Living With Ulcerative Proctitis
Many people with ulcerative proctitis lead normal active lives. Symptoms may vary from person to person. Whether symptoms are constant or present only during a flare-up, regular appointments with a physician are necessary to monitor the disease and adjust medications where necessary.
Stress and tension can make symptoms of ulcerative proctitis worse. Decreasing stress and practicing relaxation techniques may help.
Those living with ulcerative proctitis may find it helpful to talk to others experiencing the same symptoms. Support groups are a good place to start. The Crohns and Colitis Foundation has a register of over 200 support groups across the United States.
Proctosigmoiditis Causes And Risk Factors
Proctosigmoiditis is a result of chronic inflammation in the colon, like all types of ulcerative colitis. This inflammation is the result of an immune response. Doctors dont know what triggers this immune response.
Some people are more likely than others to develop ulcerative colitis. The risk factors for all types of ulcerative colitis are the same. They include:
- having a family history of ulcerative colitis
- having a history of infection with Salmonella or Campylobacter bacteria
- living at a higher latitude
- living in a developed nation
These factors only increase the risks for ulcerative colitis. Having one or more of these risk factors doesnt mean youll get the condition.
Ways To Manage Up And Uc
When it comes to treating both UP and UC, there are a number of different paths you can take. But unfortunately, there isnt a cure for either condition yet.
Like most inflammatory conditions, treatment of UP and UC is multifaceted. Your treatment plan will be designed to ease your , while also addressing the underlying inflammation. The end goal of treatment is to help you reach remissiona period of time when you are symptom-free. Your will depend on the severity of your condition, and may involve a combination of therapies, says Dr. Kinnucan. For example, if your symptoms are relatively mild and limited to the rectum, then your doctor may recommend rectum therapies such as steroids and mesalamine , Dr. Kinnucan says. In more severe cases, or if the inflammation has spread into other parts of the colon, systemic medications like biologics or other small molecule therapies may be necessary, she adds.
Read Also: Foods That Affect Ulcerative Colitis
What Causes Ulcerative Colitis
Ulcerative colitis is thought to be an autoimmune condition.
This means the immune system, the body’s defence against infection, goes wrong and attacks healthy tissue.
The most popular theory is that the immune system mistakes harmless bacteria inside the colon as a threat and attacks the tissues of the colon, causing it to become inflamed.
Exactly what causes the immune system to behave in this way is unclear.
Many experts think it’s a combination of genetic and environmental factors.
Doctors Who Treat Ulcerative Colitis
Cleveland Clinic recommends beginning UC treatment with your usual doctor. If more testing is needed, theyll refer you to a gastroenterologist or colorectal surgeon for a colonoscopy. A gastroenterologist treats digestive issues. Colorectal surgeons conduct colon and rectum procedures. GIs manage UC treatment.
Other doctors will also help. A nutritionist will ensure you eat things your body can handle and obtain enough nutrientsa dermatologist for skin disorders and a rheumatologist for joint difficulties. Living with a chronic ailment is difficult therefore, physicians suggest visiting a psychologist for depression or anxiety. A third of UC patients require colorectal surgery.
You May Also Like
The Crohns & Colitis Foundation advises choosing a UC specialist carefully. Check that the doctor accepts your insurance, is nearby, and has a good bedside manner.
