Ulcerative Colitis Questions To Ask Your Doctor
Whether youâre worried your symptoms are UC, or you already have the condition and want more information, here are questions to ask your doctor:
- Are my symptoms a sign of ulcerative colitis or another condition?
- Are there different kinds of UC? Do they have different symptoms?
- What tests will I need?
- If I have ulcerative colitis, what will my treatment plan be?
- Will changing my diet or lifestyle help ease my symptoms?
- How serious is my ulcerative colitis?
- If I take medication for ulcerative colitis, will there be side effects?
- Should I take nutritional supplements like probiotics?
- How often will I need to come in for checkups?
- What should I do if my symptoms suddenly get worse?
- How do I know if my ulcerative colitis is getting worse?
- How do I know if I should change my ulcerative colitis medication?
- Should I consider surgery? What does surgery involve?
- What is my risk of getting colon cancer?
Why Choose Mount Sinai
Mount Sinai has a unique and rich tradition of specialized and individualized treatment and scientific research and discovery in ulcerative colitis. The physicians/scientists in the Mount Sinai Health System are constantly conducting clinical trials and are developing new drug therapies to help patients manage their disease. Learn more about ulcerative colitis.
There are 3 basic tests for colon cancer a stool test , sigmoidoscopy , and colonoscopy . All 3 are effective in catching cancers in the early stages, when treatment is most beneficial.
The esophagus, stomach, large and small intestine, aided by the liver, gallbladder and pancreas convert the nutritive components of food into energy and break down the non-nutritive components into waste to be excreted.
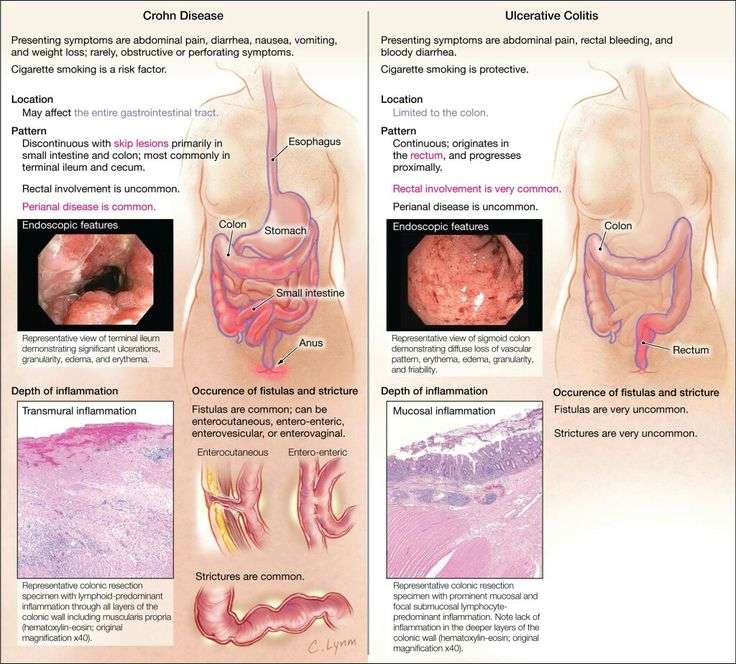
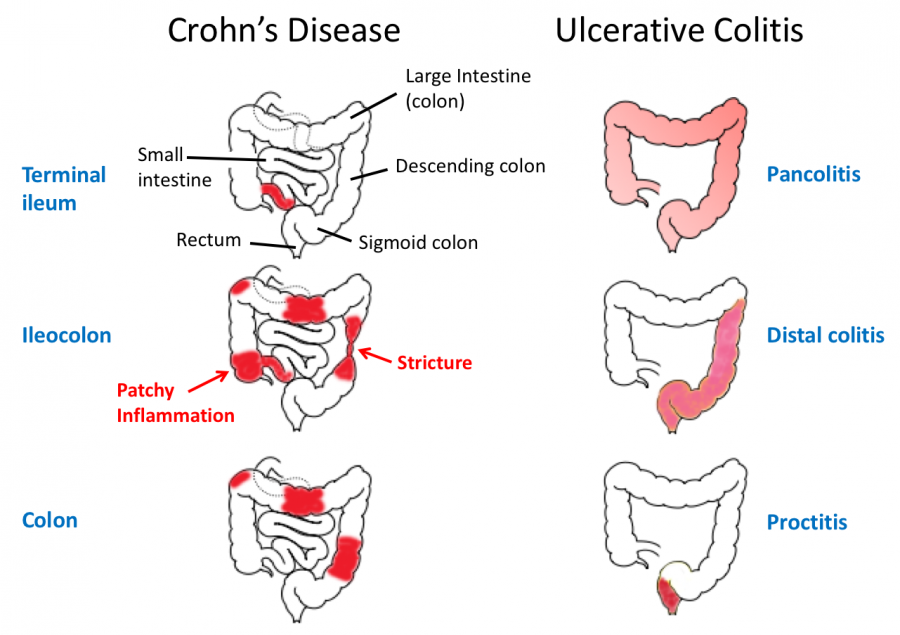
Ulcerative colitis is categorized according to location. Proctitis involves only the rectum. Proctosigmoiditis affects the rectum and sigmoid colon. Left-sided colitis encompasses the entire left side of the large intestine. Pancolitis inflames the entire colon.
