Peptic Ulcers: Is Stress A Culprit
Contrary to popular belief, most ulcers do not actually result from stress or eating too many spicy foods.
In 2005, Drs. Barry Marshal and Robin Warren, from Australia, received the Nobel Prize in Medicine for discovering that a spiral-shaped bacterium that can colonize the human stomach is the offending cause in many cases.
Smoking tobacco, and drinking alcohol, may worsen ulcers, and as little as one baby aspirin daily can cause an ulcer.
What Treatments Heal Rectal Ulcers Without Surgery
To relieve symptoms of a rectal ulcer and help it heal, you should:
- Drink plenty of water: Dehydration can make stool hard, dry and more difficult to pass.
- Eat a healthy diet: Fiber-rich foods can relieve constipation. Fiber softens stool and helps it pass through your intestines faster.
- Avoid straining: Straining or pushing too hard when defecating can cause rectal ulcers. Your doctor or physical therapist can show you how to control the muscles in your anus so you can have a bowel movement without damaging your anus or rectum.
- Ask your doctor about laxatives: Your doctor may recommend taking a stool softener or laxative. These medications can relieve constipation by making your stool easier to pass. Talk to your doctor about which laxative you should take and how long you should take it.
- Try a topical medication: A corticosteroid cream or suppository can reduce inflammation, relieve pain and help the ulcers heal. Talk to your doctor about how to use this medication.
- Take antibiotics: If an STD or STI is causing rectal ulcers, your doctor will prescribe medicine to treat the infection.
If you have an inflammatory bowel disease such as ulcerative colitis, your doctor will recommend a treatment plan. Your plan may include a combination of prescription anti-inflammatory drugs, immunosuppressant drugs and dietary changes.
What Is Inflammatory Bowel Disease
Inflammatory bowel disease causes parts of the intestine to get red and swollen . It’s a chronic problem, which means it lasts a long time or constantly comes and goes.
There are two kinds of IBD: Crohn’s disease and ulcerative colitis. These diseases have many things in common, but there are important differences:
- Crohn’s disease can happen in any part of the gastrointestinal tract from mouth to anus . Crohn’s disease damages the entire bowel wall.
- Ulcerative colitis happens only in the large intestine, also called the colon. It causes sores called ulcers on the inner lining of the colon.
What Are the Signs & Symptoms of Inflammatory Bowel Disease?
The most common symptoms of IBD are belly pain and diarrhea. Other symptoms include:
- blood in the toilet, on toilet paper, or in the poop
- fever
- weight loss
When symptoms happen, its called a flare-up.
IBD can make it hard for someone to get all the calories and nutrition they need. Some kids and teens may grow slowly or start puberty later than usual. It can cause other problems, such as rashes, eye problems, joint pain and arthritis, and liver problems.
Also Check: Best Mattress For Pressure Ulcers
How Are Rectal Ulcers Diagnosed
Your doctor will examine you and ask about habits that may have caused your symptoms . To check for rectal ulcers, doctors use physical examination, tests and imaging studies. These tests include:
- Anoscopy: Your doctor may use a tool called an anoscope to examine you. An anoscope is a short tube that your doctor inserts into your anus. Your doctor uses a light to see through the tube and check for ulcers or lesions inside your rectum.
- Sigmoidoscopy: Doctors insert a flexible instrument into your rectum during a sigmoidoscopy. The thin device has a camera on the end. With it, your doctor can see inside your rectum and the lower part of the colon.
- Colonoscopy: To look at the entire colon, doctors insert a long scope with a camera. Like a sigmoidoscopy, a colonoscopy is an outpatient procedure . It is a more invasive test than a sigmoidoscopy.
- Rectal ultrasound: During this test, doctors insert a small probe in your rectum. The probe uses sound waves to show images of the inside of the rectum so your doctor can see ulcers and other growths.
- Biopsy: Your doctor may take a biopsy of the tissue surrounding the ulcer and send it to a lab. The lab tests the tissue for other conditions, such as cancer.
Is It Important To Treat A Flare Early Or Is It Ok To Wait A Bit

Inflammation typically does not resolve without treatment and early intervention has a better outcome than waiting to treat. At an early stage of a flare, a more optimal baseline treatment is often enough to get the inflammation under control. If you wait, there is a greater risk that you might need drugs with greater side effects, such as oral steroids. By waiting, you will have to manage longer with your symptoms before getting relief. Living with constant or longer periods of inflammation might increase your risk for future complications, as inflammation might cause damage to the gut wall that accumulates in severity with each flare.
