Are Leg Ulcers Serious
A venous skin ulcer is a sore on your leg thats very slow to heal, usually because of weak blood circulation in the limb. They can last anywhere from a few weeks to years. You may hear a doctor or nurse call them venous leg ulcers. They can sometimes lead to more serious problems if you dont have them treated.
What Are Leg Ulcers And How Are They Treated
Leg ulcers are open, non-healing wounds of the legs. They are usually on the lower legs or the feet. They can be thought of as open sores.
Ulcers can be painful or not painful. They can be big or small, wet or dry, smelly or not smelly. Leg ulcers can have many different appearances. Therefore, it can be very confusing if they are only assessed by their appearance. Many nurses and dermatologists use the surface appearance as part of their assessment often leading to incorrect diagnosis and sub-optimal care .
There is little information that can be gleaned just by looking at the ulcer. However, a rare skin cancer called a can be noted by seeing a rolled edge. So although not the most important part of the assessment nowadays, it is still essential to have a look at the ulcer itself.
As stated above, there is very little that can be found just from looking at a leg ulcer in the majority of cases. Unquestionably, it is impossible to tell if a leg ulcer is curable or incurable just from looking at the surface alone.
How Venous Leg Ulcers Are Treated
Most venous leg ulcers heal within 3 to 4 months if they’re treated by a healthcare professional trained in compression therapy for leg ulcers.
But some ulcers may take longer to heal, and a very small number never heal.
Treatment usually involves:
- cleaning and dressing the wound
- using compression, such as bandages or stockings, to improve the flow of blood in the legs
Antibiotics may also be used if the ulcer becomes infected, but they do not help ulcers heal.
But unless the underlying cause of the ulcer is addressed, there’s a high risk of a venous leg ulcer coming back after treatment.
Underlying causes could include immobility, obesity, previous DVT or varicose veins.
Recommended Reading: Food To Avoid For Ulcer Patient
Other Types Of Leg Ulcer
Other common types of leg ulcer include:
- arterial leg ulcers caused by poor blood circulation in the arteries
- diabetic leg ulcers caused by the high blood sugar associated with diabetes
- vasculitic leg ulcers associated with chronic inflammatory disorders such as rheumatoid arthritis and lupus
- traumatic leg ulcers caused by injury to the leg
- malignant leg ulcers caused by a tumour of the skin of the leg
Most ulcers caused by artery disease or diabetes occur on the foot rather than the leg.
Page last reviewed: 11 January 2019 Next review due: 11 January 2022
Why Might A Wound On The Leg Not Heal And Turn Into A Leg Ulcer
This is because the wound is on the leg and is much more difficult to heal than wounds on another part of the body. We spend a lot of time on our feet and if we have any swelling, this will interfere with healing. If you stand a great deal, or you are carrying excessive weight, this will not help your circulation. Any wound, except those caused by arterial disease will benefit from some form of compression therapy
Also Check: Worst Foods For Stomach Ulcers
Can Venous Leg Ulcers Be Prevented
There are several ways to help prevent developing a venous leg ulcer in people at risk.
These include:
- elevating your leg when possible
- stopping smoking if you smoke
These measures are particularly important if you previously had a leg ulcer.
This is because you’re at increased risk of having another one in the same leg within months or years.