When Should You Call Your Doctor
if you have been diagnosed with ulcerative colitis and you have:
- Fever over 38.3°C or shaking chills.
- Light-headedness, passing out, or rapid heart rate.
- Stools that are almost always bloody.
- Severe dehydration, such as passing little or no urine for 12 or more hours.
- Severe belly pain with or without bloating.
- Pus draining from the area around the anus or pain and swelling in the anal area.
- Repeated vomiting.
- Not passing any stools or gas.
If you have any of these symptoms and you have been diagnosed with ulcerative colitis, your disease may have become significantly worse. Some of these symptoms also may be signs of toxic megacolon. This is a condition in which the colon swells to many times its normal size. Toxic megacolon requires emergency treatment. Left untreated, it can cause the colon to leak or rupture. This can be fatal.
People with ulcerative colitis usually know their normal pattern of symptoms. Call your doctor if there is a change in your usual symptoms or if:
- Your symptoms become significantly worse than usual.
- You have persistent diarrhea for more than 2 weeks.
- You have lost weight.
You May Like: What Should You Eat With Ulcerative Colitis
You May Like: What Does An Ulcerative Colitis Flare Up Feel Like
Microscopic Featuresappraisal Of The Diagnosis
4.3.1 Early stage disease
It has been proposed that a non-specific increase in the inflammatory infiltrate in the lamina propria in combination with absent crypt architectural distortion, indicates a diagnosis of acute, infective colitis, rather than UC. This finding, however, is not confirmed in those studies of patients with early onset colitis .,
Basal plasmacytosis at the initial onset has a high predictive value for the diagnosis of IBD Repeat biopsies after an interval may help to solve differential diagnostic problems and establish a definitive diagnosis especially in adults, by showing additional features
Basal plasmacytosis is observed in biopsies obtained at early onset in 38100% of adult patients, and can help differentiate between UC and infectious colitis. It is particularly a feature in young children in these cases it is notably present in rectal biopsies and decreases proximally. It is an early feature, sometimes the first lesion to appear,,,, and a good predictive marker.
In young children or patients with an aberrant presentation of colitis, UC should always be considered in the differential diagnosis even if the pathology is not typical
Reliable diagnostic features may be absent from biopsies obtained in early onset disease, in acute severe colitis, or in patients with an atypical immunological response . The routine use of additional techniques such as immunohistochemistry is not recommended at present.
4.3.2 Established disease
Association With Clinical Phenotypes And Prognostic Indicators
In UC, very few studies have assessed acute phase markers in predicting outcome of disease or association with clinical phenotypes. In severe UC, after three days of intensive treatment patients with frequent stools , or 3-8 stools/d and CRP > 45 mg/L should be identified, as most of them will need to undergo colectomy. It is commonly accepted that the presence of ANCA in UC is not related to the duration and age of onset. Previous studies agree that in patients affected with CD, the presence of atypical pANCAs in serum characterizes an UC-like clinical phenotype.
Don’t Miss: Can Tylenol Cause Stomach Ulcers
How Do You Diagnose Ulcerative Colitis
It is OK to experience a bout of occasional abdominal cramps and diarrhea. However, if you have been experiencing these symptoms frequently, consult your doctor. It may be a sign of inflammatory bowel disease , such as ulcerative colitis.
Your doctor will diagnose ulcerative colitis after looking at several factors, including your medical history, a physical exam and a series of medical tests. They will ask if anyone in your family has ulcerative colitis. They will also ask you about other signs and symptoms of ulcerative colitis, including
In children, the condition can also affect their rate of growth.
The symptoms of ulcerative colitis are not the same in each affected person. Nearly half of the affected people experience mild symptoms of the disease. The condition increases your risk of colorectal cancer. Hence, visiting your doctor and getting diagnosed and treated early is important.
What Happens During These Ulcerative Colitis Tests
If youve ever found yourself with nothing but a thin hospital gown separating you from a room full of medical professionals ready to look in your colon, you probably know it can feel a little weird. But lets not scare those who havent been there yet. Its really not that bad. In the case of a colonoscopy, youll likely be sedated, and wont be aware of anything anyway.