Also Check: What Foods To Avoid If You Have Ulcerative Colitis
What Is Ulcerative Colitis
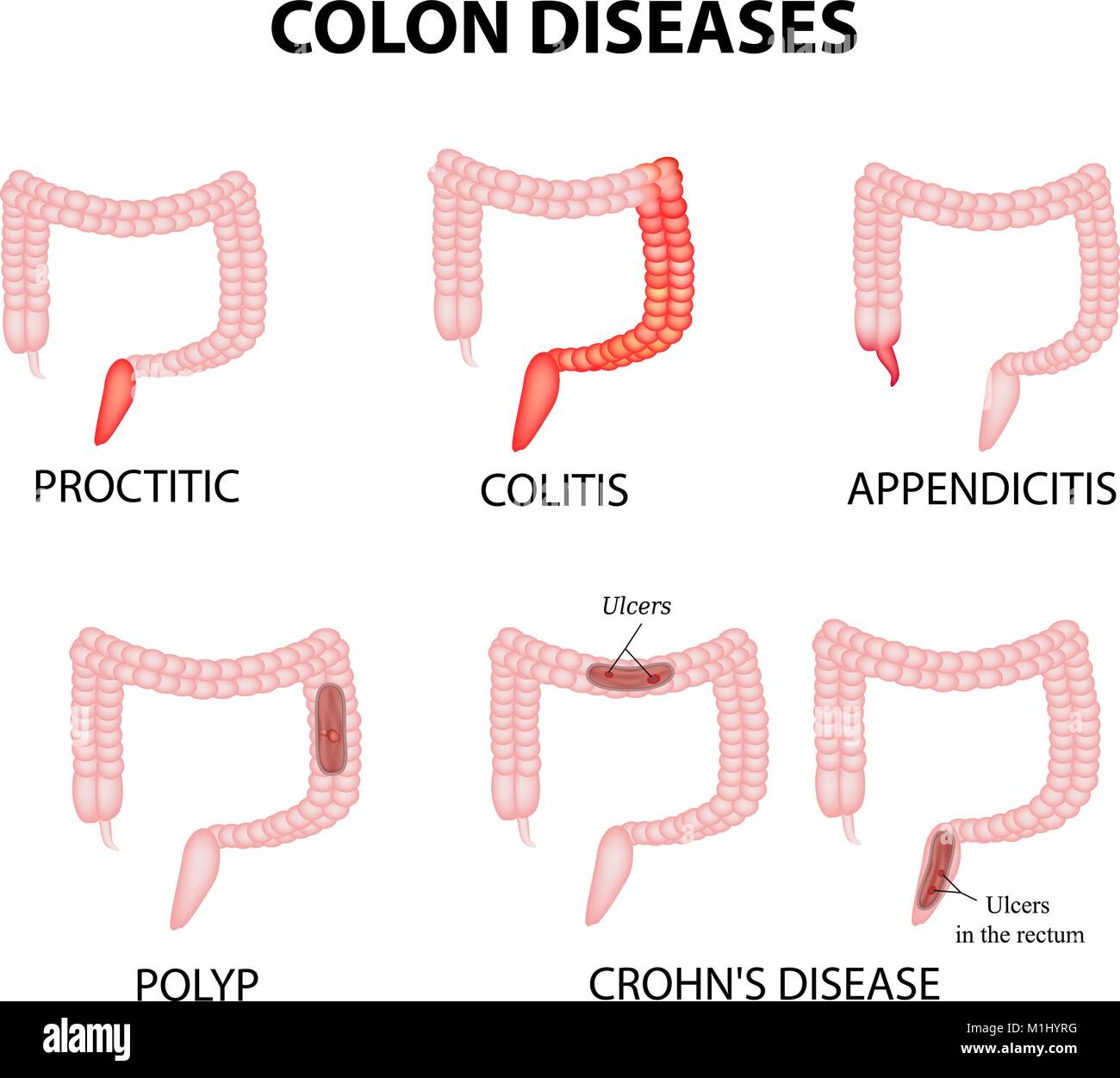
Ulcerative colitis is a chronic disease of the colon . The disease is marked by inflammation and ulceration of the colon lining which makes the colon empty frequently. Symptoms include diarrhea and often crampy abdominal pain. The inflammation usually begins in the rectum and lower colon, but it may also involve the entire colon. When ulcerative colitis affects only the rectum, it is called ulcerative proctitis.
Ulcerative colitis differs from Crohns disease. Both diseases are called inflammatory bowel disease . Crohns disease can affect any part of the GI tract, whereas ulcerative colitis affects only the colon. The inflammation affects only the innermost lining of the colon, but in Crohns disease, it can affect the entire thickness. Inflammation from ulcerative colitis occurs in a continuous process there are no areas of normal intestine between the areas of the diseased intestine. In contrast, skip areas may occur in Crohns disease.