What Does A Venous Leg Ulcer Look Like And What Causes Them
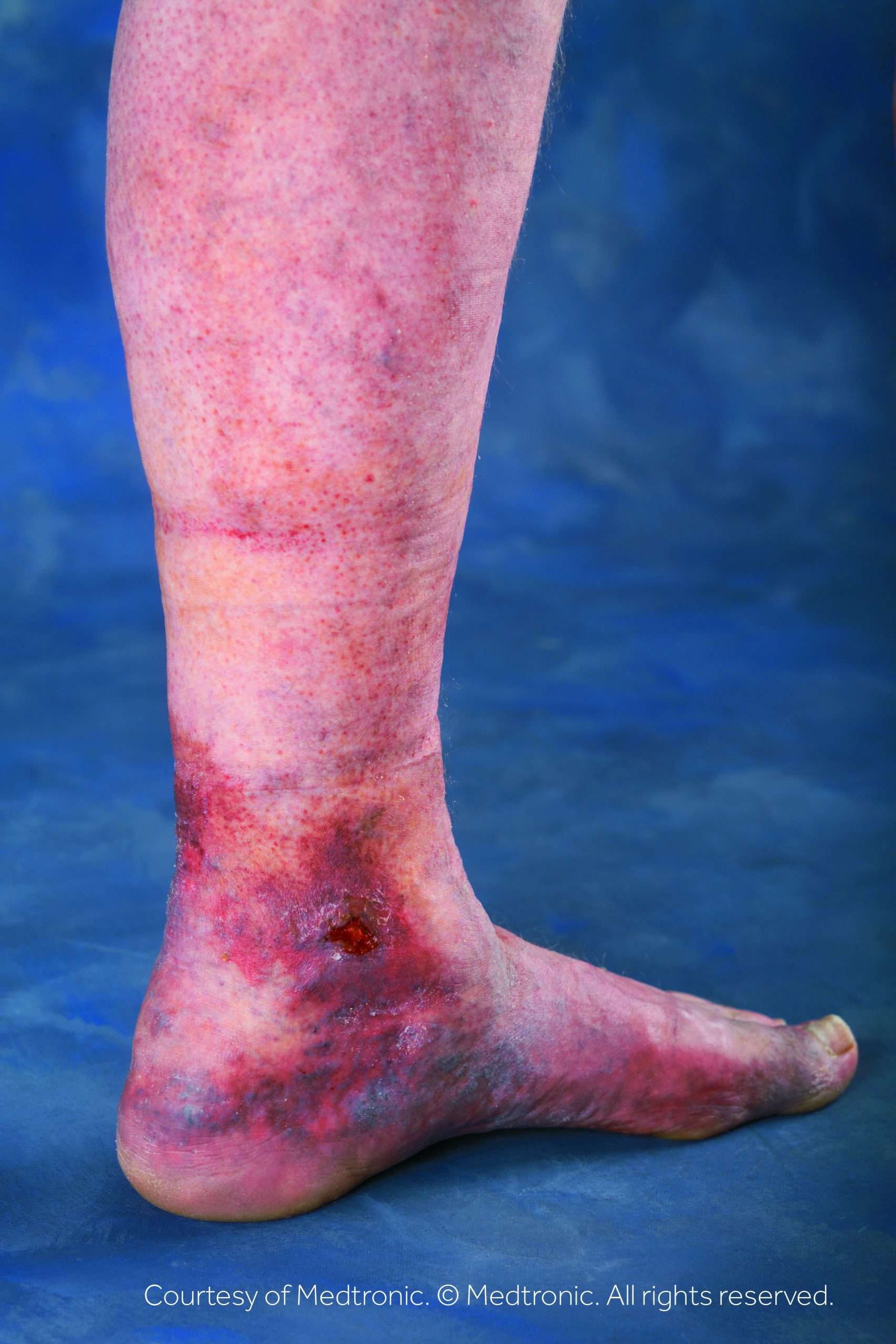
Venous leg ulcers are sores that develop between your knee and ankle, but they typically form inside the leg near or around the ankle. They are large, shallow ulcers with uneven edges that drain or weep a lot.
Youll likely see swelling in your leg, with red, itchy skin around the wound. You may also experience tightness in your calves, as well as aching, throbbing or a feeling of heaviness in your legs. Pooled and trapped blood often causes discolored splotches in the area.
The sores sometimes affect only the skin or they may sink deeper into the fat layer, muscle, tendon and bone, she says. Severe ulcers are more likely to become infected and take longer to heal.
Your veins carry blood back to your heart, and valves in the veins stop the blood from flowing backward. When your veins have trouble sending blood from your limbs to the heart, its known as venous insufficiency. In this condition, blood doesnt flow back properly to the heart, causing blood to pool in the veins in your legs.
Our veins are just like pipes, says Ehren. When theres persistently high blood pressure in the veins of the legs with a valve that doesnt work correctly, it causes damage to the skin, which eventually breaks down and forms an ulcer.
Other possible causes for venous leg ulcers include:
- Varicose veins.
- Cancer.
- Swelling of a superficial vein .
Don’t Miss: Signs Of Having An Ulcer
How Do You Stop A Leg Ulcer From Weeping
To help treat a venous ulcer, the high pressure in the leg veins needs to be relieved.