That said, youll be asked to lay on your side with your knees tucked up by your chest. Your doctor will then insert the scope into your rectum and pump air or carbon dioxide as they move through, which inflates the colon so they can see the lining better. The camera sends images to an external monitor, where the doctor will look for any issues. Other tools can also be inserted to take a biopsy or remove abnormal tissue, such as polyps, according to the Mayo Clinic.
The exam itself can take anywhere from 15 minutes to 30 minutes to an hour for a colonoscopy. If you have a colonoscopy, youll have to stick around for an hour or so as the sedative wears off and have someone drive you home. As you recover, you might feel some abdominal cramping and the urge to pass gas. Our advice? Just let it go, everyone else in recovery is doing it too.
Also Check: How Long Do Stomach Ulcers Last
How Do I Prepare For A Sigmoidoscopy Or Colonoscopy
Truly the worst part of these tests is the prep you have to do before. Both require that you follow a special diet before the procedurethink clear liquidsand take a laxative, to effectively clean out your colon for the scope. You may also be asked to fast for a period of time and use an enema to flush out anything that remains in your colon . Your doctor may also need to adjust your medication schedule, if you take any, according to the Mayo Clinic.
Ruling Out Other Conditions
The symptoms of Crohns and Colitis can often be quite similar to other conditions like Irritable Bowel Syndrome , so your GP should first order some tests to rule them out. These tests cant confirm whether or not you have Crohns or Colitis, but they can help narrow down the possible causes of your symptoms.
For years I was misdiagnosed with skin conditions and allergies it only was after finally getting a faecal calproctectin test that I was diagnosed with Colitis. One year later, Im in remission and getting on with my life.
Megan, age 25Living with Colitis
Also Check: What Can You Do For An Ulcer In Your Mouth
You May Like: Foods To Treat Ulcerative Colitis
How Do We Diagnose Ulcerative Colitis
The Digestive Health Center at Stanford Health Care delivers expert diagnosis for all forms of inflammatory bowel disease, including ulcerative colitis. Part of what makes Stanford different is our expertise in measuring the degree of intestinal injury for each patient. This helps us understand the severity of your condition and how best to treat it.
Who Gets Ulcerative Colitis And What Causes It
Colitis can develop at any age, but usually first appears in people aged 15 to 30.
Experts are not sure why UC or Crohns disease occurs in some people. It may be due to a combination of genetic, environmental and infectious factors that cause a fault in the immune system leading to inflammation of the bowel.
You May Like: Whey Protein And Ulcerative Colitis
What Can I Expect If I Have A Diagnosis Of Ulcerative Colitis
Ulcerative colitis is a lifelong condition that can have mild to severe symptoms. For most people, the symptoms come and go. Some people have just one episode and recover. A few others develop a nonstop form that rapidly advances. In up to 30% of people, the disease spreads from the rectum to the colon. When both the rectum and colon are affected, ulcerative symptoms can be worse and happen more often.
You may be able to manage the disease with medications. But surgery to remove your colon and rectum is the only cure. About 30% of people with ulcerative colitis need surgery.
Simple Blood Test Possible For Detecting Ulcerative Colitis
Infrared spectroscopy and blood samples provide cheaper, less invasive screening alternative for inflammatory bowel disease.
Low-cost diagnostic tools for inflammatory bowel disease are lacking, but a simple blood test and infrared technology could detect the presence of disease and reduce the need for colonoscopies.
New study findings published in the Journal of Biophotonics suggest a novel testing procedure could be developed to help physicians more easily screen for ulcerative colitis.
IBDwhich includes ulcerative colitis and Crohns diseaseaffects an estimated 1.6 million individuals in the United States. Adults 50 years and older are expected to undergo a colonoscopy to search for any abnormalities in the intestine, which is a costly procedure.
Colonoscopy is used as a screening technique, so even if you dont know if a person has colitis or not, thats currently the only way to clearly check and say they do, said investigator Dr A.G. Unil Perera. We are not talking about replacing colonoscopy. We have shown that a minimally invasive blood test can tell if a patient has an indication of colitis. Then, doctors can perform a colonoscopy to see how far the disease has spread and whether there are signs of cancer.
The screening only requires a simple finger prick to obtain a blood sample and infrared spectroscopy. Furthermore, it is faster, less invasive, and less costly compared with a colonoscopy.
Related Content:
Don’t Miss: Can You Have Constipation With Ulcerative Colitis
Blood And Stool Tests
A blood test can show if you have anemia, which is a symptom of ulcerative colitis. Anemia happens when your red blood cells decrease and there arenât enough of them to carry adequate oxygen to your tissues. A blood test will also help identify or rule out other infections.
The blood test can also detect an increase in white blood cells, a low level of the protein albumin, and an elevated C-reactive protein level — all indications of inflammation in your body.
When you go to the doctorâs office, they will take a little of your blood and send it off for analysis. The results will come back anywhere from a couple of days to several weeks later.