Sudden Severe Ulcerative Colitis
This complication is the main cause of emergency surgery in patients with ulcerative colitis. With sudden, severe ulcerative colitis, medications and intravenous steroids, are unable to control the symptoms.
-
Uncontrolled bleeding can occur from deep ulcerations in the colon, though that is rare.
-
Severe, sudden ulcerative colitis can lead to toxic megacolon, a potentially life-threatening complication caused by severe inflammation.
-
Toxic megacolon leads to rapid enlargement of the colon. Symptoms include pain, distension or swelling of the abdomen, fever, rapid heart rate, constipation, and dehydration.
-
Toxic megacolon requires immediate treatment and surgery.
Read Also: Ulcerative Colitis And Inflammatory Bowel Disease
How Can I Manage The Symptoms Of Ulcerative Proctitis
If you have ulcerative proctitis or ulcerative colitis, here are some treatment options your doctor may recommend to help manage and reduce the symptoms.
- For pain: To help reduce pain, doctors prefer to prescribe acetaminophens, such as Dayquil or Percocet, over nonsteroidal anti-inflammatory drugs, such as ibuprofen.
- For hard stool: A doctor may suggest stool looseners that can help.
- For blood loss: Doctors may recommend you start taking iron supplements.
- For diarrhea: Anti-diarrheal medications or lifestyle changes can help you ease diarrhea, including codeine, plant-based fibers, dietary adjustments, and more.
In case of complications that require hospitalization, a doctor may prescribe antibiotics, or order a blood transfusion, electrolytes, or IV fluids.
Learn treatment options for ulcerative colitis.
Ulcerative Proctitis: What Is It And How Is It Treated
Patologies
Ulcerative proctitis1 is the inflammation of the lining in the inner wall of the rectum. Given that feces pass through the rectum to come out the organism, the evacuation act becomes painful for the patient. Besides, this kind of ulcerative colitis causes diarrhea, bleeding, secretion and the feeling of having the urgent need to go to the bathroom. All these symptoms can last a short time or, conversely, become chronic.
There exist numerous causes2 for a person to suffer from ulcerative proctitis. The most frequent is to suffer an inflammatory bowel disease . But there are also other factors that may cause this condition. Some motives for suffering proctitis are sexually transmitted diseases, organism immunodeficiency, bacteria like Salmonella or antibiotics that destroy the gut flora. It may also be a side effect of radiotherapy used to treat prostate and rectal cancer.
What are the symptoms of the ulcerative proctitis?
The most frequent signs of ulcerative proctitis are constant urge to defecate, rectal bleeding or painful depositions. The mucus discharge of the rectum, the rectal or abdominal pain and diarrhea are also typical symptoms. If you experience any one of them, it is convenient for you to visit your physician.
What is the appropriate treatment for the ulcerative proctitis?
The treatment3 for this disease depends on the cause of the inflammation.
How is ulcerative proctitis diagnosed?
What is the appropriate treatment for the ulcerative proctitis?
You May Like: How To Heal Ulcers In Large Intestine
What If Proctitis Is Not Treated
Proctitis that is not treated or does not respond to treatment may lead to complications, including
- Severe bleeding and anemiaa condition in which red blood cells are fewer or smaller than normal, which means less oxygen is carried to the bodys cells
- Abscessespainful, swollen, pus-filled areas caused by infection
- Ulcers on the intestinal lining
- Fistulasabnormal connections between two parts inside the body
People with proctitis symptoms need medical attention. If diagnosed with proctitis, patients should take all medications as prescribed and see their doctor for a followup appointment to be sure the cause of the inflammation has been treated successfully.
What Should I Ask My Doctor On Behalf Of My Child Or Teenager
Ask your healthcare provider the following questions in addition to the ones listed above:
- What vitamins should my child take?
