Surgery In Crohn’s Disease
Surgery is avoided in Crohn’s disease if possible because it is likely that inflammation will recur even when it appears that all inflammation has been removed during surgery. There are situations in which surgery often becomes necessary such as with strictures, intestinal obstruction, or symptoms that do not respond to any medical treatment. Usually, the surgery that is done is kept to the minimum that is necessary to take care of the complication. Surgery may include removal of parts of the intestine, stretching of strictures, and removal of fistulas. But at times it may require resection of the entire colon, which may necessitate a colostomy or ileostomy.
How To Reduce Risks For Ulcer
The American Association of Equine Practitioners recommends the following management tips for ulcer-prone horses:
- Allow free-choice access to grass or hay
- Feed smaller, more frequent meals
Though some ulcers may spontaneously resolve on their own, most will need treatment in order to heal, especially when horses remain in performance or training. There are several different approaches to treating ulcers in horses, but the primary one is acid suppressive therapy.
The most commonly prescribed ulcer treatment is omeprazole, an FDA approved proton pump inhibiting drug that has been well studied. Other drugs may prescribed depending on the location and severity of your horses ulcers. Some of these treatments include histamine blockers, coating or binding agents, synthetic hormones, prokinetic agents, and antibiotics, and a combination of several therapies is used in some instances.
Complications Of Crohn’s Disease
Several complications of Crohn’s disease have already been mentioned, including nutritional deficiencies, loss of weight, anemia, growth retardation, and delayed puberty. Two more serious complications also mentioned previously are strictures or narrowing of the intestine due to scarring and the formation of fistulas. Massive intestinal bleeding and perforation are unusual.
Recommended Reading: Does Ulcerative Colitis Make You Tired
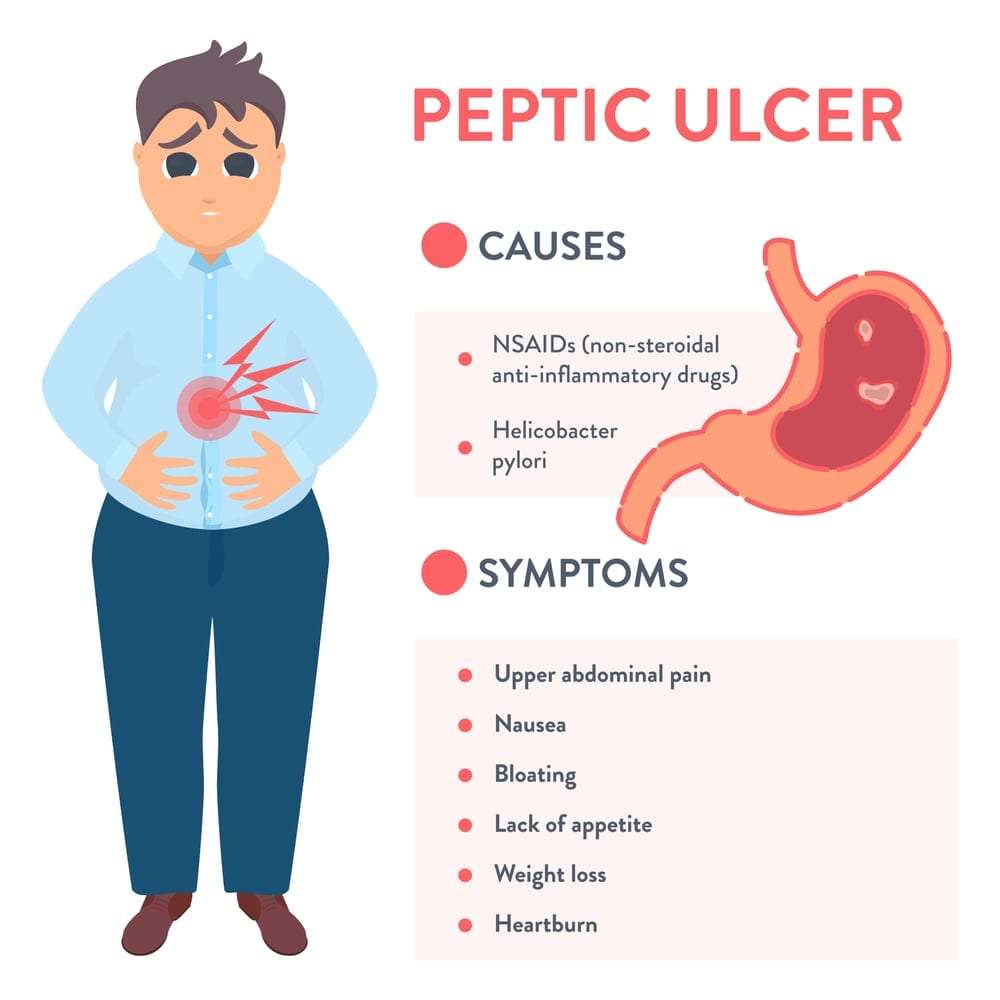
How Do Nsaids Cause A Peptic Ulcer
To understand how NSAIDs cause peptic ulcer disease, it is important to understand how NSAIDs work. Nonsteroidal anti-inflammatory drugs reduce pain, fever, and inflammation, or swelling.