If you are experiencing worsening symptoms, you have probably already had the flare for some time without symptoms. Evidence shows that a stool test for inflammation in the colon, called fecal calprotectin, is often elevated for two to three months before any symptoms appear. Your colon might also start to show visual evidence of inflammation before you have symptoms, or at least indicate an increased risk for a flare.
Read Also: Best Pain Relief For Leg Ulcers
Mri Scans And Mr Enterography
An MRI scan uses a magnetic field and radio waves to create two- and three-dimensional images of the body. MRI scans are especially helpful when doctors need to visualize soft tissues, such as the lining of the intestines. They may reveal small tears or ulcers, as well as irritation or bleeding.
To get a better look at the gastrointestinal tract, the doctor may ask you to drink a contrast agent just before the MRI. This is called MR enterography.
What Causes Crohns Disease
The cause of the chronic inflammation in Crohns disease is unknown. The leading theory is that inflammation is initiated by bacteria that reside within the intestine. Whereas most inflammation usually is suppressed, and the disease caused by the inflammation subsides, in Crohns disease the inflammation is not suppressed, and the inflammation continues. The continuing inflammation probably occurs because of environmental factors as well as genetic factors that affect the immune system. Crohns sometimes runs in families, too. Having a parent or sibling with the disease raises your own risk.
Recommended Reading: How Do You Check For A Stomach Ulcer
Can I Get Surgery For My Ulcerative Colitis
Surgery is an option if medications arent working or you have complications, such as bleeding or abnormal growths. You might develop precancerous lesions, or growths that can turn into colorectal cancer. A doctor can remove these lesions with surgery or during a colonoscopy.
Research shows that about 30% of people with ulcerative colitis need surgery sometime during their life. About 20% of children with ulcerative colitis will need surgery during their childhood years.
There are two kinds of surgery for ulcerative colitis:
Proctocolectomy and ileoanal pouch
The proctocolectomy and ileoanal pouch is the most common procedure for ulcerative colitis. This procedure typically requires more than one surgery, and there are several ways to do it. First, your surgeon does a proctocolectomy a procedure that removes your colon and rectum. Then the surgeon forms an ileoanal pouch to create a new rectum. While your body and newly made pouch is healing, your surgeon may perform a temporary ileostomy at the same time. This creates an opening in your lower belly. Your small intestines attach to the stoma, which looks like a small piece of pink skin on your belly.
After you heal, waste from your small intestines comes out through the stoma and into an attached bag called an ostomy bag. The small bag lies flat on the outside of your body, below your beltline. Youll need to wear the bag at all times to collect waste. Youll have to change the bag frequently throughout the day.
When To Call The Doctor
- Cramps or pain in your lower stomach area
- Bloody diarrhea, often with mucus or pus
- Diarrhea that cannot be controlled with diet changes and drugs
- Rectal bleeding, drainage, or sores
- Fever that lasts more than 2 or 3 days, or a fever higher than 100.4°F without an explanation
- Nausea and vomiting that lasts more than a day
- Skin sores or lesions that do not heal
- Joint pain that keeps you from doing your everyday activities
- A feeling of having little warning before you need to have a bowel movement
- A need to wake up from sleeping to have a bowel movement
- Failure to gain weight, a concern for a growing infant or child
- Side effects from any drugs prescribed for your condition
Recommended Reading: Can Diverticulitis Cause Ulcerative Colitis
What Are Rectal Ulcers
A rectal ulcer is a painful sore that develops inside the rectum. The rectum is a tube connecting the colon to the anal opening . Stool passes through the rectum and anus when it leaves the body.
These ulcers are related to several different conditions. People who have a condition called solitary rectal ulcer syndrome can develop rectal ulcers. Inflammatory bowel disease , including ulcerative colitis and Crohns disease, may also cause ulcers to form in the rectum and intestines. Constipation and straining during a bowel movement can cause rectal ulcers to develop as well.
Signs of a rectal ulcer may include:
- Blood in the stool.
- Painful Bowel movements.