- Will my other children have pediatric ulcerative colitis?
- Is my child at risk for other conditions?
- Can you recommend a psychiatrist or therapist to help my child with emotional issues related to pediatric ulcerative colitis?
- Is my child growing at a normal rate?
- What can I do to help my child cope at school?
A note from Cleveland Clinic
When you have ulcerative colitis, its essential to work closely with your healthcare team.
Take your medications as prescribed, even when you dont have symptoms. Skipping medications youre supposed to take can lead to flareups and make the disease harder to control. Your best shot at managing ulcerative colitis is to follow your treatment plan and talk to your healthcare provider regularly.
Donât Miss: Can I Eat Oatmeal With Ulcerative Colitis
You May Like: Is Nexium Good For Ulcers
Complications Outside The Bowel
Colitis doesnt just affect the bowel. As many as 1 in 5 people with Colitis develop problems in other parts of the body. Most affected are joints, eyes or skin. These are known as extraintestinal manifestations . They usually happen during a flare-up, but can occur without or before any bowel symptoms. These complications can often happen to people who dont have Colitis too. For many of the complications, there are things you can do to reduce your risk.
Joints
You may have pain and/or swelling in your joints. Around 1 in 6 people with Colitis experiences joint problems. For some, this will get worse during a flare, but will usually improve with treatment for Colitis. Others may have joint problems even when bowel symptoms feel better. Find out more in Joints.
Bones
People with Colitis are more at risk of developing thinner and weaker bones or osteoporosis. This can be due to ongoing inflammation, smoking, taking steroids or low levels of physical activity. Calcium is needed for bone formation, and this may be low if your diet doesnt contain enough dairy. Weight-bearing exercise, calcium and vitamin D supplements, not smoking and avoiding long-term steroid use can help. Some people may also take bisphosphonate medicines. Find out more in our information on Bones.
Skin
Colitis can affect the skin in different parts of the body.
Eyes
Anemia
Anaemia can make you feel very tired. If its more severe you may also have shortness of breath, headaches, and general weakness.
Liver
What Can Cause Ulcerative Proctitis
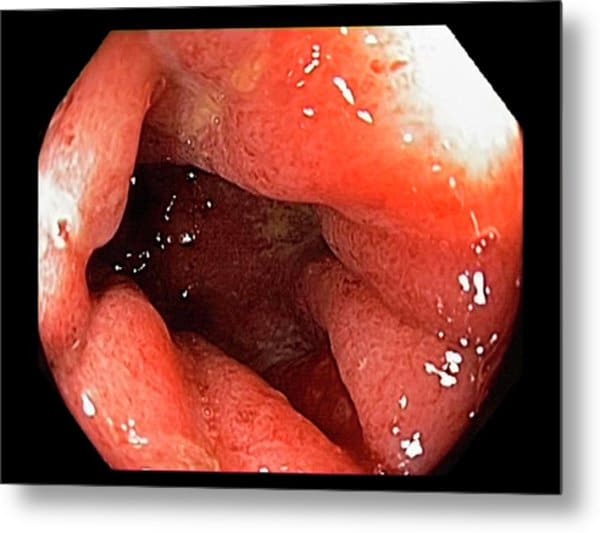
The actual cause of the inflammation is still unknown, but there is considerable evidence pointing towards the environmental factors, intestinal flora, immune dysregulation, and genetic predisposition. The genetic transformation is slightly higher in this case. However, it is still unclear why the inflammation is limited to the rectum.
You May Like: Foods To Avoid During Ulcerative Colitis Flare Up
What Is Ulcerative Proctitis
Of the people who have UC, about 25% to 55% have ulcerative proctitis when they are diagnosed. Your doctor diagnoses ulcerative proctitis based on where in the colon UC is present. When the disease is located in the last 15 centimeters of the colon , it’s termed ulcerative proctitis. If you have UP, you may experience:
-
Rectal bleeding
-
An urgency in your bowel movements
Ulcerative proctitis presents with symptoms such as rectal bleeding and pain, a persistent feeling that you need to have a bowel movement, says Elena Ivanina, M.D., and director of neuro-integrative gastroenterology at Lenox Hill Hospital in New York City. That, or your rectum feels full and your bowel movements have changed, most often to diarrhea.