Everyone has two enzymes that produce chemicals in your bodys cells that promote pain, inflammation, and fever. NSAIDs work by blocking or reducing the amount of these enzymes that your body makes. However, one of the enzymes also produces another type of chemical that protects the stomach lining from stomach acid and helps control bleeding. When NSAIDs block or reduce the amount of this enzyme in your body, they also increase your chance of developing a peptic ulcer.
How Are Peptic Ulcers Diagnosed
Your healthcare provider will look at your past health and give you a physical exam. You may also have some tests.
Imaging tests used to diagnose ulcers include:
- Upper GI series or barium swallow. This test looks at the organs of the top part of your digestive system. It checks your food pipe , stomach, and the first part of the small intestine . You will swallow a metallic fluid called barium. Barium coats the organs so that they can be seen on an X-ray.
- Upper endoscopy or EGD . This test looks at the lining of your esophagus, stomach, and duodenum. It uses a thin lighted tube called an endoscope. The tube has a camera at one end. The tube is put into your mouth and throat. Then it goes into your esophagus, stomach, and duodenum. Your health care provider can see the inside of these organs. A small tissue sample can be taken. This can be checked for H. pylori.
You may also have the following lab tests to see if you have an H. pylori infection:
Also Check: What Is The Medication For Ulcerative Colitis
Visceral+ For Equine Ulcers
Mad Barns Visceral+ is a comprehensive nutritional supplement designed specifically for horses with EGUS as well as other digestive issues. Visceral+ has been clinically studied in horses and shown to maintain healthy stomach tissue.
Visceral+ is formulated with the highest quality probiotic ingredients, natural nutrients, minerals, and amino acids that naturally support the bodys own healing mechanisms. This supplement provides complete nutritional support for your horses digestive system. Unlike certain ulcer treatments, it does not inhibit the natural production of stomach acid which is vital to proper digestion.
Visceral+ was developed in conjunction with veterinarians who were looking for a natural nutritional formula that could support a healthy gastro-intestinal system.
This product works in four key ways to maintain and balance the horses digestive system:
Diagnosis Of A Stomach Ulcer
Diagnosing a stomach ulcer is done using a range of methods, including:
- Endoscopy a thin flexible tube is threaded down the oesophagus into the stomach under light anaesthesia. The endoscope is fitted with a small camera so the physician can see if there is an ulcer.
- Barium meal a chalky liquid is drunk and an x-ray is performed, showing the stomach lining. These tests are less common nowadays, but may be useful where endoscopy is unavailable.
- Biopsy a small tissue sample is taken during an endoscopy and tested in a laboratory. This biopsy should always be done if a gastric ulcer is found.
- C14 breath test this checks for the presence of H. pylori. The bacteria convert urea into carbon dioxide. The test involves swallowing an amount of radioactive carbon and testing the air exhaled from the lungs. A non-radioactive test can be used for children and pregnant women.
You May Like: Ulcerative Colitis Rectal Pain Relief
Youve Had Unexplained Vomiting
From time to time, the nausea brought on by ulcers may become so intense that it could actually cause you to vomit. Frequent vomiting is never a fun experience, but whatever you do, stay away from medications like ibuprofen and aspirin when treating the condition and other ulcer symptoms. According to Dr. Sengupta, these over-the-counter pain medications actually put you at a higher risk of developing ulcers, and can make your current ulcers worse.
How Can I Be Sure Its An Ulcer
The only way to be sure an ulcer is causing your discomfort is with a medical diagnosis. We will evaluate your medical history and conduct a thorough physical examination.