Infection Of Venous Leg Ulcers
The most common complication of venous leg ulcers is infection, which can arise from a variety of sources, including the following:1
- Bacterial: furuncles, ecthyma, mycobacterioses, syphilis, erysipelas, anthrax, diphtheria, chronic vegetative pyoderma, tropical ulcer
- Viral: herpes, variola virus infection, cytomegalovirus infection
- Fungal: sporotrichosis, histoplasmosis, blastomycosis, coccidioidomycosis
- Protozoal: leishmaniasis
When infection is present in the VLU, the patient may present with fever, wound fluid rich in leukocytes, increasing pain, cellulitis, necrotic tissue, and purulent exudate with or without odor. When signs of infection are present, the patient should be treated with appropriate systemic antibiotics, topical antimicrobials, or antiseptics.2 However, VLUs that are critically colonized with bacteria or bacterial biofilms without signs of systemic infection may be treated in multiple ways, including topical antibiotics. Sequential, aggressive debridement can also be used to treat infected ulcers.1
Don’t Miss: Indian Diet For Ulcerative Colitis
What Is The Fastest Way To Heal A Leg Ulcer
The following advice may help your ulcer heal more quickly.
Can Leg Ulcers Be Prevented
To prevent and promote healing of ulcers:
- Avoid injury, particularly when pushing a supermarket trolley. Consider protective shin splints.
- Walk and exercise for at least an hour a day to keep the calf muscle pump working properly.
- Lose weight if you are overweight.
- Stop smoking.
- Check your feet and legs regularly. Look for cracks, sores or changes in colour. Moisturise after bathing.
- Wear comfortable well-fitting shoes and socks. Avoid socks with a tight garter or cuff. Check the inside of shoes for small stones or rough patches before you put them on.
- If you have to stand for more than a few minutes, try to vary your stance as much as possible.
- When sitting, wriggle your toes, move your feet up and down and take frequent walks.
- Avoid sitting with your legs crossed. Put your feet up on a padded stool to reduce swelling.
- Avoid extremes of temperature such as hot baths or sitting close to a heater. Keep cold feet warm with socks and slippers.
- Consult a chiropodist or podiatrist to remove a callus or hard skin.
- Wear at least Grade 2 support stockings if your doctor has advised these. This is particularly important for the post-thrombotic syndrome, leg swelling or discomfort, and for long-distance flights.
- Have a vascular ultrasound assessment and consult a vascular surgeon to determine whether any vein treatment should be carried out.
- Horse chestnut extract appears to be of benefit for at least some patients with venous disease.
Also Check: What Foods Should You Eat If You Have An Ulcer
Definition Of Leg Ulcer
The word ulcer means a break in the layer of cells forming a surface. This is called the epithelial layer and epithelial cells line any outside surface of the body.
Hence ulcers can occur in many different areas of the body. Ulcers cause different problems depending on what surface they are breaking up. For example, a stomach ulcer is a break in the cells forming the lining of the stomach. This allows gastric acid to attack the underlying tissue. This can result in pain, bleeding or even perforation. A more common ulcer is a mouth ulcer. Most of us will have had one at some time. This is a break in the mucosal cells lining the inner surface of the cheeks. It allows saliva to get the underlying tissue and causes severe pain.
In the case of leg ulcers, the skin breaks down and this allows air and bacteria to get into the tissue below. When an ulcer occurs on the leg, it is tempting to cover it up, hoping the skin will grow back. This is why humans, throughout history, have put dressings over leg ulcers, hiding them away and hoping they will heal.
However, such simple actions miss out one major point. By covering the ulcer, the person doing the covering is not thinking about why the ulcer occurred in the first place.