What Are The Signs & Symptoms Of Ulcerative Colitis
The most common symptoms of ulcerative colitis are cramping belly pain and diarrhea. Other symptoms include:
- blood in the toilet, on toilet paper, or in the stool
- urgent need to poop
- low energy
- weight loss
Ulcerative coliits can cause other problems, such as rashes, eye problems, joint pain and arthritis, and liver disease. Kids with ulcerative colitis may not grow well as well as other kids their age and puberty may happen later than normal.
Read Also: Classic Features Of Ulcerative Colitis
How Do H Pylori Cause A Peptic Ulcer And Peptic Ulcer Disease
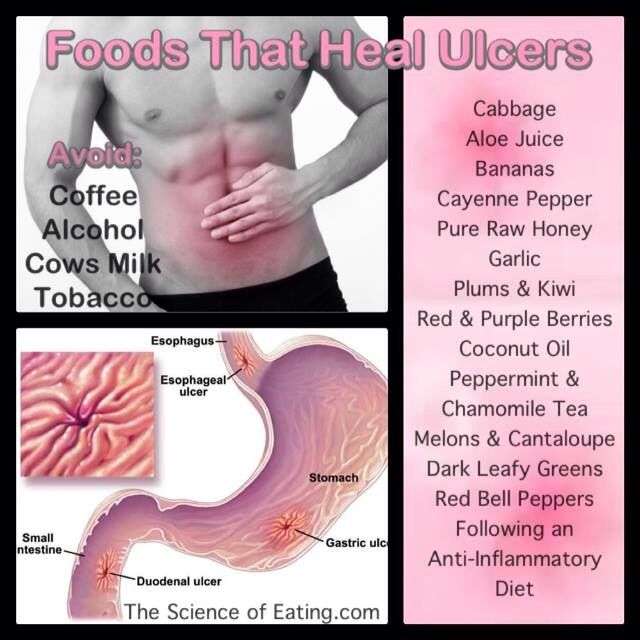
H. pylori are spiral-shaped bacteria that can cause peptic ulcer disease by damaging the mucous coating that protects the lining of the stomach and duodenum. Once H. pylori have damaged the mucous coating, powerful stomach acid can get through to the sensitive lining. Together, the stomach acid and H. pylori irritate the lining of the stomach or duodenum and cause a peptic ulcer.
In My Shoes: 24 Hours With Crohns Or Colitis App
In My Shoes is an immersive experience that allows anyone to find out first-hand what its like to have Colitis.
From low energy levels to managing pain, from rushing to the toilet to juggling work and a social life, the app will allow friends, family and anyone you want, to see first-hand how the condition can affect every part of your body, and every aspect of your life.
We have information for friends and family, employers, and colleagues. Find all our information online.
We have around 50 Local Networks across the UK that bring local people affected by Crohns and Colitis together. They are run by volunteers and host a range of events, from educational talks to socials. Check our website or call our Helpline to find your nearest Local Network.
Also Check: What Does A Foot Ulcer Look Like
What Are The Symptoms Of A Peptic Ulcer
A dull or burning pain in your stomach is the most common symptom of a peptic ulcer. You may feel the pain anywhere between your belly button and breastbone. The pain most often
- happens when your stomach is emptysuch as between meals or during the night
- stops briefly if you eat or if you take antacids
- lasts for minutes to hours
- comes and goes for several days, weeks, or months
Less common symptoms may include
- bloating
- feeling sick to your stomach
- poor appetite
- vomiting
- weight loss
Even if your symptoms are mild, you may have a peptic ulcer. You should see your doctor to talk about your symptoms. Without treatment, your peptic ulcer can get worse.
What Should I Ask My Doctor On Behalf Of My Child Or Teenager
Ask your healthcare provider the following questions in addition to the ones listed above:
- What vitamins should my child take?
- Will my other children have pediatric ulcerative colitis?
- Is my child at risk for other conditions?
- Can you recommend a psychiatrist or therapist to help my child with emotional issues related to pediatric ulcerative colitis?
- Is my child growing at a normal rate?
- What can I do to help my child cope at school?
A note from Cleveland Clinic
When you have ulcerative colitis, its essential to work closely with your healthcare team.