To determine the root cause of your ulcer, we may run blood, stool, or breath tests. These tests are designed to look for signs of helicobacter pylori, the bacteria linked to ulcers.
Depending on your unique symptoms, we may also order an endoscopy. During an endoscopy, we insert a tube with a tiny camera down your throat and into your stomach to take pictures of any potential damage and collect tissue samples for analysis.
Read Also: Are Ulcerative Colitis And Ibs The Same
Treatment Of A Bleeding Peptic Ulcer
The initial treatment for a bleeding peptic ulcer is the same as a non-bleeding ulcer provided that the bleed is minor. Firstly the cause of the ulcers need to be removed. NSAIDs and other drugs that may be causing the peptic ulcers need to be discontinued or change to alternate medication that are less likely to affect the gut lining. Secondly peptic ulcer treatment needs to be initiated as soon as possible.
- Antibiotics to eradicate H.pylori bacteria.
- Antacids to neutralize stomach acid.
- Acid-suppressing medication to reduce stomach acid production.
- Ulcer-protecting drugs to assist ulcers to heal.
These measures should assist with the healing of the ulcer and the bleed may therefore cease. However, if there is a continuous minor bleed or massive blood loss from an ulcer then more invasive procedures are necessary. Endoscopic therapy where the site of the bleed is sealed is the first option. For acute bleeds, hemoclips may also be used during or after endotherapy to stop the bleed.
What Are The Complications Of Inflammatory Bowel Disease Or Ibd
The complications of inflammatory bowel disease or IBD are many. Below mentioned are the complications of crohns disease and ulcerative colitis separately:
Some of the complications because of the onset of crohns diseases are as follows:
Complications of inflammatory bowel disease or IBD arising out of ulcerative colitis are as follows:
- Acute bleeding is a complication in ulcerative colitis.
- Numerous perforations along the walls of the colon are a possible complication in ulcerative colitis.
- Acute dehydration.
- Osteoporosis is a complication in ulcerative colitis.
- Skin along with eyes can be affected by inflammation.
- Mouth ulcers are a likely complication in ulcerative colitis.
- Vulnerabilities to the occurrence of cancer in colon are a complication in ulcerative colitis.
- Clotting in arteries and veins are likely complications in ulcerative colitis.
Also Check: How Do Doctors Test For Ulcerative Colitis
How Are Peptic Ulcers Treated
Treatment will depend on the type of ulcer you have. Your healthcare provider will create a care plan for you based on what is causing your ulcer.
Treatment can include making lifestyle changes, taking medicines, or in some cases having surgery.
Lifestyle changes may include:
- Not eating certain foods. Avoid any foods that make your symptoms worse.
- Quitting smoking. Smoking can keep your ulcer from healing. It is also linked to ulcers coming back after treatment.
- Limiting alcohol and caffeine. They can make your symptoms worse.
- Not using NSAIDs . These include aspirin and ibuprofen.
Medicines to treat ulcers may include:
- Antibiotics. These bacteria-fighting medicines are used to kill the H. pylori bacteria. Often a mix of antibiotics and other medicines is used to cure the ulcer and get rid of the infection.
- H2-blockers . These reduce the amount of acid your stomach makes by blocking the hormone histamine. Histamine helps to make acid.
- Proton pump inhibitors or PPIs. These lower stomach acid levels and protect the lining of your stomach and duodenum.
- Mucosal protective agents. These medicines protect the stomach’s mucus lining from acid damage so that it can heal.
- Antacids. These quickly weaken or neutralize stomach acid to ease your symptoms.
In most cases, medicines can heal ulcers quickly. Once the H. pylori bacteria is removed, most ulcers do not come back.
Key Points About Ulcerative Colitis In Children
-
Ulcerative colitis is an inflammatory bowel disease. In this condition, the inner lining of your childs large intestine and rectum gets inflamed.
-
This inflammation causes diarrhea or frequent emptying of the colon. Your child may also have stomach pain and diarrhea.
-
Treatment may include avoiding foods that cause symptoms, taking medicine, and having surgery.
-
Children with this condition need long-term care. Your child may have times when symptoms go away. But symptoms usually come back.