What Can Cause Leg Ulcers
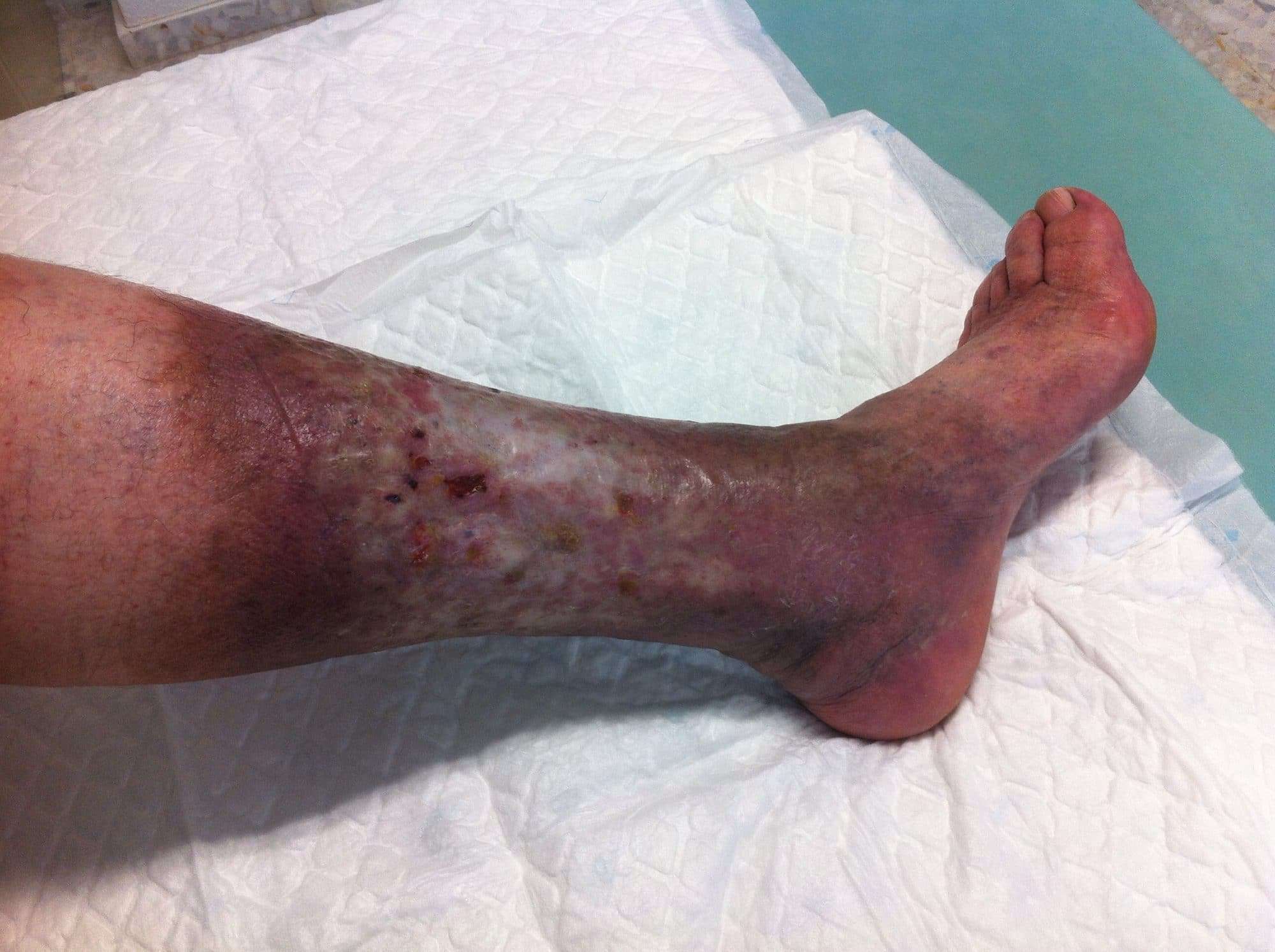
Venous hypertension / insufficiency the most common cause of poor healing on the lower leg is venous hypertension. This is when the veins struggle to take the blood back up the leg, so the blood can pool at the ankle creating pressure in your veins
Peripheral arterial disease another reason why our lower leg wound might not be healing is because not enough blood is getting down to our feet to heal the wound. This is then the opposite of the problem described above with veins.
Diabetes peripheral arterial disease is a known complication of diabetes, which can lead to developing a leg ulcer or diabetic foot ulcer.
Don’t Miss: What To Eat With An Ulcerative Colitis Flare Up
What Is The Home Remedy For Leg Ulcer
At-home remedies
When Is Surgery Needed
Sometimes, more serious cases of venous insufficiency require surgery. Your doctor may suggest one of the following:
- Surgically repairing veins or valves.
- Removing the damaged vein.
- Minimally invasive endoscopic surgery .
- Vein bypass .
- Laser surgery .
Surgical procedures include:
Also Check: Aip Diet For Ulcerative Colitis
What Are The Symptoms Of A Venous Leg Ulcer
The most common symptom of a venous leg ulcer is a wound that doesnt heal and is irregularly shaped with dry, hard skin around the outside. Other symptoms include:
- swelling, especially around the ankle of your affected leg
- aching legs
- pain
- clear discharge.
Venous leg ulcers are at risk of becoming infected because theyre slow to heal. Signs of an infected leg ulcer include:
- increased pain
- an increase in swelling and redness around the wound.
Referral To A Specialist
In some cases, your GP or nurse may decide to refer you to a specialist in conditions affecting the blood vessels .
For example, you may be referred to a vascular specialist if your GP or nurse is unsure about your diagnosis, or if they suspect your ulcer may be caused by artery diseases, diabetes or rheumatoid arthritis.