A stool test may be ordered to rule out infection. Learn more about stool testing.
How Do Doctors Use Endoscopy To Monitor Disease Activity
GI specialists use endoscopy not only to diagnose UC but also to learn how the condition is responding to treatment. This can help them determine whether a person needs changes to their treatment plan.
The goal of treatment is to bring UC into remission. This happens when someone with UC has few to no symptoms and the lining of their colon has healed.
Once a patient improved, a colonoscopy is often repeated 6 to 12 months later to make sure that the lining of the colon has healed with treatment. Then, colonoscopy may be repeated at varying intervals based on patient symptoms, said Dr. Jeffry A. Katz, M.D., a professor of medicine at Case Western Reserve University School of Medicine and the medical director of IBD at University Hospitals Cleveland Medical Center in Ohio.
In a 2017 review, researchers found that when the lining of the colon had healed, people with UC were more likely to stay in remission. They were also less likely to need surgery to remove the colon.
It is possible for someone with UC to have few symptoms while their colon still has inflammation. A 2013 study involved 149 people with UC who had few symptoms following treatment. Endoscopy showed that 45% of the participants still had inflammation in the colon.
Blood test results are also imperfect markers of disease activity in UC. For example, the ACG reports that up to a quarter of people with active UC have normal levels of C-reactive protein in their blood. This protein is a marker of inflammation.
You May Like: What Is Ultra Ulcerative Colitis
How Is Ulcerative Colitis Diagnosed
To diagnose ulcerative colitis in children, teenagers and adults, your healthcare provider has to rule out other illnesses. After a physical exam, your provider may order:
- Blood tests: Your blood can show signs of infection or anemia. Anemia is a low level of iron in your blood. It can mean you have bleeding in the colon or rectum.
- Stool samples: Signs of infection, parasites , and inflammation can show up in your poop.
- Imaging tests: Your healthcare provider may need a picture of your colon and rectum. You may have tests including a magnetic resonance imaging scan or computed tomography scan.
- Endoscopic tests: An endoscope is a thin, flexible tube with a tiny camera. Specialized doctors can slide the endoscope in through the anus to check the health of the rectum and colon. Common endoscopic tests include colonoscopy and sigmoidoscopy.
How Ulcerative Colitis Is Diagnosed
Ulcerative colitis has symptoms similar to many other digestive conditions, which can make diagnosis challenging. Because treatment is needed to induce remission and to prevent the disease from worsening, getting an accurate and timely diagnosis is important.
Gastroenterologists may use a variety of tests in order to understand whats going on with a patient who is suspected of having ulcerative colitis, but it is typically a colonoscopy with biopsies that is used to make the diagnosis.
You May Like: What Foods Irritate An Ulcer
Recommended Reading: Best Medicine For Ulcerative Colitis
Initial Testing And Evaluation
Your doctor will conduct a physical exam and ask you questions about your general health, diet, family history, home environment, and your daily activities.
Your doctor may then recommend a series of diagnostic tests. In addition to diagnosing ulcerative colitis, these tests are also performed to rule out infection.
Radiology Scans Or Diagnostic Imaging
Traditional upper GI endoscopy and colonoscopy are not be able to reach about two-thirds of the small intestine. Therefore, in addition to capsule endoscopy, various radiologic exams or diagnostic imaging may be performed to evaluate these parts of the intestines as well as to evaluate the actual wall of the bowel and surrounding areas outside the bowel.
X-rays
X-rays are the oldest way of imaging the inside of the body. X-rays are cost-effective and useful for detection of blockages in the small or large intestine.
Barium contrast studies
During a barium study, you will ingest a contrast material and have images taken with traditional X-ray technology. Barium is a chalky/milky liquid that you drink prior to the procedure. A series of X-rays are taken to observe the material flowing through the digestive system. These studies include:
Upper GI series examines the esophagus, stomach, and first part of the small bowel for patients with Crohns disease
Small bowel series and small bowel enteroclysis examines the entire small bowel. For a small bowel series, you will drink several cups of barium, and then have an X-ray taken every 1530 minutes as the barium travels down the small intestine and enters the large intestine. The time required varies but may take four to five hours. An enteroclysis is similar, except that the barium is placed directly into the small intestine through a tube introduced into the GI tract via the nose or mouth.
Cross-sectional imaging
Don’t Miss: Foods To Eat When You Have An Ulcer
Be Ready For Every Doctor Visit Test And Procedure
Whether youre seeing your gastroenterologist for a check-up or scheduled for a colonoscopy, its always important to be prepared for your visit and to maintain good communication with your doctormaking the most out of each experience. There are 2 main reasons for UC tests and procedures:
Diagnosis
How much of your time is your UC impacting?Find out and make a personal action plan.