Don’t Miss: Can Ulcerative Colitis Cause Blood In Urine
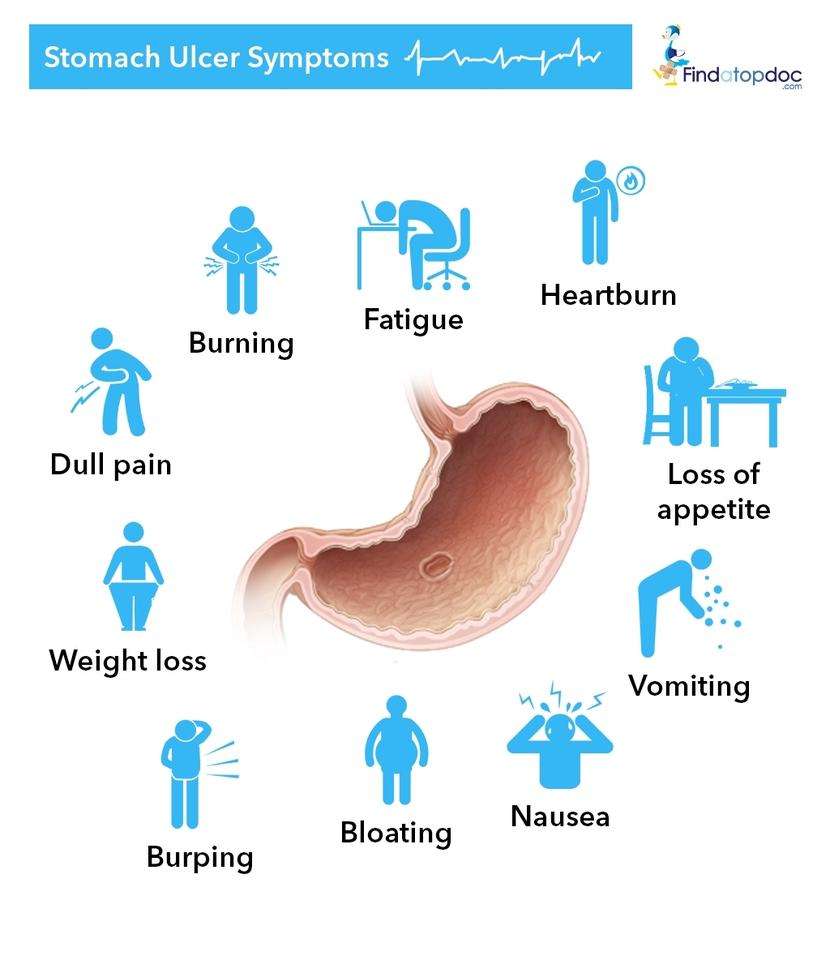
Stomach Ulcer 15 Common Signs & Symptoms
Gastric ulcers, also known as stomach ulcers are one of two types of ulcers that affect the stomach and small intestine. An ulcer can be defined as a break in the continuity of the skin or mucous lining due to multiple reasons such as acid overload, drug abuse, stress, and infections. Similarly, stomach ulcers are a discontinuity in the stomach lining that leads to various troublesome signs and symptoms. They occur when the thick mucus layer that protects the stomach from harsh acid and digestive juices is reduced or broken down. It allows acid to digest the tissues and stomach lining, causing a stomach ulcer.
Peptic ulcers are common among men and elderly around the world. They may affect 10-15% of the population. The most common causes of stomach ulcers include long term use of aspirin or other nonsteroidal anti-inflammatory drugs such as Aleve, Advil, etc. and infection with the bacterium H. Pylori., Although spicy foods and stress dont cause stomach ulcers, they can aggravate the underlying condition and make your symptoms worse.
The most common signs and symptoms of gastric ulcers include
How Does Pediatric Ulcerative Colitis Affect My Childs Mental/emotional Health
Like many conditions, ulcerative colitis can have a negative psychological effect, especially on children. They can experience physical, emotional, social and family problems. Because of the medications and/or general stress from the situation, your child may experience:
- Mood swings.
- Worry about appearance and physical stamina.
- Vulnerability because their body doesnt function normally.
- Poor concentration.
- Misunderstandings with friends and family.
Children need mutual support from all family members. Its helpful for the entire family to learn about the disease and try to be empathetic. Seek out a psychiatrist and therapist to help your child manage such challenges of their ulcerative colitis.
You May Like: Diet For Gerd And Ulcers
Is It Important To Treat A Flare Early Or Is It Ok To Wait A Bit
Inflammation typically does not resolve without treatment and early intervention has a better outcome than waiting to treat. At an early stage of a flare, a more optimal baseline treatment is often enough to get the inflammation under control. If you wait, there is a greater risk that you might need drugs with greater side effects, such as oral steroids. By waiting, you will have to manage longer with your symptoms before getting relief. Living with constant or longer periods of inflammation might increase your risk for future complications, as inflammation might cause damage to the gut wall that accumulates in severity with each flare.