Can I Die Of Ulcerative Colitis Or Ulcerative Proctitis
Are they fatal? This is one of the most frequently asked questions when one realizes that one has to fight against this chronic disease. Even though it is a long-term situation, the condition itself is not fatal but can cause life-threatening complications. Talking about ulcerative proctitis, the symptoms are quite similar to that of ulcerative colitis. However, ulcerative proctitis is not as serious as colitis, as it is limited to the rectum.
Also Check: Ulcerative Colitis Flare Up Foods To Eat
How Can I Find Support After An Ulcerative Colitis Diagnosis
When taking care of your physical well-being, dont forget that ulcerative colitis can take a toll on your emotional and mental well-being too. If it turns out your symptoms are ulcerative colitis, you can find a support group, or ask your doctor if they can connect you with a therapist or G.I. psychologist. Dr. Riehl, for example, works with patients on aspects of body image and even connects them with other patients who have experienced colectomy or ostomy . We talk openly about the impact that it can have on them from an intimacy perspective to how it impacts their self-identity, she says.
Since ulcerative colitis often starts at an age when people are thinking about their first job or starting a family, it can be particularly tough. One of the reasons that I and several of my colleagues went into this field is precisely because of thatso that we can hopefully make a difference in peoples lives early, and have them be able to lead productive and complete lives by putting their disease in remission, Dr. Sinha says.
What Is The Difference Between Ulcerative Colitis And Pancolitis
Ask U.S. doctors your own question and get educational, text answers â its anonymous and free!
Ask U.S. doctors your own question and get educational, text answers â its anonymous and free!
HealthTap doctors are based in the U.S., board certified, and available by text or video.
Read Also: What Foods Should You Avoid When You Have An Ulcer
Read Also: Mouth Ulcer On Tongue Remedies
Complementary And Alternative Medicine
Probiotics may modestly reduce disease activity in active disease, but do not increase remission rates.34 However, Lactobacillus GG and Escherichia coli Nissle 1917 have been shown to be as effective as 5-ASA for maintenance therapy.16,17 Acupuncture has shown a small symptomatic benefit in active disease.35 Wheatgrass has also shown some effectiveness in reducing symptoms of active disease.36
Also Check: How To Reduce Stomach Ulcer
Types Of Ulcerative Colitis
Becoming well-informed about your chronic illness is a helpful part of your journey. It is important to learn all you can about your diagnosis and how it may affect you. We can help you understand the different types of ulcerative colitis, as well as the common symptoms and complications.
Ulcerative colitis is a chronic illness that can affect different parts of the colon and rectum. There is a wide array of symptoms and complications depending on the extent of your disease and the type of ulcerative colitis you have.
Getting diagnosed with a chronic, lifelong disease is overwhelming. It is important to learn all you can about your diagnosis and how it may affect you. We can help you understand the different types of ulcerative colitis, as well as the common symptoms and complications.
Also Check: Is Ulcerative Colitis The Same As Colitis
Do Different Types Of Ulcerative Colitis Cause Different Symptoms
Certain symptoms may point to different types of ulcerative colitis. These types, as outlined by the Mayo Clinic, are classified by location within the body:
- Ulcerative proctitis: With this form of the condition, which tends to be the mildest, a person has inflammation in the area closest to the rectum. Rectal bleeding may be the only sign of the disease.
- Proctosigmoiditis: Inflammation with this form of the disease involves a persons rectum and lower end of the colon. Symptoms can include bloody diarrhea, abdominal pain, and an inability to go despite feeling like you need to let loose.
- Left-sided colitis: This involves inflammation from the rectum, through the lower colon, and into the descending colon. In addition to bloody diarrhea and abdominal pain on the left side, you may also experience weight loss. Most patients will have left-sided disease, Dr. Sinha says.
- Pancolitis: This usually impacts a persons entire colon, causing bloody diarrhea that can be severe, abdominal pain, fatigue, and rapid weight loss.
Read Also: Foam Boots For Pressure Ulcers
What Are The Causes Of Ulcerative Colitis
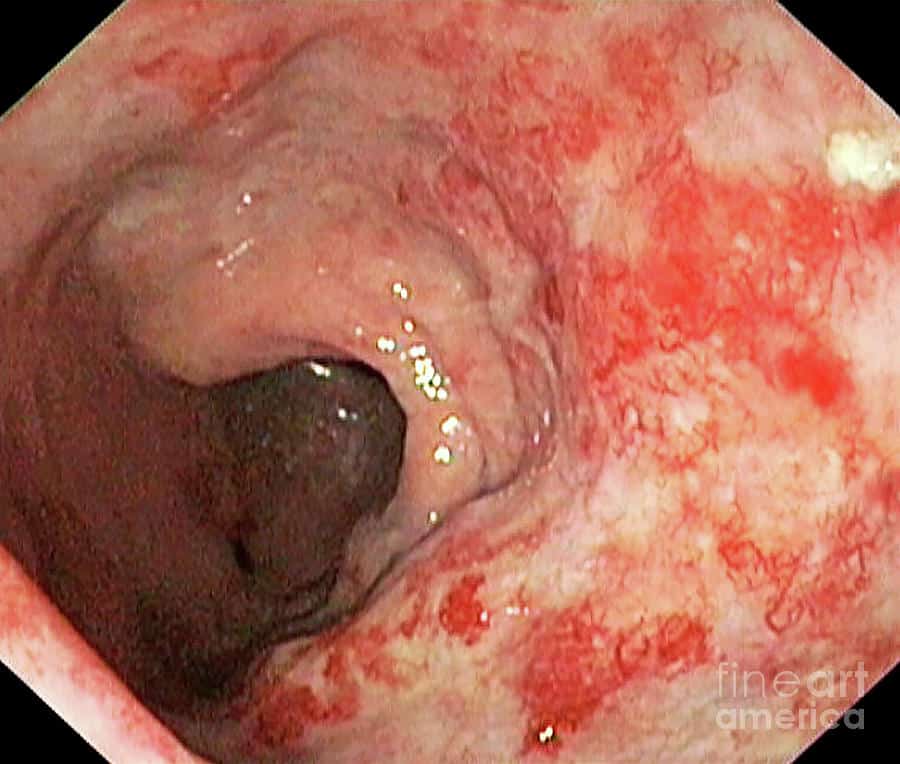
We do not yet know what causes this disease. Studies indicate that the inflammation in ulcerative colitis involves a complex interaction of factors: the genes the person has inherited, the immune system, and something in the environment. Foreign substances in the environment may be the direct cause of the inflammation, or they may stimulate the bodys defenses to produce an inflammation that continues without control. In patients with ulcerative colitis, once the patients immune system is turned on, it does not know how to properly turn off. As a result, inflammation damages the intestine and causes the symptoms of ulcerative colitis. One of the major goals of medical therapy is to help patients to better regulate their immune system.
You May Like: Foods To Help Ulcer Pain
What Are The Signs And Symptoms Of Ulcerative Colitis
Symptoms of ulcerative colitis include diarrhea which may be associated with crampy abdominal pain and sudden urgency to have a bowel movement. Diarrhea may begin slowly or quite suddenly. Loss of appetite, weight loss, and fatigue are also common symptoms. In cases of severe bleeding, anemia may occur. Approximately half of all patients with ulcerative colitis have relatively mild symptoms. The symptoms of ulcerative colitis tend to come and go, with fairly long periods in between flare-ups in which patients may experience no distress at all. These periods of remission can span months or even years, although symptoms do eventually return. Of note is that the disease is not always limited to the GI tract it can also affect the joints, eyes, skin, and liver.