After taking your medical history and examining you, the vascular specialist may need to arrange further investigations to plan your treatment.
Read Also: How To Know You Have A Ulcer
Caring For Venous Ulcers
Venous ulcers need proper care and treatment to prevent infection and to heal. It’s important to have any venous ulcers checked right away by your healthcare provider.
Treatment may require focusing on the circulatory or vein problems that are causing the ulcers. Or it may mean removing some tissue around the wound. You may be asked to:
-
Clean the wound regularly
-
Apply a dressing to the ulcer
-
Avoid products that cause skin sensitivity
-
Wear compression stockings to prevent blood from pooling in the legs and to speed healing
-
Apply an antibacterial ointment or another topical medicine to prevent or treat an infection
-
Take oral antibiotic medicines to prevent or treat an infection
-
Have allergy testing done
Wearing a compression wrap to keep blood flowing back up to your heart can also help ulcers heal more quickly. In some cases, surgery or a skin graft is needed to close up the opening in the skin.
Chronic Leg Ulcers: Epidemiology Aetiopathogenesis And Management
Shubhangi Vinayak Agale
1Department of Pathology, Grant Govt Medical College, Byculla, Mumbai 400008, India
Academic Editor:
Abstract
Chronic leg ulcer is defined as a defect in the skin below the level of knee persisting for more than six weeks and shows no tendency to heal after three or more months. Chronic ulceration of the lower legs is a relatively common condition amongst adults, one that causes pain and social distress. The condition affects 1% of the adult population and 3.6% of people older than 65 years. Leg ulcers are debilitating and greatly reduce patients’ quality of life. The common causes are venous disease, arterial disease, and neuropathy. Less common causes are metabolic disorders, hematological disorders, and infective diseases. As many factors lead to chronic lower leg ulceration, an interdisciplinary approach to the systematic assessment of the patient is required, in order to ascertain the pathogenesis, definitive diagnosis, and optimal treatment. A correct diagnosis is essential to avoid inappropriate treatment that may cause deterioration of the wound, delay wound healing, or harm the patient. The researchers are inventing newer modalities of treatments for patients with chronic leg ulceration, so that they can have better quality life and reduction in personal financial burden.
1. Introduction
2. Epidemiology
3. Aetiopathogenesis
| Vascular |
4. Pathogenesis of Chronic Leg Ulcers
4.1. Venous Ulcers
4.2. Arterial Ulcers
4.3. Diabetic Foot Ulcer
You May Like: Can Stress Give You An Ulcer
How Diabetes Causes Ulcers
Diabetes typically causes ulcers on your foot. But diabetes also increases your risk of developing atherosclerosis, so you may end up with a leg ulcer, too.
High blood sugar damages small blood vessels and nerves. Nerve damage causes numbness, so you dont notice small cuts, scrapes, and pressure sores on your foot. Then diminished blood flow hinders healing, turning a minor cut into a nonhealing ulcer.
The best way to prevent a diabetic ulcer is to check your feet every day, looking for signs of a cut or abrasion. If you notice a problem, get medical care right away to ensure the wound heals.
If you have questions about leg ulcers or symptoms you may have, contact us today at our Memphis, Tennessee, office.