If you are experiencing worsening symptoms, you have probably already had the flare for some time without symptoms. Evidence shows that a stool test for inflammation in the colon, called fecal calprotectin, is often elevated for two to three months before any symptoms appear. Your colon might also start to show visual evidence of inflammation before you have symptoms, or at least indicate an increased risk for a flare.
Dietary And Lifestyle Modifications
As most nutrients are absorbed higher up in the digestive tract, those with ulcerative colitis generally do not have nutrient deficiencies however, other factors might influence your nutritional state. Disease symptoms may cause food avoidance, leading to food choices that might not provide a balanced diet. If bleeding is excessive, problems such as anemia may occur, and modifications to the diet will be necessary to compensate for this.
Generally, better overall nutrition provides the body with the means to heal itself, but research and clinical experience show that diet changes alone cannot manage this disease. Depending on the extent and location of inflammation, you may have to follow a special diet, including supplementation. It is important to follow Canadas Food Guide, but this is not always easy for individuals with ulcerative colitis. We encourage you to consult a registered dietitian, who can help set up an effective, personalized nutrition plan by addressing disease-specific deficiencies and your sensitive digestive tract. Some foods may irritate the bowel and increase symptoms even though they do not worsen the disease.
In more severe cases, it might be necessary to allow the bowel time to rest and heal. Specialized diets, easy to digest meal substitutes , and fasting with intravenous feeding can achieve incremental degrees of bowel rest.
Read Also: Medication For Ulcerative Colitis Flare Up
Stretching As If To Urinate
A horse suffering from EGUS may frequently stretch out like he needs to urinate. This behavior is likely an attempt to relieve discomfort in the abdominal region and is easy to recognize.
It should be noted that horses may also stretch out like this if they are experiencing gas colic. But if your horse displays this behavior on a frequent basis, it could very well be ulcers.
Complications Of Ulcerative Colitis
UC increases your risk of developing colon cancer. The longer you have the disease, the higher your risk of this cancer.
Because of this increased risk, your doctor will perform a colonoscopy and check for cancer when you receive your diagnosis.
Repeat screenings are recommended thereafter, according to the American Cancer Society. Regular screenings help lower your risk of colon cancer. Follow-up screenings can detect precancerous cells early.
Other complications of UC include:
- thickening of the intestinal wall
- intestinal bleeding
Read Also: Symptoms Of Crohn’s Vs Ulcerative Colitis
How Is An Ulcer Diagnosed
Your doctor will ask you about your symptoms. They may do an endoscopy. This procedure involves inserting a thin, flexible tube attached to a camera down your throat and into your stomach. Your doctor will test your blood, breath or stool for H. pylori. They also can test a sample of your stomach lining. Your doctor also will ask you if you regularly take aspirin or anti-inflammatory medicines.
Peptic Ulcers: Is Stress A Culprit

Contrary to popular belief, most ulcers do not actually result from stress or eating too many spicy foods.
In 2005, Drs. Barry Marshal and Robin Warren, from Australia, received the Nobel Prize in Medicine for discovering that a spiral-shaped bacterium that can colonize the human stomach is the offending cause in many cases.
Smoking tobacco, and drinking alcohol, may worsen ulcers, and as little as one baby aspirin daily can cause an ulcer.
Also Check: What Foods Should Be Avoided With Stomach Ulcers
Types Of Ulcerative Colitis
UC can be categorized according to the parts of the GI tract that it affects.
- Ulcerative proctitis. In ulcerative proctitis, only the rectum is inflamed. Its considered a mild form of UC.
- Left-sided colitis. Left-sided colitis causes inflammation in the area between the splenic flexure and the last section of the colon. The last section of the colon, known as the distal colon, includes the descending colon and sigmoid colon. Left-sided colitis is also known as distal ulcerative colitis.
- Proctosigmoiditis. Proctosigmoiditis is a form of left-sided colitis. It causes inflammation in the rectum and sigmoid colon.
Different tests can help a doctor diagnose UC. UC mimics other bowel diseases such as Crohns disease. A doctor will order multiple tests to rule out other conditions.
Tests to diagnose UC often include: