. This helps blood circulate and get back to your heart
What Causes Diabetic Wounds
- Elevated blood glucose: When blood sugars reach levels higher than 200 the immune system lowers. This can contribute to the formation of wounds. A small cut that may normally heal without problems may actually become a larger, deeper ulcer due to the dysfunction of the immune system.
- Poor circulation: A common problem in patients with diabetes, is poor circulation. Elevated sugars in the blood can damage the small blood vessels, especially the ones to the foot and toes. When your foot or toes are lacking enough blood, they do not receive proper nutrients. The skin can begin to break down and an ulcer can form. This is similar to a plant that is not receiving proper water- the ends become brown, crisp and dry out.
- Neuropathy: Another common condition that can lead to diabetic ulcers, is neuropathy. Neuropathy is a loss of sensation or feeling, typically in the toes and the feet. You may step on something sharp and not feel it. This can result in a small cut that later becomes a deep wound. If you put a lot of pressure in the same place on your foot, daily, this can also result in a special type of ulcer called a pressure ulcer.
HOW CAN I PREVENT GETTING A DIABETIC WOUND?
HOW CAN I HEAL MY WOUND FASTER?
Read Also: Stage 2 Pressure Ulcer Treatment Dressing
Does Cleaning Venous Leg Ulcers Help Them To Heal
Background
Leg ulcers are open skin wounds that develop below the knee, usually because blood flow is poor in the lower leg. This can occur because of blockages, for example when small blood clots form in the veins. It can also happen when the valves in the veins that prevent blood from flowing backwards stop working properly. Poor blood flow damages the skin and tissue, and creates venous leg ulcers.
Ulcers are unsightly and may become painful or infected. On average, ulcers take from six to nine months to heal. However, some ulcers can take years to heal, and a small number never do. Once ulcers have healed, they can reoccur.
The main treatment for venous leg ulcers is to use bandages or stockings that compress the leg , to increase blood flow in the veins. It is also thought to be important to clean the wound. Different types of cleaning solutions can be used, including: normal saline water antiseptics detergents or disinfectants .
Cleaning solutions can be applied to the ulcer using a swab , a syringe with a needle, or a spray canister. Ulcers can also be bathed in the cleaning solution, using a basin or bucket, or during a shower. Cleaning can cause discomfort, and may be painful.
What did we want to find out?
We wanted to find out:
– whether cleaning venous leg ulcers helps them to become smaller and heal
– whether some cleaning solutions, or methods of applying solutions, are more effective than others
– how much cleaning wounds costs and
Our methods
How Can Ulcers Be Prevented
Controlling risk factors can help you prevent ulcers from developing or getting worse. Here are some ways to reduce your risk factors:
- Quit smoking
- Manage your blood pressure
- Control your blood cholesterol and triglyceride levels by making dietary changes and taking medications as prescribed
- Limit your intake of sodium
- Manage your diabetes and other health conditions, if applicable
- Exercise â start a walking program after speaking with your doctor
- Lose weight if you are overweight
- Ask your doctor about aspirin therapy to prevent blood clots
Recommended Reading: Pressure Ulcer Prevention Care Plan