You Might Also Enjoy…
Venous Hypertension / Insufficiency
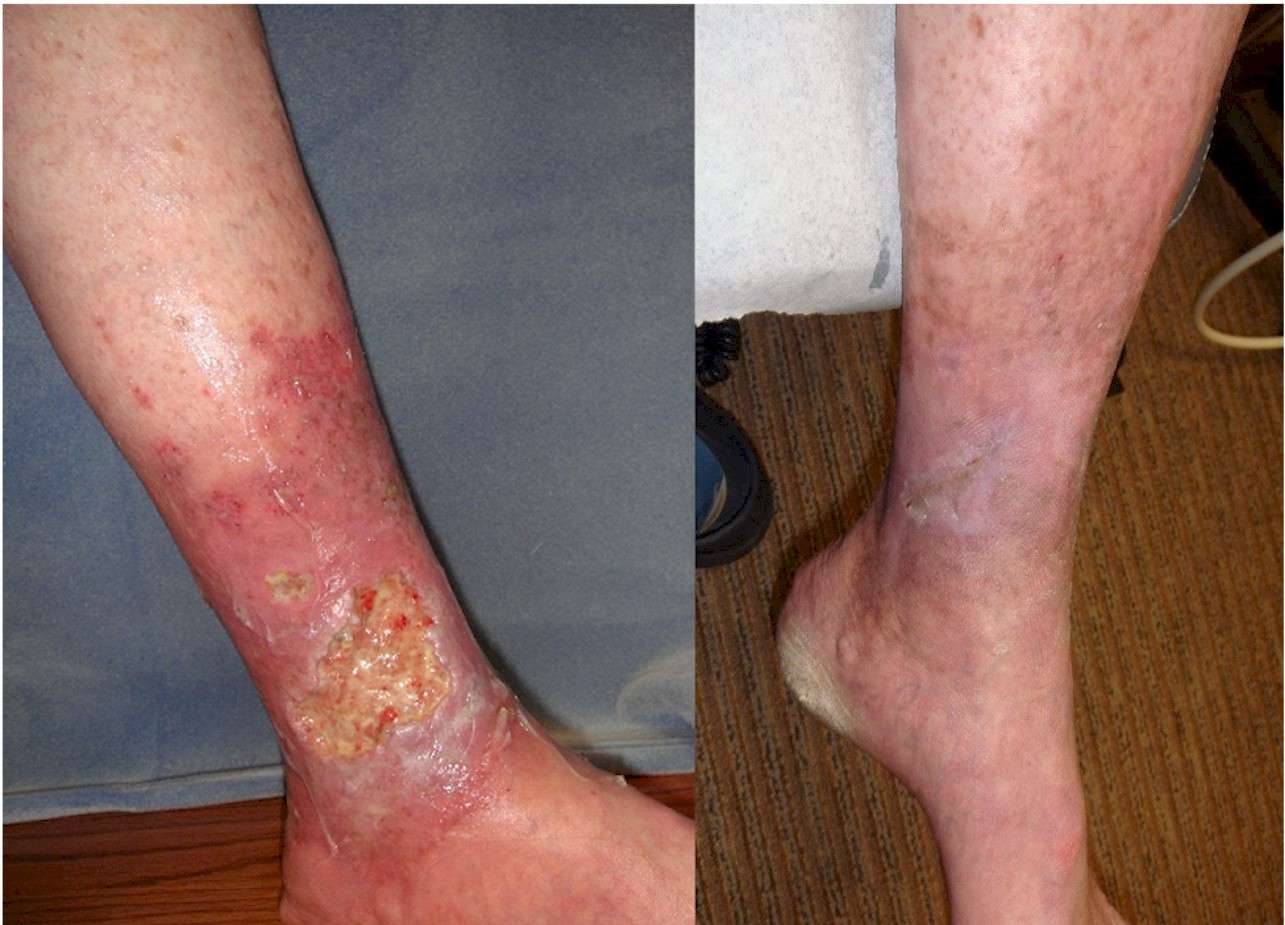
The most common cause of poor healing on the lower leg is venous hypertension. You may also hear it referred to as venous insufficiency, venous reflux or venous disease. Venous means anything related to our veins. Blood is pumped from our heart to the rest of our body through our arteries and returns to our heart through our veins. It is then propelled back to our heart by our heart pumping. Our leg and foot muscles help this along by circulating blood as we walk and move our ankles. This is why standing a lot or sitting with our legs down for long periods may stop a wound from healing.
Our veins contain one-way valves to stop the blood falling back towards your feet. These valves can become weak or damaged. When this happens, our veins become so swollen that blood is forced into the tissue of your skin. This makes our skin swollen, fragile and unable to heal as normal.
You might also notice that your ankles are swollen, that there is brown staining on your legs or that your wound is leaking.
To help our veins work better and to control any swelling, compression therapy is an essential part of any treatment plan.
Don’t Miss: How To Gain Weight With Ulcerative Colitis
Treatment What Treatment Will I Be Offered For My Leg Ulcer
If your wound isnt healing because of venous hypertension and there are no problems with the blood supply to your legs, then you should be offered compression therapy.
Compression therapy improves blood supply by applying pressure to the leg. This can be done by bandaging the lower leg or by wearing supportive socks, stockings or tights. Compression therapy is very effective at reducing swelling, improving blood flow in the veins and healing or preventing sores or ulcers.
There are lots of different types of compression therapy so ask your nurse to find something that is right for you.
Compression can be a little uncomfortable when you first start treatment but should not cause you any pain. Any discomfort should reduce as the swelling goes down. If you do experience discomfort, talk to your nurse or doctor about it and they will advise you on ways of alleviating this.
In addition to the compression, your nurse should also advise you on wound care and dressings to keep your wound healthy.