Take your medications as prescribed, even when you dont have symptoms. Skipping medications youre supposed to take can lead to flareups and make the disease harder to control. Your best shot at managing ulcerative colitis is to follow your treatment plan and talk to your healthcare provider regularly.
Read Also: Stomach Ulcer Treatment In Homeopathy
Possible Complications From Surgery
Part of bowel surgery involves creating a pouch near the anus, which collects waste prior to defecation.
One of the complications of surgery is that the pouch can become inflamed, which causes diarrhea, cramps, and fever. This is called pouchitis, and it can be treated with an extended course of antibiotics.
The other main complication of bowel resection is small bowel obstruction. A small bowel obstruction is first treated with intravenous fluid and bowel rest . However, a severe small bowel obstruction may need to be treated with surgery.
Although surgery may cure the gastrointestinal symptoms of UC, it may not always cure other affected sites. Occasionally, people with UC have inflammation of the eyes, skin, or joints.
These types of inflammation may persist even after the bowel has been totally removed. While this is uncommon, it is something to consider before getting surgery.
Symptoms Of A Duodenal Ulcer
If you have a duodenal ulcer, you might:
- have pain in the stomach or abdomen
- have indigestion
Very occasionally, an ulcer can cause serious complications. Go to the emergency department if:
- you have a sharp pain in your stomach that doesnt go away
- your vomit or stools look bloody or a black colour
If you are concerned about symptoms, you can use healthdirects online Symptom Checker to get advice on the next appropriate healthcare steps and when to seek medical attention.
Read Also: Is Ulcerative Colitis And Colitis The Same Thing
Don’t Miss: How To Ease Mouth Ulcer Pain
Oral Vs Rectal Treatments
Most physicians prescribe ulcerative colitis patients oral versions of 5-ASAs or corticosteroids, since this is a patient-preferred delivery method of medication. However, even if they have a specially designed release mechanism, they might not reach and treat the area where the disease is most active.
For example, when you apply sunscreen to your skin, you need to make sure that you cover every exposed part to protect it from the sun. Similarly, when applying these treatments to your rectum and lower colon, you need to make sure that the product covers all of the inflamed areas.
Oral tablets might not be the optimal way to reach the end of the colon, where stool and the fact that ulcerative colitis patients have diarrhea, might interfere with its effectiveness. Unfortunately, this is also the area in the colon where a flare usually starts. The best way to reach this particular area is by inserting the drug directly into the rectum.
The medication released from a suppository will travel upward and usually reach about 15 cm inside from the anus. An enema will reach farther, about 60 cm. Those with ulcerative colitis usually insert these formulations before bedtime, and this way the medication is retained as long as possible. Stool does not typically interfere with the drug, since the bowel area is typically relatively empty right before bed.
Does Ulcerative Colitis Make You Immunocompromised
Ulcerative colitis doesnt make you immunocompromised. Some of the medicines that treat it may change the way your immune system responds. This change is different for each medication. Some of these changes may increase the risk of certain infections or other issues. A discussion with your health care team before starting a medication is the best way to understand these risks and ways to prevent them.
You May Like: Ulcerative Colitis Rectal Pain Relief
Who Gets Ulcerative Colitis
Anyone at any age, including young children, can get ulcerative colitis. Your chance of getting it is slightly higher if you:
- Have a close relative with inflammatory bowel disease .
- Are between 15 and 30 years old, or older than 60.
- Are Jewish.
- Use frequent nonsteroidal anti-inflammatory drugs like ibuprofen .
Diet And Nutrition In Crohns Disease
MMaintaining good nutrition with Crohns disease can be a challenge. Some foods may provoke your symptoms, and others may ease them. But no single meal plan will work for every person with Crohns. Weight loss as well as specific vitamin and mineral deficiencies may occur. Patients whose inflammation is still active do not have much of an appetite, so their intake of food is reduced or the types of foods they eat are restricted. Eating can also make symptoms worse, so people with this disease may eat less. Finally, if a substantial portion of the small intestine is inflamed, the inflamed intestine may not absorb nutrients normally. Good nutrition depends on the control of inflammation, but when that is not achievable, it depends on supplemental vitamins, minerals, and calories.
Dont Miss: Ulcerative Colitis Abdominal Pain Relief
Read Also: What Should You Eat If You Have Ulcerative Colitis